ATI PHARMACOLOGY PRACTICE QUESTIONS
00:00
A client with cancer has been taking an opioid analgesic four times daily for chronic pain and reports needing increased doses for pain. What will the nurse tell the client?
A.
Over time, people can develop tolerance to opioids. We can discuss this with your provider
B. Take your medication more often to help control the pain
C. You are addicted and should take a different medication. We can discuss this with your provider
D. The risk of respiratory depression increases over time
Rationale
The nurse will tell the client that over time, people can develop tolerance to opioids, and they can discuss the need for dose adjustment with the provider, which appropriately addresses the client's concern while providing accurate information and maintaining a therapeutic relationship.
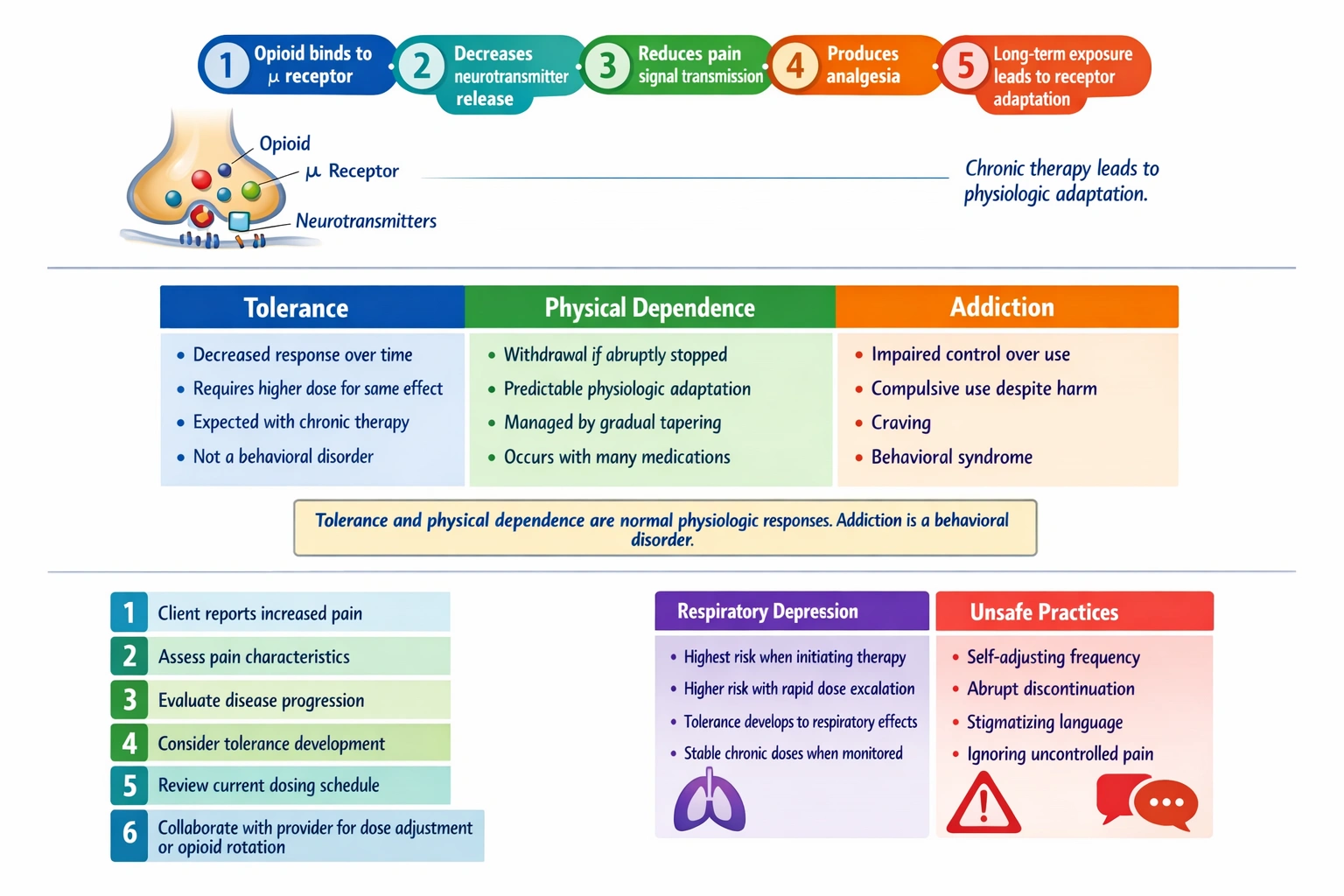
Pain management in patients with cancer is a complex and essential component of comprehensive oncologic care. Cancer-related pain can arise from the tumor itself compressing or infiltrating tissues, from diagnostic and therapeutic procedures, or from treatment-related side effects. Opioid analgesics remain the cornerstone of moderate to severe cancer pain management, and patients often require long-term opioid therapy throughout their disease course. A fundamental concept in understanding opioid therapy is the distinction between tolerance, physical dependence, and addiction, which are often confused by both patients and healthcare providers. Tolerance is a predictable physiological phenomenon characterized by a decreased response to a given dose of opioid over time, requiring higher doses to achieve the same analgesic effect. This occurs through multiple mechanisms including downregulation of opioid receptors at the cell surface, changes in receptor coupling to intracellular signaling pathways, and activation of compensatory neurotransmitter systems that oppose opioid effects. In patients with cancer pain, tolerance is expected and does not indicate any problematic behavior or psychological condition. The client's report of needing increased doses for pain is a common and expected occurrence that should be addressed through appropriate dose adjustment based on pain assessment and clinical judgment.
A) Over time, people can develop tolerance to opioids. We can discuss this with your provider
This response is accurate, therapeutic, and demonstrates excellent communication skills that maintain the nurse-client relationship while addressing the client's concern appropriately. By explaining tolerance as a normal physiological phenomenon, the nurse validates the client's experience and provides education that reduces anxiety and misunderstanding. The term "tolerance" is used correctly to describe the decreased response to a given dose over time, which is exactly what the client is experiencing. The nurse does not use stigmatizing language or make assumptions about addiction, which is crucial because patients with cancer pain are already vulnerable and may fear being labeled as drug-seeking or addictive when they report inadequate pain relief. The offer to discuss this with the provider demonstrates advocacy and collaboration, showing the client that the nurse is on their side and will help facilitate appropriate pain management. This response opens the door for a thorough pain assessment, evaluation of possible causes for increased pain such as disease progression, and appropriate adjustment of the analgesic regimen under medical supervision. The nurse understands that dose adjustments for chronic cancer pain are expected and appropriate, and that the goal is to maintain adequate pain control throughout the disease course.
B) Take your medication more often to help control the pain
This response is inappropriate and potentially dangerous for several important reasons. Instructing the client to take medication more often than prescribed constitutes unauthorized medication regimen changes that could lead to serious consequences. The dosing interval for opioids is determined by the pharmacokinetic properties of the specific drug, including its time to peak effect, duration of action, and elimination half-life. Changing the frequency without a prescriber's order could result in drug accumulation, particularly if the drug or its active metabolites have long half-lives, leading to excessive sedation, respiratory depression, and other signs of opioid toxicity. Additionally, taking medication more often may not address the underlying issue if the client has developed tolerance, as tolerance affects the peak effect of each dose rather than the duration of action. The appropriate response to tolerance is typically to increase the dose of each administration while maintaining the same interval, or to switch to a different opioid, a practice known as opioid rotation, both of which require prescriber input. The nurse should never advise a client to alter the prescribed dosing regimen, as this violates safe medication administration principles and could result in patient harm. Instead, the nurse should facilitate a discussion with the provider about appropriate adjustments based on a comprehensive pain assessment.
C) You are addicted and should take a different medication. We can discuss this with your provider
This response is inaccurate, harmful, and reflects a profound misunderstanding of the difference between tolerance, physical dependence, and addiction. Addiction is a primary, chronic, neurobiologic disease characterized by impaired control over drug use, compulsive use, continued use despite harm, and craving. It is a behavioral syndrome, not simply a physiological response to medication. The client with cancer pain who requires increased doses due to disease progression, development of tolerance, or other legitimate medical reasons is not exhibiting addiction. Physical dependence, which is characterized by the development of withdrawal symptoms upon abrupt discontinuation or dose reduction, is also distinct from addiction and is expected with chronic opioid therapy. Labeling the client as addicted carries significant stigma and could have devastating consequences, including the client becoming reluctant to report pain or request adequate medication, leading to unnecessary suffering. The nurse who makes this accusation is also likely to damage the therapeutic relationship irreparably, undermining trust and communication. Even the offer to discuss a different medication with the provider is framed in a way that suggests the client is at fault rather than that the current regimen is inadequate. This response demonstrates critical gaps in knowledge about pain management, addiction medicine, and therapeutic communication.
D) The risk of respiratory depression increases over time
regarding chronic opioid use and could cause unnecessary fear that might discourage the client from seeking adequate pain relief. The risk of respiratory depression is highest when opioids are initiated or when doses are increased significantly, particularly in opioid-naïve individuals. With chronic use, tolerance develops not only to the analgesic effects of opioids but also to the respiratory depressant effects. This means that patients on stable, long-term opioid therapy are actually at lower risk of respiratory depression from their usual doses than they were when starting therapy. The development of tolerance to respiratory depression is one of the reasons that stable doses in tolerant patients are relatively safe. If the client's dose is increased appropriately under medical supervision to address tolerance or increased pain, the risk of respiratory depression is managed by gradual titration and careful monitoring, not by an inevitable increase in risk over time. Providing this inaccurate information could lead the client to resist necessary dose increases and suffer needlessly from uncontrolled pain. The nurse should provide accurate information about the balance of benefits and risks of opioid therapy and the measures taken to ensure safety, not frightening and incorrect statements about increasing risk.
Conclusion
When a client with cancer pain reports needing increased doses of their opioid analgesic, the nurse should explain that tolerance is a normal physiological phenomenon that occurs over time with chronic opioid use, and offer to discuss dose adjustment with the provider. Advising the client to take medication more often than prescribed is unsafe and unauthorized. Labeling the client as addicted is inaccurate, stigmatizing, and damaging to the therapeutic relationship. Claiming that respiratory depression risk increases over time is incorrect, as tolerance develops to this effect as well. Therefore, the correct response is to acknowledge tolerance as expected and facilitate appropriate medical evaluation and dose adjustment through the provider.
Naloxone is effective because of which action?
A.
Preventing activation of opioid receptors through antagonist actions
B. Regulating the sensitivity of opioid receptors by neurochemical alterations
C. Increasing the excretion of morphine sulfate by altering serum pH
D. Countering the effects of morphine sulfate by agonist actions
Rationale
Naloxone is effective because it prevents activation of opioid receptors through competitive antagonist actions, rapidly reversing the effects of opioid agonists by displacing them from receptor sites without producing any opioid effects itself.
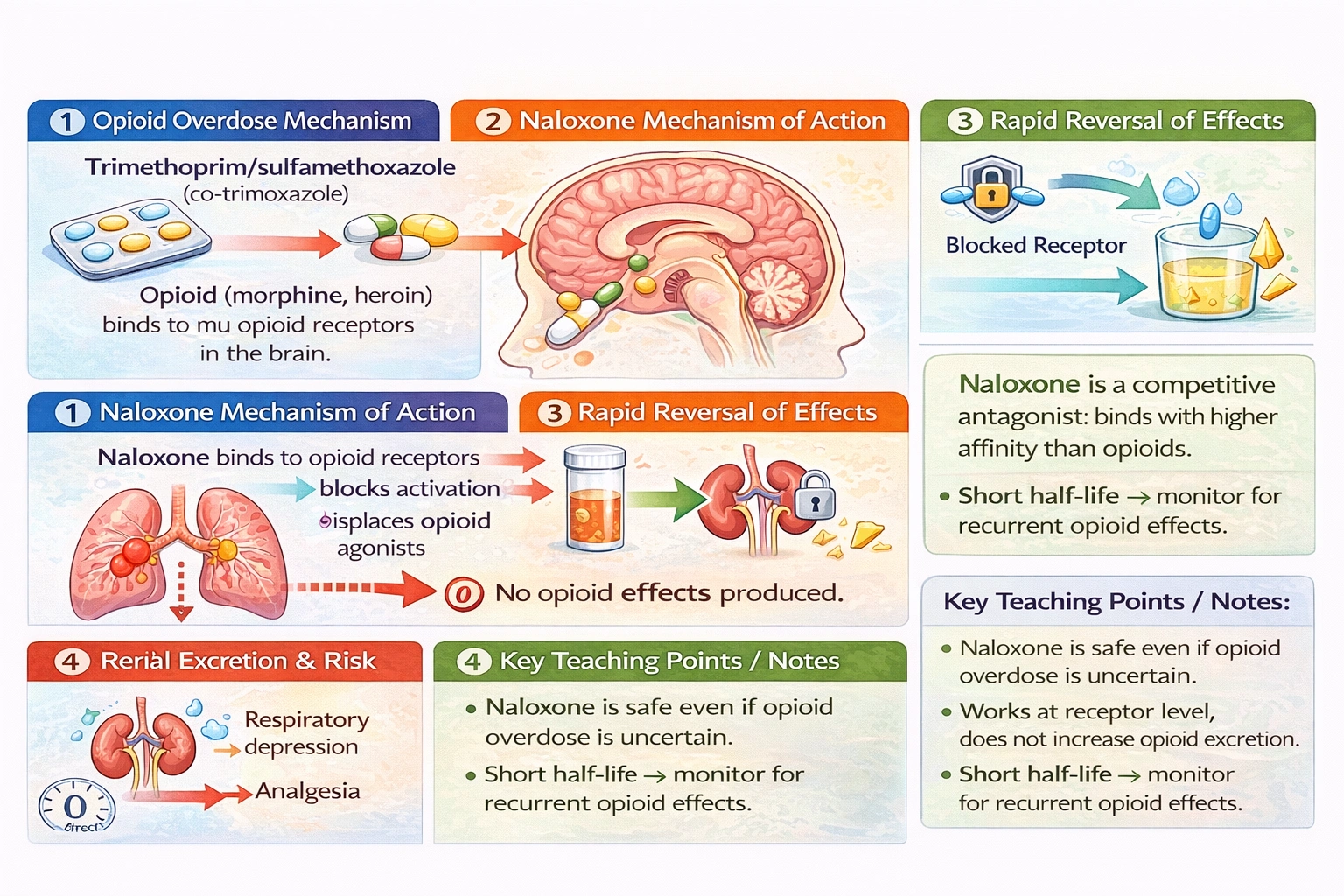
Naloxone is a life-saving medication used in the emergency management of opioid overdose, a situation that has reached epidemic proportions in many parts of the world. Opioids such as heroin, morphine, oxycodone, and fentanyl produce their effects by binding to and activating mu, kappa, and delta opioid receptors in the central nervous system and elsewhere. Activation of mu receptors in the brainstem produces respiratory depression, which is the primary cause of death in opioid overdose. Activation of these receptors also produces analgesia, sedation, and euphoria. Understanding the mechanism by which naloxone reverses these effects is fundamental to its appropriate use and to appreciating why it is such an effective antidote. Naloxone is a pure opioid antagonist, meaning it binds to opioid receptors but does not activate them, and its presence prevents agonists from binding and exerting their effects.
A) Preventing activation of opioid receptors through antagonist actions
This statement accurately describes naloxone's mechanism of action and is the correct explanation for its effectiveness. Naloxone is a competitive antagonist at mu, kappa, and sigma opioid receptors. It has a high affinity for these receptors, meaning it binds tightly and effectively. When administered to a patient with opioid overdose, naloxone molecules compete with the opioid agonist molecules for binding sites on the receptors. Because naloxone has higher affinity than many agonists, it can displace agonists that are already bound and prevent additional agonist molecules from binding. However, crucially, naloxone binding does not trigger the intracellular signaling pathways that are activated when an agonist binds. It occupies the receptor without producing any effect, essentially blocking the receptor and preventing it from being activated. This rapidly reverses the effects of the agonist, including respiratory depression, sedation, and hypotension. The onset of action is rapid, usually within minutes of intravenous administration, making it ideal for emergency use. Naloxone has no intrinsic activity at opioid receptors and produces no effects in the absence of opioids, which is why it is safe to administer even if the diagnosis of opioid overdose is uncertain.
B) Regulating the sensitivity of opioid receptors by neurochemical alterations
This description does not accurately represent naloxone's mechanism of action. Naloxone does not alter receptor sensitivity through neurochemical changes or any form of receptor regulation. It works through direct competitive antagonism at the receptor site, meaning it physically occupies the receptor and prevents agonist binding. It does not change the sensitivity of receptors or alter the neurochemical environment. This description is vague and suggests a mechanism that is not applicable to naloxone. Receptor sensitivity regulation is a longer-term adaptive process that occurs with chronic agonist or antagonist exposure, such as upregulation or downregulation of receptors, not the acute reversal of overdose.
C) Increasing the excretion of morphine sulfate by altering serum pH
This statement reflects a misunderstanding of how naloxone works. Naloxone does not affect drug excretion in any way. It does not alter serum pH, enhance renal clearance, or change the metabolism of opioids. Opioid elimination occurs through hepatic metabolism, primarily by cytochrome P450 enzymes, and renal excretion of metabolites, processes that are not influenced by naloxone administration. The reason naloxone works so rapidly is that it acts at the receptor level, not by removing the drug from the body. The opioid molecules remain in the body, but their effects are blocked because naloxone occupies the receptors. Once naloxone is metabolized and cleared, which occurs relatively quickly with a half-life of about 60 to 90 minutes, the opioid molecules can rebind to receptors and cause recurrent respiratory depression if the opioid itself has not yet been eliminated. This is why patients who have received naloxone for overdose must be monitored closely for signs of recurrent respiratory depression.
D) Countering the effects of morphine sulfate by agonist actions
This statement is contradictory and incorrect. Agonists are drugs that bind to receptors and activate them, producing an effect. Antagonists are drugs that bind to receptors but do not activate them, blocking the effects of agonists. Naloxone is a pure antagonist, not an agonist. If naloxone had agonist actions, it would produce opioid-like effects such as respiratory depression, sedation, and analgesia, which would worsen an overdose rather than reverse it. The term "countering" is correct in that naloxone does counter the effects of morphine, but the mechanism described is wrong. Naloxone counters opioid effects through antagonism, not agonism. This distinction is fundamental to understanding how naloxone works and why it is safe and effective for overdose reversal.
Conclusion
Naloxone is effective because it prevents activation of opioid receptors through competitive antagonist actions, binding to receptors with high affinity, displacing opioid agonists, and blocking receptor activation without producing any opioid effects itself. It does not regulate receptor sensitivity through neurochemical alterations. It does not increase drug excretion or alter serum pH. It does not counter opioid effects through agonist actions, as agonists would produce rather than reverse opioid effects. Therefore, the correct description is preventing receptor activation through antagonist actions, which is the mechanism that makes naloxone a life-saving antidote for opioid overdose.
Which of these findings, from a client taking steroids, should the nurse report immediately?
A.
Temperature of 101.2 degrees F
B. Glucose 128 mg/dL
C. Blood pressure of 144/68 mm Hg
D. Heart rate of 102 beats per minute
Rationale
The nurse should report a temperature of 101.2 degrees Fahrenheit immediately in a client taking steroids because glucocorticoids have immunosuppressive effects that can mask the signs and symptoms of infection, making fever a potentially late and ominous sign of serious underlying infection.
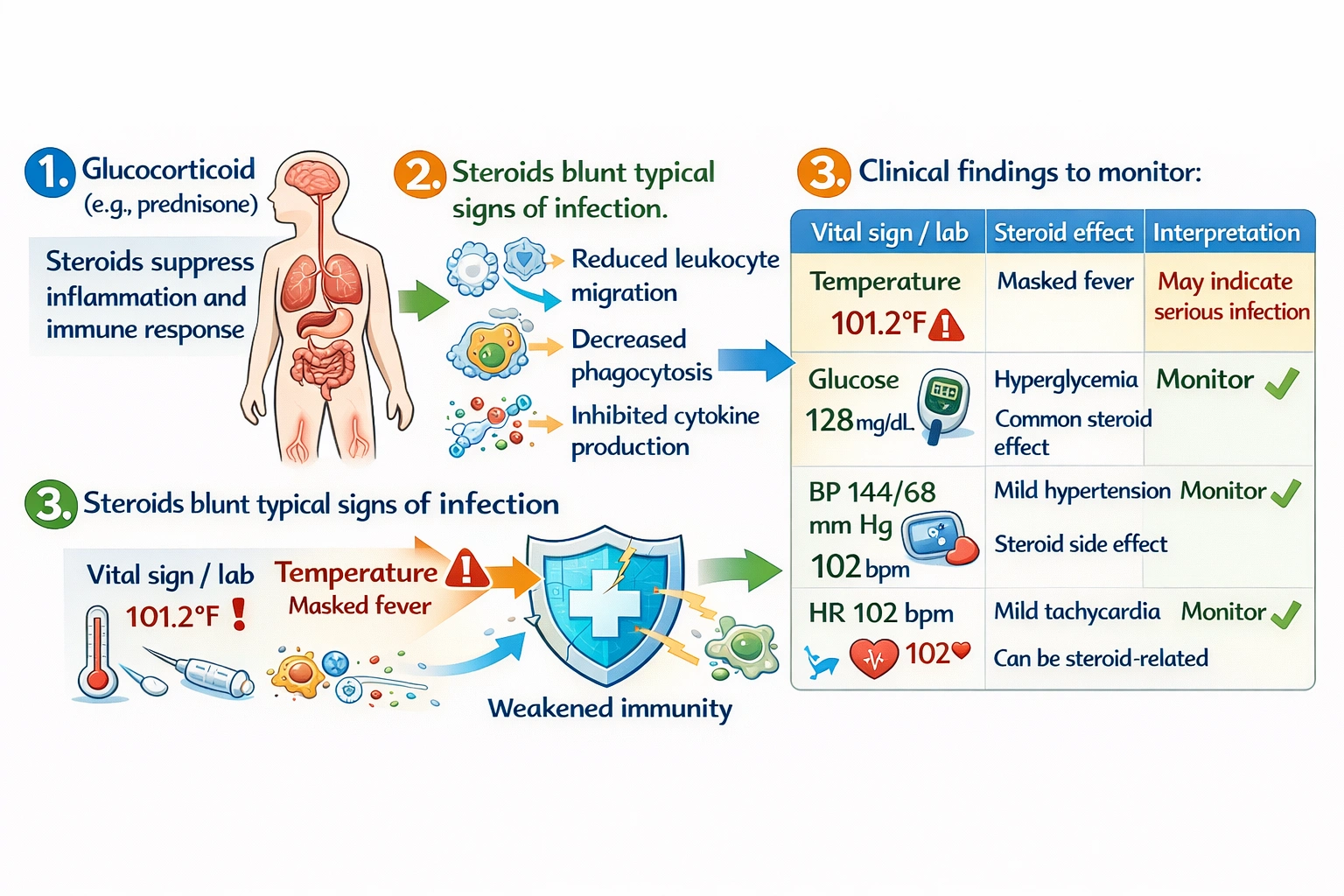
Glucocorticoids are among the most potent anti-inflammatory and immunosuppressive medications available, and these effects have important implications for how infections present in patients taking them. Corticosteroids suppress the immune system through multiple mechanisms, including inhibition of cytokine production, reduced leukocyte migration to sites of inflammation, decreased phagocytosis, and suppression of fever production. Fever is normally generated through the action of prostaglandins on the hypothalamus, and glucocorticoids inhibit the production of prostaglandins by blocking phospholipase A2 and cyclooxygenase. This means that a patient taking steroids may have a serious infection but mount little or no febrile response. When fever does occur in a steroid-treated patient, it may indicate that the infection is severe enough to overcome this suppression, or that the steroid dose is inadequate to mask the fever. In either case, fever in a patient on steroids warrants immediate attention because it may indicate a significant infection that requires prompt diagnosis and treatment.
A) Temperature of 101.2 degrees F
This finding should be reported immediately. Fever in a client taking steroids is concerning because steroids mask typical infectious signs, meaning that the infection causing this fever could be significant and potentially life-threatening. The client's immunosuppressed state increases the risk of rapid progression of infection, and delay in treatment could have serious consequences. The nurse should report this finding immediately for prompt evaluation, which may include a thorough physical assessment, laboratory studies such as complete blood count and cultures, and imaging studies as indicated. Early identification and treatment of infection in immunosuppressed patients is critical to prevent morbidity and mortality.
B) Glucose 128 mg/dL
A glucose of 128 mg/dL is elevated but not immediately reportable in a client taking steroids. Steroids commonly cause hyperglycemia through several mechanisms, including promoting gluconeogenesis in the liver, reducing glucose uptake in peripheral tissues, and increasing insulin resistance. This level is above the normal range but not critical. The nurse should monitor glucose trends and may need to report if persistent or rising, but it does not require immediate emergency reporting. Management may include dietary modifications, increased monitoring, or adjustment of diabetic medications if the client has diabetes.
C) Blood pressure of 144/68 mm Hg
This blood pressure is elevated but not immediately reportable. Steroids can cause hypertension through mineralocorticoid effects, including sodium and water retention, and through increased vascular reactivity to vasoconstrictors. A systolic of 144 is above normal but not a hypertensive emergency requiring immediate intervention. The nurse should monitor and may report if sustained, but this finding alone does not warrant immediate action. The diastolic pressure is normal, which is somewhat reassuring.
D) Heart rate of 102 beats per minute
A heart rate of 102 is mildly tachycardic but not immediately reportable. Steroids can cause tachycardia through various mechanisms, and this rate could also be due to other factors such as anxiety, pain, dehydration, or mild infection. Without other concerning symptoms, this does not warrant immediate reporting. The nurse should assess for other signs and consider possible causes, but this finding alone is not an emergency.
Conclusion
In a client taking steroids, a temperature of 101.2 degrees Fahrenheit should be reported immediately due to the masking effect of steroids on infection, which means that fever may indicate serious underlying infection requiring prompt diagnosis and treatment. Mild hyperglycemia, mild hypertension, and mild tachycardia are common steroid side effects that do not require immediate reporting. Therefore, fever is the finding that warrants immediate attention, and the nurse should act promptly to ensure appropriate evaluation and management.
A client will receive oral ciprofloxacin to treat a urinary tract infection. The nurse provides teaching for this client. Which statement by the client indicates further teaching?
A.
I should take this medication with milk to improve absorption
B. I will need to use sunscreen every time I go outdoors
C. I should stop taking the medication immediately if I experience heel pain
D. I may have abdominal pain and nausea, but these are usually mild
Rationale
The statement that the client should take ciprofloxacin with milk to improve absorption indicates need for further teaching, as milk contains calcium that chelates ciprofloxacin and significantly reduces its absorption, potentially leading to therapeutic failure of the antibiotic.
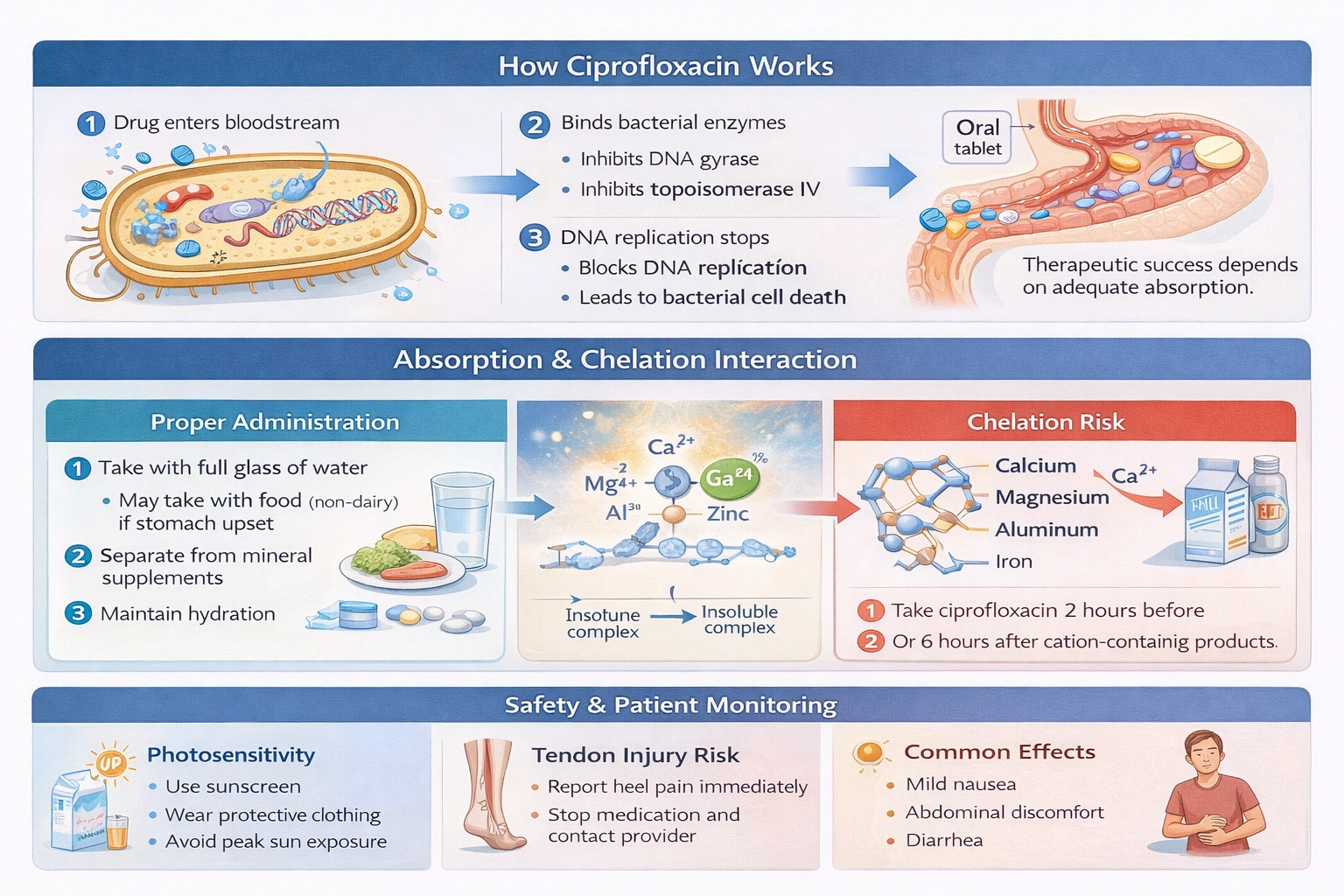
Ciprofloxacin is a fluoroquinolone antibiotic with broad-spectrum activity against both gram-negative and gram-positive bacteria, making it useful for a variety of infections including urinary tract infections, respiratory infections, and gastrointestinal infections. Its mechanism of action involves inhibition of bacterial DNA gyrase and topoisomerase IV, enzymes essential for bacterial DNA replication, transcription, and repair. For ciprofloxacin to be effective, it must be adequately absorbed from the gastrointestinal tract into the systemic circulation, where it can reach the site of infection. However, ciprofloxacin has a significant and well-documented drug interaction with divalent and trivalent cations, including calcium, magnesium, aluminum, iron, and zinc. These cations form insoluble chelates with ciprofloxacin in the gut, meaning that the drug binds to the cation and forms a complex that cannot be absorbed across the intestinal epithelium. This can reduce ciprofloxacin bioavailability by up to 50 percent or more, potentially leading to subtherapeutic antibiotic levels and treatment failure. Milk is a rich source of calcium, and taking ciprofloxacin with milk will result in this chelation interaction, significantly reducing drug absorption.
A) I should take this medication with milk to improve absorption
This statement demonstrates a critical misunderstanding that requires immediate correction. The client has the interaction exactly backwards, believing that milk will improve absorption when in fact it dramatically reduces it. This misconception could lead to therapeutic failure of the antibiotic, meaning the urinary tract infection might not resolve, symptoms could persist or worsen, and the bacteria could develop resistance. The nurse must explain that ciprofloxacin should be taken either two hours before or six hours after any dairy products, calcium supplements, or other cation-containing products. This timing allows the medication to be absorbed before the calcium is introduced, or allows the calcium from a previous dose to clear before the next antibiotic dose. The client should be instructed to take ciprofloxacin with a full glass of water, on an empty stomach if possible, and to separate it from dairy and other cation-containing products by the specified intervals.
B) I will need to use sunscreen every time I go outdoors
This statement shows appropriate understanding of an important precaution with ciprofloxacin therapy. Fluoroquinolones, including ciprofloxacin, can cause photosensitivity, which is an exaggerated skin reaction to ultraviolet light exposure. Patients taking these medications may experience severe sunburn, rash, or blistering with even modest sun exposure. The risk persists throughout the course of therapy and for several days after discontinuation. The client who understands that they need to use sunscreen and take other sun protection measures, such as wearing protective clothing and avoiding peak sun hours, demonstrates knowledge of this common side effect and how to prevent it. This is a correct and important part of ciprofloxacin education.
C) I should stop taking the medication immediately if I experience heel pain
This statement shows appropriate understanding of a serious but rare adverse effect of fluoroquinolones. Ciprofloxacin and other drugs in this class are associated with an increased risk of tendonitis and tendon rupture, most commonly affecting the Achilles tendon but potentially involving other tendons as well. The risk is higher in patients over 60 years of age, those taking concomitant corticosteroids, and those with kidney, heart, or lung transplants. Heel pain could indicate inflammation of the Achilles tendon, and if tendonitis develops, continuing the medication could increase the risk of tendon rupture, which would be a serious complication requiring surgical repair and prolonged recovery. The client who knows to stop the medication and contact their provider if they experience heel pain demonstrates understanding of this important safety warning. This is correct and essential education for anyone taking a fluoroquinolone antibiotic.
D) I may have abdominal pain and nausea, but these are usually mild
This statement shows appropriate understanding of common gastrointestinal side effects associated with ciprofloxacin. Like many antibiotics, ciprofloxacin can cause gastrointestinal disturbances including nausea, abdominal discomfort, diarrhea, and vomiting. These effects are usually mild and self-limiting, and they often improve as the body adjusts to the medication. The client who expects these symptoms and understands that they are typically not a cause for alarm demonstrates appropriate knowledge. However, the client should also be instructed to report severe or persistent gastrointestinal symptoms, as they could indicate a more serious problem such as Clostridium difficile infection. But for mild, expected symptoms, this understanding is appropriate and correct.
Conclusion
The client needs further teaching when stating they should take ciprofloxacin with milk to improve absorption, as milk actually decreases absorption due to calcium chelation. Sunscreen use for photosensitivity, stopping for heel pain due to tendonitis risk, and expecting mild GI effects all demonstrate appropriate understanding. Therefore, the milk statement requires correction, and the nurse must explain the importance of separating ciprofloxacin from dairy and other cation-containing products to ensure adequate antibiotic absorption and therapeutic success.
A client receiving a cephalosporin develops a secondary intestinal infection caused by Clostridium difficile. What treatment plan would the nurse advocate for?
A.
Discontinue the cephalosporin and begin metronidazole or oral vancomycin as ordered
B. Increase the dose of the cephalosporin and provide isolation measures
C. Stop all antibiotics and probiotics
D. Add an antibiotic, such as tobramycin, to the client's regimen
Rationale
The nurse would advocate to discontinue the cephalosporin and begin metronidazole or oral vancomycin as ordered, as this is the standard evidence-based treatment for Clostridium difficile infection, removing the offending antibiotic and providing specific therapy against C. difficile.
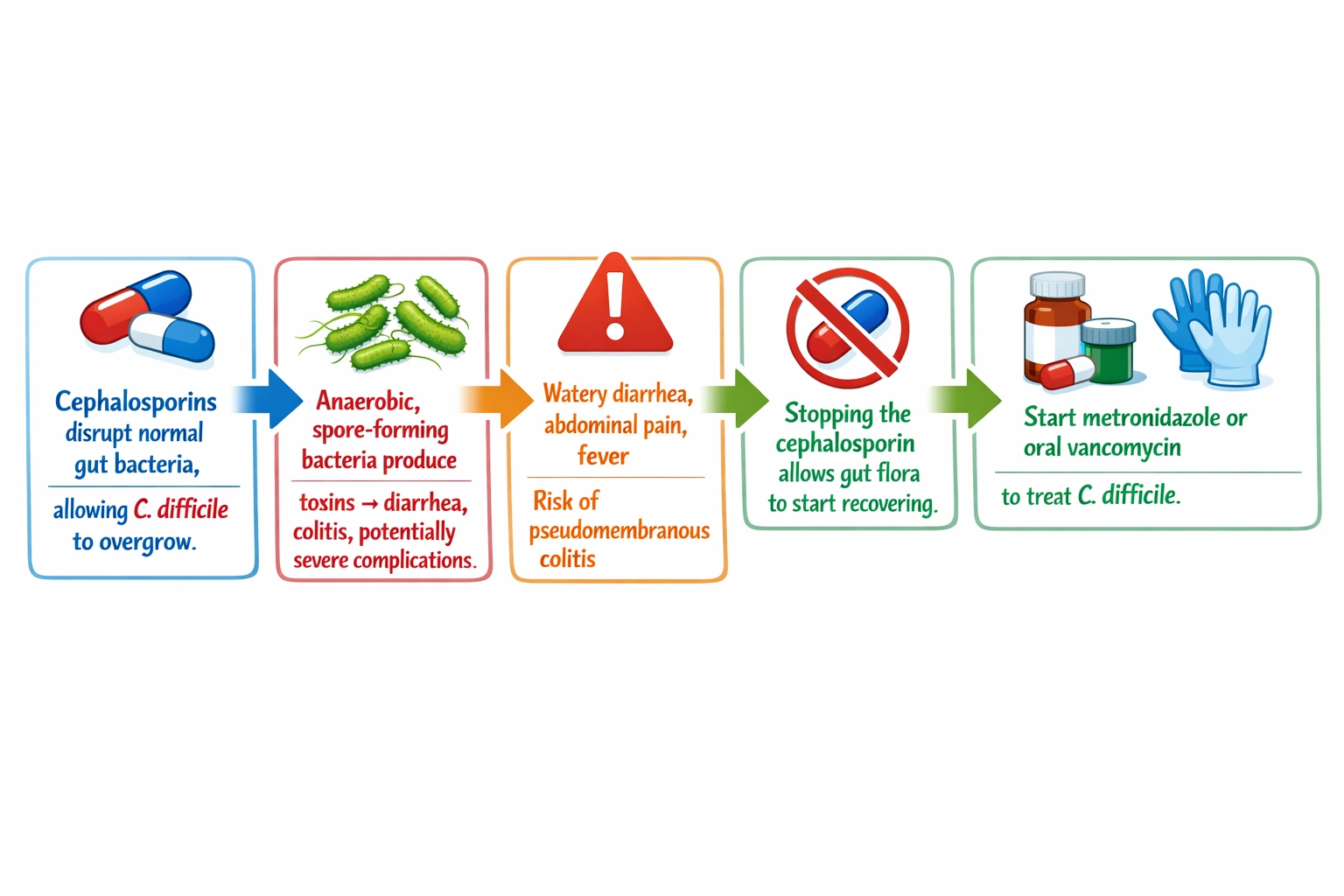
Clostridium difficile infection is a significant healthcare-associated infection that occurs when broad-spectrum antibiotics disrupt the normal gut flora, allowing C. difficile, an anaerobic, spore-forming, toxin-producing bacterium, to overgrow and cause disease. Cephalosporins are among the antibiotics most commonly associated with CDI because they have broad-spectrum activity that suppresses many normal protective bacteria while having limited activity against C. difficile itself. The infection ranges from mild, self-limited diarrhea to severe, life-threatening pseudomembranous colitis. The treatment of CDI involves several key principles based on clinical practice guidelines. First, the inciting antibiotic should be discontinued whenever possible. Continuing the offending antibiotic perpetuates the disruption of gut flora and allows C. difficile to continue proliferating. Second, specific antibiotic therapy directed against C. difficile should be initiated. Metronidazole was historically first-line for mild to moderate CDI, but current guidelines favor oral vancomycin or fidaxomicin as first-line therapy for most cases, with metronidazole reserved for situations where vancomycin is not available or for initial episodes of non-severe CDI when access to vancomycin is limited. Third, infection control measures, including contact precautions, should be implemented to prevent transmission to other patients.
A) Discontinue the cephalosporin and begin metronidazole or oral vancomycin as ordered
This is the correct treatment plan that the nurse should advocate for. Discontinuing the cephalosporin removes the ongoing disruption of gut flora, allowing the normal microbiome to begin recovering. Initiating specific therapy against C. difficile with metronidazole or oral vancomycin targets the pathogen directly. Oral vancomycin is preferred for severe CDI because it achieves high concentrations in the colon with minimal systemic absorption. The nurse should support this evidence-based approach and ensure that appropriate orders are obtained.
B) Increase the dose of the cephalosporin and provide isolation measures
Increasing the dose of the cephalosporin would worsen the CDI by further disrupting gut flora and providing no benefit against C. difficile. Isolation measures are important to prevent transmission to other patients, but they do not treat the infection. This plan is incorrect and would likely lead to progression of the CDI.
C) Stop all antibiotics and probiotics
Stopping all antibiotics may be appropriate in some cases, but specific treatment for C. difficile is needed. Probiotics alone are not sufficient to treat active CDI, and their role in prevention or treatment is controversial. While some probiotics may help restore gut flora, they should not be used as primary treatment for active infection. The patient requires specific antibiotic therapy directed against C. difficile.
D) Add an antibiotic, such as tobramycin, to the client's regimen
Adding another antibiotic, especially one that further disrupts gut flora, would likely worsen CDI. Tobramycin is an aminoglycoside that has no activity against C. difficile and would contribute to further disruption of the normal microbiome. This plan is incorrect and potentially harmful.
Conclusion
For C. difficile infection secondary to cephalosporin use, the nurse should advocate to discontinue the cephalosporin and begin metronidazole or oral vancomycin as ordered. Increasing the cephalosporin, stopping all antibiotics without specific therapy, or adding tobramycin are all incorrect. Therefore, discontinuing cephalosporin and starting CDI therapy is correct, following established treatment guidelines for this potentially serious infection
A pregnant client stopped using a prescription medication she takes for asthma because she doesn't want to harm her baby. What will the nurse tell the client?
A.
Stopping medications for asthma doubles the chances of stillbirth
B. Resume the medicines in her second trimester
C. Avoid taking medications during her pregnancy
D. Asthma medications will not affect the fetus
Rationale
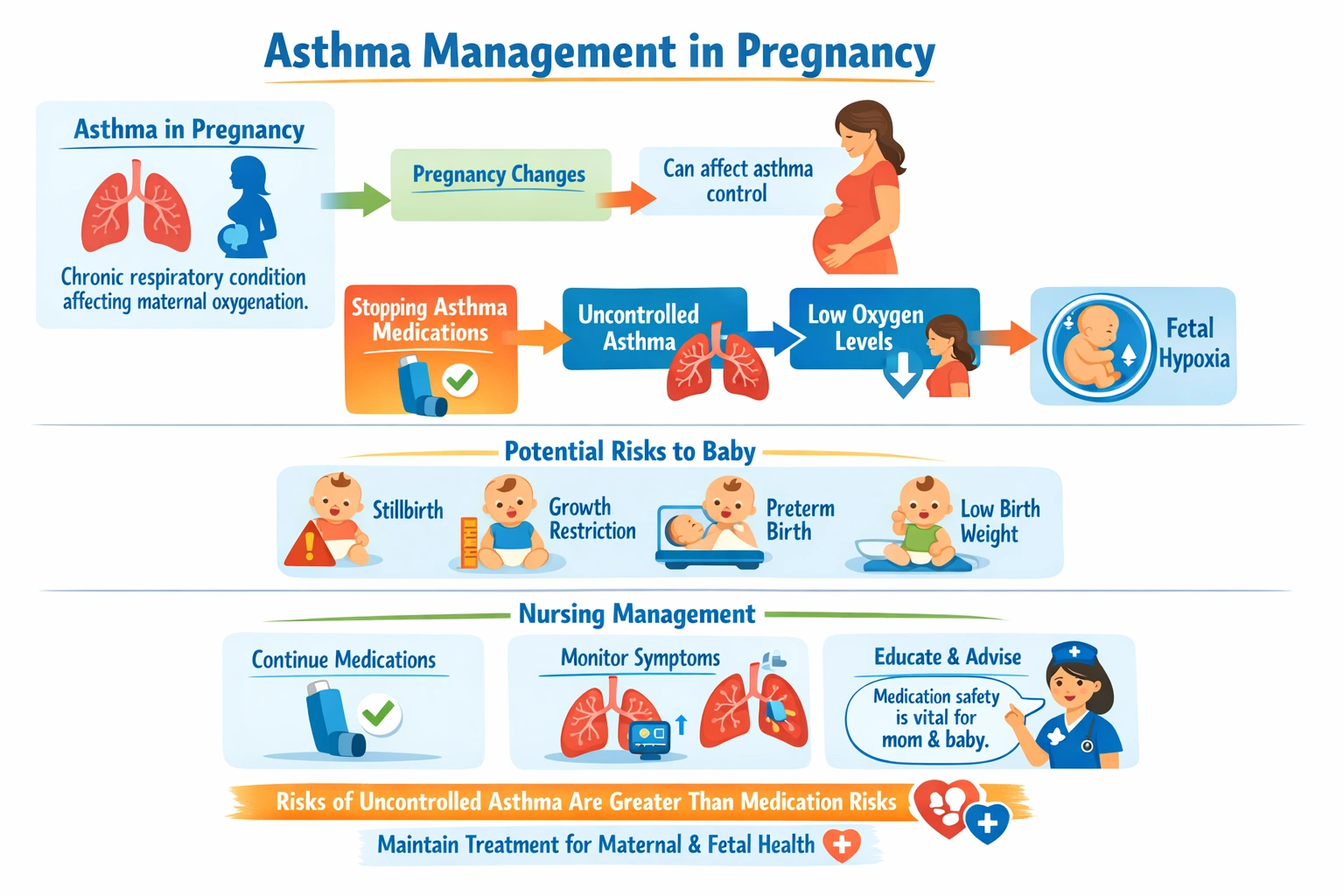
The nurse will tell the client that stopping medications for asthma doubles the chances of stillbirth, conveying that uncontrolled asthma poses significant risks to the fetus, and continuing prescribed asthma medications is essential for maternal and fetal health.
Asthma is one of the most common medical conditions complicating pregnancy, affecting up to 8 percent of pregnant women. The physiologic changes of pregnancy can affect asthma control, and asthma itself can affect pregnancy outcomes. Uncontrolled asthma during pregnancy poses significant risks to both the mother and fetus. Maternal hypoxemia from poor asthma control can lead to fetal hypoxia, as the fetus depends on adequate maternal oxygenation. This can result in intrauterine growth restriction, preterm birth, low birth weight, and increased risk of perinatal mortality. Studies have shown that women with uncontrolled asthma have higher rates of preeclampsia, gestational hypertension, and cesarean delivery. The risks of uncontrolled asthma far outweigh the risks of most asthma medications, which have been studied extensively in pregnancy and are generally considered safe. The nurse must emphasize that continuing prescribed asthma medications is essential for maintaining adequate oxygenation and preventing complications.
A) Stopping medications for asthma doubles the chances of stillbirth
This statement, while direct and concerning, conveys the serious risk of uncontrolled asthma and the importance of continuing medication. Research has shown that poorly controlled asthma is associated with increased perinatal mortality, and this message helps the client understand that stopping medication is not protecting her baby but actually endangering it.
B) Resume the medicines in her second trimester
Delaying treatment until the second trimester leaves the client untreated during the first trimester, a critical period for fetal development. Asthma can worsen at any time during pregnancy, and treatment should be continued as prescribed throughout. This advice is incorrect and dangerous.
C) Avoid taking medications during her pregnancy
This advice is the opposite of what the client needs to hear. Avoiding medications would lead to uncontrolled asthma, which poses greater risks than the medications themselves. The nurse must correct this misconception.
D) Asthma medications will not affect the fetus
This statement is not entirely accurate. Some asthma medications may have risks, but the benefits of controlling asthma outweigh those risks. The statement oversimplifies and may not be fully truthful. The nurse should provide balanced information about risks and benefits, emphasizing that the risks of uncontrolled asthma are greater than the risks of the medications.
Conclusion
The nurse should explain that stopping asthma medications increases risks including stillbirth, and that continuing prescribed treatment is essential for fetal and maternal health. Delaying, avoiding, or falsely claiming no fetal effects are incorrect. Therefore, the stillbirth risk statement is correct, conveying the serious consequences of untreated asthma during pregnancy.
Which actions occur in fatal medication errors?
A.
Confusing drugs with similar packaging
B. Confusing drugs with names that look or sound alike
C. Giving a drug intravenously instead of intramuscularly
D. Using barcode scanning to verify client's name and birthdate
Rationale
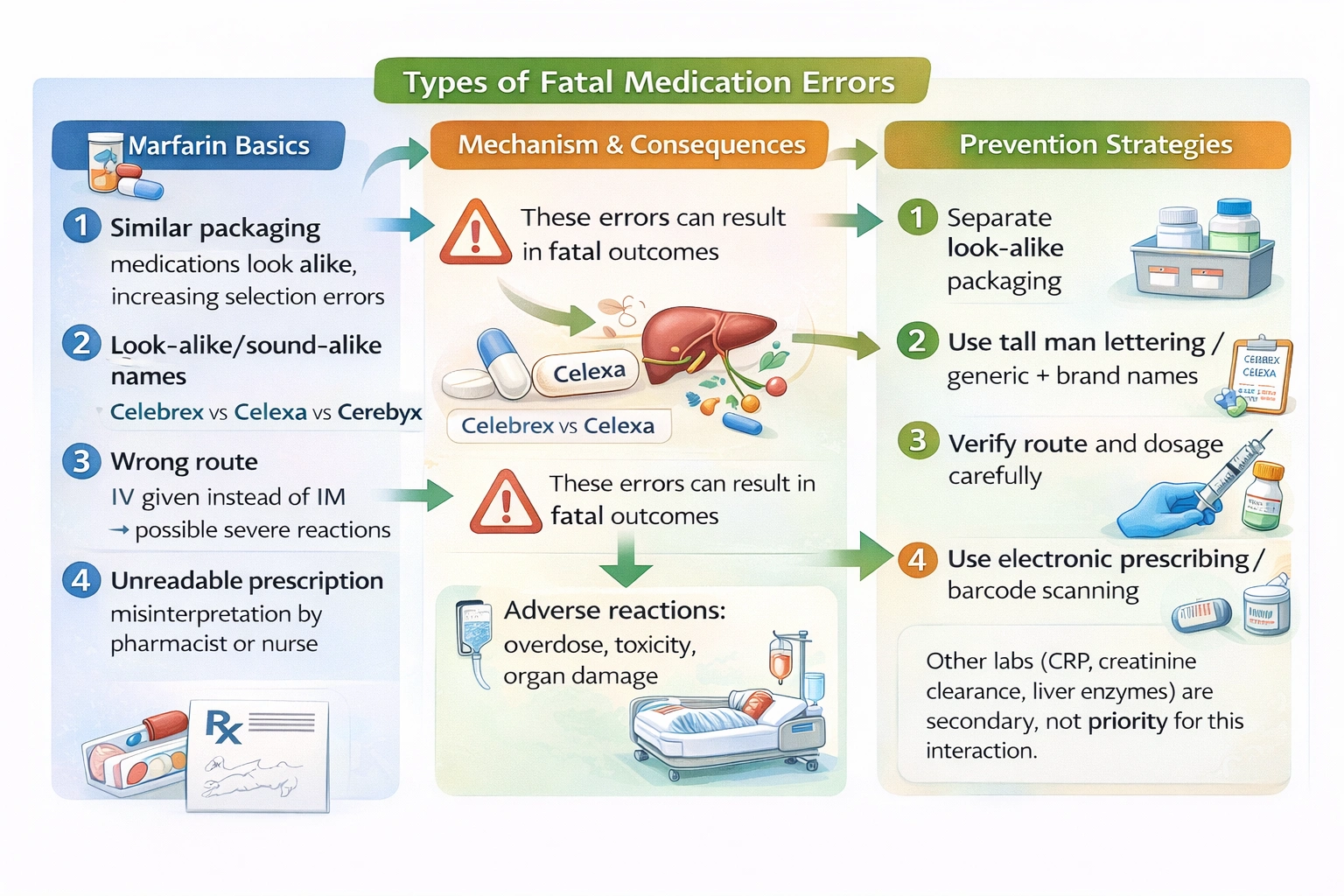
Actions that occur in fatal medication errors include confusing drugs with similar packaging, confusing drugs with names that look or sound alike, giving a drug intravenously instead of intramuscularly, and writing a prescription that is unreadable, as these represent preventable mistakes at various points in the medication use process that have been identified in root cause analyses of fatal errors.
Medication errors are a significant cause of morbidity and mortality in healthcare systems worldwide. Understanding the common causes of fatal medication errors is essential for developing prevention strategies and improving patient safety. The medication use process involves multiple steps, including prescribing, transcribing, dispensing, administering, and monitoring, and errors can occur at any of these points. Root cause analyses of fatal errors have identified several recurring themes and contributing factors. Look-alike and sound-alike drug names are a well-documented cause of errors, as similar names can lead to selection of the wrong drug, particularly when orders are handwritten or when medications are stocked near each other. Similar packaging can also contribute to selection errors when products look alike on the shelf. Wrong route errors, such as giving an intravenous formulation when intramuscular was intended, can have catastrophic consequences, especially if the drug is not intended for IV use or causes severe reactions when given by the wrong route. Unreadable prescriptions lead to misinterpretation and incorrect dispensing or administration. These factors have been consistently identified in analyses of medication errors that resulted in patient death.
A) Confusing drugs with similar packaging
This is a known cause of medication errors that can have fatal consequences. When multiple medications have similar packaging, such as similar vial sizes, labels, or colors, there is increased risk that a healthcare provider will select the wrong drug, particularly in stressful or busy situations. For example, if two medications are stored next to each other and have similar appearance, a nurse might inadvertently pick up the wrong vial and administer the wrong drug. This type of error has been implicated in fatal outcomes and is why organizations like the Institute for Safe Medication Practices advocate for distinctive packaging and storage practices that separate look-alike products.
B) Confusing drugs with names that look or sound alike
This is another well-documented cause of fatal medication errors. The FDA and ISMP maintain lists of look-alike/sound-alike drug names to increase awareness and prevent errors. Examples include Celebrex, Celexa, and Cerebyx, which have been confused with each other with serious consequences. These errors can occur at any point in the medication use process, from prescribing to administration. Strategies to prevent these errors include using both brand and generic names, including the indication on prescriptions, and using tall man lettering to highlight differences in similar names.
C) Giving a drug intravenously instead of intramuscularly
Wrong route errors can be fatal, especially when the drug is not formulated for intravenous administration. Some medications intended for intramuscular use contain preservatives or other additives that can be toxic when given intravenously. Others may cause severe hypotension, cardiac arrhythmias, or anaphylactoid reactions when given by the wrong route. Even drugs that are available in both IV and IM formulations can cause harm if the IV dose is given when a smaller IM dose was intended, or if the IV formulation is given too rapidly. These errors are preventable with careful attention to the prescribed route and verification before administration.
D) Using barcode scanning to verify client's name and birthdate
Barcode scanning is an error-prevention strategy, not a cause of errors. Barcode medication administration systems are designed to ensure the five rights of medication administration: right patient, right drug, right dose, right route, and right time. When the nurse scans the patient's wristband and the medication, the system verifies that the medication is correct for that patient at that time. This technology has been shown to significantly reduce medication administration errors and is considered a best practice for patient safety. It is not a cause of fatal errors but rather a prevention measure.
E) Writing a prescription that is unreadable
Illegible prescriptions have been identified as a cause of serious and fatal medication errors for decades. When a prescription is difficult to read, the pharmacist may misinterpret the drug name, dose, or directions, leading to dispensing of the wrong medication or incorrect dose. This can result in patient harm or death. The move toward electronic prescribing has been driven in part by the need to eliminate illegible handwriting as a source of errors. When handwritten prescriptions are necessary, they should be printed clearly, and the use of dangerous abbreviations should be avoided.
Conclusion
Actions that occur in fatal medication errors include confusing drugs with similar packaging or look-alike names, giving drugs by the wrong route, and writing unreadable prescriptions. Barcode scanning is an error-prevention strategy, not a cause of errors. Therefore, A, B, C, and E are correct, representing common contributing factors to fatal medication errors that have been identified through patient safety research and root cause analyses.
A 50-year-old postmenopausal client who has had a hysterectomy has moderate to severe hot flashes and is discussing estrogen therapy with the nurse. What will the nurse tell the client regarding the side effect of estrogen therapy?
A.
An estrogen progesterone product will increase side effects
B. Transdermal preparations of estrogen therapy have reduced side effects
C. Side effects of estrogen therapy are uncommon among women of her age
D. An intravaginal preparation may be best
Rationale
The nurse will tell the client that transdermal preparations of estrogen therapy have reduced side effects compared to oral formulations.
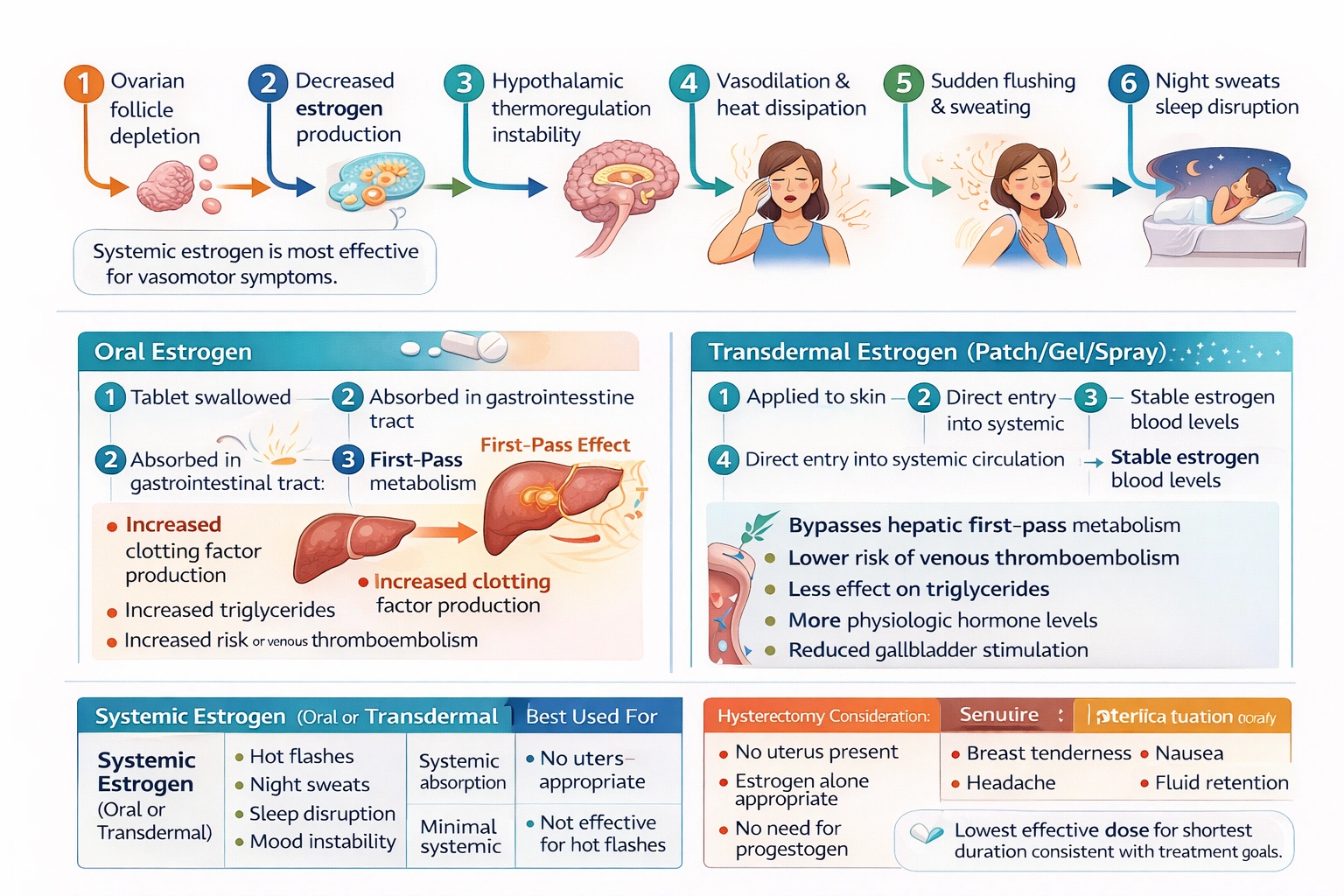
Menopause represents a normal physiological transition in a woman's life marked by the permanent cessation of menstruation resulting from loss of ovarian follicular function. The declining levels of estrogen produced by the ovaries lead to a variety of symptoms that can significantly impact quality of life, with vasomotor symptoms such as hot flashes and night sweats being among the most common and bothersome complaints. Hot flashes are characterized by sudden sensations of intense heat, often accompanied by sweating, flushing, palpitations, and anxiety, and can occur at any time of day or night, disrupting sleep and daily activities. For women with moderate to severe vasomotor symptoms, hormone therapy in the form of estrogen remains the most effective treatment option available. The client in this scenario is 50 years old, postmenopausal, and importantly, has undergone a hysterectomy, which means her uterus has been surgically removed. This surgical history has significant implications for hormone therapy because women with an intact uterus require the addition of progestogen to estrogen therapy to prevent endometrial hyperplasia and cancer, while women without a uterus can take estrogen alone, known as unopposed estrogen therapy. When discussing estrogen therapy with this client, the nurse must provide accurate information about the various formulations available and their respective side effect profiles to help her make an informed decision about her treatment.
A) An estrogen progesterone product will increase side effects
This statement is misleading and does not accurately address the client's specific situation or provide useful information for her decision-making process. For women who have an intact uterus, combination estrogen-progesterone therapy is indeed necessary to prevent the endometrial hyperplasia and endometrial cancer that can result from unopposed estrogen stimulation of the uterine lining. The addition of progesterone to estrogen therapy does introduce its own side effects, which can include breast tenderness, mood changes, headaches, bloating, and resumption of monthly bleeding in women who are perimenopausal or early postmenopausal. However, this client has had a hysterectomy, meaning her uterus has been removed, and therefore she does not require progesterone for endometrial protection. She is a candidate for estrogen-alone therapy, also called unopposed estrogen. The statement about estrogen-progesterone products increasing side effects is irrelevant to her situation because she will not be taking progesterone at all. Furthermore, even if she did need combination therapy, the statement is presented as a definitive fact without context or explanation, and it does not address the client's actual question about the side effects of estrogen therapy specifically. The nurse should provide information that is relevant to this client's unique circumstances rather than general statements that do not apply to her.
B) Transdermal preparations of estrogen therapy have reduced side effects
This statement accurately reflects current understanding of hormone therapy and provides valuable information that can guide the client's decision-making process. Transdermal estrogen preparations, which include patches, gels, sprays, and creams applied to the skin, offer several advantages over oral estrogen in terms of their side effect profile and safety. The key difference lies in how these formulations are metabolized by the body. When estrogen is taken orally, it is absorbed from the gastrointestinal tract and transported via the portal vein to the liver before entering the systemic circulation. This first-pass hepatic metabolism results in several effects that are not seen with transdermal administration. Oral estrogen stimulates the liver to produce increased amounts of various proteins, including clotting factors, which increases the risk of venous thromboembolism. It also increases the production of triglycerides and C-reactive protein, a marker of inflammation associated with cardiovascular risk. The high concentrations of estrogen reaching the liver can also affect bile composition and increase the risk of gallbladder disease. In contrast, transdermal estrogen bypasses this first-pass hepatic metabolism entirely, being absorbed directly into the systemic circulation. This route results in more stable and physiologic blood levels of estrogen without the peaks and troughs associated with oral dosing, and it avoids the hepatic effects that contribute to the increased risks of thromboembolism, gallbladder disease, and hypertension. Clinical studies have consistently demonstrated lower risks of venous thromboembolism with transdermal compared to oral estrogen, making it a preferred option for many women, particularly those with additional risk factors. For a postmenopausal woman who has had a hysterectomy and is seeking relief from moderate to severe hot flashes, transdermal estrogen represents an excellent option that offers efficacy with an improved safety profile and reduced side effects compared to oral formulations.
C) Side effects of estrogen therapy are uncommon among women of her age
This statement is inaccurate and could give the client false reassurance that is not supported by clinical evidence. Side effects of estrogen therapy are not uncommon and can occur in women of any age, including those in the early postmenopausal period. The risks and side effects associated with hormone therapy vary depending on multiple factors including the woman's age, time since menopause onset, type and dose of estrogen used, route of administration, and individual patient characteristics. Women taking estrogen may experience common side effects such as breast tenderness, which can occur in up to 10% to 20% of users, nausea, particularly with oral preparations, headaches, mood changes, and vaginal bleeding patterns in women with an intact uterus. More serious risks are also associated with estrogen therapy and must be discussed as part of informed consent. These include an increased risk of venous thromboembolism, which is higher with oral than transdermal preparations, an increased risk of stroke, particularly in older women, and a possible increased risk of cardiovascular events when hormone therapy is initiated in women who are more than 10 years past menopause onset. The landmark Women's Health Initiative study, which included a large cohort of postmenopausal women, demonstrated that the risks of hormone therapy vary by age and time since menopause, with the lowest risks seen in women who initiate therapy close to menopause onset. However, even in younger postmenopausal women, side effects are not uncommon and must be discussed honestly to allow for informed decision-making. The nurse has an ethical and professional obligation to provide balanced information about both the benefits and the potential risks and side effects of any medication, including estrogen therapy.
D) An intravaginal preparation may be best
This recommendation does not match the client's primary concern and would not address the symptoms she is seeking to treat. Intravaginal estrogen preparations, which include creams, rings, and tablets inserted directly into the vagina, are formulated specifically to treat the genitourinary syndrome of menopause. This condition, previously known as vulvovaginal atrophy, encompasses symptoms related to estrogen deficiency affecting the lower genital and urinary tracts. These symptoms include vaginal dryness, burning, and itching, dyspareunia or pain with intercourse, and urinary symptoms such as urgency, frequency, and recurrent urinary tract infections. Intravaginal estrogen is highly effective for these local symptoms because it delivers estrogen directly to the vaginal tissues, restoring epithelial thickness, increasing blood flow, and improving lubrication and elasticity. However, because the doses used are low and the estrogen is primarily absorbed locally rather than systemically, intravaginal preparations provide minimal systemic estrogen levels and are not effective for treating vasomotor symptoms such as hot flashes and night sweats. Hot flashes are mediated by the effects of estrogen on the thermoregulatory center in the hypothalamus, which requires adequate systemic estrogen levels to modulate. The client in this scenario specifically reports moderate to severe hot flashes as her primary concern, and intravaginal estrogen would do nothing to alleviate these symptoms. While she may also have genitourinary symptoms that could benefit from local therapy, the intravaginal route is not the best recommendation for her stated concern about hot flashes, and systemic estrogen therapy is required for adequate relief of vasomotor symptoms.
Conclusion
When discussing estrogen therapy with a 50-year-old postmenopausal woman who has had a hysterectomy and is experiencing moderate to severe hot flashes, the nurse should explain that transdermal preparations of estrogen have reduced side effects compared to oral formulations. The statement about estrogen-progesterone products increasing side effects is not relevant to this client because she does not require progesterone due to her hysterectomy. The claim that side effects are uncommon among women her age is inaccurate and would not provide truthful information for informed consent. The recommendation of an intravaginal preparation is inappropriate because such formulations are designed for local genitourinary symptoms and will not treat vasomotor symptoms like hot flashes. Therefore, the correct information to provide is that transdermal estrogen offers the efficacy needed for symptom relief while minimizing the risks and side effects associated with oral estrogen, particularly regarding venous thromboembolism, gallbladder disease, and effects on triglycerides and inflammatory markers.
The parents of a child with asthma ask the nurse why their child cannot use oral corticosteroids more often because they are so effective. What is the correct response by the nurse?
A.
Frequent use of this drug may lead to a decreased response
B. Chronic steroid use can slow growth
C. A hypersensitivity reaction to this drug may occur
D. Systemic steroids are more toxic in children
Rationale
The correct response is that chronic steroid use can slow growth, which addresses a major concern specific to the pediatric population and explains why oral corticosteroids are reserved for acute exacerbations rather than used frequently for maintenance therapy.
Asthma is the most common chronic disease of childhood, affecting millions of children worldwide and representing a significant cause of morbidity, healthcare utilization, and school absenteeism. The management of pediatric asthma follows a stepwise approach based on symptom frequency and severity, with the goals of achieving good symptom control, maintaining normal activity levels, and preventing exacerbations. Corticosteroids are among the most effective anti-inflammatory medications available for asthma, working through multiple mechanisms including suppression of inflammatory gene transcription, reduction of cytokine production, decreased eosinophil survival, and inhibition of airway remodeling. However, the route of administration and dosing schedule dramatically affect the risk-benefit ratio of corticosteroid therapy. Inhaled corticosteroids are the mainstay of long-term controller therapy because they deliver medication directly to the airways with minimal systemic absorption, providing anti-inflammatory effects at the site of disease while limiting systemic exposure. Oral corticosteroids, in contrast, are absorbed systemically and distribute throughout the body, producing potent anti-inflammatory effects but also exposing all tissues to the medication. This systemic exposure carries significant risks, particularly in children, that must be balanced against the therapeutic benefits.
A) Frequent use of this drug may lead to a decreased response
This statement is not accurate for corticosteroids and does not reflect the primary concern with frequent oral steroid use in children. Unlike bronchodilators such as beta-2 agonists, which can demonstrate tachyphylaxis or decreased response with frequent use due to downregulation of beta receptors, corticosteroids do not typically lose effectiveness with repeated use. The anti-inflammatory effects of steroids are mediated through genomic and non-genomic mechanisms that remain effective over time. The concern with frequent or chronic corticosteroid use is not that they stop working, but rather that their potent systemic effects accumulate and cause toxicity. The concept of decreased response with frequent use is more applicable to medications like albuterol, where overuse can lead to tolerance and reduced bronchodilator effect. Therefore, this explanation would be incorrect and would not accurately address the parents' question about why oral steroids cannot be used more often.
B) Chronic steroid use can slow growth
This statement is accurate and addresses a major concern specific to the pediatric population that justifies limiting oral corticosteroid use to short courses for acute exacerbations. Growth suppression is a well-documented adverse effect of chronic systemic corticosteroid therapy in children. The mechanisms by which corticosteroids impair growth are multifactorial. They interfere with the secretion of growth hormone from the pituitary gland and reduce the production of insulin-like growth factor-1, a key mediator of growth hormone effects. They also have direct inhibitory effects on bone growth plates, suppressing chondrocyte proliferation and matrix synthesis. Additionally, corticosteroids can affect collagen synthesis and bone mineralization. The degree of growth impairment is related to both the dose and duration of treatment, with higher doses and longer treatment periods causing more significant effects. Studies have shown that even alternate-day oral steroid regimens can result in decreased linear growth velocity. This is why inhaled corticosteroids, which have minimal systemic absorption when used at recommended doses, are preferred for long-term asthma control in children. Oral steroids are reserved for acute exacerbations and used for short courses, typically 3 to 10 days, which minimizes growth suppression while still providing the potent anti-inflammatory effects needed to treat severe exacerbations. Explaining this risk helps parents understand the rationale for limiting oral steroid use and the importance of using inhaled corticosteroids as prescribed for maintenance therapy.
C) A hypersensitivity reaction to this drug may occur
While hypersensitivity reactions to corticosteroids are possible, they are rare and not the primary reason for limiting oral steroid use in children. Allergic reactions can occur with any medication and may manifest as rashes, urticaria, angioedema, or in very rare cases, anaphylaxis. However, these reactions are unpredictable and idiosyncratic, occurring in susceptible individuals regardless of dosing frequency. They do not represent the dose-dependent, predictable toxicity that guides clinical decisions about chronic steroid use. The more significant and predictable risks of systemic corticosteroids are the dose-dependent adverse effects such as growth suppression, adrenal suppression, immunosuppression, osteoporosis, cataracts, glucose intolerance, and Cushing's syndrome. These effects accumulate with prolonged exposure and represent the true rationale for limiting the frequency of oral steroid courses. Focusing on hypersensitivity reactions would not provide the parents with an accurate understanding of why their child cannot use oral steroids more often, as this is not the major concern that guides clinical practice.
D) Systemic steroids are more toxic in children
This statement is overly broad and potentially misleading, and it does not provide the specific information that parents need to understand the rationale for limiting oral steroid use. While children are at risk for specific adverse effects such as growth suppression that do not occur in adults whose growth is complete, the statement that systemic steroids are "more toxic" in children is not entirely accurate. Children and adults experience similar types of corticosteroid toxicity, though the manifestations may differ based on developmental stage. Both children and adults are at risk for adrenal suppression, immunosuppression, weight gain, glucose intolerance, cataracts, and mood changes with chronic steroid use. Adults are at risk for osteoporosis, while children are at risk for growth suppression. The key point is that chronic use carries significant risks in any patient, and these risks must be weighed against benefits. The more specific and accurate response about growth suppression directly addresses a parent's likely concern about their child's development and provides a clear, understandable reason for limiting oral steroid use. A vague statement about increased toxicity does not provide the same level of useful information and may not effectively address the parents' question.
Conclusion
The correct response to parents asking why their child cannot use oral corticosteroids more often is that chronic steroid use can slow growth, which explains a major pediatric-specific concern that justifies limiting systemic steroid exposure. The statement about decreased response with frequent use is not characteristic of corticosteroids. Hypersensitivity reactions are rare and not the primary concern. The statement that systemic steroids are more toxic in children is overly broad and less informative than the specific information about growth suppression. Therefore, the nurse should explain that growth suppression is a significant risk of chronic oral steroid use in children, which is why these medications are reserved for short courses during acute asthma exacerbations rather than used frequently for maintenance therapy.
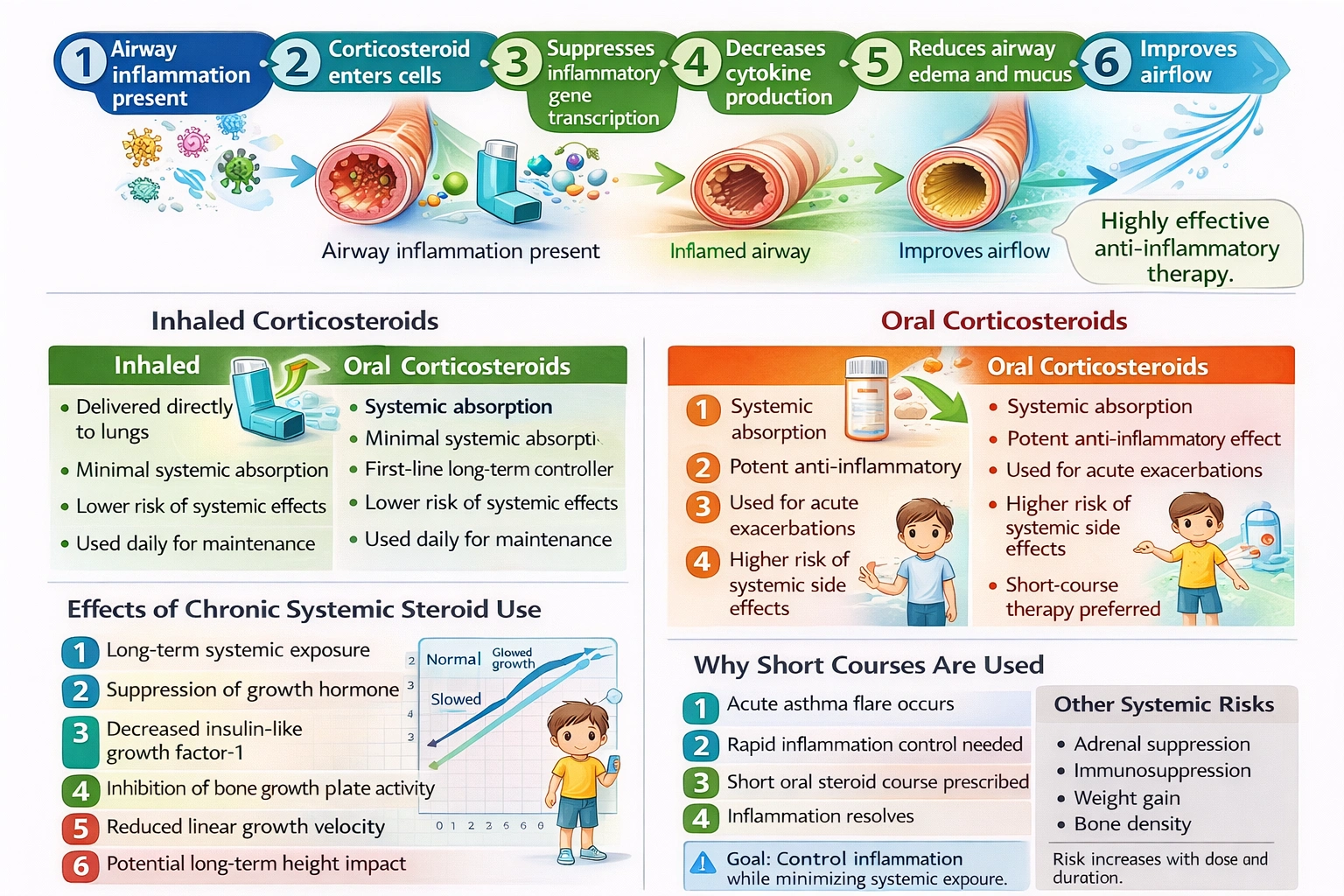
A client who is receiving a final dose of intravenous cephalosporin complains of pain and irritation at the infusion site. The nurse observes signs of redness at the intravenous site. What is the nurse's action?
A.
Apply warm packs to the arm and infuse the medication at a slower rate
B. Immediately stop the infusion and select an alternate intravenous site
C. Request central venous access
D. Continue the infusion while elevating the arm
Rationale
The nurse should immediately stop the infusion and select an alternate intravenous site when a client complains of pain and irritation with redness at the IV site during cephalosporin administration, as these signs indicate phlebitis or infiltration that requires prompt intervention to prevent further tissue damage.
Intravenous therapy is a common and essential component of hospital care, allowing for the administration of medications, fluids, and nutrients directly into the bloodstream. However, intravenous access is not without risks, and complications can arise that require prompt recognition and intervention to prevent patient harm. Phlebitis, which is inflammation of the vein wall, is one of the most common complications of peripheral IV therapy. It can be caused by mechanical irritation from the catheter, chemical irritation from infused medications, or bacterial infection. Chemical phlebitis is particularly common with medications that are irritating to veins, including many antibiotics such as cephalosporins, vancomycin, and certain chemotherapeutic agents. The signs of phlebitis include pain, tenderness, erythema, warmth, and sometimes a palpable venous cord. Infiltration, which is the leakage of fluid into surrounding tissues, can also cause pain and swelling and may occur with or without phlebitis. Both conditions require immediate action to prevent progression and more serious complications.
A) Apply warm packs to the arm and infuse the medication at a slower rate
This response is inadequate and potentially harmful. While warm packs might provide some comfort and could theoretically help with vasodilation and resolution of phlebitis, they do not address the underlying problem of vein irritation from the medication. Continuing the infusion, even at a slower rate, allows further exposure of the already irritated vein to the irritating medication, potentially worsening the phlebitis and leading to more extensive damage. Additionally, if the problem is infiltration rather than simple phlebitis, continuing the infusion would allow more fluid to leak into the tissues, potentially causing tissue damage, compartment syndrome, or necrosis depending on the medication. The priority is to stop the offending infusion, not to modify its rate while hoping the symptoms improve.
B) Immediately stop the infusion and select an alternate intravenous site
This is the correct and appropriate nursing action. Stopping the infusion immediately prevents additional irritation and damage to the current vein and surrounding tissues. This is the first and most important step in managing any IV complication. After stopping the infusion, the nurse should assess the affected site for signs of phlebitis, infiltration, or extravasation, and document the findings. The IV catheter should be removed from the affected site. A new IV site should then be established in a different location, preferably in the opposite arm or in a different vein on the same arm proximal to the affected site if the opposite arm is not available. The medication can then be restarted through the new line after verifying patency. This action prioritizes client safety and prevents further injury while ensuring that the client continues to receive the prescribed medication through a new, healthy site.
C) Request central venous access
Requesting central venous access is premature and not indicated based on the information given. The client is receiving a final dose of cephalosporin, meaning that only one dose remains in the course of therapy. The client has presumably received multiple previous doses through peripheral IV without problems, and a single episode of phlebitis at the end of therapy does not warrant central line placement. Central venous access carries its own risks, including pneumothorax, arterial puncture, infection, and thrombosis, and should only be used when truly indicated, such as for long-term therapy, infusion of highly irritating medications that cannot be given peripherally, or when peripheral access is not feasible. For a single remaining dose, a new peripheral site is the appropriate choice.
D) Continue the infusion while elevating the arm
Continuing the infusion while elevating the arm is unsafe and ignores the signs of vein irritation. Elevation does not prevent phlebitis or tissue damage and does not address the ongoing irritation from the medication. This action could result in worsening of the complication, potentially leading to thrombophlebitis, which is inflammation with clot formation, or extension of tissue damage if infiltration is occurring. The infusion must be stopped, not continued with adjunctive measures.
Conclusion
When a client receiving IV cephalosporin complains of pain and irritation with redness at the site, the nurse should immediately stop the infusion and select an alternate intravenous site to prevent further vein damage and potential tissue injury. Applying warm packs and slowing the infusion does not address the underlying problem and allows continued irritation. Requesting central access is premature for a final dose. Continuing the infusion is unsafe. Therefore, stopping and restarting in a new site is the correct action that prioritizes client safety while ensuring completion of the medication course.
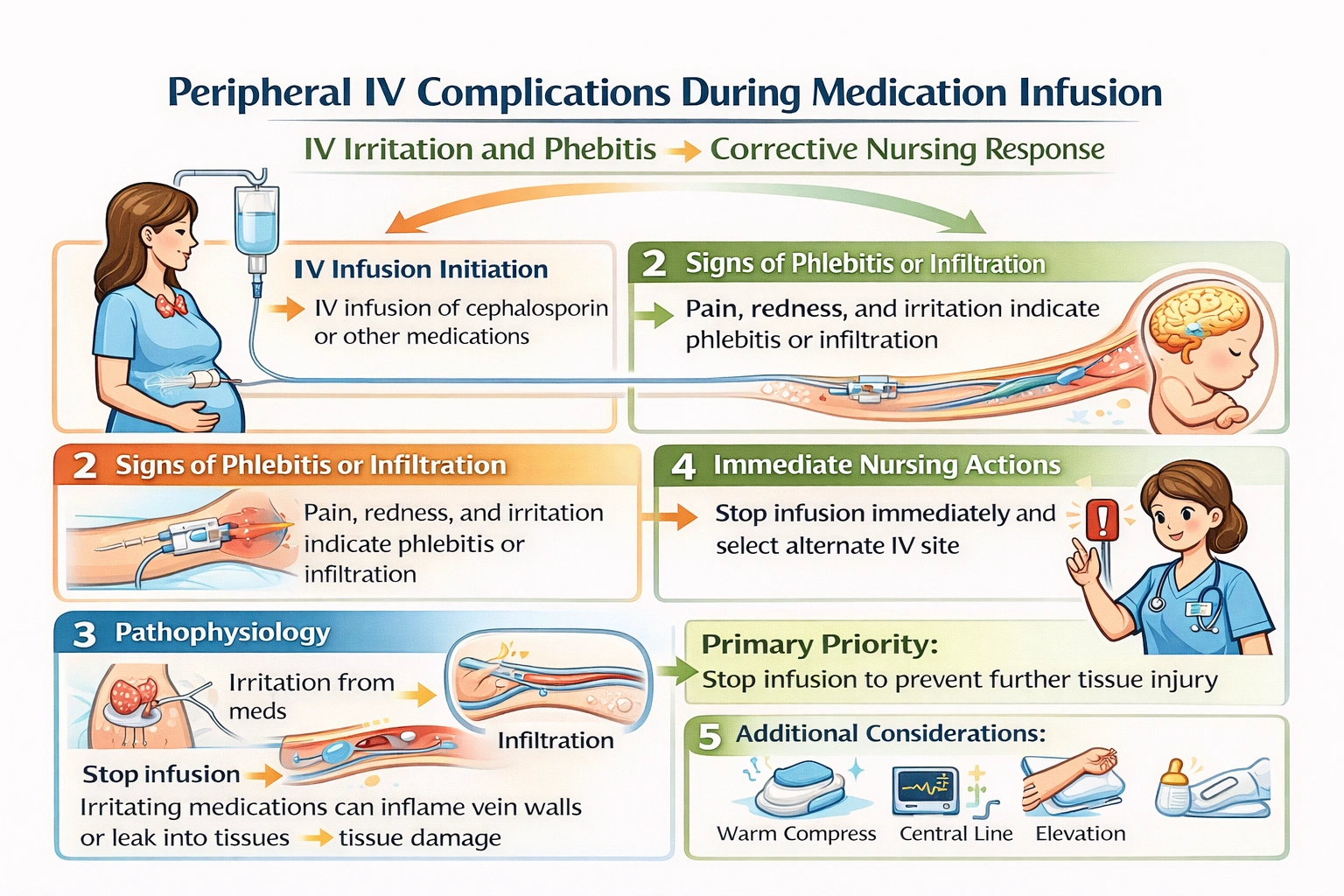
In Which situation would the nurse hold digoxin?
A.
When the client is pacing and very thirsty
B. When the client complains of seeing yellow-green halos
C. When the lab reports a digoxin level 1.2 ng/mL
D. When the client is edematous
Rationale
The nurse would hold digoxin when the client complains of seeing yellow-green halos, as this visual disturbance is a classic sign of digoxin toxicity that requires withholding the next dose and notifying the provider for further evaluation.
Digoxin has a narrow therapeutic index, meaning that the margin between therapeutic and toxic levels is small. Toxicity can occur even at levels within the therapeutic range in some patients, particularly those with electrolyte imbalances such as hypokalemia, hypomagnesemia, or hypercalcemia. Recognizing the early signs of digoxin toxicity is essential for preventing progression to more severe manifestations, which can include life-threatening cardiac arrhythmias. Digoxin toxicity affects multiple organ systems, producing gastrointestinal symptoms such as nausea, vomiting, anorexia, and abdominal pain, neurological symptoms such as headache, confusion, dizziness, and visual disturbances, and cardiac effects including bradycardia, heart block, and various arrhythmias. Visual disturbances are particularly characteristic of digoxin toxicity and include blurred vision, altered color perception, and the classic complaint of seeing yellow-green halos around lights.
A) When the client is pacing and very thirsty
Pacing and thirst are not specific signs of digoxin toxicity. Pacing could indicate anxiety, restlessness, or agitation from various causes, and thirst may indicate dehydration or hyperglycemia. Neither is a classic indication to hold digoxin. The nurse should assess further to determine the cause of these symptoms but would not withhold digoxin based on these findings alone.
B) When the client complains of seeing yellow-green halos
This is a classic sign of digoxin toxicity and requires holding the medication and notifying the provider. Visual disturbances occur due to digoxin's effects on the retina and optic nerve, possibly related to inhibition of the sodium-potassium ATPase in retinal cells. The perception of yellow-green halos around lights is a well-recognized symptom that should prompt immediate evaluation. The nurse should withhold the next dose, assess for other signs of toxicity, check the most recent digoxin level and electrolytes, and report the findings to the provider for further orders, which may include holding additional doses, obtaining a stat digoxin level, and adjusting the regimen.
C) When the lab reports a digoxin level 1.2 ng/mL
A digoxin level of 1.2 ng/mL is within the therapeutic range, which is typically 0.5 to 2.0 ng/mL for heart failure and 0.8 to 2.0 ng/mL for arrhythmias. This level does not indicate toxicity and would not be a reason to hold the medication unless the client also has signs of toxicity despite therapeutic levels. Some patients develop toxicity at levels within the therapeutic range, particularly with electrolyte abnormalities, but the level alone at 1.2 is not concerning.
D) When the client is edematous
Edema is a sign of heart failure, which is an indication for digoxin therapy, not a reason to hold it. Digoxin is used to improve cardiac output and reduce symptoms of heart failure, including edema. Edema would not be a reason to withhold the medication; rather, it suggests that the current regimen may not be adequately controlling the heart failure and may require adjustment of diuretics or other medications, not digoxin discontinuation.
Conclusion
The nurse would hold digoxin when the client reports seeing yellow-green halos, a classic sign of digoxin toxicity that requires immediate evaluation. Pacing and thirst are not toxicity signs. A level of 1.2 ng/mL is therapeutic. Edema is an indication for digoxin. Therefore, visual disturbances warrant holding the medication and notifying the provider to prevent progression to more severe toxicity.
Which of a client's medications is the most likely cause of a persistent, dry cough?
A.
Nifedipine
B. Enalapril
C. Atorvastatin
D. Hydrochlorothiazide
Rationale
Enalapril is the most likely cause of a persistent, dry cough among the medications listed, as angiotensin-converting enzyme inhibitors are well-known for causing this characteristic adverse effect through accumulation of bradykinin and substance P.
Angiotensin-converting enzyme inhibitors are a class of medications widely used for hypertension, heart failure, diabetic nephropathy, and other cardiovascular conditions. They work by inhibiting the enzyme that converts angiotensin I to angiotensin II, a potent vasoconstrictor, thereby reducing blood pressure and improving hemodynamics. However, ACE inhibitors also inhibit the breakdown of other peptides, including bradykinin and substance P. Bradykinin is a vasoactive peptide that causes vasodilation and increased vascular permeability, and it also stimulates sensory nerve endings in the respiratory tract. Accumulation of bradykinin and substance P in the lungs and airways triggers a cough reflex, producing a persistent, dry, non-productive cough that can be bothersome enough to require medication discontinuation. This cough occurs in up to 20% of patients taking ACE inhibitors and can develop anytime from hours to months after starting therapy.
A) Nifedipine
Nifedipine is a calcium channel blocker used for hypertension and angina. Common side effects include peripheral edema, headache, dizziness, flushing, and constipation. Cough is not a typical side effect of calcium channel blockers. Nifedipine does not affect bradykinin metabolism and is not associated with the persistent dry cough characteristic of ACE inhibitors.
B) Enalapril
Enalapril is correctly identified as the most likely cause of persistent dry cough. As an ACE inhibitor, it prevents the breakdown of bradykinin and substance P, leading to accumulation of these peptides in the respiratory tract and stimulation of cough receptors. The cough is typically dry, non-productive, and can be severe enough to interfere with sleep and daily activities. If the cough is bothersome, switching to an angiotensin receptor blocker, which does not affect bradykinin, usually resolves the symptom while maintaining similar cardiovascular benefits.
C) Atorvastatin
Atorvastatin is an HMG-CoA reductase inhibitor, or statin, used for lowering cholesterol. Common side effects include myalgia, muscle weakness, elevated liver enzymes, and rarely, rhabdomyolysis. Cough is not associated with statin use. Atorvastatin does not affect the renin-angiotensin system or bradykinin metabolism and would not cause a persistent dry cough.
D) Hydrochlorothiazide
Hydrochlorothiazide is a thiazide diuretic used for hypertension and edema. Common side effects include electrolyte imbalances, particularly hypokalemia, hyperglycemia, hyperuricemia, and orthostatic hypotension. Cough is not a typical side effect of thiazide diuretics. While rare cases of pulmonary edema or hypersensitivity reactions could cause respiratory symptoms, a persistent dry cough is not characteristic of hydrochlorothiazide.
Conclusion
Enalapril, an ACE inhibitor, is the most likely cause of a persistent, dry cough due to bradykinin and substance P accumulation. Nifedipine, atorvastatin, and hydrochlorothiazide do not typically cause cough and are not associated with this adverse effect. Therefore, enalapril is the correct identification, and if a patient develops this symptom, the provider may consider switching to an ARB to maintain blood pressure control while eliminating the cough.

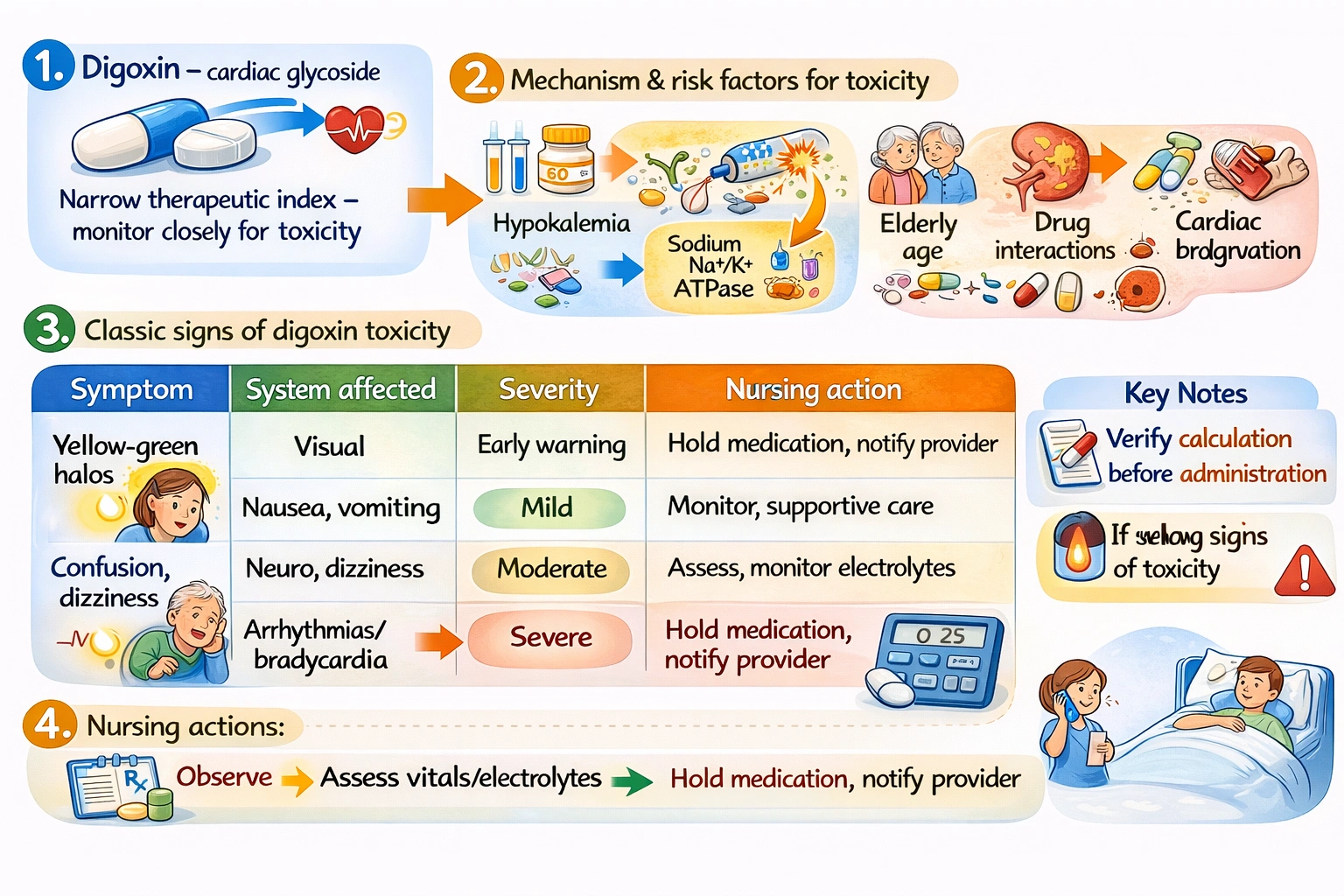
A client with a new diagnosis of atrial fibrillation is receiving a continuous infusion of heparin. Which finding will the nurse report immediately?
A.
The most recent lab results indicate that the client has an international normalized ratio of 0.8
B. The client reports dark, tarry stools
C. The client states that they have been taking acetaminophen for pain
D. The most recent lab results indicate that the client has an aPTT of 60 seconds
Rationale
The nurse will report immediately that the client reports dark, tarry stools, as this finding indicates gastrointestinal bleeding, a potentially serious complication of heparin therapy that requires prompt evaluation and intervention.
Heparin is an anticoagulant used in the acute management of thrombotic conditions, including atrial fibrillation, deep vein thrombosis, and pulmonary embolism. It works by binding to antithrombin III and accelerating its inactivation of thrombin and factor Xa. While effective for preventing and treating clots, heparin significantly increases bleeding risk. Continuous infusion requires monitoring of activated partial thromboplastin time to maintain therapeutic anticoagulation while avoiding excessive levels that increase bleeding risk. Any sign of bleeding in a patient receiving heparin is a potential emergency that requires immediate reporting and intervention.
A) The most recent lab results indicate that the client has an international normalized ratio of 0.8
INR is used to monitor warfarin therapy, not heparin. Heparin is monitored by aPTT. An INR of 0.8 is normal and not relevant to heparin infusion. This does not require reporting.
B) The client reports dark, tarry stools
This finding indicates melena, which is blood in the stool from upper gastrointestinal bleeding. This is a serious complication of anticoagulation that requires immediate reporting. The nurse should stop the heparin infusion, notify the provider, and prepare for interventions such as reversing anticoagulation with protamine sulfate, evaluating the source of bleeding, and providing supportive care. This finding suggests the client may be over-anticoagulated or have an underlying bleeding source.
C) The client states that they have been taking acetaminophen for pain
Acetaminophen is not contraindicated with heparin and does not affect coagulation. This does not require immediate reporting. The nurse may note this information but it is not an emergency.
D) The most recent lab results indicate that the client has an aPTT of 60 seconds
aPTT is the appropriate monitoring test for heparin. The therapeutic range depends on the institution but is typically 1.5 to 2.5 times control, often around 60 to 80 seconds. An aPTT of 60 seconds is likely within or near therapeutic range and does not require immediate reporting unless it is significantly elevated or there are signs of bleeding.
Conclusion
The nurse must immediately report dark, tarry stools as they indicate gastrointestinal bleeding in a client receiving heparin. INR is not relevant to heparin monitoring. Acetaminophen use is not concerning. aPTT of 60 seconds may be therapeutic. Therefore, melena requires immediate reporting and intervention to prevent further blood loss and complications.
A client is starting to take furosemide and asks the nurse, \When is the best time to take this medication?\" What is the nurse's response?"""
A.
1600
B. 800
C. 2200
D. 1900
Rationale
The nurse should respond that the best time to take furosemide is 0800, as morning dosing aligns the peak diuretic effect with waking hours, minimizing sleep disruption from nocturia and reducing fall risk.
Furosemide is a loop diuretic that works by inhibiting the sodium-potassium-chloride cotransporter in the thick ascending limb of the loop of Henle. This inhibition prevents the reabsorption of sodium, chloride, and potassium, leading to increased excretion of these electrolytes along with water. The result is a significant increase in urine output that begins within 30 to 60 minutes of oral administration, peaks at 1 to 2 hours, and lasts for approximately 6 to 8 hours. The timing of furosemide administration has important implications for patient comfort, adherence, and safety. If taken later in the day, the peak diuretic effect will occur during evening or nighttime hours, causing the patient to wake repeatedly to urinate. This sleep disruption can lead to daytime fatigue, decreased quality of life, and increased risk of falls if the patient gets up in the dark. Additionally, nocturia in elderly patients is associated with increased risk of falls and fractures, which can have serious consequences.
A) 1600
4 PM is too late for furosemide administration. The peak diuretic effect would occur in the early evening, and the duration would extend into the nighttime hours. This would likely cause the patient to experience nocturia, disrupting sleep and increasing fall risk. Evening dosing is not recommended for diuretics.
B) 0800
8 AM is the optimal time for furosemide administration. Taking it with or after breakfast ensures that the peak diuretic effect occurs during the morning and early afternoon when the patient is awake, active, and near a bathroom. By the time the patient goes to bed, the diuretic effect has largely subsided, allowing for uninterrupted sleep. This timing maximizes therapeutic benefit while minimizing disruption to daily activities and sleep.
C) 2200
10 PM is the worst possible time for furosemide administration. The peak effect would occur around midnight, and the patient would be up multiple times during the night to urinate. This would severely disrupt sleep and significantly increase fall risk, particularly in elderly patients who may need to navigate to the bathroom in the dark. Bedtime dosing of diuretics is contraindicated.
D) 1900
7 PM is also too late. The peak effect would occur around 8 to 9 PM, and the diuretic effect would continue into the nighttime hours. While slightly better than bedtime dosing, it would still likely cause nocturia and sleep disruption. Afternoon and evening dosing should be avoided for diuretics.
Conclusion
The best time to take furosemide is in the morning at 0800 to align diuretic effect with waking hours and prevent sleep disruption and fall risk. Afternoon, bedtime, and evening dosing are all incorrect. Therefore, 0800 is correct, and the nurse should instruct the client to take it at that time daily.

Which is a common side effect caused by atenolol?
A.
Memory loss
B. Bradycardia
C. Neuropathy
D. Hyperglycemia
Rationale
A common side effect caused by atenolol is bradycardia, as beta-blockers work by blocking the effects of catecholamines on the heart, reducing heart rate through their primary mechanism of action.
Atenolol is a beta-1 selective adrenergic antagonist, commonly referred to as a beta-blocker, used in the management of hypertension, angina pectoris, post-myocardial infarction, and certain arrhythmias. It works by competitively blocking the effects of catecholamines such as epinephrine and norepinephrine at beta-adrenergic receptors. Atenolol is cardioselective, meaning it has greater affinity for beta-1 receptors, which are predominantly located in the heart, than for beta-2 receptors, which are found in bronchial and vascular smooth muscle. In the heart, beta-1 receptor blockade decreases sinoatrial node automaticity, slowing heart rate, decreases atrioventricular node conduction velocity, and reduces myocardial contractility. These effects are therapeutic for conditions like hypertension and angina, but they also produce predictable side effects. Bradycardia, or a heart rate slower than 60 beats per minute, is a common and expected consequence of beta-blockade. While mild bradycardia may be asymptomatic and even therapeutic, excessive bradycardia can cause symptoms such as dizziness, fatigue, and syncope, and may require dose adjustment.
A) Memory loss
Memory loss is not a common side effect of atenolol. Beta-blockers can cause central nervous system effects such as fatigue, dizziness, and sleep disturbances, but memory loss is not typically associated with atenolol. Some patients report cognitive slowing, but significant memory impairment is not characteristic of this medication.
B) Bradycardia
Bradycardia is a common and expected side effect of atenolol due to its beta-blocking action on the sinoatrial and atrioventricular nodes. The degree of bradycardia is dose-dependent, and patients should be advised to monitor their heart rate and report if it becomes excessively slow, particularly if accompanied by symptoms.
C) Neuropathy
Peripheral neuropathy is not associated with atenolol use. Neuropathy, characterized by numbness, tingling, or pain in the extremities, is not a typical adverse effect of beta-blockers and would not be expected with atenolol therapy.
D) Hyperglycemia
Atenolol does not typically cause hyperglycemia. Beta-blockers can mask the symptoms of hypoglycemia, such as tachycardia, which is an important consideration in diabetic patients, but they do not significantly raise blood glucose levels. Some non-selective beta-blockers may have minor effects on glucose metabolism, but hyperglycemia is not a common side effect of atenolol.
Conclusion
Bradycardia is a common side effect of atenolol due to its beta-blocking action on the heart. Memory loss, neuropathy, and hyperglycemia are not typical. Therefore, bradycardia is correct, and the nurse should monitor heart rate and educate the client about this expected effect.
A Client who is taking warfarin has started on cephalexin. What are the nursing implications of this medication change?
A.
The provider should be asked to consider increasing the client's dose of cephalexin
B. The provider should be reminded to recheck the client's international normalized ratio
C. The client should not be allowed to eat leafy greens in excess
D. The client should be assessed for bruising
Rationale
The nursing implications when a client on warfarin starts cephalexin include reminding the provider to recheck the INR, advising the client to maintain consistent intake of leafy greens rather than eating them in excess, and assessing the client for signs of bleeding such as bruising, as antibiotics can affect INR and increase bleeding risk.
Warfarin is an oral anticoagulant with a narrow therapeutic index that is highly susceptible to interactions with other medications, including antibiotics. Cephalexin is a first-generation cephalosporin antibiotic commonly used for various infections. When a patient on stable warfarin therapy starts cephalexin, several mechanisms can alter the anticoagulant effect. Antibiotics can kill gut flora that produce vitamin K, reducing the availability of this vitamin and potentiating warfarin's effect. Some antibiotics may also directly affect warfarin metabolism or protein binding. The net effect is often an increase in INR and increased bleeding risk. Therefore, close monitoring is essential when any antibiotic is added to warfarin therapy.
A) The provider should be asked to consider increasing the client's dose of cephalexin
Cephalexin dose does not need adjustment based on warfarin therapy. The antibiotic is dosed based on the type and severity of infection, renal function, and other factors, not on concurrent warfarin use. This is not an appropriate nursing implication.
B) The provider should be reminded to recheck the client's international normalized ratio
This is correct. The INR should be rechecked within a few days of starting cephalexin to detect any change in anticoagulation status. The frequency of monitoring may need to be increased until the INR stabilizes. The nurse should ensure that this monitoring occurs.
C) The client should not be allowed to eat leafy greens in excess
This is correct in terms of maintaining consistent vitamin K intake. Leafy greens are high in vitamin K, which antagonizes warfarin's effect. Large variations in intake can cause INR fluctuations. The client should be advised to maintain a consistent intake, not to avoid greens entirely, but to avoid suddenly increasing or decreasing consumption. The wording "not allowed to eat in excess" is appropriate as it discourages large variations.
D) The client should be assessed for bruising
This is correct. Assessing for signs of bleeding, including easy bruising, bleeding gums, nosebleeds, dark tarry stools, and pink urine, is essential when INR may increase. Early detection allows prompt intervention.
E) The provider should be asked to consider increasing the client's dose of warfarin
Increasing warfarin without evidence would be dangerous. If INR increases, the dose may need reduction, not increase. If INR decreases, an increase might be considered, but this would be based on monitoring, not assumed. This is not an appropriate implication without INR results.
Conclusion
When a client on warfarin starts cephalexin, nursing implications include rechecking INR, maintaining consistent vitamin K intake, and assessing for bleeding. Increasing cephalexin or warfarin doses is not indicated. Therefore, B, C, and D are correct, reflecting appropriate monitoring and assessment for this potential drug interaction.

When administering medications to infants, it is essential to remember which of the following?
A.
Oral medications are contraindicated in infants
B. Infants are more sensitive to medications that act on the CNS
C. Immaturity of renal function in infancy causes infants to excrete drugs less efficiently
D. Infants have immature livers, which slows drug metabolism
Rationale
When administering medications to infants, it is essential to remember that infants are more sensitive to CNS medications, have immature renal function causing inefficient drug excretion, have immature livers slowing drug metabolism, and breastfed infants are more likely to develop toxicity from lipid-soluble drugs, all of which reflect the unique physiological characteristics of this vulnerable population.
Medication administration to infants requires specialized knowledge and extreme caution due to the profound physiological differences between infants and older children or adults. The infant's body is undergoing rapid development and maturation, and all organ systems involved in drug handling are immature to varying degrees. These differences affect every phase of pharmacokinetics: absorption, distribution, metabolism, and excretion. Additionally, pharmacodynamics, or the relationship between drug concentration and effect, may differ due to developing receptor systems and immature regulatory mechanisms. Understanding these differences is essential for nurses to ensure safe and effective medication administration, to anticipate potential adverse effects, and to recognize early signs of toxicity. The unique characteristics of infants require careful medication selection, precise weight-based dosing, and vigilant monitoring for both therapeutic and adverse effects.
A) Oral medications are contraindicated in infants
This statement is false and should not be remembered as a principle of infant medication administration. Oral medications are commonly administered to infants and are not contraindicated. Many medications are formulated specifically for infants as liquids, suspensions, or easily dissolvable tablets to facilitate oral administration. While there are considerations for oral medication administration in infants, such as the need for accurate measurement of small volumes, assessment of the infant's ability to swallow, and potential for regurgitation or spitting up, oral medications are a standard and appropriate route for many conditions. Absorption may differ from adults due to gastrointestinal immaturity, including slower gastric emptying, variable intestinal pH, and reduced bile acid secretion, but this does not contraindicate oral administration. The nurse should be aware of these differences but should not believe that oral medications are contraindicated.
B) Infants are more sensitive to medications that act on the CNS
This is correct and essential to remember. The infant's central nervous system is uniquely vulnerable to medication effects for several reasons. The blood-brain barrier, which in adults restricts the passage of many substances from the bloodstream into the brain, is immature and more permeable in infants. This allows greater penetration of drugs into the central nervous system, potentially leading to higher brain concentrations than would occur in adults receiving equivalent doses. Additionally, receptor systems in the infant brain are developing and may show enhanced or altered sensitivity to medications. Myelination, which insulates nerve fibers and affects nerve conduction, is incomplete. The combination of increased drug penetration and developing neural circuits means that CNS-active medications can produce exaggerated effects, including respiratory depression, profound sedation, paradoxical excitation, and seizures. This increased sensitivity requires cautious dosing and close monitoring whenever CNS-active medications are used in infants.
C) Immaturity of renal function in infancy causes infants to excrete drugs less efficiently
This is correct and a critical consideration for medication safety in infants. Renal function is immature at birth and develops progressively over the first months to years of life. Glomerular filtration rate is low in term newborns, approximately 30% to 40% of adult values when corrected for body surface area. Tubular secretion and reabsorption mechanisms are also immature. This means that drugs eliminated primarily by renal excretion will have prolonged half-lives and will accumulate to higher levels if dosed based on adult intervals. The maturation of renal function follows a predictable pattern, with GFR reaching adult levels by approximately one to two years of age. Premature infants have even more pronounced renal immaturity. For medications such as aminoglycoside antibiotics, digoxin, and many others that are renally eliminated, dosing intervals must be extended, and drug levels must be monitored to prevent toxicity. The nurse must be aware of which medications are renally eliminated and ensure appropriate monitoring.
D) Infants have immature livers, which slows drug metabolism
This is correct and fundamental to understanding medication dosing in infants. Hepatic drug metabolism is mediated by a variety of enzymes, particularly the cytochrome P450 family, which catalyze phase I reactions such as oxidation, reduction, and hydrolysis. These enzymes have reduced activity at birth and mature at different rates over the first months to years of life. Phase II conjugation reactions, such as glucuronidation, are also immature, with particularly low activity of UDP-glucuronosyltransferase, the enzyme responsible for glucuronide conjugation. This immaturity affects drugs metabolized by these pathways, including many commonly used medications such as acetaminophen, morphine, and caffeine. Slower metabolism leads to prolonged drug half-lives and higher drug concentrations for a given dose. The rate of maturation varies among enzymes, making drug metabolism in early infancy somewhat unpredictable and requiring careful dose individualization. The nurse should anticipate that hepatically metabolized drugs may require reduced doses or extended dosing intervals in infants.
E) Breastfeeding infants are more likely to develop toxicity when given lipid-soluble drugs
This is correct and highlights an important consideration for medications administered directly to breastfed infants or for medications taken by breastfeeding mothers that may reach the infant through milk. Lipid-soluble drugs have properties that make them more likely to distribute into breast milk, which has a higher fat content than plasma. These drugs can accumulate in the milk and be ingested by the infant with each feeding. Once ingested, the infant's immature metabolism and excretion mean that the drug will be cleared slowly, leading to accumulation and potential toxicity. Additionally, lipid-soluble drugs may have large volumes of distribution and may accumulate in the infant's adipose tissue, which constitutes a higher percentage of body weight than in older children and adults. This combination of factors makes breastfed infants particularly vulnerable to toxicity from lipid-soluble drugs, whether administered directly or acquired through breast milk. The nurse must consider this when administering lipid-soluble medications to breastfed infants or when counseling breastfeeding mothers about medication use.
Conclusion
When administering medications to infants, essential considerations include increased CNS sensitivity due to immature blood-brain barrier and developing neural systems, immature renal function causing inefficient drug excretion, immature hepatic function slowing drug metabolism, and increased toxicity risk from lipid-soluble drugs in breastfed infants due to distribution into milk and accumulation in the infant. Oral medications are not contraindicated and are commonly used. Therefore, the correct factors to remember are B, C, D, and E, reflecting the unique physiological characteristics that make medication administration in infants a complex and high-risk activity requiring specialized knowledge and careful monitoring.
The nurse will caution a client taking immunosuppressant drugs to avoid which dietary supplement?
A.
Glucosamine
B. Feverfew
C. Echinacea
D. Black cohosh
Rationale
The nurse will caution a client taking immunosuppressant drugs to avoid echinacea, as this herbal supplement has immunostimulant properties that can theoretically counteract the effects of immunosuppressive therapy and potentially lead to treatment failure.
Immunosuppressant medications are used in a variety of clinical situations where suppression of the immune system is desired. These include prevention of organ rejection in transplant recipients, treatment of autoimmune diseases such as rheumatoid arthritis, lupus, and inflammatory bowel disease, and management of certain hematologic and oncologic conditions. The goal of immunosuppressive therapy is to dampen immune responses that are inappropriately targeting the body's own tissues or foreign but desired grafts. Medications in this class include calcineurin inhibitors such as tacrolimus and cyclosporine, antiproliferative agents such as mycophenolate and azathioprine, mTOR inhibitors such as sirolimus, and corticosteroids among others. Patients taking these medications must be extremely cautious about any additional substances they introduce into their bodies, including over-the-counter products and herbal supplements, because many of these can interact with immunosuppressants or have independent effects on immune function that could undermine therapy. The growing popularity of herbal supplements, many of which are marketed as natural and therefore assumed to be safe, creates significant potential for harmful interactions that patients may not anticipate.
A) Glucosamine
Glucosamine is a dietary supplement commonly used for osteoarthritis, based on the theory that it provides building blocks for cartilage synthesis and may have mild anti-inflammatory effects. It is one of the most widely used supplements among older adults for joint health. Glucosamine does not have significant immunostimulant properties and is generally not considered contraindicated with immunosuppressant drugs. While patients should always consult their healthcare provider before taking any supplement, glucosamine is not known to counteract immunosuppression. The main concerns with glucosamine involve its potential effects on blood glucose levels, as some studies have suggested it may impair insulin sensitivity, and possible interactions with anticoagulants due to mild antiplatelet effects. However, it is not the supplement the nurse would specifically caution about in relation to immunosuppressant drugs.
B) Feverfew
Feverfew is an herbal supplement derived from the Tanacetum parthenium plant and has been used primarily for the prevention and treatment of migraines. Its mechanism is thought to involve inhibition of platelet aggregation and serotonin release, as well as anti-inflammatory effects through inhibition of prostaglandin synthesis. While feverfew does have some biological activity, its primary concern in patients taking other medications involves its antiplatelet effects, which can increase bleeding risk when combined with anticoagulants or antiplatelet agents. Feverfew is not known for significant immunostimulant properties and would not directly counteract immunosuppression. Therefore, while patients on immunosuppressants should use caution with any supplement and discuss all products with their provider, feverfew is not the specific supplement that requires special caution regarding immune stimulation.
C) Echinacea
Echinacea is the supplement that requires specific caution in clients taking immunosuppressant drugs due to its well-documented immunostimulant properties. Echinacea is derived from plants in the genus Echinacea, most commonly Echinacea purpurea, Echinacea angustifolia, and Echinacea pallida, and has been used for centuries in traditional medicine, particularly for preventing and treating upper respiratory infections. The purported mechanism of echinacea involves stimulation of the immune system through multiple pathways. Research has shown that echinacea can activate macrophages, which are immune cells that engulf and destroy pathogens, increase the production of cytokines such as tumor necrosis factor-alpha, interleukins, and interferons, which are signaling molecules that coordinate immune responses, and enhance the activity of natural killer cells and T-lymphocytes, which are critical for cell-mediated immunity. These immunostimulant effects directly oppose the mechanism of immunosuppressant medications, which are designed to dampen immune responses. In a transplant recipient, echinacea could theoretically trigger immune activation that might lead to rejection of the transplanted organ. In a patient with autoimmune disease, echinacea could potentially exacerbate the underlying condition by activating the very immune responses that the immunosuppressants are intended to suppress. For these reasons, patients taking immunosuppressants should be strongly cautioned against using echinacea, and the nurse must include this warning in client education.
D) Black cohosh
Black cohosh is an herbal supplement derived from the Actaea racemosa plant and is used primarily for menopausal symptoms such as hot flashes, night sweats, and mood disturbances. It is believed to have estrogenic effects or to influence serotonin receptors, though its exact mechanism remains unclear. Black cohosh does not have significant immunostimulant properties and is not known to interact with immunosuppressant medications. The primary concerns with black cohosh involve potential hepatotoxicity, as there have been rare case reports of liver injury associated with its use, and possible interactions with other medications metabolized by the liver. However, it is not the supplement that would specifically counteract immunosuppression, and it is not the one the nurse would caution about in relation to immunosuppressant drugs.
Conclusion
The nurse will caution a client taking immunosuppressant drugs to avoid echinacea due to its immunostimulant properties that can activate macrophages, increase cytokine production, and enhance T-cell activity, all of which directly oppose the effects of immunosuppressive therapy. Glucosamine, feverfew, and black cohosh do not have significant immunostimulant effects and are not specifically contraindicated with immunosuppressants, though patients should always consult their provider before taking any supplement. Therefore, echinacea is the correct supplement to avoid for clients on immunosuppressant therapy to prevent potential treatment failure, whether that be organ rejection in transplant recipients or disease flare in patients with autoimmune conditions.
A nurse is talking to the client who wants to stop taking glucocorticoids after taking them for 3 months. Which statement by the client indicates a good understanding of the teaching about withdrawal?
A.
Once I am off of the steroids, I should never take them again
B. I should monitor for Cushing's symptoms during the withdrawal process
C. I should not try to taper off the medication without consulting my provider
D. I should reduce the dose by half each day until I am at 5mg, then I can stop the medication
Rationale
The client demonstrates understanding of glucocorticoid withdrawal teaching by stating that they should not try to taper off the medication without consulting their provider, recognizing that withdrawal from chronic steroid therapy requires medical supervision to prevent adrenal insufficiency.
Glucocorticoids are powerful hormones with diverse effects throughout the body, and their therapeutic use for three months or longer has significant physiological consequences. One of the most important of these consequences is suppression of the hypothalamic-pituitary-adrenal axis. Under normal conditions, the hypothalamus secretes corticotropin-releasing hormone, which stimulates the pituitary to release adrenocorticotropic hormone, which in turn stimulates the adrenal cortex to produce cortisol. Cortisol is essential for life, helping to maintain blood glucose levels, blood pressure, and the body's response to stress. When exogenous glucocorticoids are administered, they provide negative feedback to the hypothalamus and pituitary, reducing the secretion of CRH and ACTH. Over time, this leads to atrophy of the adrenal cortex and loss of the ability to produce endogenous cortisol. The degree of suppression depends on the dose, duration, and potency of the glucocorticoid used. After three months of therapy, significant suppression is likely. Abrupt discontinuation or too-rapid tapering can precipitate acute adrenal insufficiency, a life-threatening condition characterized by hypotension, shock, nausea, vomiting, weakness, and electrolyte imbalances.
A) Once I am off of the steroids, I should never take them again
This statement does not demonstrate understanding of appropriate glucocorticoid use. There is no indication that glucocorticoids can never be used again after a course of therapy. Future use depends on the medical condition and may be appropriate if the same or a different condition arises that requires steroid treatment. The issue is safe withdrawal from the current course, not permanent prohibition. This statement suggests misunderstanding and could lead the client to refuse necessary future steroid therapy.
B) I should monitor for Cushing's symptoms during the withdrawal process
This statement reflects misunderstanding of what to monitor during withdrawal. Cushing's symptoms, such as moon face, buffalo hump, central obesity, and striae, are caused by excess glucocorticoids. During withdrawal, as steroid doses decrease, Cushing's symptoms should improve, not worsen. The client should monitor for signs of adrenal insufficiency during withdrawal, including fatigue, weakness, nausea, vomiting, abdominal pain, dizziness, and hypotension. This statement indicates confusion between the signs of excess and the signs of deficiency, and the client needs further teaching about what symptoms actually warrant concern during withdrawal.
C) I should not try to taper off the medication without consulting my provider
This statement correctly reflects understanding of the need for medical supervision during glucocorticoid withdrawal. Tapering glucocorticoids requires a gradual reduction in dose over weeks to months, allowing the suppressed HPA axis to recover and resume endogenous cortisol production. The appropriate tapering schedule depends on the specific drug, dose, duration of therapy, and individual patient factors. The provider determines the schedule based on these factors and may adjust it based on the patient's response. The client who recognizes that self-tapering is dangerous and that provider consultation is necessary demonstrates appropriate understanding of this critical safety principle.
D) I should reduce the dose by half each day until I am at 5mg, then I can stop the medication
This statement describes a specific tapering regimen that the client should not implement independently. Halving the dose daily is likely too rapid and could precipitate adrenal insufficiency. Tapering schedules are typically more gradual, with dose reductions occurring over weeks, not days, particularly after three months of therapy. The client should not determine their own tapering schedule, and this statement indicates lack of understanding that the provider must prescribe the taper and that self-management is dangerous.
Conclusion
The client demonstrates understanding of glucocorticoid withdrawal by stating that they should not try to taper off the medication without consulting their provider, recognizing that medical supervision is essential to prevent adrenal insufficiency. The statements about never taking steroids again, monitoring for Cushing's symptoms, and self-tapering with a specific schedule all indicate misunderstanding. Therefore, consulting the provider before tapering is the correct understanding, reflecting awareness that glucocorticoid withdrawal requires gradual reduction under medical supervision to allow recovery of the HPA axis.
A person with type 2 diabetes is starting metformin therapy. Which comment by the client indicates a need for further teaching?
A.
This medication may be hard on my kidneys. I should take it with plenty of water
B. I should not take metformin on the day I have contrast dye or on the two days after the dye study
C. This medication makes my pancreas put out more insulin
D. This medication may bother my stomach
Rationale
The client needs further teaching when stating that metformin makes the pancreas put out more insulin, as this reflects confusion between metformin and other classes of diabetes medications, and demonstrates misunderstanding of metformin's actual mechanism of action.
Metformin is a biguanide medication that is widely considered the first-line pharmacologic therapy for type 2 diabetes mellitus. It has been used for decades and has an excellent safety profile, low cost, and potential cardiovascular benefits. Understanding how metformin works is important for patients to have realistic expectations about its effects and to understand why it is used. Metformin's primary mechanism of action is reduction of hepatic glucose production through inhibition of gluconeogenesis. It also improves peripheral insulin sensitivity, increasing glucose uptake in muscle and adipose tissue, and may have minor effects on intestinal glucose absorption. Importantly, metformin does NOT stimulate insulin secretion from pancreatic beta cells. This distinguishes it from sulfonylureas and meglitinides, which do increase insulin release and carry a risk of hypoglycemia.
A) This medication may be hard on my kidneys. I should take it with plenty of water
This statement shows partial understanding but requires clarification. Metformin is not nephrotoxic; it does not damage the kidneys. However, it is eliminated renally, meaning that it is excreted by the kidneys. If renal function is impaired, metformin can accumulate and increase the risk of lactic acidosis, a rare but serious complication. Adequate hydration is generally good advice but not specific to metformin's mechanism. The statement is not entirely accurate but does not represent a critical misunderstanding.
B) I should not take metformin on the day I have contrast dye or on the two days after the dye study
This statement shows understanding of an important safety precaution. Intravenous contrast dye used for imaging studies can cause acute kidney injury, particularly in patients with diabetes or pre-existing renal impairment. If kidney injury occurs, metformin elimination would be impaired, increasing lactic acidosis risk. The standard recommendation is to hold metformin on the day of contrast study and for 48 hours afterward, resuming only after renal function is confirmed normal. This demonstrates appropriate knowledge.
C) This medication makes my pancreas put out more insulin
This statement indicates need for further teaching. Metformin does not stimulate insulin secretion; it works through other mechanisms including reducing hepatic glucose output and increasing peripheral insulin sensitivity. The client confuses metformin with insulin secretagogues such as sulfonylureas. This misunderstanding could lead to incorrect expectations about how the medication works and about the risk of hypoglycemia. Metformin alone does not typically cause hypoglycemia because it does not increase insulin levels. The nurse should correct this misconception.
D) This medication may bother my stomach
This statement shows understanding. Gastrointestinal side effects are common with metformin, particularly when starting therapy or with dose increases. These effects include nausea, diarrhea, abdominal discomfort, and loss of appetite. Taking with food and gradual dose titration can minimize these effects. This demonstrates appropriate knowledge of expected side effects.
Conclusion
The client needs further teaching when stating that metformin makes the pancreas put out more insulin, as metformin does not stimulate insulin secretion. The statements about kidney effects, contrast dye precautions, and stomach upset all show appropriate understanding, though the kidney statement could be refined. Therefore, the incorrect statement is about metformin's mechanism of action, and the nurse should provide education about how metformin actually works to lower blood glucose through effects on the liver and peripheral tissues, not through insulin stimulation.

What should the nurse include in discharge teaching regarding self-care for a client taking loop or thiazide diuretics?
A.
Take the medication after supper to avoid mid-day urgency
B. Walk at least a mile a day
C. Weigh daily and report any loss or gain exceeding two pounds in 24 hours to your provider
D. Avoid fruits and potatoes
Rationale
The nurse should include in discharge teaching that the client should weigh daily and report any loss or gain exceeding two pounds in 24 hours to the provider, as daily weight measurement is the most reliable indicator of fluid status in clients taking diuretics.
Loop diuretics such as furosemide and thiazide diuretics such as hydrochlorothiazide are commonly prescribed for conditions involving fluid overload, including hypertension, heart failure, and renal disease. These medications work by increasing urine output, reducing plasma volume, and decreasing blood pressure. Monitoring fluid status is essential for evaluating the effectiveness of diuretic therapy and for detecting complications such as excessive diuresis leading to dehydration or inadequate diuresis leading to fluid retention. Daily weight measurement is the most sensitive and reliable method for assessing fluid balance in the outpatient setting because it reflects changes in total body water.
A) Take the medication after supper to avoid mid-day urgency
This instruction is incorrect. Diuretics are usually taken in the morning to avoid nocturia and sleep disruption. Taking them after supper would cause the peak diuretic effect to occur during the night, leading to frequent awakenings to urinate, disturbed sleep, and increased fall risk if the client gets up in the dark. Morning dosing is standard.
B) Walk at least a mile a day
While exercise is generally beneficial for cardiovascular health, it is not specific to diuretic therapy and is not the priority discharge teaching for clients taking these medications. The client should be encouraged to exercise as tolerated, but this is not the essential teaching point related to medication safety.
C) Weigh daily and report any loss or gain exceeding two pounds in 24 hours to your provider
This is the correct and essential teaching. Daily weights should be measured at the same time each day, on the same scale, with similar clothing, and after voiding but before eating. A gain of more than 2 pounds in 24 hours or 5 pounds in a week may indicate fluid retention and worsening heart failure, requiring medication adjustment. A loss of more than 2 pounds in 24 hours may indicate excessive diuresis and dehydration. This self-monitoring allows early detection of problems and timely intervention.
D) Avoid fruits and potatoes
This instruction is incorrect and potentially harmful. Clients taking loop and thiazide diuretics may lose potassium in the urine and need to consume potassium-rich foods such as fruits and potatoes to prevent hypokalemia. Avoiding these foods could lead to potassium depletion. Some potassium-sparing diuretics require potassium restriction, but this is not true for loop and thiazide diuretics.
Conclusion
For clients taking loop or thiazide diuretics, discharge teaching must include daily weight monitoring and reporting significant changes, as this is the most reliable indicator of fluid status. Taking medication after supper is incorrect timing. Walking is not the priority teaching. Avoiding fruits and potatoes is harmful as these provide potassium. Therefore, daily weight monitoring is the correct instruction that empowers the client to participate in managing their condition and detecting problems early.

Which statement indicates an asthmatic client understands discharge teaching regarding a leukotriene blocker?
A.
This medication could cause me to develop a thrush infection
B. I should take this medication whenever I suddenly have difficulty breathing
C. This medication is taken once daily for the prevention of asthma
D. I should expect this medication will make me agitated, but I don't need to report that effect
Rationale
The client demonstrates understanding by stating that a leukotriene blocker is taken once daily for the prevention of asthma, accurately reflecting that this medication is a controller used for long-term management rather than for acute symptom relief.
Asthma is a chronic inflammatory disease of the airways characterized by variable airflow obstruction, bronchial hyperresponsiveness, and respiratory symptoms including wheezing, shortness of breath, chest tightness, and cough. The management of asthma involves two distinct categories of medications: controllers, which are taken regularly to maintain control and prevent exacerbations, and relievers, which are used as needed for acute symptom relief. Leukotriene receptor antagonists, such as montelukast, belong to the controller category. They work by blocking the action of leukotrienes, which are inflammatory mediators released from mast cells, eosinophils, and other cells involved in the asthmatic response. Leukotrienes cause bronchoconstriction, increased mucus production, and airway edema, contributing to both the chronic inflammation and acute symptoms of asthma. By blocking leukotriene receptors, these medications reduce airway inflammation, decrease bronchial hyperresponsiveness, and help prevent asthma symptoms and exacerbations over time. They are not effective for acute bronchospasm because they do not relax already constricted airways, and their onset of action is too slow for acute relief. Understanding this distinction between controller and reliever medications is essential for proper asthma self-management.
A) This medication could cause me to develop a thrush infection
This statement reflects confusion between different classes of asthma medications and indicates misunderstanding of leukotriene blockers. Thrush, or oropharyngeal candidiasis, is a fungal infection of the mouth and throat that occurs as a local side effect of inhaled corticosteroids. When inhaled steroids are used, medication can deposit in the oropharynx and suppress local immunity, allowing Candida organisms to overgrow. This is why patients using inhaled corticosteroids are instructed to rinse their mouth with water after each use and spit it out. Leukotriene blockers are taken orally as tablets or granules and do not cause thrush because they are not deposited in the mouth and do not have local immunosuppressive effects in the oropharynx. The client who makes this statement has confused different asthma medications and needs education about the specific side effect profile of leukotriene blockers.
B) I should take this medication whenever I suddenly have difficulty breathing
This statement reveals a fundamental misunderstanding of the role of leukotriene blockers in asthma management. Leukotriene blockers are controller medications, meaning they are taken regularly on a long-term basis to maintain asthma control and prevent symptoms, not for acute relief of breathing difficulty. They work by reducing airway inflammation over time, which helps decrease the frequency and severity of asthma exacerbations, but they do not provide immediate bronchodilation. When a patient suddenly has difficulty breathing, they need a rescue medication, typically a short-acting beta-agonist such as albuterol, which rapidly relaxes bronchial smooth muscle and relieves acute bronchospasm. Taking a leukotriene blocker during an acute attack would not provide immediate relief and could delay appropriate treatment. The client needs to understand that controller medications are taken daily regardless of symptoms, while rescue medications are used as needed for acute symptoms.
C) This medication is taken once daily for the prevention of asthma
This statement correctly reflects the appropriate use of leukotriene blockers as controller medications for asthma prevention. Montelukast, the most commonly prescribed leukotriene receptor antagonist, is typically taken once daily in the evening. The once-daily dosing schedule is convenient and promotes adherence, and the evening timing may be beneficial because leukotriene levels can increase during the night, contributing to nocturnal asthma symptoms. The medication works by blocking the inflammatory effects of leukotrienes, reducing airway inflammation and hyperresponsiveness over time. Regular daily use is essential for maintaining these effects, and skipping doses can lead to loss of asthma control. The client who understands that this is a preventive medication taken daily, not as needed for symptoms, demonstrates appropriate knowledge of its role in their asthma management plan.
D) I should expect this medication will make me agitated, but I don't need to report that effect
This statement contains two dangerous misunderstandings. First, while neuropsychiatric events including agitation, aggression, mood changes, and depression have been reported with montelukast, these are not expected effects that patients should simply accept. The U.S. Food and Drug Administration has issued a boxed warning for montelukast regarding serious neuropsychiatric events, and patients must be informed of this risk. Second, and more critically, the statement that these effects do not need to be reported is completely incorrect. Any neuropsychiatric symptoms occurring during montelukast therapy should be reported to the healthcare provider immediately, as they may require discontinuation of the medication. The FDA warning emphasizes that healthcare providers should consider the benefits and risks of montelukast and discuss these potential effects with patients. Patients should be instructed to stop taking montelukast and contact their provider if they experience any behavioral or mood-related changes. The client who believes these effects are expected and not reportable is at risk for continued exposure to a medication that may be causing significant adverse effects without seeking appropriate medical attention.
Conclusion
The client demonstrates understanding by stating that a leukotriene blocker is taken once daily for the prevention of asthma, correctly identifying this medication as a controller used for long-term management. The statement about thrush reflects confusion with inhaled corticosteroids. The belief that it should be taken for acute breathing difficulty misunderstands its role as a preventive medication. The statement about agitation being expected and not reportable is dangerous and ignores important FDA warnings. Therefore, the correct statement is about daily preventive use, reflecting appropriate knowledge of the medication's role in asthma management.
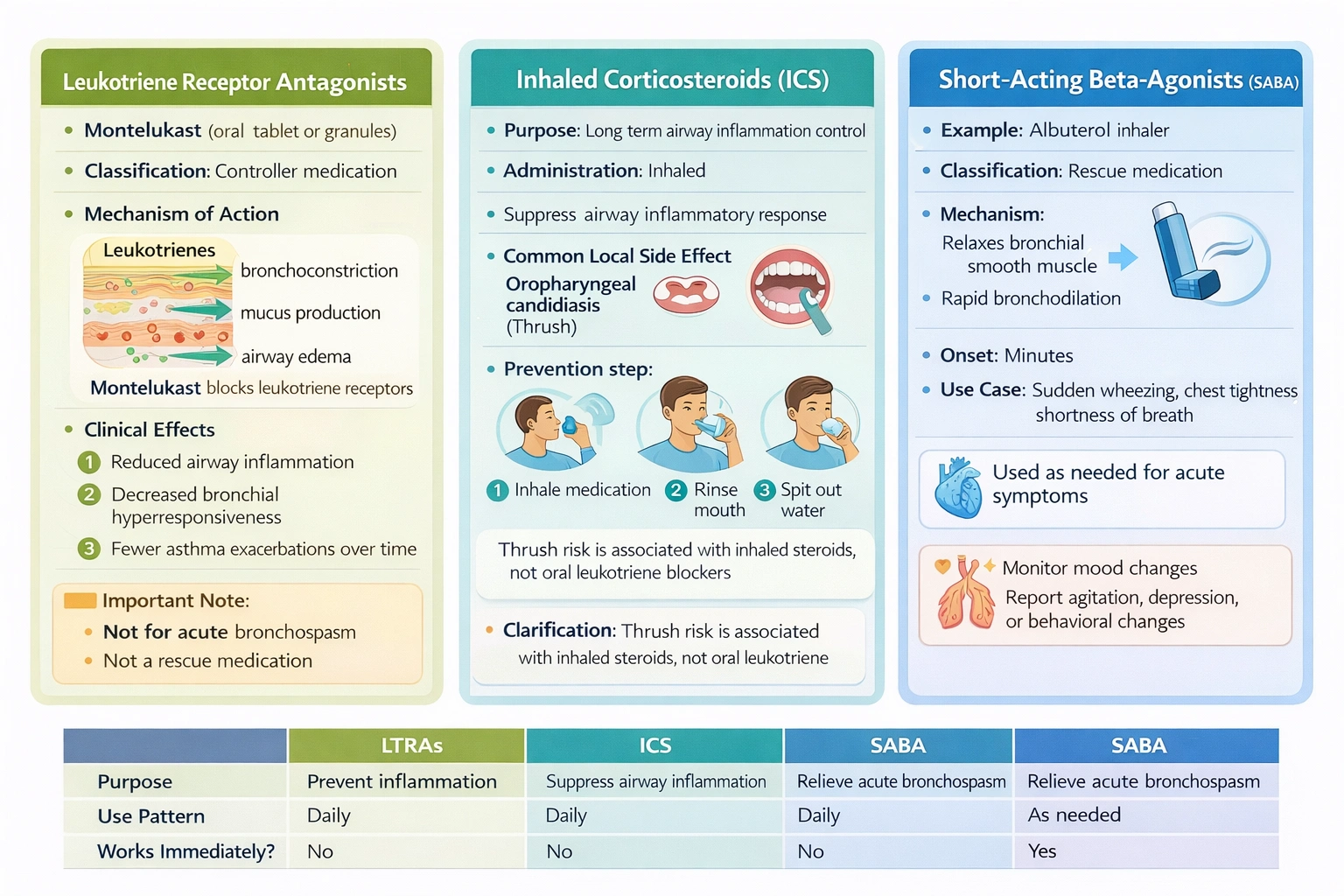
A client with an infection is being treated with vancomycin. The nurse providing care reviews the client's laboratory reports and notes that the client's blood urea nitrogen and serum creatinine levels are newly elevated. What would be the appropriate nursing intervention?
A.
Consult the provider about the need for a less nephrotoxic medication
B. Assess the client's urine output
C. Interpret the peak and trough levels
D. Instruct the client to notify the nurse if they have any tingling in their toes
Rationale
The appropriate nursing intervention is to interpret the peak and trough levels, as elevated BUN and creatinine indicate possible nephrotoxicity, and vancomycin levels will determine if the drug is in the toxic range and contributing to renal impairment, guiding further management.
Vancomycin is a glycopeptide antibiotic used for serious gram-positive infections, including methicillin-resistant Staphylococcus aureus. It is associated with nephrotoxicity, particularly when trough levels are elevated. The mechanism of vancomycin-induced nephrotoxicity involves oxidative stress and tubular injury in the kidneys. Risk factors include high doses, prolonged therapy, concomitant nephrotoxic medications, and pre-existing renal impairment. Monitoring vancomycin levels, specifically trough levels, is essential for ensuring therapeutic efficacy while minimizing toxicity. Trough levels are drawn just before the next dose and reflect the lowest concentration of the drug. Target trough levels vary by infection type but are typically 10 to 20 mcg/mL for most infections, with higher targets for more serious infections like pneumonia or bacteremia. When BUN and creatinine are elevated, indicating possible renal impairment, the nurse must determine whether this is related to vancomycin toxicity or other causes. Interpreting the vancomycin levels will show whether the drug is in the toxic range and likely contributing to the renal injury.
A) Consult the provider about the need for a less nephrotoxic medication
While this may eventually be necessary, it is premature without first assessing vancomycin levels. The provider will need to know the vancomycin levels to make an informed decision about whether to continue, adjust, or change therapy. Consulting without this information may lead to unnecessary changes or delays in appropriate treatment.
B) Assess the client's urine output
Assessing urine output is important for monitoring renal function, but it does not directly address the relationship between vancomycin therapy and the elevated BUN/creatinine. Urine output could be normal even with early nephrotoxicity, and this assessment alone does not provide information about vancomycin levels or whether the drug is the cause.
C) Interpret the peak and trough levels
This is the most appropriate immediate intervention. The nurse should review the most recent vancomycin levels, particularly the trough level, to determine if they are within the therapeutic range or elevated. If the trough is elevated, it suggests vancomycin accumulation and likely contribution to the renal impairment. The nurse should then report these findings to the provider, along with the elevated BUN and creatinine, to guide further management, which may include holding doses, adjusting the dosing interval, or changing therapy.
D) Instruct the client to notify the nurse if they have any tingling in their toes
Tingling in the toes could indicate peripheral neuropathy, a possible but less common side effect of vancomycin. It does not address the acute concern of elevated renal function tests and potential nephrotoxicity. This instruction is not the priority and would not help in managing the current situation.
Conclusion
With elevated BUN and creatinine in a client receiving vancomycin, the nurse should first interpret the peak and trough levels to assess for vancomycin accumulation and toxicity. Consulting about alternative medication, assessing urine output, and monitoring for tingling are secondary or less specific. Therefore, interpreting peak and trough is correct, guiding further management based on drug levels.

A nurse is preparing discharge teaching for a client who will be going home on warfarin. Which of these statements indicates the need for further instruction?
A.
I should avoid alcohol and herbal remedies while I am taking warfarin
B. I should have my bleeding time checked when I am taking antibiotics
C. I should stop taking my warfarin if I get bruises or black stools
D. I should be consistent with my intake of leafy greens because they reverse warfarin effects
Rationale
The statement that the client should stop taking warfarin if they get bruises or black stools indicates need for further instruction, as these signs of bleeding should be reported to the provider, but the client should not independently stop the medication without consultation.
Warfarin is an anticoagulant with a narrow therapeutic index that requires careful management and patient education for safe use. Bruises and black, tarry stools are signs of bleeding that should be reported to the healthcare provider immediately. Bruising may indicate that the INR is too high, and black stools suggest gastrointestinal bleeding, which can be serious. However, the client should not independently stop taking warfarin without consulting the provider. Abruptly stopping warfarin can lead to rebound hypercoagulability and increase the risk of thrombosis, including stroke, pulmonary embolism, or deep vein thrombosis, depending on the indication for anticoagulation. The correct action is to report the symptoms and seek guidance. The provider will determine if the dose needs adjustment or if the medication should be temporarily held based on the severity of the bleeding and the INR value.
A) I should avoid alcohol and herbal remedies while I am taking warfarin
This statement shows understanding. Alcohol and many herbal remedies interact with warfarin and can affect INR, increasing bleeding or clotting risk. Avoiding them is appropriate.
B) I should have my bleeding time checked when I am taking antibiotics
This statement shows understanding. Antibiotics can affect INR, and monitoring is appropriate. The client may mean INR rather than bleeding time, but the intent is correct.
C) I should stop taking my warfarin if I get bruises or black stools
This statement indicates need for further instruction. The client should report these signs but not self-discontinue. The nurse must explain the importance of contacting the provider for guidance rather than independently stopping the medication.
D) I should be consistent with my intake of leafy greens because they reverse warfarin effects
This statement shows understanding. Consistent vitamin K intake helps maintain stable INR. Large variations can cause fluctuations.
Conclusion
The client needs further instruction when stating they should stop warfarin if they get bruises or black stools, as they should report but not self-discontinue. The other statements about alcohol, antibiotic monitoring, and consistent greens are correct. Therefore, the self-discontinuation statement requires further teaching, emphasizing the importance of reporting rather than independently stopping the medication.
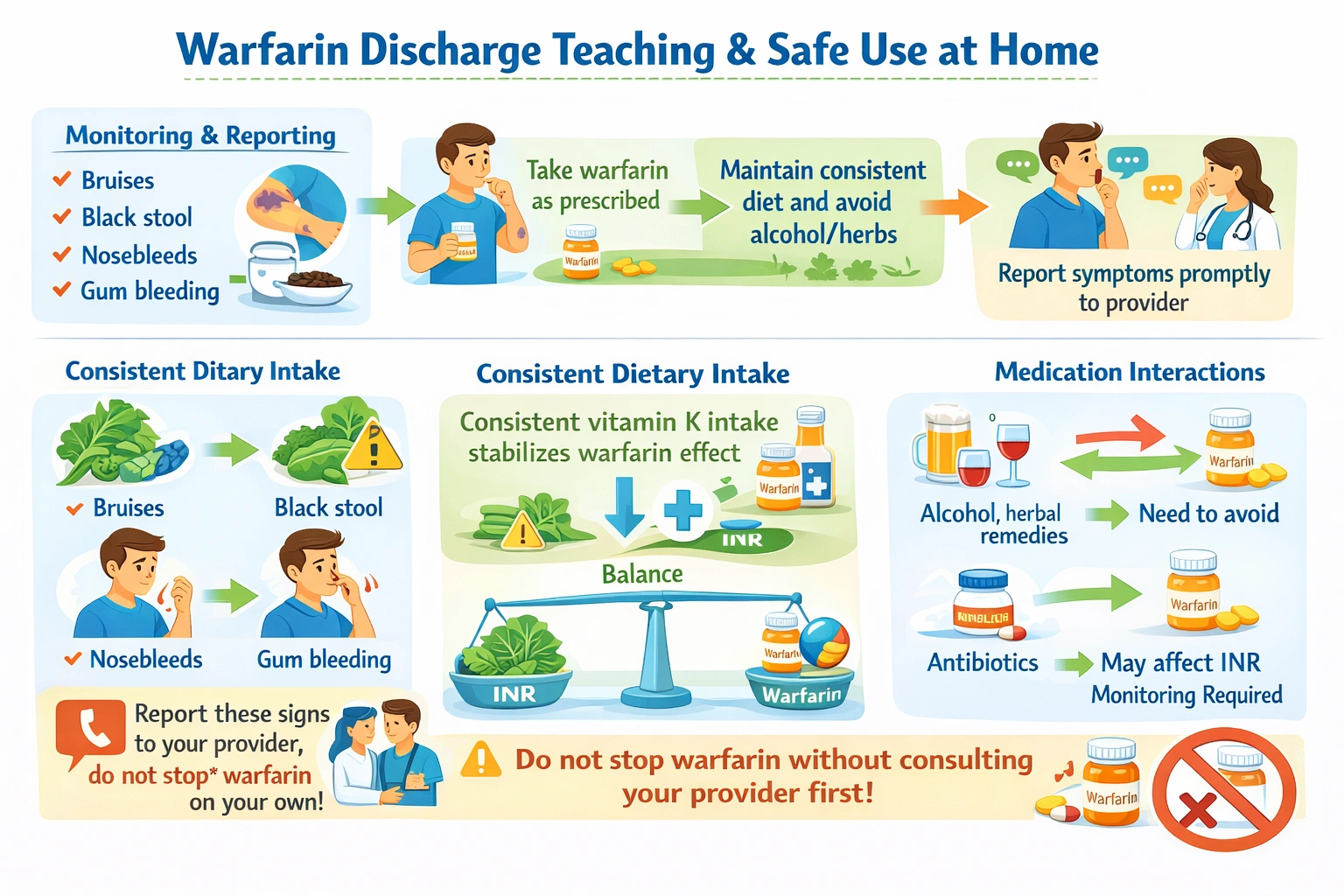
The nurse understands that a bronchodilator would be most therapeutic in which situation?
A.
Irregular respiration, snoring, and intermittent episodes of apnea
B. Fine, scattered crackles heard bilaterally in the bases
C. Coarse crackles in the right lower lobe
D. Expiratory wheezing
Rationale
The nurse understands that a bronchodilator would be most therapeutic in a situation with expiratory wheezing, as this finding indicates bronchoconstriction, which is the primary pathophysiologic mechanism that bronchodilators are designed to reverse.
Bronchodilators are a class of medications that work by relaxing the smooth muscle surrounding the airways, leading to bronchodilation and reduced airway resistance. They are fundamental to the management of conditions characterized by bronchoconstriction, such as asthma and chronic obstructive pulmonary disease. The two main classes of bronchodilators are beta-2 adrenergic agonists, which stimulate beta-2 receptors on airway smooth muscle to cause relaxation, and anticholinergics, which block muscarinic receptors to prevent acetylcholine-mediated bronchoconstriction. The effectiveness of bronchodilators depends entirely on whether the underlying respiratory problem involves bronchial smooth muscle constriction as a significant component. Therefore, identifying clinical findings that specifically indicate bronchoconstriction is essential for appropriate medication selection. Expiratory wheezing is the classic auscultatory finding associated with bronchoconstriction and represents the situation where bronchodilators would be most directly therapeutic.
A) Irregular respiration, snoring, and intermittent episodes of apnea
These findings suggest obstructive sleep apnea rather than bronchoconstriction. Obstructive sleep apnea is a sleep-disordered breathing condition characterized by repeated episodes of upper airway collapse during sleep, leading to reduced or absent airflow despite continued respiratory effort. The snoring results from vibration of pharyngeal tissues as air passes through a narrowed upper airway, and the apneic episodes occur when the airway completely collapses. This condition involves mechanical obstruction of the pharyngeal airway, typically at the level of the soft palate, uvula, tonsils, or tongue base, not constriction of the bronchial smooth muscle. Bronchodilators have no role in treating obstructive sleep apnea because they do not affect the structural or neuromuscular factors that cause upper airway collapse during sleep. Management of sleep apnea involves positive airway pressure devices such as CPAP, positional therapy, oral appliances, weight loss, and in some cases, surgical interventions. The irregular respirations and apnea are due to upper airway mechanics, not bronchial smooth muscle spasm, and bronchodilators would not be therapeutic in this situation.
B) Fine, scattered crackles heard bilaterally in the bases
Crackles, also known as rales, are discontinuous, non-musical sounds produced by air passing through fluid or secretions in the small airways or by the sudden opening of closed airways during inspiration. Fine crackles are high-pitched, brief, and soft sounds that resemble the sound of hair being rubbed between fingers. When heard bilaterally in the lung bases, they suggest conditions such as pulmonary edema, where fluid accumulates in the interstitial and alveolar spaces, interstitial lung disease, where fibrosis alters lung compliance and airway dynamics, or early pneumonia with inflammatory exudate. These findings indicate the presence of fluid or inflammatory material in the airways or interstitium, not bronchoconstriction. Bronchodilators would not address the underlying pathophysiology in these conditions. Pulmonary edema requires diuretics to reduce fluid overload and interventions to improve cardiac function if the edema is cardiogenic. Interstitial lung disease may require anti-inflammatory or immunosuppressive therapy. Pneumonia requires antibiotics and supportive care. While bronchodilators might be used as adjunctive therapy in some respiratory conditions to help with associated bronchospasm or to improve mucociliary clearance, they are not the primary therapeutic intervention for crackles, and this situation would not be where they are most therapeutic.
C) Coarse crackles in the right lower lobe
Coarse crackles are louder, lower-pitched, and longer in duration than fine crackles, and they are produced by air passing through secretions in the larger airways. When localized to a specific lobe, such as the right lower lobe, they suggest localized consolidation or secretion accumulation, as seen in pneumonia. The crackles are generated as air moves through inflammatory exudate, pus, or mucus that has accumulated in the airways and alveoli of that specific region. This finding does not indicate bronchoconstriction, which would typically produce wheezing rather than crackles. While bronchodilators might be used as adjunctive therapy in pneumonia to help with associated bronchospasm or to improve airway clearance, they are not the most therapeutic intervention for this finding. The primary treatment for lobar pneumonia is antibiotic therapy directed against the causative organism, along with supportive measures such as hydration, oxygen if needed, and airway clearance techniques. Bronchodilators do not treat the infection or the inflammatory exudate, and this is not the situation where they would be most therapeutic.
D) Expiratory wheezing
Expiratory wheezing is the correct finding that indicates bronchoconstriction and represents the situation where bronchodilators are most directly therapeutic. Wheezes are continuous, musical, high-pitched sounds produced by turbulent airflow through narrowed airways. The expiratory timing is particularly significant because during expiration, the airways naturally narrow due to decreased intrathoracic pressure, and this narrowing is exaggerated when bronchial smooth muscle is constricted. The musical quality of wheezes results from the vibration of airway walls as air flows through the narrowed lumen. Conditions such as asthma, chronic obstructive pulmonary disease, and other reactive airway diseases present with wheezing as a hallmark finding. In asthma, exposure to triggers such as allergens, irritants, or respiratory infections leads to bronchial smooth muscle constriction, airway inflammation, and increased mucus production. Bronchodilators such as albuterol, a beta-2 agonist, work by binding to beta-2 receptors on airway smooth muscle, activating adenylate cyclase, increasing intracellular cyclic AMP, and ultimately causing smooth muscle relaxation. This dilates the airways, reduces airway resistance, and relieves wheezing. Anticholinergic bronchodilators such as ipratropium work by blocking muscarinic receptors, reducing vagally-mediated bronchomotor tone. The presence of expiratory wheezing signals that airway narrowing due to smooth muscle constriction is present, making this the situation where bronchodilator administration would be most directly therapeutic and would address the primary pathophysiologic mechanism.
Conclusion
The nurse understands that bronchodilators are most therapeutic for expiratory wheezing, which indicates bronchoconstriction as the underlying mechanism. Irregular respiration, snoring, and apnea suggest obstructive sleep apnea, a condition of upper airway collapse not responsive to bronchodilators. Fine, scattered crackles in the bases suggest pulmonary edema or interstitial disease involving fluid or inflammation, not bronchoconstriction. Coarse crackles in a single lobe suggest pneumonia with localized consolidation and secretions. Therefore, expiratory wheezing is the correct indication for bronchodilator therapy, as it directly targets the bronchial smooth muscle constriction that produces this finding.
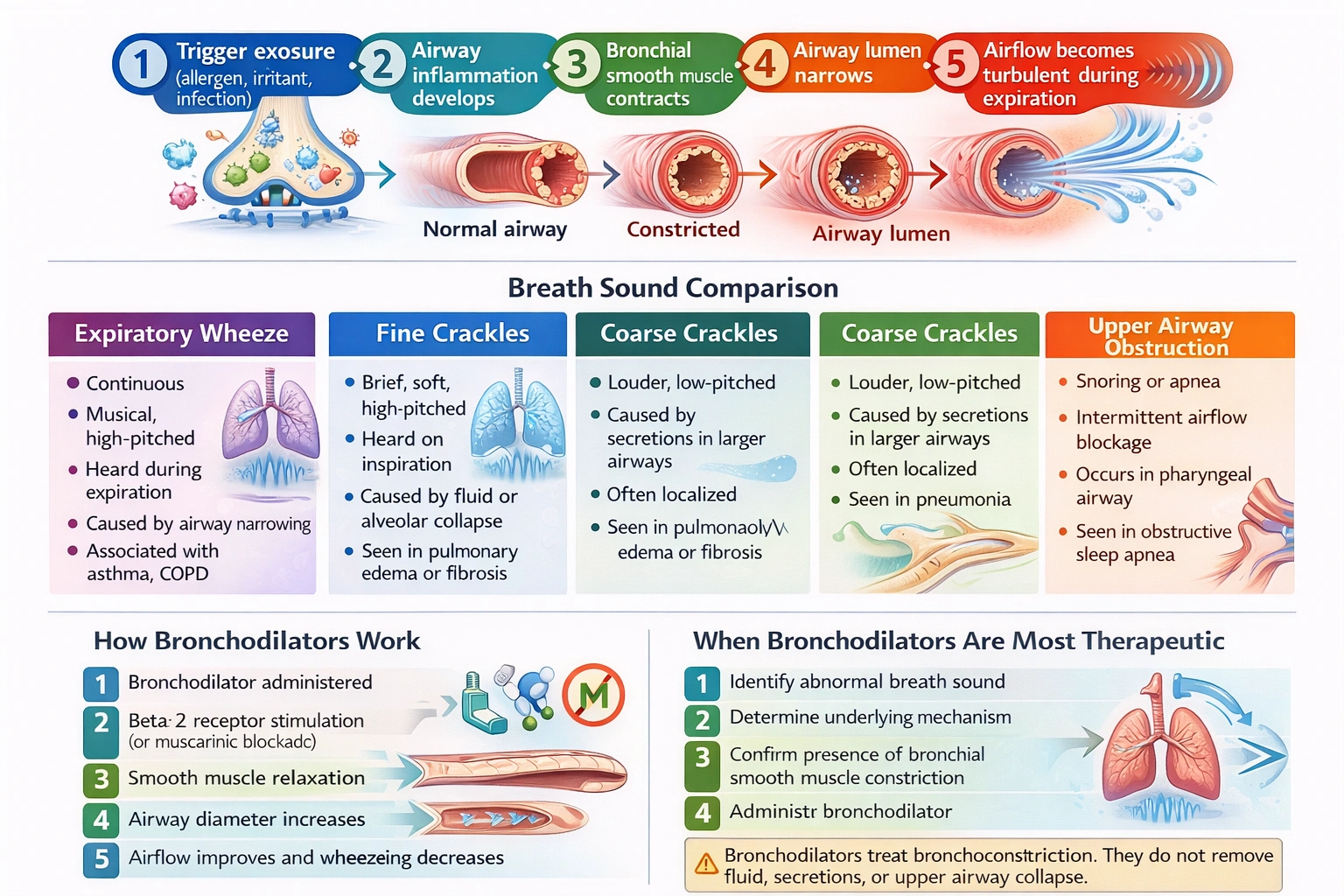
A Prescriber has ordered medication for a newborn that is eliminated primarily by hepatic Metabolism. What would the nurse expect the prescriber to order?
A.
Order a dose that is higher than an adult dose
B. Discontinue the drug after one or two treatments
C. Increase the frequency of medication dosing
D. Order a dose that is lower than an adult dose
Rationale
The nurse would expect the prescriber to order a dose that is lower than an adult dose for a newborn receiving a medication eliminated primarily by hepatic metabolism, due to the immaturity of the newborn's hepatic enzyme systems resulting in slower drug metabolism and prolonged drug effects.
The neonatal period, defined as the first 28 days of life, represents a time of profound physiological change and maturation as the infant transitions from the intrauterine environment to independent existence. All organ systems are immature at birth, and this immaturity has significant implications for drug therapy. The liver, which is the primary site of drug metabolism, undergoes substantial development during the neonatal period and continues to mature throughout the first years of life. Hepatic drug metabolism occurs through two main types of reactions: phase I reactions, which include oxidation, reduction, and hydrolysis, and phase II reactions, which involve conjugation with glucuronide, sulfate, or other molecules to increase water solubility. The enzymes responsible for these reactions, particularly the cytochrome P450 family, have reduced activity at birth and mature at different rates. This developmental immaturity means that newborns metabolize drugs more slowly than older children and adults, leading to prolonged drug half-lives and higher drug concentrations for a given weight-based dose.
A) Order a dose that is higher than an adult dose
This expectation is incorrect and would be dangerous for a newborn. Newborns have immature hepatic metabolism, leading to slower drug clearance and prolonged half-lives. Higher doses would result in even greater drug accumulation and increased risk of toxicity. While newborns may require higher weight-based doses of some medications due to larger volume of distribution from higher total body water, this is not the case for hepatically metabolized drugs where clearance is the limiting factor. The nurse should not expect higher doses and would be concerned if such an order were written.
B) Discontinue the drug after one or two treatments
There is no indication that the medication should be discontinued after one or two treatments based on the information provided. The question addresses dosing for a medication that is ordered, implying ongoing therapy as needed for the newborn's condition. Discontinuing after limited doses is not related to hepatic metabolism considerations and would not be an expected order based on the newborn's age alone. The duration of therapy depends on the condition being treated, not on the route of drug elimination.
C) Increase the frequency of medication dosing
Increasing dosing frequency would be opposite of what is needed for a newborn with immature hepatic metabolism. Slower metabolism means that the drug remains in the body longer, so dosing intervals may need to be extended, not shortened. More frequent dosing would lead to drug accumulation as each subsequent dose is administered before the previous dose has been adequately cleared. This would result in increasing drug levels and potentially severe toxicity. The nurse would expect the prescriber to consider longer dosing intervals, not more frequent dosing, for medications eliminated by hepatic metabolism in newborns.
D) Order a dose that is lower than an adult dose
This is the correct expectation for medication dosing in newborns, particularly for drugs eliminated by hepatic metabolism. The dose is typically calculated based on the infant's weight in kilograms and is significantly lower than the adult dose on a total milligram basis. Even when comparing weight-based doses, newborns often require lower mg/kg doses than older children and adults due to their reduced metabolic capacity. The prescriber must account for the developmental differences in hepatic enzyme activity, which can result in drug clearance that is only 20% to 50% of adult values for some medications. The nurse should anticipate that the prescriber will order an appropriate reduced dose to ensure safety and efficacy, and should verify that the dose is appropriate for the newborn's age, weight, and clinical condition.
Conclusion
For a newborn receiving a medication eliminated primarily by hepatic metabolism, the nurse would expect the prescriber to order a dose lower than an adult dose due to immature hepatic function resulting in slower drug metabolism and prolonged half-lives. Higher doses would increase toxicity risk. Early discontinuation is not related to metabolism. Increased dosing frequency would lead to accumulation. Therefore, a reduced dose is the correct expectation, and the nurse should verify that the ordered dose is appropriate for the newborn's developmental stage.
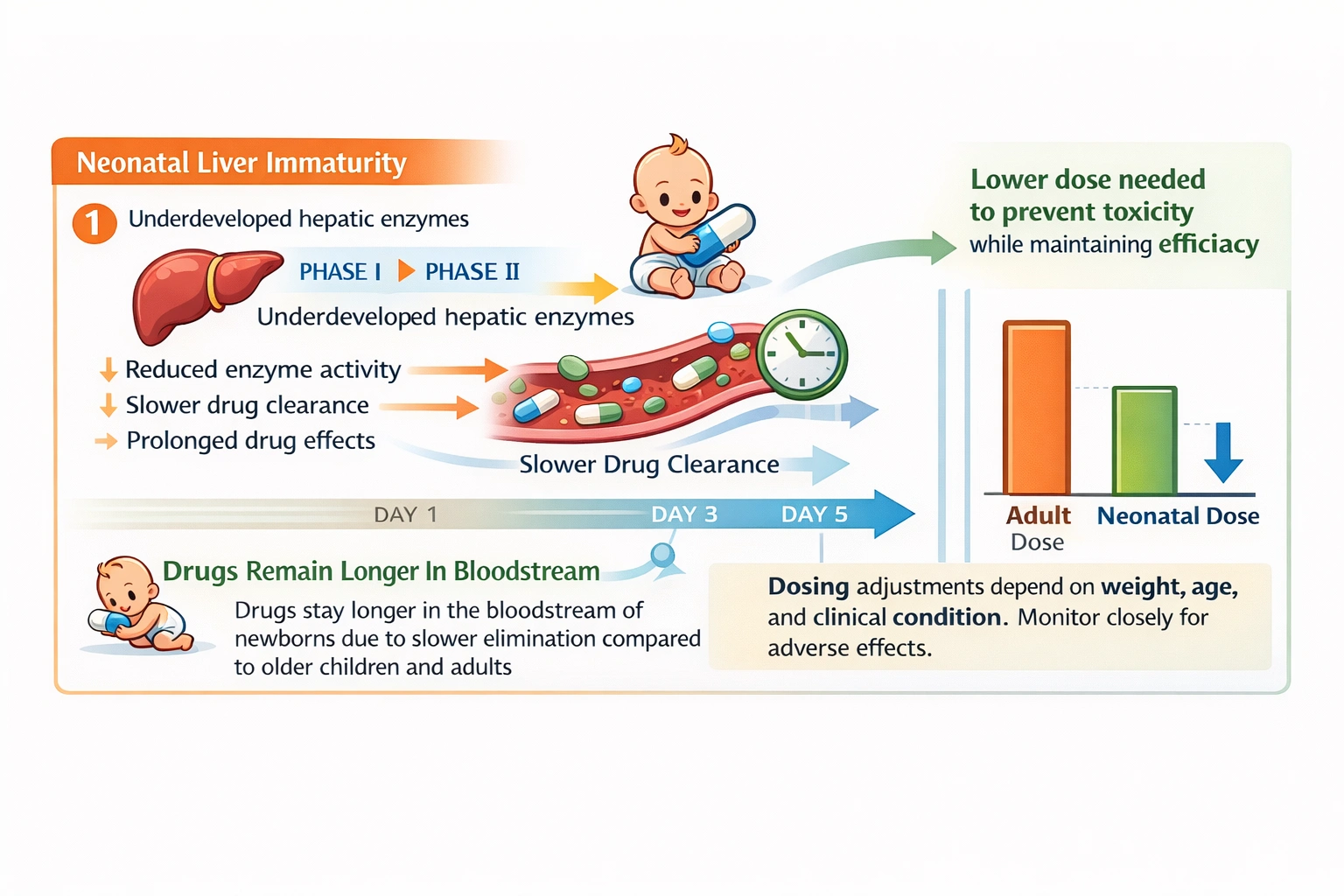
A nurse is providing education to a client who is beginning therapy with testosterone gel 1%. Which statement made by the client demonstrates a need for additional teaching?
A.
I should avoid direct skin-to-skin contact with my spouse where the medication was applied
B. I should not shower or swim for at least five to six hours after application
C. I should have my blood drawn for laboratory tests in 14 days
D. I should apply the medication to my genitals for the best results
Rationale
The client needs additional teaching when stating they should apply the medication to their genitals for best results, as testosterone gel should never be applied to genital skin due to excessively high absorption and the risk of adverse effects.
Testosterone gel is a topical androgen replacement therapy used for male hypogonadism, a condition in which the body does not produce enough testosterone. The gel is designed to be applied to clean, dry, intact skin, typically on the shoulders, upper arms, or abdomen, where it is absorbed through the skin into the systemic circulation. Proper application technique is essential for achieving therapeutic testosterone levels and for minimizing the risk of transfer to others, particularly women and children who could experience adverse effects from unintentional exposure. The pharmacokinetics of transdermal testosterone depend on the characteristics of the skin at the application site, including thickness, vascularity, and presence of hair. Genital skin is thin, highly vascular, and has different absorption characteristics than the skin on the shoulders or arms, leading to excessively rapid and high absorption that can result in supratherapeutic testosterone levels and increased risk of adverse effects.
A) I should avoid direct skin-to-skin contact with my spouse where the medication was applied
This statement shows understanding. Testosterone can transfer from the application site to another person through direct skin contact, potentially causing adverse effects in women and children, including masculinization in women and premature sexual development in children. The client should cover the application site with clothing after the gel dries and wash hands thoroughly after application. Avoiding skin-to-skin contact demonstrates appropriate knowledge of this risk.
B) I should not shower or swim for at least five to six hours after application
This statement shows understanding. Testosterone gel requires time for absorption through the skin. Showering, swimming, or washing the area too soon can wash off medication that has not yet been absorbed, reducing effectiveness. Waiting 5 to 6 hours allows adequate absorption. This demonstrates appropriate knowledge of the application requirements.
C) I should have my blood drawn for laboratory tests in 14 days
This statement shows understanding. Testosterone levels should be monitored after starting therapy to ensure therapeutic levels are achieved and to avoid toxicity. Initial monitoring typically occurs about 14 days after initiation to allow steady-state concentrations to be reached. This demonstrates appropriate knowledge of the need for therapeutic monitoring.
D) I should apply the medication to my genitals for the best results
This statement demonstrates need for additional teaching. Testosterone gel is not for genital application and should never be applied to the genitals. Application to genital skin results in excessively high absorption due to the thin, highly vascular nature of genital skin, leading to supratherapeutic testosterone levels and increased risk of adverse effects including skin irritation, pain, and potential long-term consequences. The medication should be applied to nongenital skin as directed, typically to the shoulders, upper arms, or abdomen. The client requires correction of this dangerous misunderstanding.
Conclusion
The client needs additional teaching when stating they should apply testosterone gel to their genitals for best results, as this is incorrect and potentially harmful. The statements about avoiding skin contact, not showering for 5 to 6 hours, and having blood drawn in 14 days all demonstrate understanding. Therefore, the genital application statement requires further education, and the nurse must provide clear instructions about appropriate application sites and the reasons why genital application is contraindicated.

A client who is pregnant has a history of recurrent genital herpes virus. The client asks the nurse what will be done to suppress an outbreak when she is near term. What is the nurse's response?
A.
Topical acyclovir must be used to control outbreaks
B. Intravenous antiviral agents will be used if an outbreak occurs
C. Antiviral medications are not safe during pregnancy
D. Oral acyclovir may be used during pregnancy
Rationale
The nurse should respond that oral acyclovir may be used during pregnancy to suppress genital herpes outbreaks near term, as suppressive therapy in the last month of pregnancy is recommended to prevent active lesions at delivery and reduce the need for cesarean section.
Genital herpes simplex virus infection during pregnancy presents significant concerns, particularly as delivery approaches. Active genital herpes lesions at the time of delivery pose a risk of neonatal herpes transmission, which can cause severe morbidity and mortality in the newborn. Neonatal herpes can manifest as localized skin, eye, and mouth disease, central nervous system infection with encephalitis, or disseminated disease involving multiple organs, all of which have high rates of complications and death. To prevent transmission, cesarean section is recommended for women with active genital lesions or prodromal symptoms at delivery. For women with a history of recurrent genital herpes, suppressive therapy with oral antiviral medications during the last month of pregnancy is recommended to reduce the risk of active outbreaks at term and thereby decrease the need for cesarean delivery.
A) Topical acyclovir must be used to control outbreaks
Topical acyclovir is not effective for suppressing genital herpes outbreaks and is not used for this purpose. Systemic oral therapy is required to achieve adequate drug levels in the genital tissues to suppress viral replication. Topical formulations are used for localized lesions but do not provide sufficient systemic levels for suppression.
B) Intravenous antiviral agents will be used if an outbreak occurs
This statemen alarming. Intravenous antivirals are reserved for severe infections, disseminated disease, or when oral therapy is not feasible. For routine suppression or management of outbreaks near term, oral therapy is standard. IV therapy would be excessive and not indicated.
C) Antiviral medications are not safe during pregnancy
This statement is false and would cause unnecessary concern. Acyclovir and valacyclovir are considered safe during pregnancy and are recommended for suppressive therapy near term. Extensive clinical experience and pregnancy registry data have not identified significant risks with these medications. This statement could lead the client to refuse necessary treatment.
D) Oral acyclovir may be used during pregnancy
This provides accurate information. Oral acyclovir is safe and effective for suppressing outbreaks near term. The typical regimen is acyclovir 400 mg twice daily or valacyclovir 500 mg once daily starting at 36 weeks gestation and continuing until delivery. This reduces the risk of clinical outbreaks at term and the need for cesarean section. The nurse should explain this to the client to alleviate concerns and provide accurate expectations.
Conclusion
The nurse should respond that oral acyclovir may be used during pregnancy for suppressive therapy near term to prevent outbreaks and reduce the need for cesarean section. Topical therapy is ineffective, IV therapy is not routine, and stating antivirals are unsafe is false. Therefore, oral acyclovir use is the correct information, providing the client with accurate expectations about management of recurrent genital herpes during pregnancy.
A nurse is giving discharge instructions to a client who is beginning theophylline. The nurse tells the client that this medication might cause the following adverse effects?
A.
Oliguria
B. Constipation
C. Drowsiness
D. Tachycardia
Rationale
The nurse should tell the client that theophylline might cause tachycardia as an adverse effect, as this medication is a central nervous system and cardiac stimulant that can increase heart rate through its mechanisms of action.
Theophylline is a methylxanthine bronchodilator that has been used for decades in the management of asthma and chronic obstructive pulmonary disease. Its mechanism of action is complex and involves multiple pathways. Theophylline inhibits phosphodiesterase enzymes, particularly PDE3 and PDE4, which leads to increased intracellular cyclic AMP levels. Cyclic AMP is a second messenger that promotes smooth muscle relaxation, accounting for the bronchodilator effect. Theophylline also antagonizes adenosine receptors, blocking the effects of adenosine which include bronchoconstriction and mast cell activation. Additionally, it may increase histone deacetylase activity, reducing inflammation. However, these same mechanisms produce effects throughout the body, leading to a characteristic profile of adverse effects. The stimulation of the central nervous system and cardiovascular system is particularly significant. Theophylline increases heart rate through direct cardiac stimulation and through adenosine receptor blockade, as adenosine normally has a depressant effect on the sinoatrial node. This can result in tachycardia, palpitations, and in susceptible individuals, more serious arrhythmias.
A) Oliguria
Oliguria, or decreased urine output, is not a common side effect of theophylline. In fact, theophylline has mild diuretic effects due to its ability to increase renal blood flow and glomerular filtration rate, and possibly through direct effects on renal tubules. It may actually increase urine output rather than decrease it. The client who is told to expect oliguria would be misinformed about the medication's effects.
B) Constipation
Constipation is not associated with theophylline use. Gastrointestinal effects of theophylline more commonly include nausea, vomiting, abdominal discomfort, and diarrhea, particularly at higher doses. Constipation is not a typical adverse effect and should not be included in discharge teaching as an expected outcome.
C) Drowsiness
Drowsiness is not an expected effect of theophylline and, in fact, the opposite is more common. Theophylline is a CNS stimulant and typically causes insomnia, nervousness, restlessness, and agitation rather than sedation. Patients may experience difficulty sleeping, particularly if the medication is taken later in the day. Telling the client to expect drowsiness would be incorrect and could lead to them being unprepared for the actual stimulant effects.
D) Tachycardia
Tachycardia is a correct and common adverse effect of theophylline that should be included in discharge teaching. The cardiac stimulant effects of theophylline can cause an increase in heart rate, which may be noticeable to the patient as palpitations or a racing heart. This effect is dose-related and more likely at higher serum levels, but can occur even at therapeutic doses in some individuals. The client should be advised to monitor their heart rate and report significant or persistent tachycardia to their provider. They should also be aware that other stimulants, such as caffeine, can potentiate this effect and should be used with caution.
Conclusion
The nurse should inform the client that theophylline may cause tachycardia as an adverse effect due to its cardiac stimulant properties. Oliguria, constipation, and drowsiness are not typical side effects. Therefore, tachycardia is the correct adverse effect to include, and the client should be counseled about monitoring for this and other stimulant effects.
A client who reports routine consumption of more than 3 alcoholic beverages per day asks about taking acetaminophen when needed for occasional recurrent pain. What will the nurse tell the client?
A.
Do not take more than 4 gm of acetaminophen a day
B. Do not take a scheduled-dose preparation of acetaminophen with opioid analgesics
C. Do not take more than 3 gm of acetaminophen a day
D. Do not take more than 2 gm of acetaminophen a day
Rationale
The nurse will tell the client not to take more than 2 grams of acetaminophen per day, as chronic alcohol consumption increases the risk of hepatotoxicity from acetaminophen, even at doses considered safe for non-alcohol users.
Acetaminophen is one of the most commonly used analgesics and antipyretics worldwide, available over-the-counter in many formulations and also present in numerous prescription combination products. While generally safe at recommended doses, acetaminophen has a narrow therapeutic index regarding hepatotoxicity. The maximum recommended daily dose for healthy adults is typically 3 to 4 grams, with 4 grams being the absolute upper limit. However, this limit is not universal and must be adjusted based on individual patient factors. Chronic alcohol consumption significantly alters the metabolism of acetaminophen and increases the risk of liver injury through several mechanisms. First, alcohol induces cytochrome P450 enzymes, particularly CYP2E1, which metabolizes a small portion of acetaminophen to a toxic metabolite called N-acetyl-p-benzoquinone imine. Normally, this metabolite is rapidly detoxified by conjugation with glutathione in the liver. However, chronic alcohol consumption also depletes glutathione stores, reducing the liver's ability to detoxify NAPQI. The combination of increased production of toxic metabolite and reduced detoxification capacity means that even therapeutic doses of acetaminophen can cause significant liver injury in chronic alcohol users.
A) Do not take more than 4 gm of acetaminophen a day
The 4-gram limit applies to healthy adults without risk factors for hepatotoxicity. For this client with significant alcohol use, 4 grams is too high and could potentially cause liver damage. Providing this limit would be giving false reassurance and could lead to unsafe use. The client needs a lower limit that accounts for their increased risk.
B) Do not take a scheduled-dose preparation of acetaminophen with opioid analgesics
This warning is about unintentional overdose from combination products but does not address the specific alcohol-related risk. While it is true that patients should be aware of the acetaminophen content in opioid combination products to avoid exceeding daily limits, this is not the most important teaching for this particular client. The priority is the reduced daily limit due to alcohol use.
C) Do not take more than 3 gm of acetaminophen a day
Even 3 grams may be too high for a client with significant alcohol consumption. While some sources recommend a 3-gram limit for alcohol users, many experts recommend a more conservative limit of 2 grams to provide an additional margin of safety. Given that the client reports more than 3 alcoholic beverages daily, the safest recommendation is the lower limit.
D) Do not take more than 2 gm of acetaminophen a day
This is the correct reduced limit for clients with significant alcohol consumption to prevent hepatotoxicity. The nurse should explain the reasons for this lower limit, including the enzyme induction and glutathione depletion caused by chronic alcohol use. The client should also be advised to read labels carefully to identify all sources of acetaminophen, including in combination cold and flu products and prescription pain medications, and to avoid taking more than one acetaminophen-containing product at a time.
Conclusion
For a client consuming more than 3 alcoholic beverages daily, the nurse should advise not to take more than 2 grams of acetaminophen per day due to increased hepatotoxicity risk. The 4-gram, 3-gram, and opioid warnings are not the most appropriate for this specific risk. Therefore, 2 grams is correct, providing a safe limit that accounts for the client's alcohol use.
The nurse reinforces instructions regarding when to take levothyroxine and determines teaching was effective when the client states the medication should be taken in which manner?
A.
When they feel fatigued
B. At bedtime
C. With an antacid
D. 30-60 minutes before breakfast
Rationale
The client demonstrates understanding by stating levothyroxine should be taken 30 to 60 minutes before breakfast, as this timing ensures optimal absorption on an empty stomach, avoiding interference from food and other medications.
Levothyroxine is thyroid hormone replacement medication used for hypothyroidism. Its absorption from the gastrointestinal tract is significantly affected by food, beverages, and other medications. Food can reduce levothyroxine absorption by delaying gastric emptying and by physically interfering with drug dissolution and uptake. Calcium and iron supplements, as well as medications such as antacids and proton pump inhibitors, can also bind to levothyroxine or alter gastric pH, reducing absorption. To ensure consistent and maximal absorption, levothyroxine should be taken on an empty stomach, at least 30 to 60 minutes before the first meal of the day, with a full glass of water. This timing minimizes interactions and maintains stable thyroid hormone levels. The client's correct statement indicates understanding of this essential administration instruction.
A) When they feel fatigued
Levothyroxine is taken daily for thyroid replacement, not as needed for symptoms. Fatigue may indicate hypothyroidism, but dosing is scheduled, not PRN.
B) At bedtime
Taking levothyroxine at bedtime may interfere with sleep due to potential stimulant effects in some patients and is not the optimal timing for absorption. Morning dosing on an empty stomach is preferred.
C) With an antacid
Antacids and other medications can interfere with levothyroxine absorption and should be separated by at least 4 hours. Taking with an antacid is incorrect.
D) 30-60 minutes before breakfast
This is correct and shows understanding of proper administration for optimal absorption.
Conclusion
The client demonstrates understanding by stating levothyroxine should be taken 30 to 60 minutes before breakfast. Taking when fatigued, at bedtime, or with antacids are all incorrect. Therefore, before breakfast is correct, reflecting knowledge of optimal administration for consistent absorption.
RN Exams
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests