ATI PHARMACOLOGY QUESTIONS
00:00
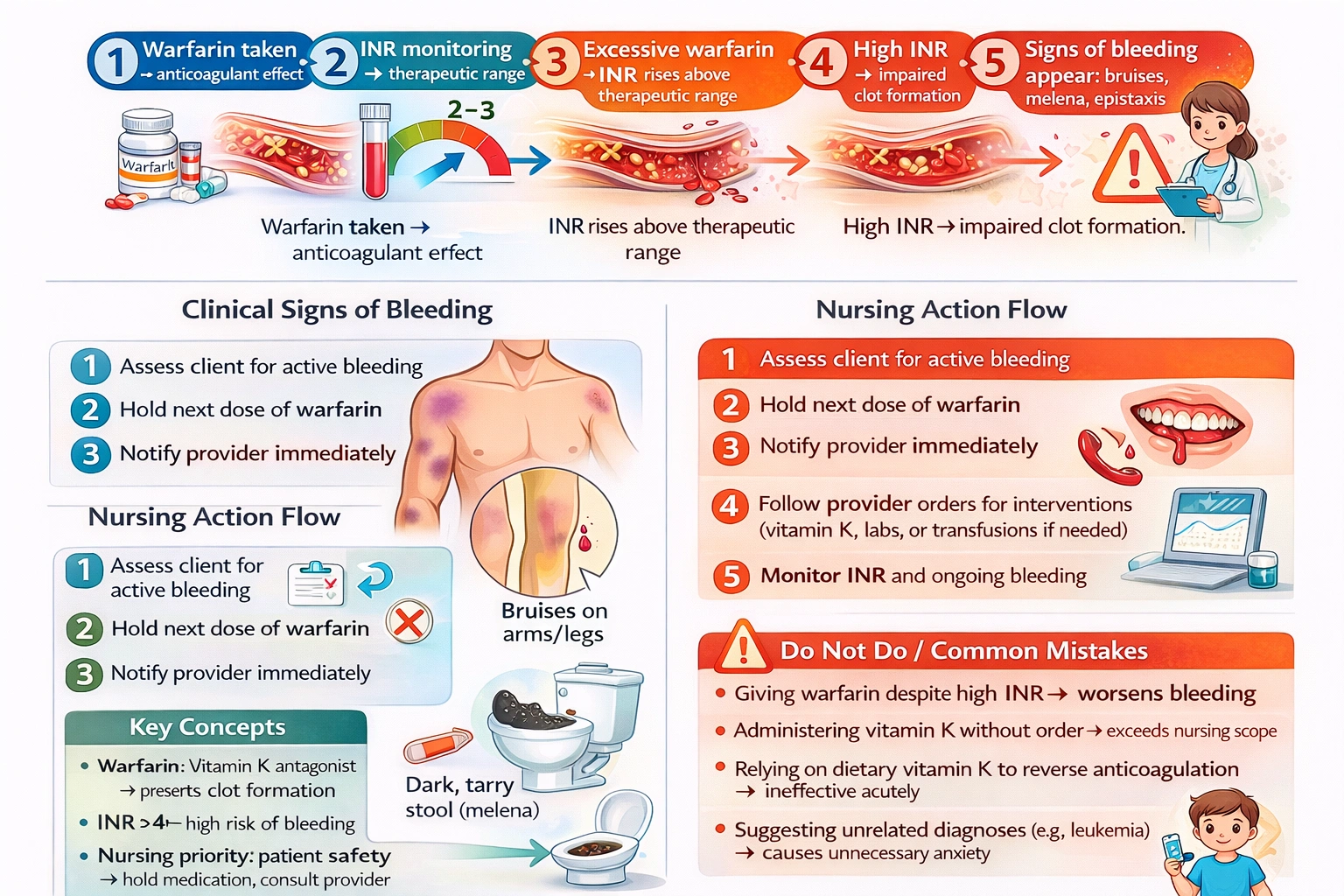
A client taking warfarin presents with bruises, dark tarry stools, and an international normalized ratio of 4.3. What is the nurse's action?
A.
Hold the warfarin and consult the provider regarding the next steps
B. Give an ampule of vitamin K, then call the physician to report client status
C. Explain to the client the nurse may ask the provider to order a test for leukemia
D. Give the warfarin with a dark green salad and check the next stool for blood
Rationale
The nurse should hold the warfarin and consult the provider immediately regarding the next steps, as this clinical presentation indicates excessive anticoagulation with evidence of active bleeding requiring prompt evaluation and intervention.
Warfarin is an oral anticoagulant that has been used for decades to prevent and treat thrombotic events in conditions such as atrial fibrillation, venous thromboembolism, and mechanical heart valves. Its narrow therapeutic index requires careful monitoring of the international normalized ratio, which measures the anticoagulant effect by comparing the patient's prothrombin time to a normal control. The target INR range varies by indication but is typically between 2 and 3 for most conditions. An INR of 4.3 is significantly above the therapeutic range, indicating that the patient is over-anticoagulated and at increased risk for bleeding complications. The client's presenting symptoms of bruises, which indicate bleeding into soft tissues, and dark tarry stools, which are classic for melena and indicate upper gastrointestinal bleeding, confirm that this over-anticoagulation has already resulted in clinically significant hemorrhage. This situation requires immediate action to prevent further bleeding and potential deterioration.
A) Hold the warfarin and consult the provider regarding the next steps
This is the correct and appropriate nursing action that prioritizes client safety while ensuring proper medical oversight. Withholding the next dose of warfarin prevents further elevation of the INR and additional worsening of the anticoagulant effect while the client is already showing signs of bleeding. This is a standard nursing intervention when a client presents with a supratherapeutic INR, particularly when accompanied by evidence of bleeding. The nurse must then consult the provider immediately to report the findings and receive further orders. The provider will need to assess the severity of the bleeding, evaluate the INR value, and determine the appropriate management strategy. For an INR of 4.3 with evidence of bleeding, the provider will likely order vitamin K to reverse the anticoagulation, with the dose and route depending on the urgency of the situation. Oral vitamin K may be appropriate for non-life-threatening bleeding, while intravenous vitamin K and possibly fresh frozen plasma or prothrombin complex concentrates may be needed for more severe hemorrhage. The nurse's role is to recognize the emergency, withhold further anticoagulant, and facilitate prompt medical evaluation and treatment.
B) Give an ampule of vitamin K, then call the physician to report client status
This action is inappropriate because administering vitamin K without a specific provider order constitutes practicing medicine without a license and exceeds the scope of nursing practice. Vitamin K is a medication that reverses the effects of warfarin by providing the substrate necessary for the synthesis of vitamin K-dependent clotting factors in the liver. While vitamin K is clearly indicated for this client given the supratherapeutic INR and evidence of bleeding, the nurse cannot independently decide to administer it. The dose, route, and formulation of vitamin K must be specified by the provider based on the clinical situation. For example, low-dose oral vitamin K might be appropriate for an elevated INR without bleeding, while intravenous vitamin K would be indicated for active bleeding. The nurse who administers vitamin K without an order could cause harm if the dose is incorrect, if the route is inappropriate, or if the client has a contraindication. The correct sequence is to hold the warfarin, notify the provider, and then implement the provider's orders, which will include specific instructions for vitamin K administration if indicated.
C) Explain to the client the nurse may ask the provider to order a test for leukemia
This response is inappropriate and may cause unnecessary alarm and anxiety for the client. While easy bruising and bleeding can occur in leukemia due to thrombocytopenia or coagulation abnormalities, the client's presentation is fully explained by excessive warfarin anticoagulation. The client has a known risk factor in warfarin therapy and a confirmed laboratory abnormality with an INR of 4.3. There is no indication to suggest leukemia, and mentioning this possibility without evidence is not only frightening but also diverts attention from the actual problem. The nurse should focus on the immediate issue of over-anticoagulation and bleeding risk, providing clear information about what is happening and what steps will be taken to address it. Introducing unrelated and concerning possibilities undermines the therapeutic relationship and causes psychological distress without any clinical benefit.
D) Give the warfarin with a dark green salad and check the next stool for blood
This action would be dangerous and demonstrates a serious misunderstanding of warfarin management. Administering another dose of warfarin to a client with a supratherapeutic INR and active bleeding would further increase the INR and worsen the bleeding risk, potentially leading to life-threatening hemorrhage. While dark green vegetables contain vitamin K, which antagonizes warfarin's effect, dietary manipulation is not an appropriate acute management strategy for a client with active bleeding and a significantly elevated INR. The amount of vitamin K in a single salad is unpredictable and insufficient to rapidly reverse anticoagulation. Additionally, relying on dietary changes rather than holding the medication and seeking medical intervention could delay appropriate treatment and allow bleeding to progress. This response demonstrates a critical gap in understanding the urgency of this situation and the appropriate interventions for warfarin-related bleeding.
Conclusion
When a client taking warfarin presents with bruises, dark tarry stools, and an INR of 4.3, the nurse should hold the warfarin and consult the provider immediately regarding the next steps. Administering vitamin K without an order exceeds nursing scope and could be dangerous if the dose or route is incorrect. Suggesting a leukemia workup is inappropriate and causes unnecessary alarm. Giving warfarin with a salad would worsen the bleeding risk and delay appropriate treatment. Therefore, holding the medication and consulting the provider is the correct action that prioritizes client safety and ensures timely medical intervention for this potentially serious bleeding complication.
The nurse is caring for a pregnant client recently diagnosed with hypothyroidism. The client tells the nurse she does not want to take medications while she is pregnant. What will the nurse tell the client?
A.
Neuropsychological deficits in the fetus can occur if the condition is not treated
B. No treatment is required if the client is experiencing symptoms
C. No danger to the fetus exists until the third trimester
D. Hypothyroidism is a normal effect of pregnancy and usually is of no consequence
Rationale
The nurse will tell the client that neuropsychological deficits in the fetus can occur if hypothyroidism is not treated during pregnancy, as maternal thyroid hormone is essential for fetal brain development, particularly during the first trimester when the fetal thyroid gland is not yet functional.
Thyroid hormone plays a critical role in fetal development, particularly in the development of the central nervous system. During the first trimester of pregnancy, the fetal thyroid gland is not yet functional; the fetus is entirely dependent on maternal thyroid hormone crossing the placenta for its neurological development. Maternal thyroxine crosses the placenta and is converted to triiodothyronine in fetal tissues, where it regulates gene expression involved in neuronal proliferation, migration, differentiation, and myelination. Even after the fetal thyroid becomes functional around 12 to 14 weeks of gestation, maternal thyroid hormone continues to contribute significantly to fetal thyroid hormone levels throughout pregnancy. When a pregnant woman has untreated hypothyroidism, insufficient thyroid hormone reaches the fetus, potentially leading to irreversible neurocognitive impairment. The recognition of this critical relationship has led to recommendations for universal screening or case finding for thyroid dysfunction in pregnancy and prompt treatment of hypothyroidism to optimize fetal outcomes.
A) Neuropsychological deficits in the fetus can occur if the condition is not treated
This statement is accurate and provides the client with essential information to make an informed decision about treatment. Multiple studies have demonstrated an association between untreated maternal hypothyroidism and adverse neurocognitive outcomes in offspring. Children born to mothers with untreated hypothyroidism during pregnancy have been shown to have lower IQ scores, reduced cognitive function, and increased risk of neuropsychological deficits compared to children of euthyroid mothers or mothers whose hypothyroidism was adequately treated. The most critical period is the first trimester, when fetal brain development is most dependent on maternal hormone, but the risk persists throughout pregnancy. The nurse should explain this risk clearly and compassionately, emphasizing that levothyroxine treatment is safe during pregnancy and that the benefits of treatment for the baby's brain development far outweigh any theoretical risks of medication. This information helps the client understand that taking medication during pregnancy is not for her own comfort but for the essential neurological development of her baby.
B) No treatment is required if the client is experiencing symptoms
This statemen dangerous. Symptoms of hypothyroidism, such as fatigue, weight gain, cold intolerance, constipation, and depression, indicate that the mother has thyroid hormone deficiency that affects her own health and well-being. More importantly, even if the mother were asymptomatic, which can occur with subclinical hypothyroidism, treatment is still required to maintain adequate hormone levels for the fetus. The goal of treatment during pregnancy is not merely to relieve maternal symptoms but to achieve normal thyroid levels to support fetal development. The presence or absence of symptoms does not determine the need for treatment. The nurse who provides this information would be giving inaccurate and potentially harmful advice that could lead to adverse fetal outcomes.
C) No danger to the fetus exists until the third trimester
This statement is false and reflects a misunderstanding of fetal thyroid development and the timing of brain development. The most critical period for fetal brain development requiring maternal thyroid hormone is the first trimester, before the fetal thyroid is functional. During this period, the fetal brain is undergoing rapid development, including neural tube formation, neuronal proliferation, and initiation of neuronal migration. These processes are exquisitely sensitive to thyroid hormone levels. Waiting until the third trimester to treat hypothyroidism would miss this crucial window of brain development and could result in irreversible deficits. While untreated hypothyroidism throughout pregnancy poses ongoing risks, the danger exists from the earliest stages, not just in the third trimester.
D) Hypothyroidism is a normal effect of pregnancy and usually is of no consequence
This statement is completely false and demonstrates a dangerous lack of understanding. Hypothyroidism is not a normal effect of pregnancy. While pregnancy does increase thyroid hormone requirements due to increased thyroxine-binding globulin, increased plasma volume, and transfer of thyroid hormone to the fetus, this increased demand can unmask underlying thyroid dysfunction in women with borderline thyroid reserve. However, hypothyroidism itself is a pathologic condition requiring treatment. It is not a normal pregnancy effect and is not without consequence. Untreated hypothyroidism during pregnancy is associated with multiple adverse outcomes including preeclampsia, gestational hypertension, placental abruption, postpartum hemorrhage, miscarriage, preterm birth, low birth weight, and the neurocognitive deficits in the offspring already discussed. The nurse who suggests it is normal and of no consequence would be providing information that is both incorrect and potentially harmful.
Conclusion
When a pregnant client with hypothyroidism expresses reluctance to take medication, the nurse should explain that neuropsychological deficits in the fetus can occur if the condition is not treated, as maternal thyroid hormone is essential for fetal brain development, particularly in the first trimester. Treatment is required regardless of symptoms to ensure adequate hormone levels for the fetus. Danger exists from the first trimester, not just the third. Hypothyroidism is not a normal pregnancy effect and has significant consequences if untreated. Therefore, the correct information emphasizes the risk of fetal neuropsychological deficits, providing the client with the knowledge needed to understand why treatment during pregnancy is essential for her baby's healthy development.

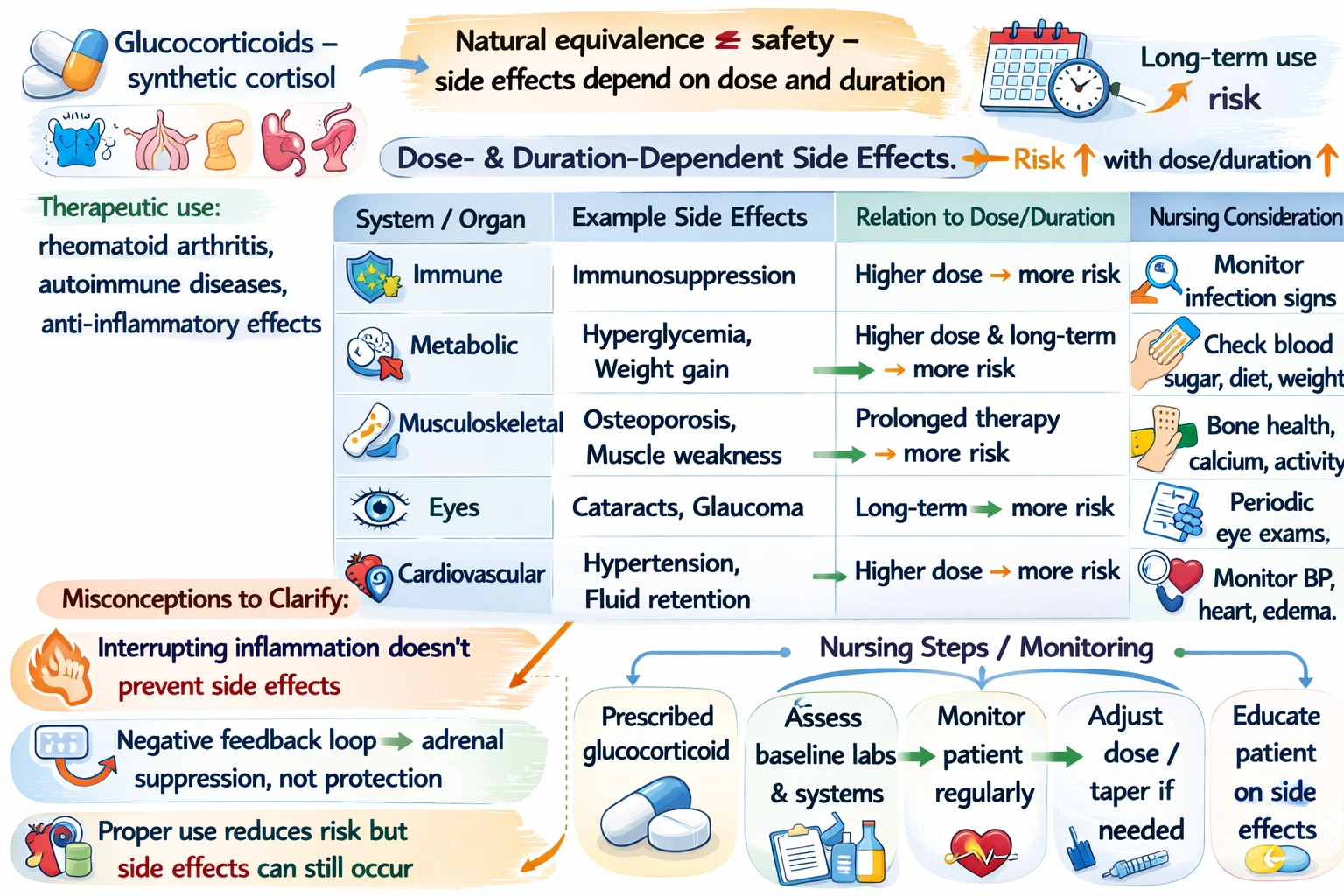
A nurse tells a nursing student glucocorticoids given for rheumatoid arthritis are nearly identical to substances produced naturally by the body. The student remarks that the drug must be very safe. Which response by the nurse is correct?
A.
Side effects can occur and are dependent on the dose and duration of treatment
B. By interrupting the inflammatory process, these drugs inhibit side effects
C. The negative feedback loop prevents side effects
D. As long as the drug is taken as prescribed, side effects usually do not occur
Rationale
The correct response is that side effects can occur and are dependent on the dose and duration of treatment, correcting the student's misconception that natural equivalence means safety and emphasizing that glucocorticoids produce predictable, dose-dependent adverse effects despite their similarity to endogenous hormones.
Glucocorticoids are indeed similar or identical to hormones produced naturally by the body's adrenal glands. Cortisol, the primary endogenous glucocorticoid, is essential for life and plays critical roles in metabolism, immune function, stress response, and maintenance of homeostasis. However, the therapeutic use of glucocorticoids differs fundamentally from normal physiology in several important ways. Endogenous cortisol is produced in a regulated manner with a circadian rhythm, with levels highest in the morning and lowest at night, and with increases in response to stress. Therapeutic glucocorticoids are administered in supraphysiologic doses that exceed normal endogenous production, often on a fixed schedule that does not mimic the natural rhythm. These high doses produce effects that go far beyond replacing what the body would normally make, leading to predictable adverse effects that are directly related to the dose and duration of therapy.
A) Side effects can occur and are dependent on the dose and duration of treatment
This response is accurate and appropriate. It corrects the student's misconception that natural equivalence means safety by explaining that side effects are real and predictable based on treatment factors. The dose-dependent nature of steroid side effects means that higher doses and longer treatment durations are associated with greater risk and severity of adverse effects. Common side effects include immunosuppression increasing infection risk, hyperglycemia and steroid-induced diabetes, osteoporosis and increased fracture risk, weight gain with central obesity, moon face and buffalo hump, adrenal suppression, hypertension, cataracts, glaucoma, mood changes, and many others. The nurse's response provides essential understanding for safe medication administration and monitoring.
B) By interrupting the inflammatory process, these drugs inhibit side effects
. Interrupting inflammation is the therapeutic effect of glucocorticoids, not a mechanism that inhibits side effects. The anti-inflammatory effects are mediated through genomic and non-genomic mechanisms, including inhibition of cytokine production, reduced inflammatory cell migration, and decreased production of inflammatory mediators. Side effects occur through various pathways unrelated to the anti-inflammatory action, including metabolic effects, mineralocorticoid effects, and direct effects on tissues such as bone. The therapeutic effect does not prevent side effects, and in fact, the same mechanisms that produce therapeutic benefit can contribute to adverse effects when excessive.
C) The negative feedback loop prevents side effects
This statemen misunderstands the physiology. The negative feedback loop is part of the body's regulatory mechanism where exogenous steroids suppress the hypothalamus and pituitary, reducing secretion of CRH and ACTH and thereby decreasing endogenous cortisol production. This suppression is itself a side effect, leading to adrenal insufficiency and the risk of adrenal crisis during stress. The negative feedback loop does not prevent other side effects; it is one of the mechanisms by which chronic steroid use causes harm.
D) As long as the drug is taken as prescribed, side effects usually do not occur
This statement is false and would provide dangerous misinformation. Side effects of glucocorticoids are expected consequences of therapy, not just results of improper use. Even when taken exactly as prescribed at appropriate doses, patients develop side effects related to the dose and duration of therapy. Some side effects are almost universal with prolonged use, such as some degree of adrenal suppression and changes in body fat distribution. This response would give false reassurance and is not accurate, potentially leading the student to underestimate the risks of steroid therapy.
Conclusion
The nurse correctly responds that side effects can occur with glucocorticoids and are dependent on dose and duration of treatment, emphasizing that natural equivalence does not mean safety. The statements that inflammation interruption inhibits side effects, negative feedback prevents side effects, or proper use prevents side effects are all incorrect. Therefore, the accurate response addresses dose-dependent and duration-dependent side effects, providing the student with essential understanding of the risk-benefit profile of glucocorticoid therapy.
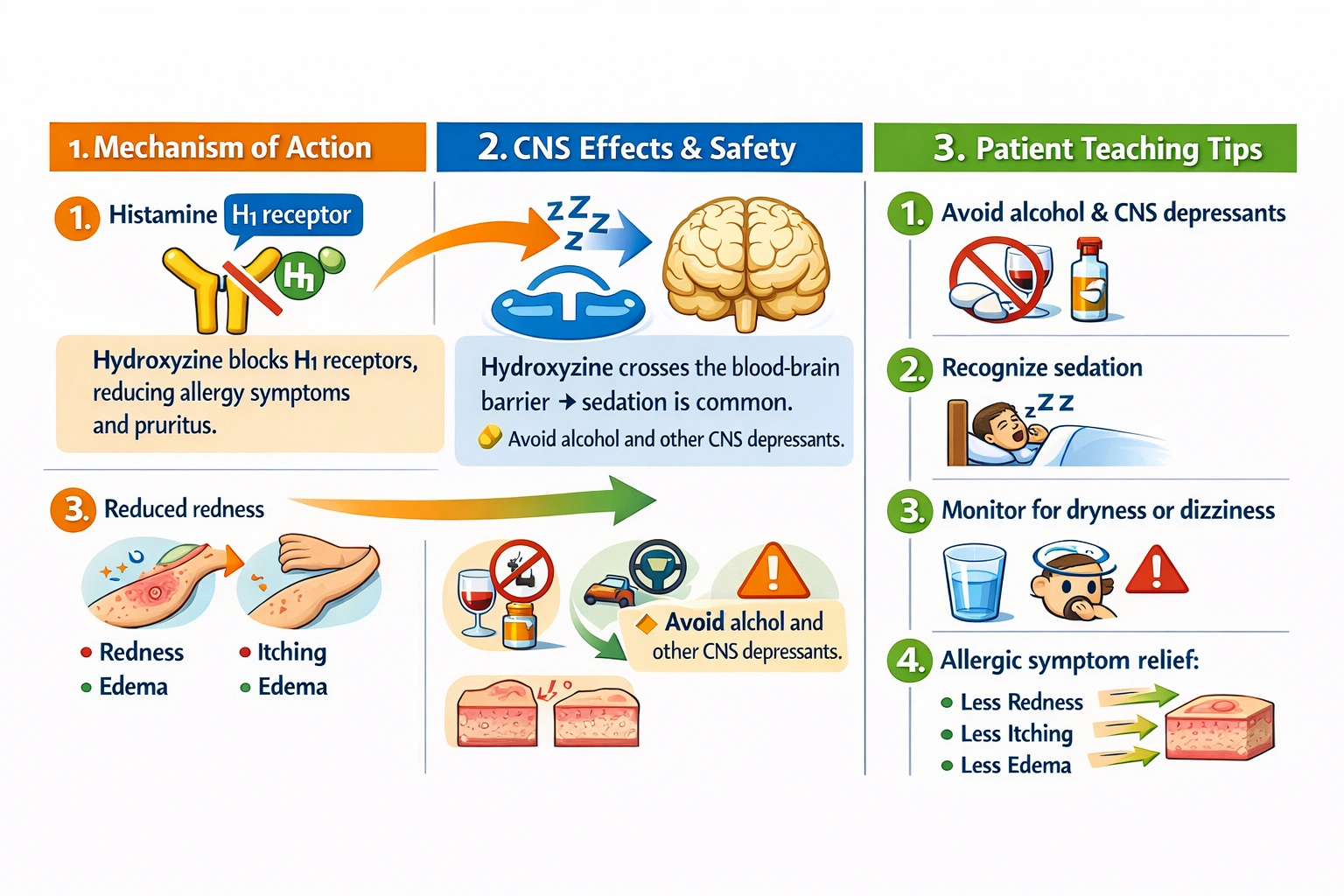
The nurse will include which information when teaching a client about hydroxyzine?
A.
The client should avoid drinking alcohol while taking the drug
B. The drug will reduce redness and itching but not edema
C. The client should report nausea while taking the medication
D. This medication is not likely to cause sedation
Rationale
The nurse should include that the client should avoid drinking alcohol while taking hydroxyzine, as both are central nervous system depressants and concurrent use can lead to excessive sedation, impaired coordination, and increased risk of accidents.
Hydroxyzine is a first-generation antihistamine that has been used for decades for various indications including anxiety, pruritus, and as a preanesthetic medication. It belongs to the piperazine class of antihistamines and works by blocking histamine H1 receptors, which accounts for its effectiveness in treating allergic conditions and itching. However, like other first-generation antihistamines, hydroxyzine readily crosses the blood-brain barrier and affects histamine receptors in the central nervous system, producing significant sedative effects. This sedation is actually part of its therapeutic effect when used for anxiety, but it also creates important safety considerations. The CNS depressant effects of hydroxyzine include drowsiness, sedation, dizziness, and impaired cognitive and motor function. Alcohol is also a CNS depressant that produces similar effects through different mechanisms, primarily by enhancing GABAergic inhibition in the brain. When hydroxyzine and alcohol are combined, their CNS depressant effects are additive, meaning the combined effect is greater than the sum of their individual effects. This can lead to profound sedation, significant impairment of coordination and judgment, increased risk of falls and accidents, and potentially dangerous levels of respiratory depression in susceptible individuals.
A) The client should avoid drinking alcohol while taking the drug
This is correct and essential safety information that must be included in teaching for any patient receiving hydroxyzine. The nurse should explain that both hydroxyzine and alcohol depress the central nervous system, and combining them can lead to excessive drowsiness, dizziness, and impaired coordination. This increases the risk of falls, motor vehicle accidents, and other injuries. The patient should be advised to avoid alcohol entirely while taking hydroxyzine, and to use caution with other CNS depressants such as benzodiazepines, opioids, and sleep aids. This teaching is critical for patient safety and should be emphasized at the start of therapy and reinforced at follow-up visits.
B) The drug will reduce redness and itching but not edema
This statement is not accurate and reflects a misunderstanding of hydroxyzine's pharmacology. As an antihistamine, hydroxyzine blocks H1 receptors and reduces all histamine-mediated effects, including redness, itching, and edema. The classic triple response of histamine includes redness from vasodilation, wheal from increased vascular permeability leading to localized edema, and flare from axon reflex. By blocking H1 receptors, hydroxyzine reduces all components of this response. It is effective for the edema associated with urticaria and other allergic skin conditions. The statement that it reduces redness and itching but not edema is incorrect and would give the patient an inaccurate understanding of the medication's effects.
C) The client should report nausea while taking the medication
Nausea is not a common or serious side effect of hydroxyzine and does not require special reporting. The most common side effects of hydroxyzine are related to its CNS depressant and anticholinergic effects and include drowsiness, sedation, dry mouth, and dizziness. Nausea can occur but is typically mild and self-limiting. Instructing the patient to report nausea is not a priority teaching point and could cause unnecessary concern. The focus of teaching should be on the more significant effects and safety considerations, particularly the sedation and the interaction with alcohol.
D) This medication is not likely to cause sedation
This statement is false and would be misleading and potentially dangerous. Hydroxyzine is a first-generation antihistamine that causes significant sedation in most patients. This is one of its most well-known effects and is actually utilized therapeutically when the medication is used for anxiety or as a preanesthetic. While some patients may develop tolerance to the sedative effects over time, sedation is expected, especially when starting therapy. Telling the patient that sedation is not likely could result in them being unprepared for this effect, potentially leading to situations where they drive or operate machinery while impaired, increasing accident risk. The nurse should instead advise the patient that sedation is common and that they should use caution until they know how the medication affects them.
Conclusion
When teaching about hydroxyzine, the nurse must include that the client should avoid alcohol due to additive CNS depression. The statements about not reducing edema, reporting nausea, and not causing sedation are all incorrect. Therefore, avoiding alcohol is the correct teaching, addressing a critical safety consideration for this medication.
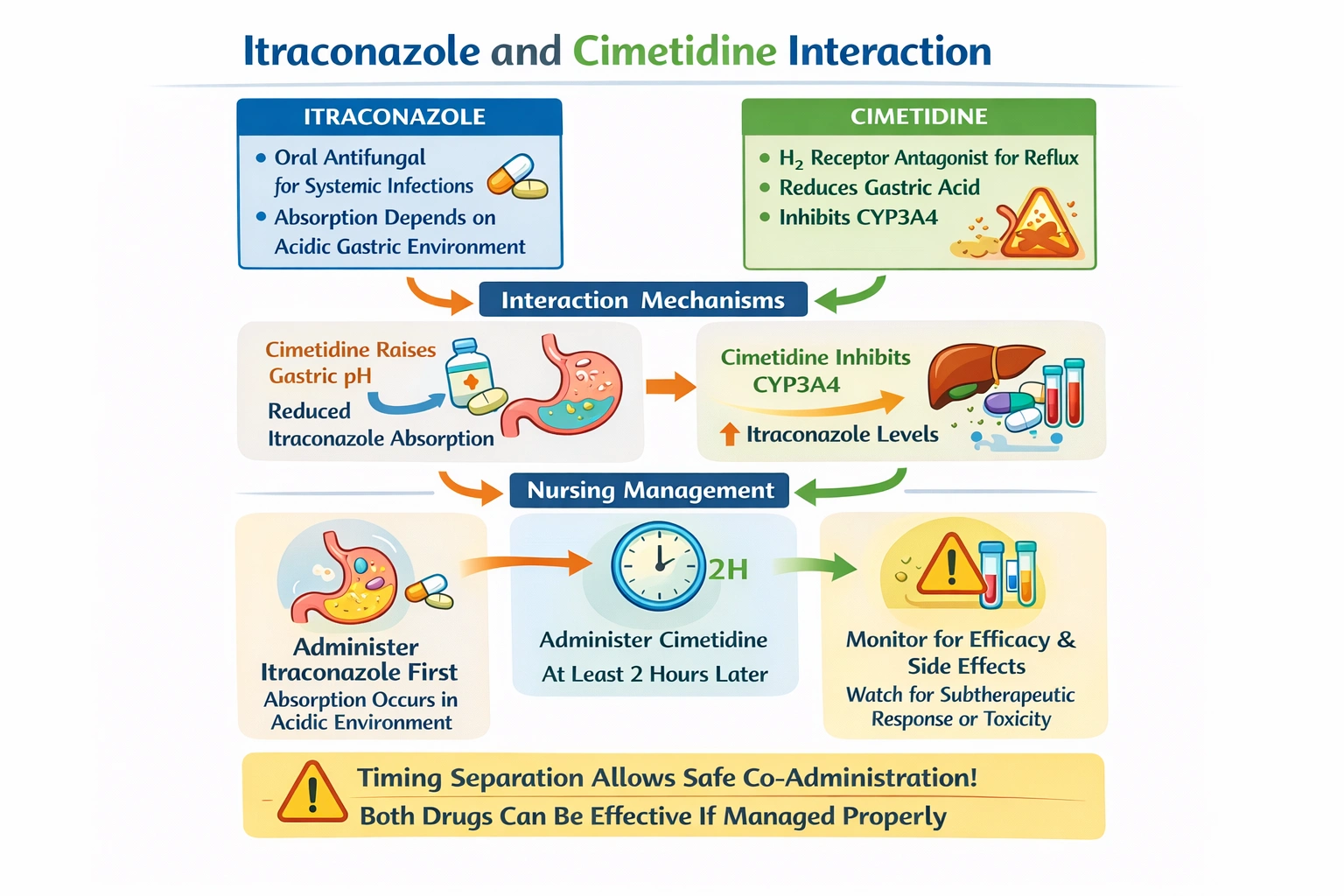
A client is taking oral itraconazole for a systemic fungal infection. The nurse reviews the medication record and notes that the client is also taking cimetidine for reflux disease. Which action should the nurse take?
A.
Administer the cimetidine at least two hours after the itraconazole
B. Don't give the cimetidine to a client receiving itraconazole
C. Administer the cimetidine with the itraconazole
D. Confer with the prescriber about a potentially hazardous interaction
Rationale
The nurse should administer the cimetidine at least two hours after the itraconazole to minimize the interaction, as cimetidine reduces gastric acid and can decrease itraconazole absorption, and also inhibits CYP enzymes potentially increasing itraconazole levels.
Itraconazole is an antifungal medication used for systemic fungal infections. Its absorption from the gastrointestinal tract is dependent on gastric acid. An acidic environment is necessary for itraconazole to dissolve and be absorbed. Cimetidine is an H2 receptor antagonist that reduces gastric acid secretion by blocking histamine at H2 receptors on parietal cells. By raising gastric pH, cimetidine can significantly decrease itraconazole absorption, potentially leading to subtherapeutic drug levels and treatment failure. Additionally, cimetidine is a potent inhibitor of cytochrome P450 enzymes, particularly CYP3A4, which metabolizes itraconazole. This inhibition could increase itraconazole levels, potentially causing toxicity. The net effect is complex and unpredictable, but the reduced absorption is a major concern. To minimize this interaction, cimetidine should be administered at least two hours after itraconazole. This allows itraconazole to be absorbed before gastric acid is reduced.
A) Administer the cimetidine at least two hours after the itraconazole
This is the correct action. Administering cimetidine after itraconazole allows the antifungal to be absorbed in an acidic environment before gastric pH is raised. This timing minimizes the impact on absorption while still allowing the patient to receive both medications.
B) Don't give the cimetidine to a client receiving itraconazole
Withholding cimetidine may not be necessary and could deprive the patient of needed treatment for reflux. The interaction can be managed with timing separation, not necessarily by avoiding one medication entirely. This action is too absolute without consulting the provider.
C) Administer the cimetidine with the itraconazole
This would worsen the interaction. Taking them together would expose itraconazole to the reduced gastric acid environment caused by cimetidine, decreasing absorption and potentially leading to treatment failure.
D) Confer with the prescriber about a potentially hazardous interaction
While conferring with the prescriber is always appropriate, the nurse already knows the interaction and the appropriate management strategy. Administering with appropriate timing is within the nurse's scope, and conferring may delay necessary medication administration. The nurse should implement the timing separation and inform the provider of the interaction and the action taken.
Conclusion
The nurse should administer cimetidine at least two hours after itraconazole to prevent reduced absorption and potential toxicity. Withholding cimetidine, giving together, or conferring without implementing timing are not optimal. Therefore, timing separation is correct, ensuring both medications can be used effectively.
A client who has erectile dysfunction asks a nurse whether sildenafil would be a suitable medication. Which aspect of this client's history would be of most concern?
A.
Occasional use of nitroglycerin
B. Mild hypertension
C. Benign prostatic hypertrophy
D. Taking finasteride
Rationale
The aspect of most concern is occasional use of nitroglycerin, as sildenafil is absolutely contraindicated with nitrates due to the risk of severe, life-threatening hypotension from synergistic vasodilation.
Sildenafil is a phosphodiesterase type 5 inhibitor used for erectile dysfunction. It works by inhibiting the enzyme that degrades cyclic guanosine monophosphate, enhancing the vasodilatory effects of nitric oxide in the corpus cavernosum, leading to increased blood flow and erection. However, PDE5 inhibitors also cause systemic vasodilation and can potentiate the hypotensive effects of other vasodilators. Nitrates, including nitroglycerin, isosorbide mononitrate, and isosorbide dinitrate, are used for angina and work by donating nitric oxide, causing vasodilation and reducing cardiac preload and afterload. When sildenafil and nitrates are combined, their vasodilatory effects are synergistic, potentially causing profound hypotension that can be life-threatening. This interaction is absolute, and sildenafil is contraindicated in patients taking any form of nitrate, regardless of frequency of use. Even occasional nitroglycerin use for angina presents a risk because the interaction can occur unpredictably.
A) Occasional use of nitroglycerin
This is a contraindication and the most concerning aspect due to risk of severe hypotension. The nurse must identify this immediately and advise the client that sildenafil cannot be used with nitrates.
B) Mild hypertension
Mild hypertension is not a contraindication to sildenafil. In fact, sildenafil may lower blood pressure slightly, which could be beneficial in some patients with hypertension.
C) Benign prostatic hypertrophy
BPH is not a contraindication. Sildenafil may actually improve urinary symptoms in some men with BPH.
D) Taking finasteride
Finasteride is used for BPH and does not interact with sildenafil. This is not concerning.
Conclusion
The most concerning aspect of the client's history for sildenafil use is occasional nitroglycerin due to risk of life-threatening hypotension. Mild hypertension, BPH, and finasteride use are not contraindications. Therefore, nitroglycerin use is the primary concern, and the nurse should advise the client that sildenafil cannot be used with nitrates.

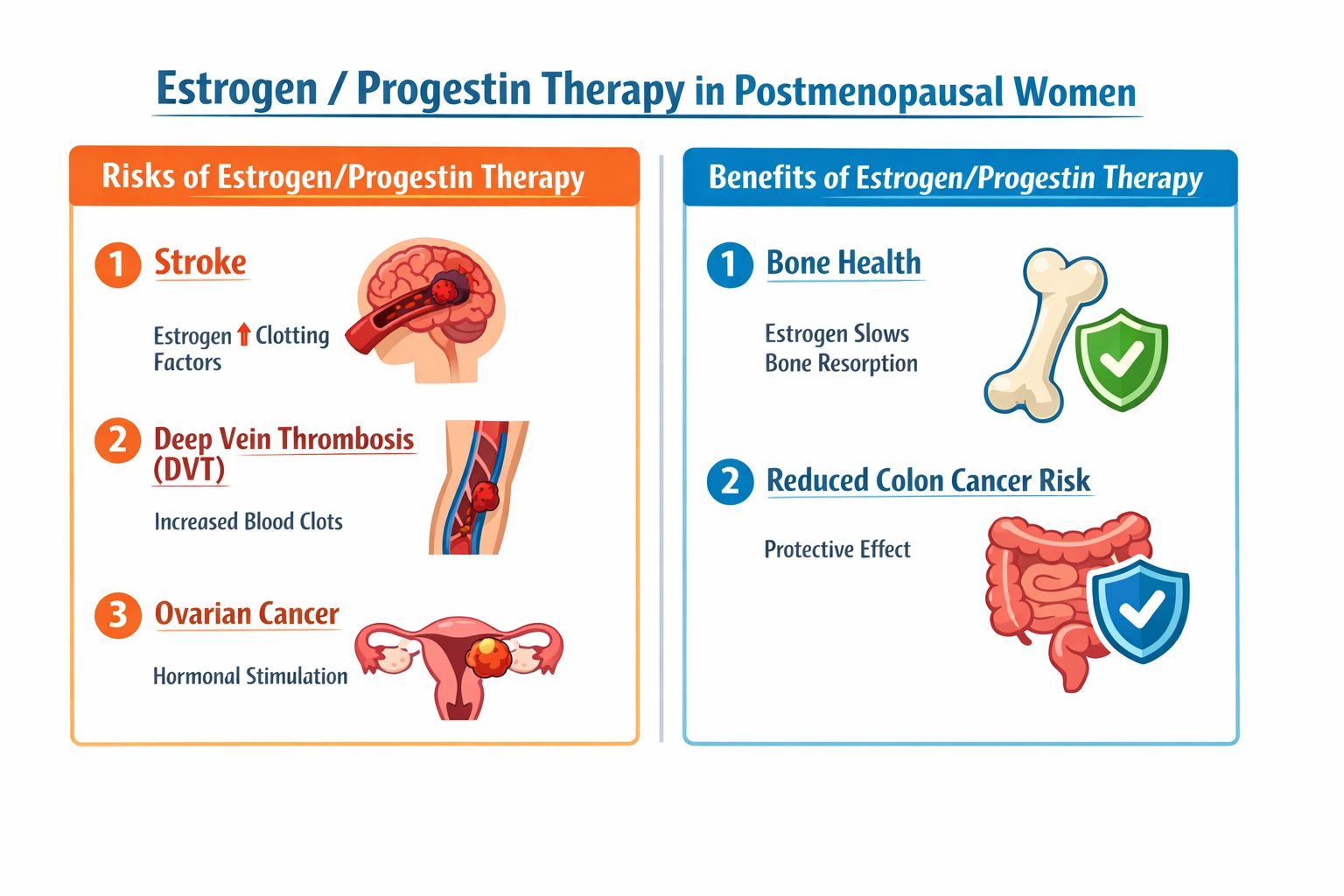
The nurse is providing client education for a postmenopausal client; which risks associated with estrogen/progestin therapy should the nurse discuss with the client?
A.
Stroke
B. DVT
C. Decreased bone density
D. Increased colon cancer
Rationale
The nurse should discuss with the client that risks associated with estrogen/progestin therapy include stroke, deep vein thrombosis, and ovarian cancer, as these have been identified in large clinical studies as potential adverse effects of hormone therapy.
Hormone therapy with estrogen and progestin has been used for decades to manage menopausal symptoms such as hot flashes, night sweats, and vaginal dryness, and to prevent osteoporosis. However, the risk-benefit profile of hormone therapy underwent significant re-evaluation following the publication of results from the Women's Health Initiative, a large, randomized, placebo-controlled trial that enrolled over 16,000 postmenopausal women. The WHI study was designed to evaluate the effects of hormone therapy on the prevention of cardiovascular disease and other conditions, as well as to assess overall risks and benefits. The estrogen-plus-progestin arm of the study was stopped early in 2002 when it was determined that the risks of therapy, including increased rates of certain conditions, outweighed the benefits for the primary prevention endpoints being studied. These findings dramatically changed clinical practice and led to current recommendations that hormone therapy be used at the lowest effective dose for the shortest duration necessary to manage menopausal symptoms, with regular re-evaluation of the need for continued treatment.
A) Stroke
Stroke is a recognized risk of estrogen/progestin therapy that the nurse must discuss with the client. The WHI study demonstrated an increased risk of ischemic stroke in women taking combined hormone therapy compared to those taking placebo. The increased risk was observed across all age groups studied, though the absolute risk was higher in older women. The mechanism by which estrogen increases stroke risk is not fully understood but may involve effects on coagulation, increasing the tendency for thrombus formation, effects on vascular inflammation, and potential direct effects on cerebral blood vessels. The increased risk translates to approximately eight additional strokes per 10,000 women per year of therapy. This risk must be balanced against the benefits of symptom relief and must be considered in the context of the individual woman's baseline cardiovascular risk factors such as hypertension, smoking, diabetes, and prior history of stroke or transient ischemic attack. The nurse should discuss this risk as part of informed consent for hormone therapy.
B) DVT
Deep vein thrombosis is a well-established risk of estrogen-containing therapy that must be discussed with any woman considering hormone therapy. Estrogen increases the hepatic production of coagulation factors, including factors VII, VIII, X, and fibrinogen, and decreases the production of anticoagulant factors such as protein S and antithrombin. This creates a prothrombotic state that increases the risk of venous thromboembolism, which includes both deep vein thrombosis and pulmonary embolism. The risk of VTE is highest in the first year of use and in women with underlying risk factors such as obesity, immobility, thrombophilia, or prior history of VTE. The WHI study found an approximate doubling of VTE risk in women taking combined hormone therapy compared to placebo, translating to about 18 additional events per 10,000 women per year. The route of estrogen administration affects this risk, with transdermal preparations associated with lower VTE risk than oral preparations because they avoid first-pass hepatic effects on coagulation factor synthesis. The nurse should discuss this risk and strategies to minimize it, such as using the lowest effective dose, considering transdermal routes, and being aware of signs and symptoms of VTE.
C) Decreased bone density
Decreased bone density is not a risk of estrogen/progestin therapy; in fact, it is the opposite. Estrogen is protective against bone loss, and hormone therapy has been shown to increase bone mineral density and reduce the risk of osteoporotic fractures. Estrogen inhibits osteoclast activity through multiple mechanisms, reducing bone resorption and slowing the rate of bone loss that accelerates after menopause. The WHI study actually demonstrated a reduction in hip and vertebral fractures in women taking hormone therapy compared to placebo. For this reason, hormone therapy is approved for the prevention of postmenopausal osteoporosis, though it is typically reserved for women who also have vasomotor symptoms, as other medications such as bisphosphonates are available for fracture prevention without the other risks of hormone therapy. The statement that hormone therapy decreases bone density is factually incorrect and reverses the actual relationship. Therefore, this should not be discussed as a risk.
D) Increased colon cancer
Increased colon cancer is not associated with combined hormone therapy. In fact, the WHI study found a decreased risk of colorectal cancer in women taking estrogen plus progestin compared to placebo. This protective effect was an unexpected finding and was one of the benefits identified in the study. The mechanism by which hormone therapy might reduce colon cancer risk is not fully understood but may involve estrogen's effects on bile acid metabolism, direct effects on colorectal mucosa, or influences on insulin-like growth factors. The reduction in risk was approximately 40%, translating to about six fewer cases per 10,000 women per year. It is important to note that this protective effect was not seen with estrogen-alone therapy in women without a uterus, suggesting that the progestin component may be important for this effect. Since colon cancer risk is decreased, not increased, the nurse should not discuss this as a risk of hormone therapy.
E) Ovarian Cancer
Ovarian cancer risk is increased with long-term use of hormone therapy and must be discussed with women considering this treatment. Multiple studies, including the WHI and other large observational studies, have shown an increased risk of ovarian cancer in women using estrogen alone or estrogen plus progestin, particularly with longer duration of use. The risk appears to increase with duration of therapy and may persist for several years after discontinuation. The absolute risk increase is relatively small, estimated at approximately one additional case per 1,000 women per five years of use, but the seriousness of ovarian cancer makes this a significant consideration. The mechanism may involve estrogen stimulation of ovarian epithelial cells or effects on ovulation and gonadotropin levels. The nurse should discuss this risk as part of comprehensive counseling about hormone therapy, particularly for women considering long-term use.
Conclusion
When educating a postmenopausal client about estrogen/progestin therapy, the nurse should discuss the risks of stroke, deep vein thrombosis, and ovarian cancer, as these have been identified in clinical studies as potential adverse effects. Decreased bone density is not a risk; estrogen protects against bone loss and reduces fracture risk. Colon cancer risk is decreased, not increased, with combined hormone therapy. Therefore, the correct risks to discuss are stroke, DVT, and ovarian cancer, along with the benefits of symptom relief and osteoporosis prevention, to allow the client to make an informed decision about hormone therapy that considers her individual risk factors and treatment goals.
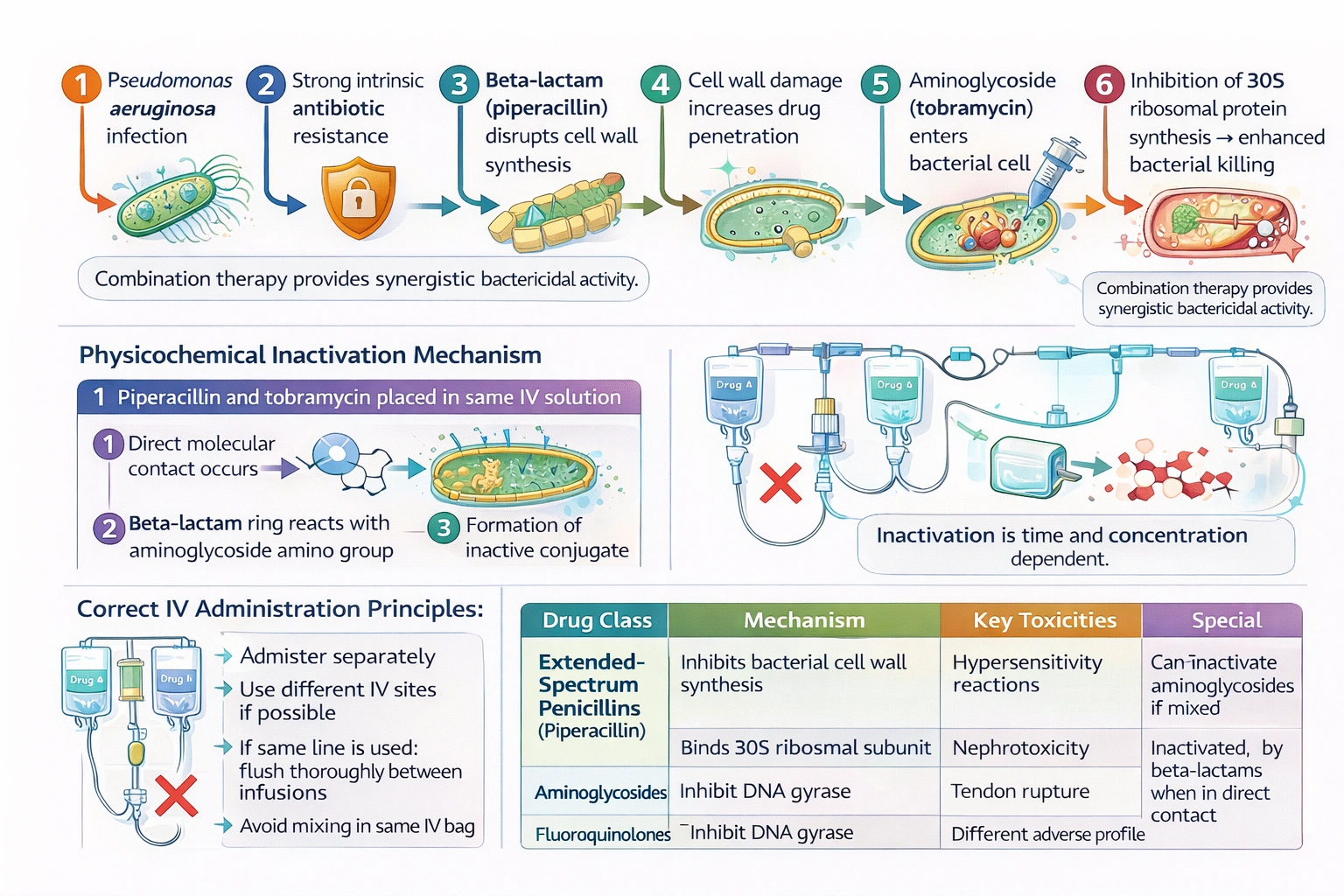
A Client has an infection caused by pseudomonas aeruginosa, and the prescriber has ordered intravenous piperacillin and tobramycin. Why might the nurse question this combination of antibiotics?
A.
This combination causes tendon rupture
B. Aminoglycosides are inactivated by penicillins
C. Aminoglycosides alone are adequate against pseudomonas. There is no need to risk penicillin allergy
D. Aminoglycosides increase the risk of penicillin allergy
Rationale
The nurse might question this combination because aminoglycosides are physically and chemically inactivated by penicillins when they come into contact with each other, particularly when mixed together in the same intravenous solution.
Pseudomonas aeruginosa is a formidable opportunistic pathogen known for its intrinsic resistance to many antibiotics and its ability to acquire additional resistance mechanisms, making infections caused by this organism challenging to treat effectively. Serious Pseudomonas infections, such as hospital-acquired pneumonia, sepsis, and infections in immunocompromised hosts, often require combination antibiotic therapy to achieve adequate bacterial killing, prevent the emergence of resistance during treatment, and improve clinical outcomes. The combination of an antipseudomonal beta-lactam antibiotic, such as piperacillin which belongs to the extended-spectrum penicillin class, and an aminoglycoside, such as tobramycin, has been a mainstay of therapy for serious Pseudomonas infections for decades due to the synergistic activity of these two drug classes. Synergy occurs because beta-lactam antibiotics disrupt bacterial cell wall synthesis, which facilitates the entry of aminoglycosides into the bacterial cell where they can then bind to the 30S ribosomal subunit and inhibit protein synthesis. While this combination is pharmacodynamically advantageous from a microbiological perspective, it presents a significant physicochemical challenge that nurses must understand to ensure safe and effective medication administration. The potential for physical incompatibility and chemical inactivation between these two drug classes requires careful attention to administration technique to maintain the therapeutic activity of both antibiotics.
A) This combination causes tendon rupture
This statement reflects confusion with an entirely different class of antibiotics. Tendon rupture, particularly affecting the Achilles tendon, is a well-documented adverse effect associated with fluoroquinolone antibiotics such as ciprofloxacin, levofloxacin, and moxifloxacin. The mechanism by which fluoroquinolones increase the risk of tendinopathy and tendon rupture is not fully understood but may involve matrix metalloproteinase inhibition, oxidative stress, or direct toxic effects on tenocytes. The risk is increased in older patients, those taking concomitant corticosteroids, and those with renal impairment, and the FDA has issued black box warnings regarding this serious adverse effect. Penicillins, including piperacillin, and aminoglycosides, including tobramycin, are not associated with tendon rupture. The client receiving piperacillin and tobramycin is not at increased risk for this specific complication, and this is not a valid reason for the nurse to question the combination. The nurse's concern must be based on accurate knowledge of the actual risks and interactions associated with these medications rather than confusing them with the side effect profiles of other antibiotic classes.
B) Aminoglycosides are inactivated by penicillins
This statement correctly identifies a significant physicochemical interaction between these two classes of antibiotics that requires careful attention to administration technique. When penicillins and aminoglycosides come into contact with each other, either in the same intravenous solution or even in the same intravenous tubing if not adequately flushed between infusions, a chemical reaction occurs that inactivates the aminoglycoside. The mechanism involves the beta-lactam ring of the penicillin undergoing nucleophilic attack by an amino group on the aminoglycoside molecule, forming a conjugate that lacks antibacterial activity. This inactivation is both time-dependent and concentration-dependent, meaning that the longer the drugs are in contact and the higher their concentrations, the greater the degree of inactivation that occurs. This interaction is clinically significant and requires that these antibiotics be administered separately. When both drugs are ordered for a patient, as is common for serious Pseudomonas infections, the nurse must ensure that they are given through different intravenous sites, or if the same line must be used, that the line is thoroughly flushed with a compatible solution between infusions to prevent any mixing of the drugs. Some sources recommend waiting at least one hour between administrations of these medications to allow for adequate clearance of the first drug from the tubing and vascular space. The inactivation can also occur in patients with renal failure, where both drugs may accumulate and have prolonged contact in the bloodstream, requiring even more careful monitoring. The nurse who understands this interaction will question the order if it specifies mixing the drugs together or if it does not include specific instructions for proper separation of administration.
C) Aminoglycosides alone are adequate against pseudomonas. There is no need to risk penicillin allergy
This statement does not reflect the standard of care for treating serious Pseudomonas infections. While aminoglycosides do have activity against Pseudomonas aeruginosa, using them as monotherapy for serious infections is generally not recommended for several important reasons. First, aminoglycosides have a narrow therapeutic index and can cause significant toxicity, particularly nephrotoxicity and ototoxicity, which limits the doses that can be safely administered. Second, resistance can emerge during monotherapy with aminoglycosides, compromising treatment efficacy. Third, the combination of an antipseudomonal beta-lactam with an aminoglycoside provides synergistic killing, meaning that the combined effect is greater than the sum of their individual effects. This synergy allows for potentially lower doses of the nephrotoxic aminoglycoside while still achieving adequate bacterial killing. Fourth, combination therapy reduces the risk of resistance developing during treatment because organisms resistant to one drug may still be susceptible to the other. For these reasons, combination therapy with a beta-lactam and an aminoglycoside is considered the standard of care for serious Pseudomonas infections such as sepsis, hospital-acquired pneumonia, and infections in neutropenic patients. The concern about penicillin allergy is valid and should be addressed through careful allergy assessment and, if necessary, skin testing or alternative antibiotic selection, but it does not negate the therapeutic benefit of the combination. The nurse should not question the combination on this basis, as the use of two agents is clinically indicated and supported by evidence.
D) Aminoglycosides increase the risk of penicillin allergy
This statement has no basis in pharmacology or immunology. Penicillin allergy is an immune-mediated hypersensitivity reaction that occurs when the immune system recognizes penicillin or its metabolites as antigens and mounts an inappropriate response. This response is unrelated to concomitant administration of other medications and is not influenced by the presence or absence of aminoglycosides. Allergic reactions to penicillins can range from mild maculopapular rashes to severe, life-threatening anaphylaxis, and they occur through mechanisms involving IgE antibodies, T-cell mediated responses, or other immune pathways depending on the type of reaction. Aminoglycosides do not potentiate these immune responses, nor do they increase the likelihood of sensitization to penicillins. While allergic reactions can occur with any medication, and patients may experience allergic reactions to both drugs independently, there is no known interaction whereby aminoglycosides increase the risk or severity of penicillin allergy. This is not a valid reason to question the combination, and the nurse who raises this concern would be acting on misinformation rather than accurate pharmacological knowledge.
Conclusion
The nurse might question the combination of intravenous piperacillin and tobramycin because aminoglycosides are physically and chemically inactivated by penicillins when they come into contact, requiring careful separation of administration to maintain therapeutic efficacy. The statement about tendon rupture reflects confusion with fluoroquinolone antibiotics and is not applicable to this combination. The claim that aminoglycosides alone are adequate against Pseudomonas is incorrect and contradicts the evidence supporting combination therapy for serious infections. The assertion that aminoglycosides increase penicillin allergy risk has no pharmacological basis. Therefore, the correct concern is the inactivation of the aminoglycoside by the penicillin, which necessitates that the drugs be administered separately, with thorough flushing of intravenous lines between infusions or through different sites entirely, to ensure that both antibiotics reach the patient in their active forms and provide the intended synergistic effect against Pseudomonas aeruginosa.
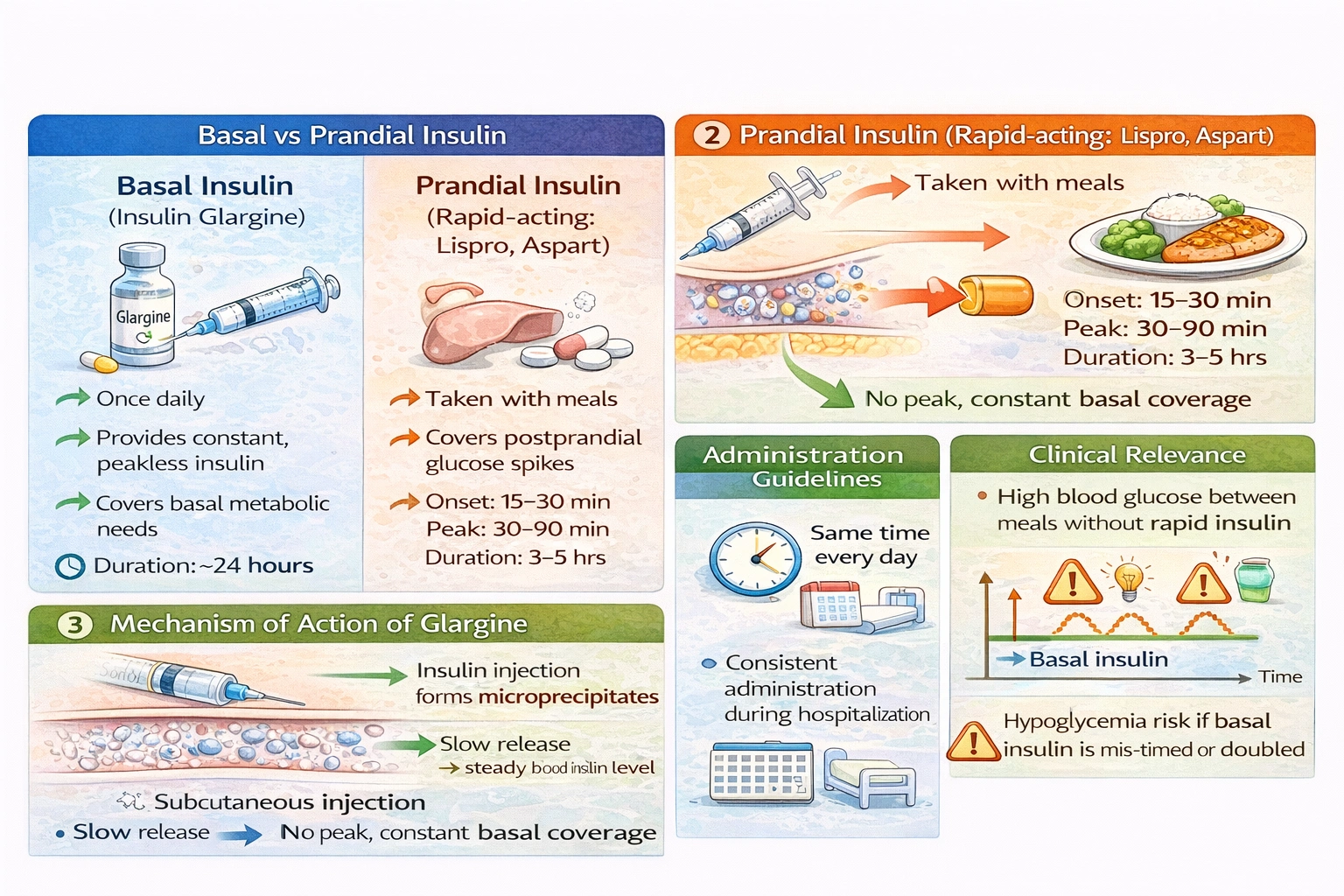
Insulin glargine is prescribed for a hospitalized client who has diabetes. When will the nurse expect to administer this drug?
A.
After meals and at bedtime
B. Once-daily at the same time every day
C. With meals
D. Approximately 15 to 30 minutes before each meal
Rationale
The nurse will expect to administer insulin glargine once-daily at the same time every day, as this long-acting basal insulin analog is designed to provide a relatively constant level of insulin over approximately 24 hours to cover basal metabolic needs.
Insulin therapy is essential for the management of type 1 diabetes and is often required for type 2 diabetes when oral agents are insufficient to achieve glycemic control. Modern insulin therapy aims to mimic the body's normal physiologic insulin secretion, which consists of two components: basal insulin secretion, which provides a constant low level of insulin to regulate hepatic glucose production and maintain stable blood glucose levels between meals and during fasting periods such as overnight, and prandial insulin secretion, which provides rapid bursts of insulin in response to meals to handle the glucose load from food. Different insulin formulations have been developed to approximate these different components of physiologic insulin secretion. Insulin glargine is a long-acting basal insulin analog specifically designed to provide the basal component. Understanding its pharmacokinetic profile is essential for correct administration and optimal glycemic control.
A) After meals and at bedtime
This timing is not appropriate for insulin glargine and would represent a misunderstanding of its role in diabetes management. Dosing after meals and at bedtime would result in multiple daily injections, which is not the intended use of a long-acting basal insulin. This schedule might be appropriate for a combination of rapid-acting insulin given with meals and an intermediate-acting insulin given at bedtime, but not for glargine alone. Administering glargine after meals would not provide the consistent basal coverage needed between meals, and giving it at both times would result in excessive dosing and severe hypoglycemia. The once-daily nature of glargine means that a single dose provides coverage for the entire 24-hour period, and additional doses are not needed or safe.
B) Once-daily at the same time every day
This is the correct administration schedule for insulin glargine. Insulin glargine is a long-acting basal insulin analog that has been modified to have a duration of action of approximately 24 hours with no pronounced peak. This is achieved through a slight modification of the human insulin molecule, where the amino acid asparagine at position A21 is replaced with glycine, and two arginines are added to the C-terminal of the B-chain. These changes shift the isoelectric point, making glargine less soluble at neutral pH. When injected into the subcutaneous tissue, which has a neutral pH, glargine forms microprecipitates that slowly dissolve and release insulin into the circulation over an extended period. This provides a relatively constant, peakless level of insulin that mimics basal insulin secretion. Once-daily dosing at the same time each day maintains stable insulin levels and optimizes glycemic control. The nurse should establish a consistent administration time, such as with breakfast or at bedtime, and maintain that schedule throughout the hospital stay to ensure consistency and prevent fluctuations in blood glucose.
C) With meals
This timing is appropriate for rapid-acting insulins such as insulin lispro, aspart, or glulisine, which are designed to cover the glycemic excursion from meals. These insulins have an onset of action within 15 minutes, peak at 30 to 90 minutes, and duration of 3 to 5 hours, making them ideal for administration just before or with meals to match the rise in blood glucose from food absorption. Insulin glargine is not intended for prandial coverage and would not provide the rapid onset needed to control postprandial glucose. Administering it with meals would not provide the continuous basal coverage needed between meals and would result in improper insulin management with inadequate coverage during fasting periods.
D) Approximately 15 to 30 minutes before each meal
This timing describes administration of rapid-acting insulins given before meals to cover carbohydrate intake. The 15 to 30 minute interval allows the insulin to begin working as food is being absorbed, providing optimal coverage of postprandial glucose. Insulin glargine is not a mealtime insulin and should not be given on this schedule. Administering glargine before each meal would result in multiple daily doses of a long-acting insulin, leading to severe and prolonged hypoglycemia as the drug accumulates and exerts its effects continuously. This represents a fundamental misunderstanding of the different roles of basal and prandial insulins.
Conclusion
The nurse will administer insulin glargine once-daily at the same time every day due to its 24-hour duration of action as a basal insulin analog that provides constant, peakless coverage of basal metabolic needs. Dosing after meals and at bedtime, with meals, or before each meal describes schedules for other insulin types such as intermediate-acting or rapid-acting insulins. Therefore, once-daily at a consistent time is the correct administration schedule for insulin glargine, and the nurse should ensure this schedule is maintained throughout the client's hospital stay.
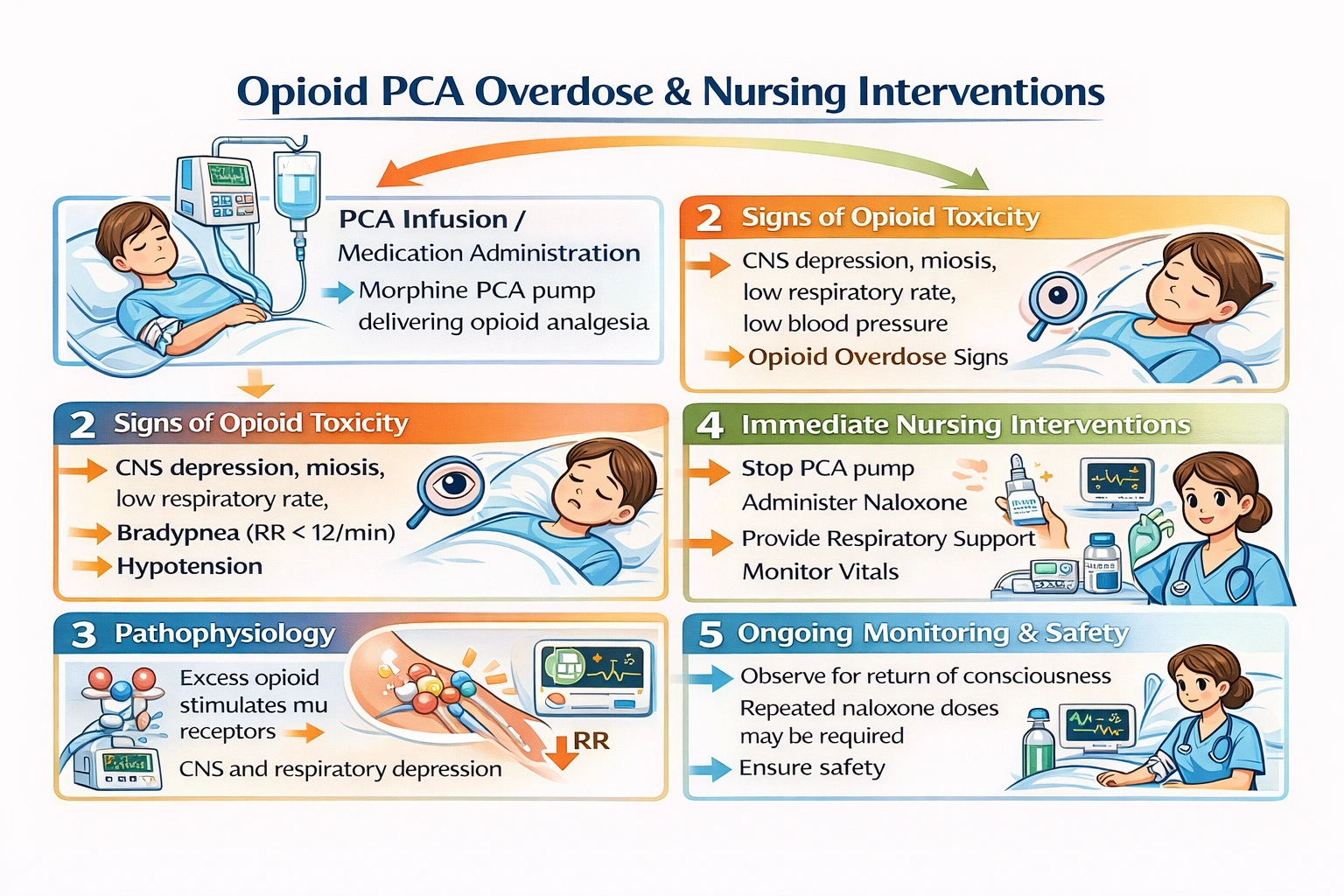
A client on a morphine PCA pump is noted to be drowsy and lethargic with pinpoint pupils and the following vitals; pulse 84 beats/min, respiratory rate 10 breaths/min, bp 90/50 mm Hg. What are the nurse's best actions?
A.
Discuss possible opiate dependence with the client's provider
B. Prepare to administer naloxone and provide respiratory support
C. Note the effectiveness of the analgesia in the client's chart
D. Encourage the client to turn over, and cough and take deep breaths
Rationale
The nurse's best actions are to prepare to administer naloxone and provide respiratory support, as the client is exhibiting classic signs of opioid overdose or toxicity including central nervous system depression, miosis, bradypnea, and hypotension, which constitute a medical emergency requiring immediate intervention.
Patient-controlled analgesia with morphine is a common method of postoperative pain management that allows patients to self-administer small doses of opioid medication within prescribed limits. While PCA pumps have safety features designed to prevent overdose, including lockout intervals and maximum dose limits, opioid toxicity can still occur due to patient factors such as advanced age, renal impairment, or altered pharmacokinetics, or due to pump malfunction or programming errors. The signs of opioid toxicity represent a progression from therapeutic effect to adverse effect to toxic effect. Early signs may include increasing sedation, while more advanced toxicity includes the classic triad of coma, pinpoint pupils, and respiratory depression. The client in this scenario is displaying multiple signs of significant opioid toxicity: drowsiness and lethargy indicate central nervous system depression, pinpoint pupils are classic miosis from mu receptor activation in the Edinger-Westphal nucleus, respiratory rate of 10 is significantly below normal indicating respiratory depression, and hypotension reflects cardiovascular effects. This constellation of findings indicates that the client is receiving more opioid than they can safely tolerate and requires immediate intervention to prevent progression to respiratory arrest and death.
A) Discuss possible opiate dependence with the client's provider
This response is inappropriate and demonstrates failure to recognize an acute emergency. The client is showing signs of opioid toxicity, not dependence. Dependence is a physiological state characterized by the development of withdrawal symptoms upon abrupt discontinuation, which is distinct from toxicity. Discussing dependence at this moment does nothing to address the life-threatening respiratory depression and hypotension. The priority is to reverse the overdose and support vital functions, not to have a theoretical discussion about dependence. The nurse who focuses on dependence rather than acute intervention is missing the immediate danger and could be liable for patient harm.
B) Prepare to administer naloxone and provide respiratory support
This is the correct and appropriate response that addresses the life-threatening emergency. Naloxone is a competitive opioid antagonist that rapidly reverses opioid effects by binding to mu receptors and displacing agonist molecules. It should be administered immediately according to protocol or provider order. While preparing naloxone, the nurse should also initiate respiratory support measures. This may include stimulating the client to breathe, administering oxygen, and preparing for bag-valve-mask ventilation if respiratory effort is inadequate. The nurse should stay with the client, monitor vital signs closely, and be prepared for additional interventions if needed. After naloxone administration, the client should show rapid improvement in level of consciousness and respiratory rate, though repeated doses may be needed because naloxone has a shorter duration of action than many opioids. The nurse must also consider that the PCA pump should be stopped or removed to prevent continued opioid administration.
C) Note the effectiveness of the analgesia in the client's chart
This response is dangerously inappropriate. The client is experiencing opioid toxicity, not effective analgesia. Documenting effectiveness while ignoring obvious signs of overdose is a serious error that could result in client harm or death. The client's drowsiness, lethargy, and respiratory depression are not signs of good pain control but of excessive opioid effect. The nurse must recognize the emergency and act accordingly, not document and ignore.
D) Encourage the client to turn over, and cough and take deep breaths
This response is grossly inadequate for the severity of the situation. The client has significant respiratory depression with a rate of 10 and is lethargic, indicating they are not fully responsive. Simple encouragement to deep breathe will not reverse opioid-induced respiratory depression, and the client may not be able to follow commands. This response delays life-saving intervention and could allow the client to deteriorate further. Postoperative turning, coughing, and deep breathing are important for preventing atelectasis and pneumonia, but they are not appropriate when a patient is showing signs of opioid toxicity requiring immediate reversal.
Conclusion
When a client on morphine PCA presents with drowsiness, lethargy, pinpoint pupils, respiratory rate of 10, and hypotension, the nurse's best actions are to prepare to administer naloxone and provide respiratory support to reverse opioid toxicity and prevent respiratory arrest. Discussing dependence, noting analgesia effectiveness, or encouraging deep breathing are all inappropriate and dangerous responses that delay life-saving treatment. Therefore, naloxone administration and respiratory support are the correct actions in this emergency situation.
A client who is taking calcium supplements receives a prescription for ciprofloxacin for a respiratory infection. What must the nurse include in client teaching?
A.
Consume extra fluids while taking the ciprofloxacin to prevent hypercalciuria
B. Take the calcium either six hours before or two hours after taking the ciprofloxacin
C. Stop taking the calcium supplements while taking the ciprofloxacin
D. Take the two medications together to increase the absorption of both
Rationale
The nurse must instruct the client to take the calcium either six hours before or two hours after taking the ciprofloxacin to prevent a chelation interaction that significantly reduces ciprofloxacin absorption and can lead to therapeutic failure.
Ciprofloxacin is a fluoroquinolone antibiotic widely used for respiratory infections, urinary tract infections, and other bacterial infections. Its mechanism of action involves inhibition of bacterial DNA gyrase and topoisomerase IV, enzymes essential for bacterial DNA replication, transcription, and repair. For ciprofloxacin to be effective, it must be adequately absorbed from the gastrointestinal tract into the systemic circulation. However, ciprofloxacin has a significant drug interaction with divalent and trivalent cations, including calcium, magnesium, aluminum, iron, and zinc. These cations form insoluble chelates with ciprofloxacin in the gut, meaning that the drug binds to the cation and forms a complex that cannot be absorbed. This can reduce ciprofloxacin bioavailability by up to 50% or more, potentially leading to subtherapeutic antibiotic levels and treatment failure.
A) Consume extra fluids while taking the ciprofloxacin to prevent hypercalciuria
This instruction is not relevant to the drug interaction. Ciprofloxacin does not cause hypercalciuria, which is excess calcium in the urine. Adequate hydration is generally recommended with ciprofloxacin to prevent crystalluria, which is formation of crystals in the urine that can damage the kidneys, but this is unrelated to calcium supplements. This instruction does not address the critical drug interaction between ciprofloxacin and calcium and would not prevent the chelation that reduces antibiotic absorption.
B) Take the calcium either six hours before or two hours after taking the ciprofloxacin
This instruction is correct and addresses the chelation interaction. Separating the doses by at least two hours after or six hours before ensures that the ciprofloxacin is absorbed before encountering the calcium in the gut. The two-hour window after ciprofloxacin allows time for absorption before calcium is introduced. The six-hour window before ensures that any calcium from a previous dose has moved through the gut and is not present when ciprofloxacin is taken. This spacing maintains antibiotic efficacy while allowing the client to continue necessary calcium supplementation. The nurse should emphasize the importance of this timing and explain why it matters.
C) Stop taking the calcium supplements while taking the ciprofloxacin
Stopping calcium supplements may not be necessary and could be detrimental if the client requires calcium for bone health, osteoporosis prevention, or other indications. Separating the doses adequately is usually sufficient to avoid the interaction without discontinuing necessary supplements. This instruction is overly restrictive and may not be appropriate for all clients. The preferred approach is to adjust timing, not to discontinue.
D) Take the two medications together to increase the absorption of both
This instruction is dangerous and incorrect. Taking them together will decrease ciprofloxacin absorption, not increase it. There is no enhancement of absorption for either medication. This would lead to antibiotic failure and potentially resistant organisms. The nurse must never provide this instruction.
Conclusion
When a client taking calcium supplements receives ciprofloxacin, the nurse must teach to take calcium either six hours before or two hours after ciprofloxacin to prevent chelation and maintain antibiotic efficacy. Extra fluids for hypercalciuria, stopping calcium entirely, or taking them together are all incorrect instructions. Therefore, the correct teaching is about appropriate dose separation, which preserves the effectiveness of the antibiotic while allowing continuation of necessary calcium supplementation.
A nurse is reviewing the chart of an adult male client who has been taking oral androgens. Which assessment would warrant notifying the provider?
A.
Increased facial hair
B. Jaundice
C. Acne
D. Increased libido
Rationale
Jaundice would warrant notifying the provider in a client taking oral androgens, as this finding indicates potential hepatotoxicity, a serious adverse effect that requires immediate evaluation and possible discontinuation of therapy.
Oral androgens, which include testosterone derivatives and other anabolic steroids, are used for various indications including male hypogonadism, delayed puberty, and certain wasting conditions. These medications have significant effects on the liver because they are metabolized hepatically and, particularly with oral formulations, undergo first-pass metabolism that exposes the liver to high drug concentrations. Hepatotoxicity is a well-recognized adverse effect of oral androgens, with manifestations ranging from mild, reversible liver enzyme elevations to more serious conditions such as cholestatic jaundice, peliosis hepatis, and hepatic adenomas or carcinomas. Cholestatic jaundice occurs when drug-induced injury impairs bile flow, leading to accumulation of bilirubin and visible yellowing of the skin and sclera.
A) Increased facial hair
Increased facial hair is an expected androgenic effect of testosterone therapy. It reflects the desired action of the medication in promoting male secondary sexual characteristics. While it may be bothersome to some clients, it does not indicate a serious adverse reaction and would not warrant provider notification unless it is causing significant distress.
B) Jaundice
Jaundice is a sign of liver dysfunction and potential hepatotoxicity from oral androgens. It indicates that bilirubin is accumulating in the blood, usually due to impaired liver function or bile flow. This requires immediate provider notification for further evaluation, which may include liver function tests, bilirubin levels, and assessment of synthetic function. The provider may need to discontinue the medication or switch to a different formulation, such as transdermal testosterone, which avoids first-pass hepatic metabolism and has lower hepatotoxicity risk.
C) Acne
Acne is a common and expected side effect of androgen therapy due to increased sebum production and sebaceous gland activity. It is not a sign of serious toxicity and does not require provider notification unless severe or causing significant distress. Acne can often be managed with topical treatments or adjustments in the medication regimen if necessary.
D) Increased libido
Increased libido is an expected therapeutic and androgenic effect of testosterone therapy. It reflects the desired action of the medication and does not indicate a problem. This would not warrant provider notification.
Conclusion
Jaundice is the assessment finding that warrants notifying the provider in a client taking oral androgens, as it indicates potential hepatotoxicity requiring immediate evaluation. Increased facial hair, acne, and increased libido are expected androgenic effects. Therefore, jaundice is the correct finding to report, and the nurse should act promptly to ensure appropriate evaluation and management of this potentially serious adverse effect.
Which of these statements indicates the client's understanding of nitroglycerin self-care practices?
A.
I can take nitroglycerin three times, but I need to space them three minutes apart
B. I should stop what I am doing and sit down before I take nitroglycerin for chest pain
C. I should keep unopened bottles of nitroglycerin in the freezer
D. I should wait until I have taken three nitroglycerin tablets before I call for help
Rationale
The client demonstrates understanding by stating they should stop what they are doing and sit down before taking nitroglycerin for chest pain, as this action prevents injury from the potential hypotension and dizziness that can occur with this medication's vasodilatory effects.
Nitroglycerin is a vasodilator used for the acute relief of angina pectoris, working through multiple mechanisms to restore the balance between myocardial oxygen supply and demand. When administered sublingually, nitroglycerin is rapidly absorbed and causes relaxation of vascular smooth muscle, particularly in the venous system, which reduces preload by decreasing the volume of blood returning to the heart. It also causes some arterial vasodilation, reducing afterload, and dilates coronary arteries, potentially improving blood flow to ischemic areas of the myocardium. While these effects are therapeutic for angina, they also produce predictable hemodynamic consequences that require specific patient actions for safety. The vasodilation can lead to a drop in blood pressure, which may be more pronounced when the patient is standing due to the effects of gravity on venous return. This orthostatic hypotension can cause dizziness, lightheadedness, and even syncope, creating a fall risk. By stopping activity, which reduces myocardial oxygen demand, and sitting or lying down before taking the medication, the patient ensures that if hypotension occurs, they are already in a safe position and will not fall and sustain injury. This simple but crucial self-care measure is essential for all patients using nitroglycerin.
A) I can take nitroglycerin three times, but I need to space them three minutes apart
This statement reveals a misunderstanding of the correct timing for nitroglycerin administration that could lead to inadequate treatment of an anginal episode. The standard and widely taught protocol for nitroglycerin use in acute angina is to take one dose, wait five minutes, and if chest pain is not relieved, take a second dose. If after another five minutes there is still no relief, a third dose should be taken and emergency medical services should be activated immediately. The five-minute interval is based on the time it takes for the medication to reach peak effect and for the patient to assess whether relief has been achieved. A three-minute interval does not allow adequate time for the medication to work and could result in the patient taking multiple doses unnecessarily or delaying appropriate medical intervention. The client who believes three minutes is correct may not wait long enough between doses, potentially taking more medication than needed without allowing time to assess effectiveness, or may not recognize the appropriate time to seek emergency care.
B) I should stop what I am doing and sit down before I take nitroglycerin for chest pain
This statement accurately reflects proper self-care practices for nitroglycerin use and demonstrates the client's understanding of an important safety measure. When angina occurs, the immediate response should be to stop all activity, as continuing to exert oneself increases myocardial oxygen demand and can worsen ischemia. Sitting or lying down serves two important purposes. First, it reduces the work of the heart by decreasing the metabolic demands of the body. Second, it positions the patient safely for the potential hypotensive effects of nitroglycerin. The medication causes vasodilation that can lead to a drop in blood pressure, and if the patient is standing, this can result in dizziness, lightheadedness, and falls. By sitting or reclining before taking the medication, the patient eliminates the risk of injury from falling. The client who understands this sequence demonstrates appropriate knowledge of both the therapeutic use of nitroglycerin and the necessary precautions to ensure safety during an anginal episode.
C) I should keep unopened bottles of nitroglycerin in the freezer
This statement reflects a misunderstanding of proper nitroglycerin storage that could lead to medication degradation and loss of effectiveness. Nitroglycerin is a volatile compound that is sensitive to heat, light, and moisture. It must be stored in its original glass container, which is designed to protect it from light and to minimize exposure to air. The bottle should be kept tightly closed because nitroglycerin can evaporate and also can be absorbed by certain types of plastic. However, refrigeration or freezing is not recommended and can actually be harmful. Extreme cold can affect the stability of the medication, and condensation that forms when the bottle is removed from the freezer can introduce moisture, which accelerates degradation. Nitroglycerin should be stored at room temperature, away from heat and direct light, in a cool, dry place. The client also needs to know that nitroglycerin has a limited shelf life and should be replaced according to the expiration date or every six months after opening, whichever comes first. The belief that freezing preserves the medication is incorrect and could result in the client using ineffective nitroglycerin during an anginal episode.
D) I should wait until I have taken three nitroglycerin tablets before I call for help
This statement contains a dangerous misunderstanding about when to seek emergency care during an anginal episode. While the standard protocol does involve taking up to three doses at five-minute intervals, the decision to call for help should not be delayed until after the third dose is taken. The correct approach is that if chest pain is not relieved after one dose, the patient should take a second dose after five minutes, and if still no relief after another five minutes, a third dose should be taken and emergency services should be called immediately. However, there are important exceptions to this sequence. If the chest pain is severe, if it is accompanied by other concerning symptoms such as shortness of breath, nausea, diaphoresis, or lightheadedness, or if the patient has any reason to believe this episode is different from their usual angina, they should call for help immediately without waiting through multiple doses. Additionally, if the patient has taken one dose and has no relief after five minutes, they should not wait for the third dose to call if they are concerned. The statement as written implies that calling for help only occurs after all three doses are taken, which could delay critical intervention for a myocardial infarction. The client needs to understand that seeking emergency care is appropriate at any point if symptoms are severe or not improving as expected.
Conclusion
The client demonstrates understanding of nitroglycerin self-care practices by stating they should stop activity and sit down before taking the medication, recognizing that this prevents injury from potential hypotension and dizziness. The statement about three-minute intervals reflects incorrect timing for dosing. The belief that nitroglycerin should be stored in the freezer is incorrect and could lead to medication degradation. The statement about waiting until three doses are taken before calling for help could dangerously delay emergency care. Therefore, the correct statement is about stopping activity and sitting down, reflecting appropriate knowledge of both therapeutic use and safety precautions with nitroglycerin.

What should the nurse advise a client on spironolactone regarding necessary self-care?
A.
Discontinue taking this medication if you feel well
B. Avoid salt substitutes
C. Check your pulse before taking this medication
D. Add as many fruits and vegetables to your diet as possible
Rationale
The nurse should advise a client on spironolactone to avoid salt substitutes, as these often contain potassium chloride and can cause dangerous hyperkalemia when combined with this potassium-sparing diuretic.
Spironolactone is a potassium-sparing diuretic that works by antagonizing aldosterone at the distal convoluted tubule of the nephron. Aldosterone normally promotes sodium reabsorption and potassium secretion. By blocking aldosterone, spironolactone increases sodium and water excretion while retaining potassium. This makes it effective for conditions such as heart failure, hypertension, and cirrhosis with ascites, but it also creates a significant risk of hyperkalemia, or elevated potassium levels. Hyperkalemia can cause muscle weakness, fatigue, and potentially life-threatening cardiac arrhythmias, including heart block and ventricular fibrillation. Patients taking spironolactone must be careful to avoid excessive potassium intake from any source. Salt substitutes are a particular concern because they are often marketed to individuals with hypertension or heart failure as a way to reduce sodium intake. However, many salt substitutes use potassium chloride instead of sodium chloride to provide a salty taste without the sodium. When a patient taking spironolactone uses these potassium-containing salt substitutes, they can unknowingly consume significant amounts of potassium, potentially pushing their levels into the dangerous range.
A) Discontinue taking this medication if you feel well
This is incorrect and potentially dangerous advice. Antihypertensive and diuretic medications must be taken consistently even when the patient feels well, as they are controlling underlying conditions that may not cause symptoms. Discontinuing spironolactone without provider guidance could lead to worsening of heart failure, hypertension, or ascites. The patient should be advised to take the medication as prescribed and to discuss any concerns with their provider.
B) Avoid salt substitutes
This is correct and essential teaching for anyone taking spironolactone. The nurse should explain that many salt substitutes contain potassium chloride and can increase the risk of hyperkalemia. The patient should read food labels carefully, avoid potassium-containing salt substitutes, and use herbs and spices for flavoring instead. If the patient has questions about specific products, they should consult their provider or pharmacist. This simple precaution can prevent dangerous elevations in potassium levels.
C) Check your pulse before taking this medication
Checking pulse is not required for spironolactone. This instruction is more appropriate for medications that affect heart rate, such as digoxin or beta-blockers. Spironolactone does not typically affect pulse rate directly, and pulse monitoring is not part of routine self-care for this medication. Providing this instruction would not be harmful but would not address the most important safety concern.
D) Add as many fruits and vegetables to your diet as possible
This advice could be harmful for a patient taking spironolactone. While fruits and vegetables are generally healthy and recommended for most people, many are high in potassium and should be consumed in moderation by patients on potassium-sparing diuretics. Foods such as bananas, oranges, potatoes, tomatoes, spinach, and avocados are particularly high in potassium. The patient does not need to avoid these foods entirely but should be advised to maintain a consistent intake and not to dramatically increase consumption without monitoring. Telling them to add as many as possible could lead to excessive potassium intake and hyperkalemia.
Conclusion
The nurse should advise a client on spironolactone to avoid salt substitutes due to the risk of hyperkalemia from potassium-containing products. Discontinuing if feeling well is incorrect. Pulse checking is not required. Adding unlimited fruits and vegetables could be harmful. Therefore, avoiding salt substitutes is correct, protecting the client from potentially dangerous potassium elevation.

The nurse working on a high-acuity medical-surgical unit is prioritizing care for four clients who were just admitted. Which client should the nurse assess first?
A.
The client with a blood pressure of 136/92 mm Hg who complains of having a headache
B. The NPO client with a blood glucose level of 80 mg/dL who just received 20 units of 70/30 insulin
C. The client with an allergy to penicillin who is receiving an infusion of vancomycin
D. The client with a pulse of 62 beats/min about to receive digoxin
Rationale
The nurse should assess first the NPO client with a blood glucose of 80 mg/dL who just received 20 units of 70/30 insulin, as this client is at immediate risk for severe hypoglycemia requiring prompt intervention.
Prioritizing care for multiple patients is a fundamental nursing skill that requires rapid assessment of acuity and risk. The nurse must identify which patient is at greatest risk for immediate deterioration and address that need first. In this scenario, the NPO client who received 20 units of 70/30 insulin is at highest risk. 70/30 insulin is a mixed insulin containing 70% intermediate-acting insulin (NPH) and 30% rapid-acting insulin (regular). The rapid-acting component will begin working within 30 minutes and peak in 2 to 4 hours, while the intermediate component will have a longer duration. The patient is NPO, meaning nothing by mouth, so there is no food intake to provide glucose and counter the insulin effect. The blood glucose of 80 mg/dL is already at the lower end of the normal range and will decrease further as the insulin peaks. This patient is at high risk for hypoglycemia, which can progress rapidly to loss of consciousness, seizures, and permanent neurological damage if not treated.
A) The client with a blood pressure of 136/92 mm Hg who complains of having a headache
This BP is mildly elevated but not in a hypertensive emergency range. Headache could have many causes, including stress, pain, or the elevated BP itself. While this patient requires assessment, they are not at immediate risk for life-threatening deterioration compared to the patient at risk for hypoglycemia.
B) The NPO client with a blood glucose level of 80 mg/dL who just received 20 units of 70/30 insulin
This patient requires immediate assessment. The nurse should check the blood glucose immediately, assess for signs of hypoglycemia, and be prepared to administer fast-acting carbohydrates. If the patient is unable to take oral carbohydrates, IV dextrose may be needed. This is a time-sensitive situation requiring prompt intervention.
C) The client with an allergy to penicillin who is receiving an infusion of vancomycin
Vancomycin infusion requires monitoring for infusion reactions such as red man syndrome, but there is no immediate emergency indicated. The nurse should ensure the infusion is running at the appropriate rate and monitor for signs of reaction, but this is not the highest priority.
D) The client with a pulse of 62 beats/min about to receive digoxin
A pulse of 62 is within normal range and not a contraindication to digoxin. Digoxin is typically held for rates below 60, so this patient is safe to receive the medication. This is stable and not a priority.
Conclusion
The nurse should assess first the NPO client who received insulin and has a blood glucose of 80 mg/dL due to high risk of hypoglycemia. The other clients have stable or non-urgent findings. Therefore, the insulin recipient is the priority, requiring immediate assessment and possible intervention to prevent severe hypoglycemia.
A nurse is administering morphine sulfate to a postoperative client. Which are appropriate routine nursing actions when giving this drug?
A.
Requesting an order for methylnaltrexone to prevent constipation
B. Evaluating for urinary retention every 4-6 hours
C. Counting respirations before and after giving the medication
D. Assist with ambulation
Rationale
Appropriate routine nursing actions when administering morphine include evaluating for urinary retention, counting respirations before and after, and assisting with ambulation, as these address common opioid side effects and safety concerns.
Morphine is an opioid analgesic used for moderate to severe pain, particularly postoperatively. It works by binding to mu receptors in the central nervous system, altering pain perception and response. However, opioid receptors are also located throughout the body, leading to predictable side effects that require nursing assessment and intervention. Urinary retention can occur due to increased smooth muscle tone in the bladder and increased sphincter tone. Respiratory depression is the most serious adverse effect, as opioids depress the brainstem respiratory centers. Sedation and dizziness increase fall risk. Routine nursing actions should address these predictable effects.
A) Requesting an order for methylnaltrexone to prevent constipation
Methylnaltrexone is a peripherally acting mu receptor antagonist used for treatment of opioid-induced constipation in patients with advanced illness, not for routine prevention. Stool softeners and stimulant laxatives are more commonly used for prevention. This is not a routine action.
B) Evaluating for urinary retention every 4-6 hours
This is appropriate. The nurse should monitor for signs of urinary retention, including inability to void, suprapubic discomfort, and decreased urine output. Bladder scanning may be used if available.
C) Counting respirations before and after giving the medication
This is essential. The nurse should count respirations for one full minute before administering morphine. If the rate is below 12 breaths per minute or if respirations are shallow, the dose should be held and the provider notified. Counting after administration allows monitoring for respiratory depression.
D) Assist with ambulation
This is appropriate. Opioids cause sedation and dizziness, increasing fall risk. The nurse should assist the patient with ambulation and ensure call light and personal items are within reach.
E) Monitoring the client's blood pressure closely for hypertension
Morphine can cause hypotension due to vasodilation and histamine release, not hypertension. Monitoring for hypotension is appropriate, not hypertension.
Conclusion
Appropriate routine nursing actions for morphine include evaluating for urinary retention, counting respirations, and assisting with ambulation. Methylnaltrexone is not routine, and hypertension monitoring is incorrect. Therefore, B, C, and D are correct, reflecting standard nursing care for patients receiving opioids.
The nurse is talking with a new mother about medications that can be safely resumed now that she is no longer pregnant. All the following medications are contraindicated during pregnancy, but which one may be ingested while breastfeeding without causing known infant harm?
A.
Lithium
B. Methotrexate
C. Ibuprofen
D. Nicotine
Rationale
Ibuprofen is the medication among the options that is considered safe for ingestion by a breastfeeding mother without causing known harm to the infant.
The question of medication safety during breastfeeding is a critical concern for new mothers, as many women require treatment for various conditions while nursing their infants. The safety of a drug during lactation is determined by several pharmacokinetic factors that influence how much of the medication passes into breast milk and how the infant's immature body handles that exposure. These factors include the drug's molecular weight, its half-life, its protein-binding capacity, its lipid solubility, and its oral bioavailability in the infant. Ibuprofen, a nonsteroidal anti-inflammatory drug (NSAID) commonly used for pain, fever, and inflammation, has been extensively studied in lactating women, and the collective evidence overwhelmingly supports its safety. When a breastfeeding mother takes ibuprofen, only minimal amounts transfer into her breast milk, typically estimated to be less than 1% of the maternal dose. For a standard 400 mg dose, the concentration found in breast milk is far below the therapeutic dose that would be given directly to an infant. This low level is physiologically insignificant and has not been associated with any documented adverse effects in nursing infants. The drug's short half-life ensures rapid elimination from the mother's system, and its high degree of protein binding limits the amount of free drug available to diffuse into the milk. Major health authorities, including the American Academy of Pediatrics and the World Health Organization, classify ibuprofen as compatible with breastfeeding, making it the analgesic and anti-inflammatory of choice for nursing mothers when medication is necessary.
A) Lithium
Lithium presents a very different safety profile that makes it unsuitable for ingestion without concern during breastfeeding. Lithium is a mood-stabilizing medication used primarily in the management of bipolar disorder, and its behavior in the body raises significant concerns for nursing infants. Unlike ibuprofen, lithium transfers extensively into breast milk, with studies demonstrating that milk concentrations can reach 40% to 50% of the maternal serum concentration. This substantial transfer results in infant serum levels that can be 10% to 50% of the mother's therapeutic level, a degree of exposure that places the breastfed infant at considerable risk. The potential consequences of this exposure are serious and well-documented in the medical literature. Infants exposed to lithium through breast milk may develop symptoms of toxicity including profound lethargy, hypotonia which manifests as diminished muscle tone and poor muscle strength, hypothermia, feeding difficulties, cyanosis indicating poor oxygenation, and electrocardiogram abnormalities that reflect cardiac involvement. These effects occur because the infant's renal and hepatic systems are immature and cannot efficiently clear the drug from their system. While there are rare circumstances where a mother's mental health stability absolutely requires lithium therapy and the benefits may outweigh the risks, this requires extremely careful risk-benefit analysis, close monitoring of infant serum levels, and vigilant observation for clinical signs of toxicity. Lithium cannot be considered a medication that can be ingested without the expectation of potential infant harm.
B) Methotrexate
Methotrexate represents another medication that is unequivocally contraindicated during breastfeeding due to its mechanism of action and potential for causing significant harm. Methotrexate is classified as an antimetabolite and immunosuppressant agent, used therapeutically for conditions including various malignancies, severe psoriasis that has not responded to other treatments, and aggressive rheumatoid arthritis. The drug works by inhibiting dihydrofolate reductase, an enzyme essential for DNA synthesis and cellular replication, which is why it is effective against rapidly dividing cells in cancer and inflammatory conditions. This same mechanism, however, poses grave risks to a nursing infant whose body is undergoing rapid growth and development. Methotrexate concentrates in breast milk and can achieve levels that pose a distinct and serious threat to the nursing infant. Potential toxicities from methotrexate exposure include bone marrow suppression, which would manifest as anemia, increased susceptibility to infections from leukopenia, and bleeding tendencies from thrombocytopenia. Gastrointestinal toxicity with mucosal damage can also occur, and there is a potential, though rare, risk of carcinogenicity with long-term exposure. The American Academy of Pediatrics explicitly recommends against breastfeeding during methotrexate therapy, a position that reflects the seriousness of these potential adverse effects. Furthermore, methotrexate can accumulate in neonatal tissues and persist for extended periods due to the infant's immature excretory mechanisms, prolonging the window of risk. Given these profound and potentially life-threatening consequences, methotrexate cannot be considered safe for the breastfeeding infant under any circumstances.
C) Ibuprofen
Ibuprofen stands in marked contrast to the other options, with a robust safety profile that makes it the appropriate choice for breastfeeding mothers. The safety of ibuprofen during lactation is supported by a wealth of pharmacokinetic data obtained from studies of lactating women. When mothers take standard analgesic doses of ibuprofen, such as 400 mg every six hours, researchers have measured drug levels in breast milk and consistently found concentrations to be extremely low, typically less than 0.1 mg/L. This amount is orders of magnitude below the therapeutic dose range for infants, which for comparison would be approximately 5 to 10 mg per kilogram of body weight. Several characteristics of ibuprofen contribute to this favorable safety profile. The drug has a relatively short elimination half-life of approximately two hours, which prevents accumulation in the mother's plasma and subsequently in her milk. It is also highly bound to plasma proteins, approximately 90% to 99%, which limits the amount of free drug available to diffuse across the alveolar epithelium into the breast milk. The drug is poorly lipid soluble, further restricting its passage into milk which has a high fat content. For breastfeeding mothers requiring relief from pain, inflammation, or fever, ibuprofen represents a well-studied, effective, and safe pharmacological option. The World Health Organization specifically includes ibuprofen on its list of drugs compatible with breastfeeding, and it is frequently the first-line analgesic recommended for nursing mothers.
D) Nicotine
Nicotine is the final option and is unequivocally contraindicated during breastfeeding, whether it comes from cigarettes, vaping devices, or nicotine replacement therapy products. Nicotine is a potent alkaloid that readily crosses biological membranes, including the alveolar cells of the breast, leading to significant transfer into breast milk. Research has demonstrated that nicotine concentrations in breast milk can reach levels that are 1.5 to 3 times higher than the maternal plasma levels, indicating active transport or concentration in the milk. This substantial exposure leads to detectable nicotine levels in the infant's bloodstream and urine. The consequences of this exposure for the nursing infant are multiple and clinically significant. Infants may exhibit irritability, tachycardia with increased heart rate, restlessness and difficulty sleeping, vomiting, and diarrhea as direct effects of nicotine on their developing nervous and gastrointestinal systems. Beyond these direct effects, nicotine has additional indirect consequences for breastfeeding. The drug inhibits prolactin, the hormone responsible for milk production, which can lead to decreased milk supply and early termination of breastfeeding. Furthermore, smoking exposes the infant to secondhand and thirdhand smoke, increasing risks for respiratory infections, otitis media, sudden infant death syndrome, and other serious health problems. While the safest approach for both mother and infant is complete smoking cessation, and breastfeeding is still recommended over formula feeding for mothers who continue to smoke due to the protective benefits of breast milk, the nicotine itself is not safe for the breastfeeding infant. Mothers should be counseled to minimize exposure by smoking immediately after breastfeeding, never smoking near the infant, and using nicotine replacement therapy only under medical supervision with careful consideration of the risks and benefits.
Conclusion
When considering which medication may be safely ingested while breastfeeding without causing known infant harm, ibuprofen emerges as the clear and correct choice based on its pharmacokinetic properties and extensive safety data. Ibuprofen transfers minimally into breast milk, achieves concentrations far below infant therapeutic levels, and has not been associated with adverse effects in nursing infants. The other options present unacceptable risks for different reasons. Lithium achieves significant milk concentrations and places the infant at risk for toxicity affecting the central nervous system and cardiac function. Methotrexate concentrates in milk and poses serious risks including bone marrow suppression and potential carcinogenicity due to its mechanism as an antimetabolite. Nicotine transfers into milk at concentrations higher than maternal plasma levels and causes direct adverse effects in infants while also reducing milk production through prolactin inhibition. Therefore, only ibuprofen among these options may be ingested while breastfeeding without the expectation of causing known infant harm, making it the appropriate medication for nursing mothers when an analgesic or anti-inflammatory is needed.
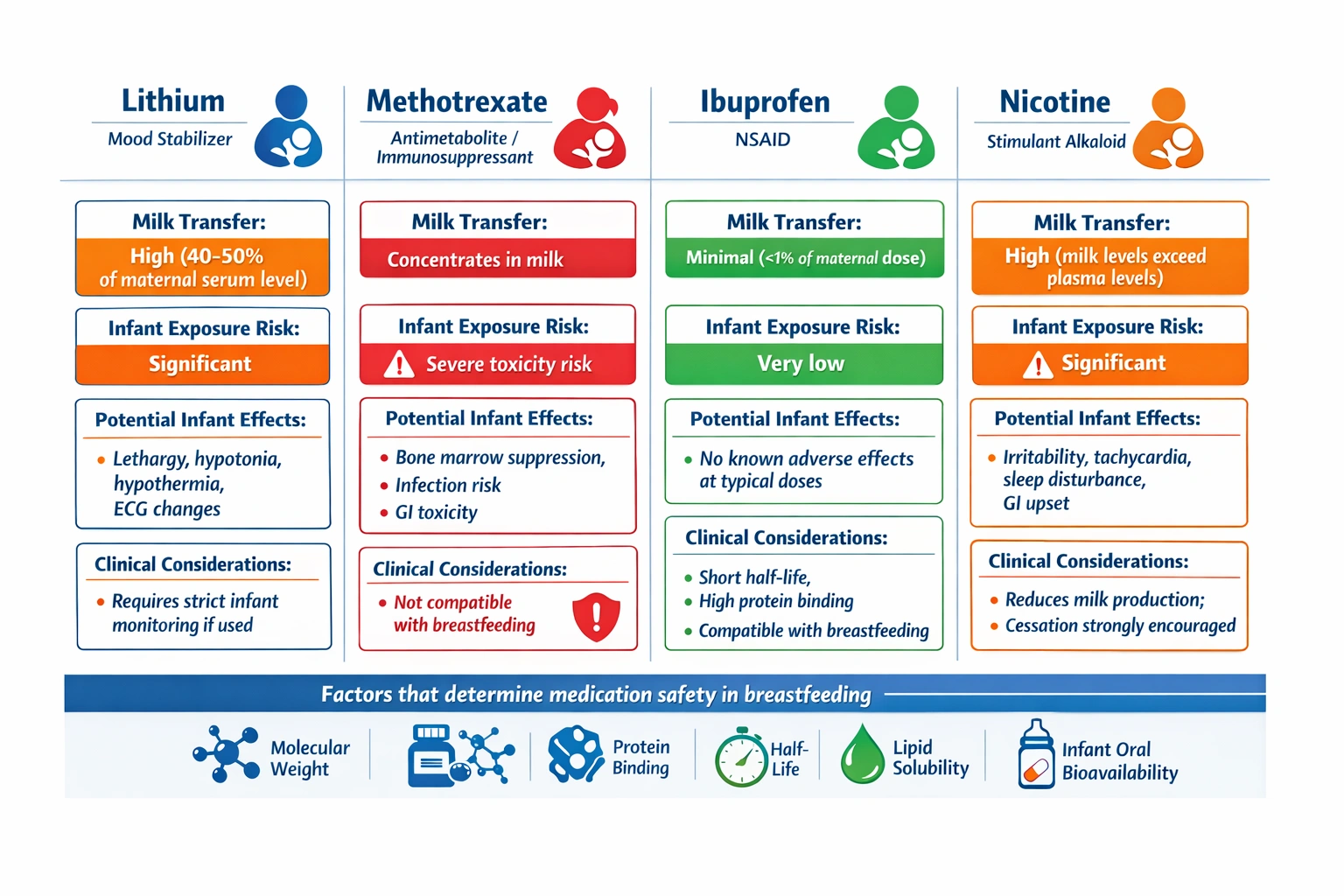
Parents ask the nurse why an over-the-counter cough suppressant with sedative side effects is not recommended for infants. Which response by the nurse is correct?
A.
Cough medicine tastes bad, and infants usually won't take it
B. Babies have a more rapid gastric emptying time and don't absorb drugs well
C. Infants are more susceptible to central nervous system effects than adults are
D. Infants metabolize drugs too rapidly, so drugs aren't as effective
Rationale
The correct response is that infants are more susceptible to central nervous system effects than adults are, which explains why cough suppressants with sedative properties can be dangerous in this age group due to their immature physiology and enhanced sensitivity to these medications.
The use of over-the-counter cough and cold medications in infants and young children has been a subject of significant concern and controversy in recent decades. These products, which often contain multiple ingredients including antitussives, expectorants, antihistamines, and decongestants, were historically widely used for symptomatic relief of upper respiratory infections in children of all ages. However, accumulating evidence of adverse events, including fatalities, led to a major re-evaluation of their safety in young children. In 2008, the U.S. Food and Drug Administration issued a public health advisory recommending that over-the-counter cough and cold products not be used in children under two years of age, and manufacturers voluntarily withdrew products labeled for infants. Subsequent recommendations have extended this caution to children under four or six years, depending on the specific organization. The rationale for these recommendations lies in the unique physiological characteristics of infants that make them more vulnerable to the effects of these medications, particularly those with sedative properties.
A) Cough medicine tastes bad, and infants usually won't take it
This response is factually incorrect and trivializes a serious safety concern. While taste may affect acceptance of oral medications in children, this is not the reason these products are not recommended for infants. Infants can and do ingest these medications, whether administered by caregivers or through accidental ingestion, and it is this ingestion that has led to adverse events and deaths. The issue is not palatability but safety. Many infants will take medications despite unpleasant taste, especially when mixed with food or sweetened liquids, and the assumption that they will not take it is false and dangerous. This response fails to provide accurate information and does not address the parents' underlying concern about why the medication is not recommended, potentially leading them to believe it is simply a matter of taste and that they could overcome this by finding ways to make it more acceptable.
B) Babies have a more rapid gastric emptying time and don't absorb drugs well
This statement reflects a misunderstanding of infant gastrointestinal physiology. Infants actually have slower and more unpredictable gastric emptying compared to adults. Gastric emptying time is prolonged in newborns and gradually matures over the first months of life. This can affect drug absorption by delaying the time it takes for medications to reach the small intestine, where most absorption occurs. Additionally, the issue with cough and cold medications in infants is not poor absorption; in fact, these medications are well absorbed and can reach toxic levels due to immature metabolism and excretion. The problem is that infants absorb the drugs effectively but cannot clear them efficiently, leading to accumulation and toxicity. This response provides inaccurate physiological information and does not explain the true safety concerns, potentially giving parents a false sense of security if they believe the drugs won't be absorbed anyway.
C) Infants are more susceptible to central nervous system effects than adults are
This response is accurate and addresses the key safety concern that underlies recommendations against using sedating cough suppressants in infants. Infants have unique physiological characteristics that make them more vulnerable to the central nervous system effects of medications. Their blood-brain barrier is immature and more permeable, allowing greater penetration of drugs into the central nervous system. This means that sedating medications can achieve higher concentrations in the infant brain compared to adults receiving equivalent weight-based doses. Additionally, infants have immature hepatic enzyme systems, particularly the cytochrome P450 enzymes responsible for metabolizing many drugs, leading to prolonged half-lives and accumulation of medications with repeated dosing. Their renal function is also immature, with glomerular filtration rates reaching adult levels only by one to two years of age, which slows the elimination of drugs and their metabolites. The combination of increased CNS penetration, slowed metabolism, and reduced excretion means that sedating medications can produce exaggerated and prolonged CNS depression in infants, leading to respiratory depression, coma, and death. This explanation helps parents understand the physiological basis for the recommendation and why these products are not safe for infants even though they may be used in older children and adults.
D) Infants metabolize drugs too rapidly, so drugs aren't as effective
This statement contradicts the actual safety concern. Infants actually have immature hepatic enzyme systems, leading to slower drug metabolism, not more rapid metabolism. The activity of many drug-metabolizing enzymes is reduced at birth and gradually increases over the first weeks to months of life. This slower metabolism contributes to drug accumulation and toxicity, not reduced effectiveness. The statement that drugs aren't as effective is also incorrect and could lead parents to believe that the medication is simply not helpful rather than dangerous. In reality, these medications are effective, sometimes too effective, producing profound sedation and respiratory depression in infants. This response provides inaccurate information that could lead parents to dismiss the warning or to use the medication believing it won't work anyway, which is a dangerous misconception.
Conclusion
The correct response is that infants are more susceptible to central nervous system effects than adults are, due to an immature blood-brain barrier, slower drug metabolism from immature hepatic enzymes, and reduced renal excretion, all of which increase the risk of serious adverse effects including respiratory depression. Taste is not the safety concern, and the statement that infants won't take it is false and trivializing. Gastric emptying and drug absorption characteristics do not explain the risk; infants absorb drugs well but clear them poorly. Infants metabolize drugs more slowly, not more rapidly, and the medications are effective, which is precisely the problem. Therefore, the accurate explanation addresses increased CNS susceptibility, providing parents with the physiological rationale for why these products are not recommended for infants.
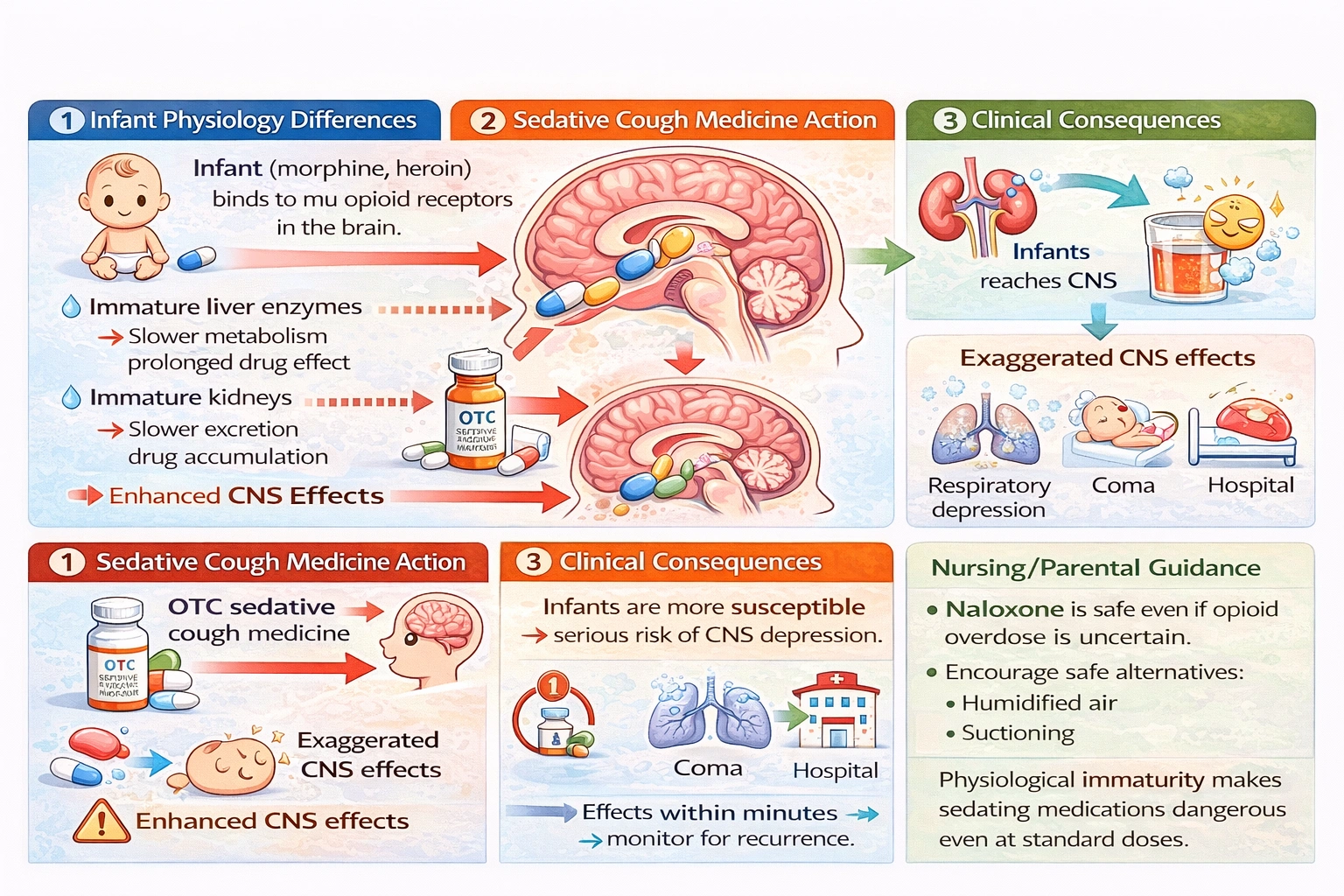
Which side effect of clindamycin causes the most concern?
A.
Vomiting
B. Headache
C. Diarrhea
D. Nausea
Rationale
Diarrhea is the side effect of clindamycin that causes the most concern because it may indicate Clostridium difficile infection, a potentially severe and life-threatening complication of antibiotic therapy that requires prompt recognition and treatment.
Clindamycin is a lincosamide antibiotic that has been used for decades to treat a variety of infections caused by anaerobic bacteria, streptococci, staphylococci, and certain other organisms. It works by binding to the 50S subunit of the bacterial ribosome and inhibiting protein synthesis. While effective for many indications, clindamycin has a well-established association with antibiotic-associated diarrhea and, more importantly, with Clostridium difficile infection. Clostridium difficile is a spore-forming, toxin-producing anaerobic bacterium that can colonize the colon when the normal gut flora is disrupted by antibiotics. Clindamycin is particularly notorious for causing CDI because it suppresses many of the normal protective bacteria while having limited activity against C. difficile itself, allowing the organism to proliferate and produce toxins A and B. These toxins cause inflammation, mucosal damage, and diarrhea that can range from mild to severe, life-threatening colitis.
A) Vomiting
Vomiting can occur with clindamycin as a gastrointestinal side effect but is not the most concerning. While vomiting can lead to dehydration and electrolyte imbalance, it does not carry the same life-threatening potential as Clostridium difficile colitis. Vomiting is manageable with antiemetics and supportive care and does not typically require antibiotic discontinuation unless severe. The nurse should address vomiting but recognize that it is not the most serious potential adverse effect.
B) Headache
Headache is a possible side effect of clindamycin but is generally mild and not a cause for major concern. It does not indicate a serious adverse reaction and can be managed with analgesics if needed. Headaches are common with many medications and are not specific to clindamycin or indicative of the more serious complications associated with this antibiotic.
C) Diarrhea
Diarrhea is the most concerning side effect because it may indicate Clostridium difficile infection. CDI can range from mild, self-limited diarrhea to severe, life-threatening pseudomembranous colitis characterized by profuse watery diarrhea, abdominal pain, fever, leukocytosis, and in severe cases, toxic megacolon, colonic perforation, and death. Any client taking clindamycin who develops diarrhea must be evaluated for CDI, which typically includes stool testing for C. difficile toxin and, in some cases, endoscopic evaluation. Treatment may include discontinuation of the offending antibiotic when possible and initiation of specific therapy with oral vancomycin or fidaxomicin. The nurse must recognize diarrhea as a potentially serious symptom requiring prompt evaluation, not merely a nuisance side effect.
D) Nausea
Nausea is a common gastrointestinal side effect but is not as concerning as diarrhea. It can often be managed by taking the medication with food. Nausea does not indicate the potentially life-threatening complication associated with clindamycin. While persistent nausea can affect nutrition and adherence, it is not the side effect that requires the most urgent evaluation and intervention.
Conclusion
Diarrhea is the side effect of clindamycin that causes the most concern due to the risk of Clostridium difficile infection, which can range from mild to severe and life-threatening. Vomiting, headache, and nausea are less concerning and do not carry the same risk of severe complications. Therefore, diarrhea requires the closest monitoring and prompt evaluation, and any client taking clindamycin who develops diarrhea should be assessed for possible CDI.
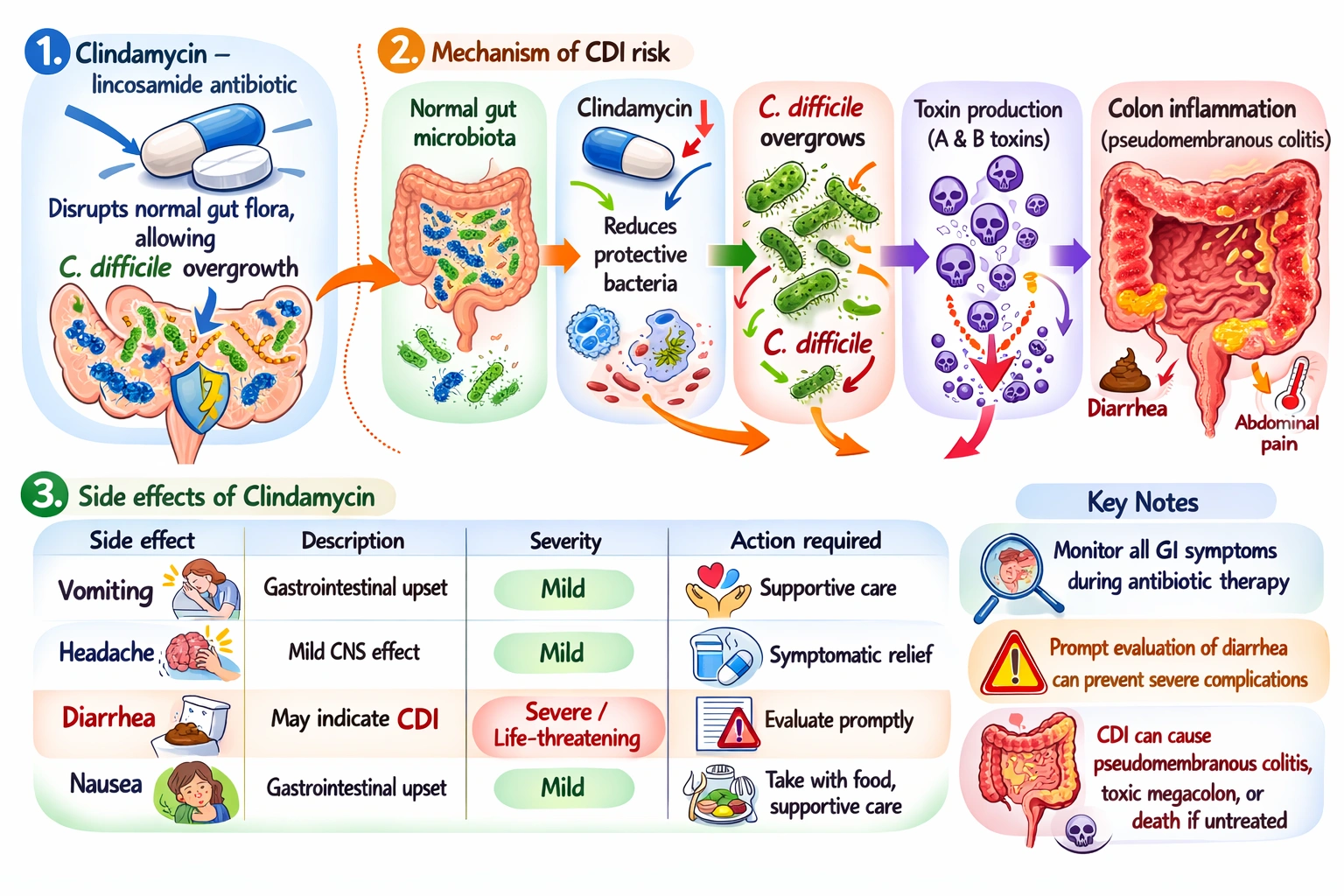
A nurse is caring for a client and her newborn immediately after delivery. The client's medication history includes prenatal vitamins throughout pregnancy, one or two glasses of wine before knowing she is pregnant, occasional use of an albuterol inhaler in her last trimester, and intravenous morphine during labor. What is the nurse's most appropriate action?
A.
Note a high-pitched cry and irritability in the infant and observe for seizures
B. Administer opioids to the infant to prevent withdrawal syndrome
C. Monitor the infant's respiration and prepare to administer naloxone if needed
D. Prepare the client for motor delays in the infant caused by alcohol use
Rationale
The nurse's most appropriate action is to monitor the infant's respiration and prepare to administer naloxone if needed, as the infant received intravenous morphine during labor that crosses the placenta and can cause neonatal respiratory depression.
Medications administered to the mother during labor can affect the newborn after delivery because many drugs cross the placenta and reach the fetal circulation. The effects depend on the specific medication, the dose, the timing of administration relative to delivery, and the infant's ability to metabolize and eliminate the drug. Opioids such as morphine are of particular concern because they can cause respiratory depression in the newborn. The fetal liver and kidneys are immature and cannot clear opioids as efficiently as older children or adults, leading to prolonged drug levels and effects. When opioids are administered close to delivery, the infant may be born with significant drug levels and exhibit signs of opioid exposure including respiratory depression, hypotonia, decreased feeding, and sedation.
A) Note a high-pitched cry and irritability in the infant and observe for seizures
This action is not indicated based on the medication history. High-pitched cry and irritability are signs of neonatal abstinence syndrome, which occurs after chronic in utero exposure to opioids, not from a single dose during labor. The infant received one dose of morphine during labor, which would not cause withdrawal. This action reflects confusion between acute opioid effects and withdrawal.
B) Administer opioids to the infant to prevent withdrawal syndrome
This action is completely inappropriate and dangerous. The infant does not have opioid exposure sufficient to cause withdrawal and should not receive opioids. Administering opioids to a newborn without indication could cause respiratory depression and other adverse effects. This reflects a fundamental misunderstanding of neonatal abstinence syndrome and opioid effects.
C) Monitor the infant's respiration and prepare to administer naloxone if needed
This is the correct action. Maternal IV morphine during labor can cause neonatal respiratory depression. The nurse should closely monitor the infant's respiratory rate, effort, and oxygen saturation, along with level of consciousness and muscle tone. If respiratory depression occurs, naloxone, an opioid antagonist, can be administered to reverse opioid effects. The nurse should have naloxone readily available and know the dose and route for neonatal administration. This action demonstrates appropriate recognition of the risk and preparation to intervene.
D) Prepare the client for motor delays in the infant caused by alcohol use
This action is inappropriate and alarming. The client reported one or two glasses of wine before knowing she was pregnant, which is not associated with fetal alcohol syndrome or motor delays. This level of alcohol exposure, occurring very early in pregnancy before most women know they are pregnant, is not considered harmful. Warning about motor delays is unnecessary and would cause undue distress.
Conclusion
The nurse's most appropriate action is to monitor the infant's respiration and prepare to administer naloxone if needed due to maternal IV morphine during labor, which can cause neonatal respiratory depression. Signs of withdrawal, administering opioids, and warning about alcohol-related motor delays are all inappropriate. Therefore, respiratory monitoring and naloxone readiness is correct, ensuring prompt intervention if the infant shows signs of opioid-induced respiratory depression.
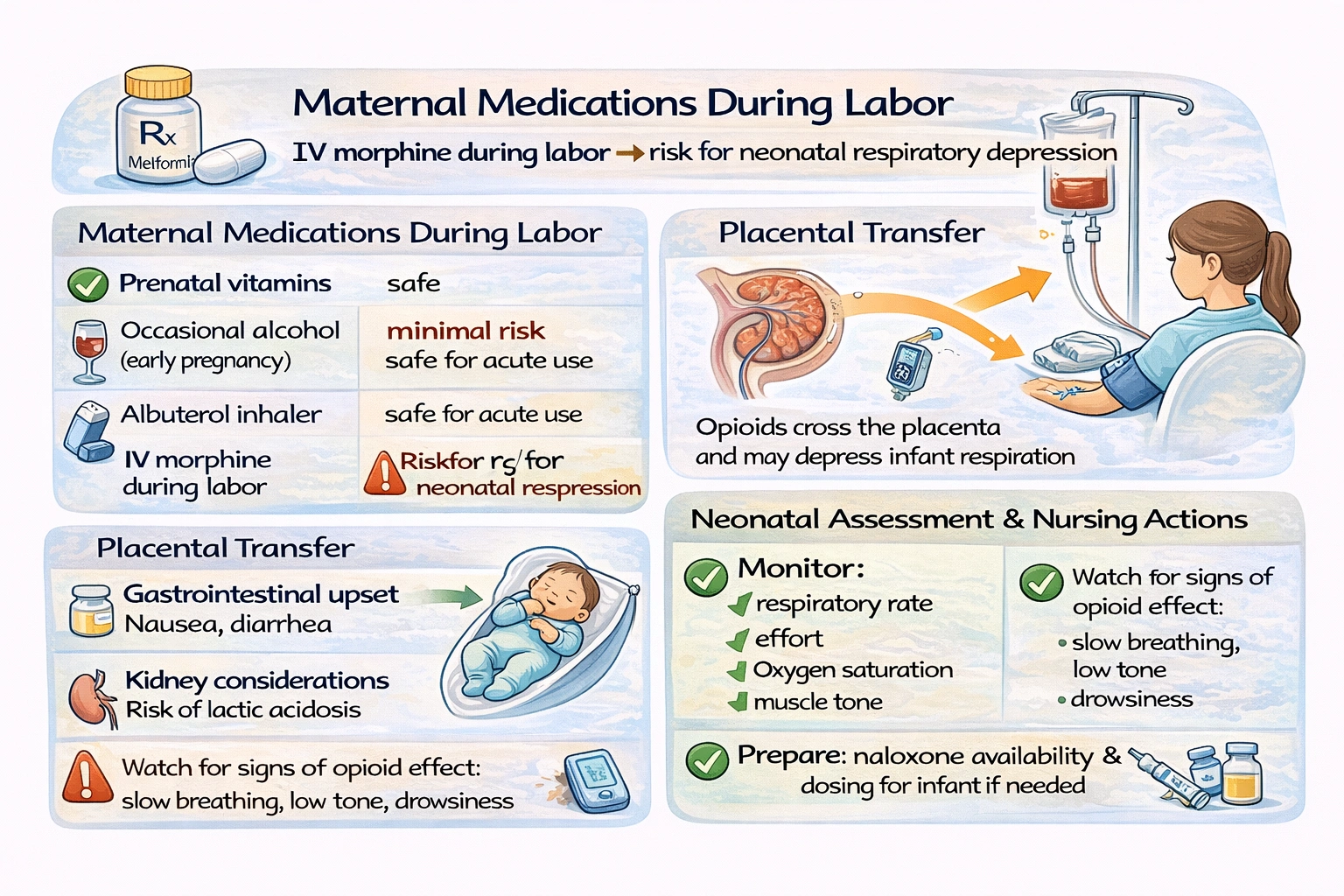
A nurse is providing teaching for an adult client with arthritis who has been instructed to take ibuprofen for discomfort. Which statement by the client indicates a need for further education?
A.
I may experience tinnitus with higher doses of this medication
B. I will take this medication with meals to help prevent stomach upset
C. I may take up to 1000 mg four times daily for pain
D. I should stop drinking alcohol
Rationale
The statement that the client may take up to 1000 mg four times daily for pain indicates a need for further education, as this would total 4000 mg per day, which exceeds safe limits and significantly increases the risk of gastrointestinal bleeding, renal impairment, and cardiovascular events.
Ibuprofen is a nonsteroidal anti-inflammatory drug widely used for pain, inflammation, and fever. It works by inhibiting cyclooxygenase enzymes, reducing the production of prostaglandins that mediate inflammation and pain. However, NSAIDs have significant dose-dependent adverse effects, particularly on the gastrointestinal tract, kidneys, and cardiovascular system. Understanding appropriate dosing is essential for safe use. The maximum recommended daily dose of ibuprofen for over-the-counter use is 1200 mg, typically 400 mg three times daily. For prescription use, the maximum is typically 3200 mg per day, but this must be under provider supervision and for short-term use. Taking 1000 mg four times daily would be 4000 mg per day, which exceeds safe limits for any indication.
A) I may experience tinnitus with higher doses of this medication
This statement indicates some misunderstanding. Tinnitus is a sign of salicylate toxicity, not ibuprofen toxicity. Ibuprofen is not a salicylate and does not typically cause tinnitus. The client may be confusing ibuprofen with aspirin. While this shows some confusion, it is not as immediately dangerous as the dosing error.
B) I will take this medication with meals to help prevent stomach upset
This statement shows understanding. Taking ibuprofen with food or milk can reduce gastrointestinal irritation, a common side effect of NSAIDs. This is appropriate self-care.
C) I may take up to 1000 mg four times daily for pain
This statement indicates dangerous misunderstanding. 1000 mg four times daily equals 4000 mg per day, which exceeds safe limits and risks serious toxicity, including gastrointestinal bleeding, renal impairment, and cardiovascular events. The client needs immediate education on appropriate dosing, which should be based on the lowest effective dose for the shortest duration necessary, and should never exceed 3200 mg per day under any circumstances, with 1200 mg per day for over-the-counter use.
D) I should stop drinking alcohol
This statement shows understanding. Alcohol increases the risk of gastrointestinal bleeding with ibuprofen and should be avoided or limited. This is appropriate self-care.
Conclusion
The client needs further education when stating they may take up to 1000 mg four times daily, as this exceeds safe dosing and risks serious toxicity. Tinnitus is not typical for ibuprofen but is less dangerous than the dosing error. Taking with meals and avoiding alcohol show understanding. Therefore, the dosing statement requires correction, and the nurse should provide clear instructions on appropriate ibuprofen dosing and the risks of exceeding recommended limits.
A client with no known drug allergies is receiving amoxicillin PO twice daily. Twenty minutes after being given a dose, the client complains of shortness of breath with a blood pressure of 100/58 mm Hg. What will the nurse do?
A.
Notify the provider if the client develops a rash
B. Withhold the next dose until symptoms subside
C. Contact the provider and prepare to administer epinephrine as ordered
D. Request an order for a skin test to evaluate possible penicillin allergy
Rationale
The nurse should contact the provider and prepare to administer epinephrine as ordered, as the client is experiencing signs of anaphylaxis, a life-threatening allergic reaction requiring immediate intervention with epinephrine as the first-line treatment.
Anaphylaxis is a severe, life-threatening, systemic hypersensitivity reaction that can occur within minutes of exposure to an allergen. It is mediated by immunoglobulin E and involves rapid release of mediators from mast cells and basophils, including histamine, leukotrienes, prostaglandins, and tryptase. These mediators cause a cascade of effects throughout the body, including bronchoconstriction and laryngeal edema leading to respiratory distress, vasodilation and increased vascular permeability leading to hypotension and shock, and cutaneous manifestations such as urticaria, angioedema, and flushing. Penicillins, including amoxicillin, are among the most common causes of drug-induced anaphylaxis. The timing of symptoms, occurring twenty minutes after medication administration, is classic for anaphylaxis. The client's symptoms of shortness of breath and hypotension are particularly concerning because they indicate involvement of the respiratory and cardiovascular systems, which are the two most critical systems in anaphylaxis and the ones most likely to lead to death if not treated promptly.
A) Notify the provider if the client develops a rash
This response demonstrates a dangerous failure to recognize the severity of the current situation. The client is already experiencing serious symptoms that require immediate attention, including respiratory distress and hypotension. Waiting for a rash to develop before notifying the provider would delay life-saving treatment and could allow the reaction to progress to complete airway obstruction or cardiovascular collapse. Anaphylaxis can progress rapidly, and delays in treatment are associated with worse outcomes. The nurse who waits for additional symptoms before acting is not prioritizing the patient's immediate safety and is failing to recognize that the current symptoms alone are sufficient to diagnose anaphylaxis and warrant emergency intervention.
B) Withhold the next dose until symptoms subside
This response is dangerously inadequate and demonstrates a complete misunderstanding of the urgency of the situation. The client is experiencing an acute anaphylactic reaction right now, not a concern about future doses. Withholding the next dose does nothing to address the current emergency and could result in the patient's condition deteriorating while the nurse focuses on an irrelevant action. The priority is to treat the anaphylaxis immediately, not to consider future medication administration. This response suggests that the nurse does not recognize anaphylaxis as a life-threatening emergency requiring immediate intervention.
C) Contact the provider and prepare to administer epinephrine as ordered
This is the correct and appropriate response that prioritizes patient safety and follows the standard of care for anaphylaxis management. The nurse should immediately activate the emergency response system, which may include calling a rapid response team or code blue depending on hospital policy. While doing so, the nurse should prepare to administer epinephrine, which is the first-line and most important treatment for anaphylaxis. Epinephrine works by causing vasoconstriction, which reverses hypotension and reduces angioedema, and by causing bronchodilation, which relieves respiratory distress. It also stabilizes mast cells and reduces further mediator release. The standard dose for adults is 0.3 mg intramuscularly in the mid-outer thigh, which provides rapid absorption and effect. The nurse should also administer supplemental oxygen, place the patient in a supine position with legs elevated if hypotensive, and prepare for possible additional interventions such as intravenous fluids and airway management. Contacting the provider is appropriate to ensure orders are obtained, but in many facilities, epinephrine may be available as a standing order for anaphylaxis, allowing the nurse to administer it immediately without waiting for a provider contact.
D) Request an order for a skin test to evaluate possible penicillin allergy
This response is completely inappropriate during an acute reaction and demonstrates a profound misunderstanding of priorities. Skin testing is a diagnostic procedure used to evaluate possible allergy in stable patients, not during an active anaphylactic reaction. Performing skin testing now would be dangerous, could exacerbate the reaction, and would delay emergency treatment. The priority is treating the life-threatening anaphylaxis, not diagnosing the allergy. The diagnosis of penicillin allergy can be addressed later, after the patient has stabilized and recovered from this acute episode.
Conclusion
When a client develops shortness of breath and hypotension twenty minutes after receiving amoxicillin, the nurse should contact the provider and prepare to administer epinephrine as ordered, recognizing this as anaphylaxis requiring immediate intervention. Notifying the provider only if a rash develops, withholding future doses, or requesting skin testing are all inappropriate and dangerous responses that delay life-saving treatment. Therefore, epinephrine preparation is correct, ensuring prompt treatment of this life-threatening emergency.
A nurse is caring for a client who was recently started on lithium and is training a new nurse. What comment by the new nurse would require further teaching?
A.
Lithium is used to treat bipolar depression
B. Lithium is used to reduce manic episodes
C. Lithium is contraindicated with antidepressant use
D. Lithium reduces hyperactivity
Rationale
The comment that lithium is contraindicated with antidepressant use requires further teaching, as lithium is not contraindicated with antidepressants and is often used in combination with them for bipolar depression, though caution is needed to monitor for manic switching.
Lithium is a mood stabilizer that has been the mainstay of treatment for bipolar disorder for decades. Its mechanism of action is complex and not fully understood, but it involves effects on intracellular signaling pathways, neurotransmitter systems, and gene expression. Lithium is effective for acute mania, for maintenance therapy to prevent both manic and depressive episodes, and for bipolar depression, though its antidepressant effects may be less robust than its antimanic effects. The management of bipolar depression often requires combination therapy, and antidepressants are sometimes used in conjunction with mood stabilizers like lithium. However, this combination requires caution because antidepressants can precipitate manic episodes in susceptible individuals, a phenomenon known as manic switching. The use of antidepressants in bipolar disorder is controversial and should be guided by careful clinical judgment, but lithium is not contraindicated with antidepressants. The statement that it is contraindicated reflects a misunderstanding of bipolar treatment principles.
A) Lithium is used to treat bipolar depression
This statement is correct. Lithium has efficacy in treating bipolar depression, though it may be more effective for mania and maintenance. It is considered a first-line treatment for bipolar disorder across all phases.
B) Lithium is used to reduce manic episodes
This statement is correct. Lithium is highly effective for acute mania and is a first-line treatment for manic episodes in bipolar disorder.
C) Lithium is contraindicated with antidepressant use
This statement requires further teaching. Lithium is not contraindicated with antidepressants, and combination therapy is often used for bipolar depression. However, caution is needed because antidepressants can trigger manic episodes, and patients should be monitored closely for signs of switching.
D) Lithium reduces hyperactivity
This statement is correct. Lithium reduces manic symptoms including hyperactivity, agitation, and impulsivity through its mood-stabilizing effects.
Conclusion
The new nurse needs further teaching when stating lithium is contraindicated with antidepressant use, as this is incorrect. The statements about treating bipolar depression, reducing mania, and reducing hyperactivity are all accurate. Therefore, the contraindication comment requires correction, clarifying that lithium can be used with antidepressants under careful monitoring.
A client has had emergency surgery for a ruptured appendix. Before surgery, the client was taking dexamethasone for three years. With the client's steroid use history, for which complication will the nurse monitor in the recovery phase?
A.
Hyperglycemia
B. Wound infection
C. Adrenal crisis
D. Delayed wound healing
Rationale
The nurse will monitor for adrenal crisis in the recovery phase, as chronic steroid use suppresses the HPA axis, and the stress of surgery may precipitate acute adrenal insufficiency requiring prompt recognition and treatment.
The client has been taking dexamethasone, a glucocorticoid, for three years. Chronic glucocorticoid therapy suppresses the hypothalamic-pituitary-adrenal axis through negative feedback. Exogenous steroids signal the hypothalamus and pituitary to reduce secretion of corticotropin-releasing hormone and adrenocorticotropic hormone, respectively. Over time, this leads to atrophy of the adrenal cortex and loss of the ability to produce endogenous cortisol. During the stress of surgery, anesthesia, and the postoperative period, the body normally increases cortisol production to maintain homeostasis. However, this client's adrenal glands may not respond adequately due to suppression. This can lead to acute adrenal insufficiency, or adrenal crisis, characterized by hypotension, shock that is resistant to fluids and vasopressors, nausea, vomiting, weakness, and electrolyte imbalances. Adrenal crisis is a life-threatening emergency requiring immediate administration of stress-dose steroids.
A) Hyperglycemia
Steroids can cause hyperglycemia, and this may occur postoperatively, but it is less immediately life-threatening than adrenal crisis. It may also be masked by the stress response.
B) Wound infection
Steroids increase infection risk due to immunosuppression, but this is not the most immediate postoperative concern. Infection typically develops over days, not in the immediate recovery phase.
C) Adrenal crisis
This is the most critical complication to monitor for in the immediate recovery phase due to HPA axis suppression. Signs include hypotension, shock, weakness, nausea, and vomiting.
D) Delayed wound healing
Steroids impair wound healing, but this is a longer-term concern, not an immediate postoperative complication.
Conclusion
For a client with chronic steroid use undergoing surgery, the nurse must monitor for adrenal crisis in the recovery phase due to HPA axis suppression. Hyperglycemia, infection, and delayed healing are also possible but less immediately life-threatening. Therefore, adrenal crisis is correct, and the nurse should be prepared to recognize and respond to signs of adrenal insufficiency.
A client is discharged from the hospital with a prescription for trimethoprim/sulfamethoxazole. What must the nurse include in the discharge teaching?
A.
Take folic acid supplements
B. Eat foods that are high in potassium
C. Take the medication with food
D. Drink eight to ten glasses of water each day
Rationale
The nurse must include in the discharge teaching that the client should drink eight to ten glasses of water each day while taking trimethoprim/sulfamethoxazole to prevent crystalluria and potential renal damage, which is the most critical safety instruction for this medication.
Trimethoprim/sulfamethoxazole, also known as co-trimoxazole, is a combination antibiotic that has been widely used for decades to treat a variety of infections including urinary tract infections, respiratory tract infections, and certain opportunistic infections. The medication works through sequential blockade of folate metabolism in bacteria, providing synergistic antibacterial activity. However, both components of this combination are excreted renally, and they have the potential to crystallize in the urine, particularly in acidic or concentrated urine. This phenomenon, known as crystalluria, occurs when the drug precipitates out of solution in the renal tubules, forming crystals that can cause mechanical obstruction, inflammation, and damage to the kidney tissue. Crystalluria can manifest as hematuria, flank pain, dysuria, and in severe cases, acute kidney injury. The risk is highest in patients who are dehydrated, those with acidic urine, and those receiving high doses. Prevention of this potentially serious complication is achieved primarily through adequate hydration, which maintains high urine flow and dilutes the urine, reducing the concentration of drug and metabolites and preventing crystal formation.
A) Take folic acid supplements
Folic acid supplementation is not routinely required for most patients taking trimethoprim/sulfamethoxazole. Trimethoprim inhibits bacterial dihydrofolate reductase, an enzyme involved in folate metabolism, but it has much lower affinity for the human form of this enzyme. At standard therapeutic doses, trimethoprim does not significantly affect human folate metabolism in most individuals. However, in certain populations, folic acid supplementation may be considered. These include pregnant women, who have increased folate requirements for fetal development, patients who are malnourished or have poor dietary folate intake, those on long-term, high-dose therapy such as for Pneumocystis jirovecii pneumonia prophylaxis in HIV patients, and patients with megaloblastic anemia. For the typical patient receiving a standard course of trimethoprim/sulfamethoxazole for an acute infection, folic acid supplementation is not necessary and is not a routine discharge instruction. The most important universal teaching point is about hydration to prevent crystalluria.
B) Eat foods that are high in potassium
Increasing dietary potassium is not a standard recommendation for trimethoprim/sulfamethoxazole therapy and, in fact, could be potentially harmful in some patients. Trimethoprim/sulfamethoxazole can actually cause hyperkalemia, or elevated potassium levels, as a potential adverse effect. This occurs because trimethoprim inhibits epithelial sodium channels in the distal nephron, similar to the mechanism of the potassium-sparing diuretic amiloride. This inhibition reduces sodium reabsorption and potassium secretion, leading to potassium retention. The risk of hyperkalemia is highest in patients with renal impairment, those taking other medications that increase potassium such as ACE inhibitors or potassium-sparing diuretics, elderly patients, and those receiving higher doses. Recommending a high-potassium diet to a patient taking this medication could exacerbate this risk and potentially lead to dangerous hyperkalemia. Therefore, this instruction would be inappropriate and potentially harmful, and it is not part of routine discharge teaching for this medication.
C) Take the medication with food
Taking trimethoprim/sulfamethoxazole with food can help reduce gastrointestinal side effects such as nausea, vomiting, and stomach upset, and this is often recommended to improve tolerability. Gastrointestinal symptoms are among the most common adverse effects of this medication, and taking it with food or milk can help minimize these symptoms. While this is a helpful instruction for patient comfort and adherence, it is not the most critical teaching point for safe medication use. The priority instruction relates to preventing crystalluria and renal damage through adequate hydration. The gastrointestinal side effects, while unpleasant, are generally not dangerous, whereas crystalluria can lead to serious renal injury. Therefore, while taking with food may be mentioned as a helpful tip, the instruction that must be included is about adequate fluid intake.
D) Drink eight to ten glasses of water each day
This is the essential instruction that must be included in discharge teaching for trimethoprim/sulfamethoxazole. Maintaining high urine output through adequate hydration is the primary preventive measure against crystalluria and nephrotoxicity. The nurse should explain the reason for this instruction so the client understands its importance and is motivated to comply. Clients should be advised to drink eight to ten 8-ounce glasses of water daily throughout the entire course of antibiotic therapy, and to maintain this level of hydration even if they do not feel thirsty. They should also be instructed to report any changes in urinary output, pain with urination, or blood in the urine, as these could be signs of crystalluria or other urinary tract complications. This teaching is critical for preventing a potentially serious adverse effect and ensuring safe medication use. The nurse should also advise the client that if they have conditions that limit fluid intake, such as heart failure or renal impairment, they should discuss appropriate hydration with their provider, but for most patients, this level of fluid intake is safe and essential.
Conclusion
When discharging a client with a prescription for trimethoprim/sulfamethoxazole, the nurse must include instruction to drink eight to ten glasses of water daily to prevent crystalluria and renal damage, as adequate hydration maintains high urine flow and dilutes the urine to prevent drug precipitation. Folic acid supplementation is not routinely needed and is not a universal discharge instruction. High-potassium foods are not recommended and could be harmful given the risk of hyperkalemia with this medication. While taking with food may help with gastrointestinal tolerability, it is not the priority safety instruction. Therefore, adequate fluid intake is the essential teaching point that must be included for all patients taking this medication.

A nurse is performing a preoperative drug history on a client who is admitted to the hospital for surgery. What dietary supplement contributes to the risk of bleeding?
A.
Probiotics
B. Coenzyme Q-10
C. Ma Huang
D. Ginkgo biloba
Rationale
Ginkgo biloba is the dietary supplement that contributes to the risk of bleeding and must be identified in preoperative drug history, as its antiplatelet effects can increase surgical bleeding risk when combined with the hemostatic challenges of surgery.
Preoperative drug history is a critical component of surgical preparation, designed to identify medications and supplements that may increase the risk of complications during and after surgery. Many patients do not consider herbal and dietary supplements as "medications" and may not volunteer information about them unless specifically asked. However, these products can have significant pharmacological effects that impact surgical outcomes. Bleeding risk is a major concern because many supplements affect platelet function, coagulation, or both. When combined with the inherent bleeding risk of surgical procedures, these effects can lead to excessive blood loss, need for transfusion, and other complications. Identifying these supplements preoperatively allows for timely discontinuation before surgery to allow normalization of hemostatic function.
A) Probiotics
Probiotics are live microorganisms intended to colonize the gut and provide health benefits by supporting a healthy microbiome. They do not affect coagulation or platelet function and do not increase bleeding risk. They are not a concern for preoperative bleeding and do not need to be discontinued for this reason.
B) Coenzyme Q-10
Coenzyme Q-10 is an antioxidant supplement used for various conditions including heart health, statin-related muscle symptoms, and mitochondrial disorders. It does not have significant antiplatelet or anticoagulant effects and is not associated with increased bleeding risk. While it may have other interactions, bleeding is not a primary concern with this supplement.
C) Ma Huang
Ma Huang, also known as ephedra, is an herbal supplement containing ephedrine and other alkaloids. It is used for weight loss, energy enhancement, and athletic performance. Its primary risks involve cardiovascular effects including hypertension, tachycardia, palpitations, arrhythmias, and in rare cases, myocardial infarction and stroke. It does not significantly affect bleeding risk. The preoperative concern with Ma Huang relates to cardiovascular stability during anesthesia and surgery, not bleeding.
D) Ginkgo biloba
Ginkgo biloba is correctly identified as contributing to bleeding risk. This herbal supplement, derived from the leaves of the Ginkgo biloba tree, is commonly used for memory enhancement, cognitive function, and peripheral vascular disease. Its mechanism of action involves multiple effects on the vascular system, including inhibition of platelet-activating factor, which is a potent platelet aggregant. By inhibiting PAF, ginkgo reduces platelet aggregation and prolongs bleeding time. It may also affect other pathways involved in hemostasis. These effects increase bleeding risk, particularly when combined with other antiplatelet or anticoagulant medications, or during surgical procedures. Ginkgo should be discontinued before surgery, typically 36 hours to 2 weeks depending on the specific recommendations, to allow platelet function to normalize. The preoperative drug history must specifically inquire about ginkgo and other supplements with bleeding risk.
Conclusion
Ginkgo biloba is the dietary supplement that contributes to bleeding risk through its antiplatelet effects and should be assessed in preoperative drug history to allow for timely discontinuation before surgery. Probiotics, coenzyme Q-10, and Ma Huang do not significantly increase bleeding risk, though Ma Huang has other cardiovascular risks that warrant attention. Therefore, ginkgo biloba is the correct supplement to identify for bleeding risk, and the nurse should ensure that it is included in the preoperative medication history and that appropriate instructions for discontinuation are provided.

The nurse is caring for a client receiving intravenous acyclovir. To prevent nephrotoxicity, what is the nurse's action?
A.
Provide a low-protein diet for one day before and two days after the acyclovir infusion
B. Increase the client's intake of food rich in vitamin C
C. Monitor urinary output every 30 minutes
D. Encourage PO fluid intake during the infusion and for 2 hours after the infusion
Rationale
To prevent nephrotoxicity from intravenous acyclovir, the nurse should encourage oral fluid intake during the infusion and for 2 hours after the infusion to maintain high urine flow and prevent drug crystallization in the renal tubules.
Acyclovir is an antiviral medication used to treat infections caused by herpes simplex virus, varicella-zoster virus, and other herpesviruses. Intravenous acyclovir is used for severe infections, in immunocompromised patients, or when oral therapy is not feasible. A significant adverse effect of IV acyclovir is nephrotoxicity, which occurs when the drug crystallizes in the renal tubules. Acyclovir has limited solubility in urine, and when urine becomes concentrated or when the drug is administered rapidly, it can precipitate and form crystals that obstruct tubules, causing inflammation and acute kidney injury. The risk is highest in dehydrated patients, those with pre-existing renal impairment, those receiving high doses, and those receiving rapid infusions. Prevention focuses on maintaining high urine flow to dilute the drug in the tubules and prevent crystal formation.
A) Provide a low-protein diet for one day before and two days after the acyclovir infusion
A low-protein diet has no role in preventing acyclovir nephrotoxicity. Protein intake does not affect drug solubility or crystallization in the tubules. This is not an appropriate intervention and would not prevent renal injury.
B) Increase the client's intake of food rich in vitamin C
Vitamin C does not prevent acyclovir nephrotoxicity. There is no relationship between vitamin C and acyclovir crystal formation. This is not an appropriate intervention and would not address the mechanism of renal injury.
C) Monitor urinary output every 30 minutes
While monitoring urinary output is important to detect decreased urine output that might indicate nephrotoxicity, it does not prevent the complication. Monitoring alone, without proactive hydration, is insufficient. The nurse should monitor output but must also implement preventive measures before problems occur. This option describes monitoring, not prevention.
D) Encourage PO fluid intake during the infusion and for 2 hours after the infusion
This is the correct preventive action. Adequate hydration maintains high urine flow, which dilutes acyclovir in the tubules and prevents crystal formation. The nurse should encourage the patient to drink fluids throughout the infusion and for several hours afterward to ensure continued urine output. If the patient cannot take adequate oral fluids, IV fluids may be administered to maintain hydration. This intervention addresses the mechanism of nephrotoxicity and is the standard preventive measure for IV acyclovir administration.
Conclusion
To prevent nephrotoxicity from IV acyclovir, the nurse should encourage PO fluid intake during and for 2 hours after the infusion to maintain high urine flow and prevent crystal formation in the renal tubules. Low-protein diet, vitamin C, and monitoring alone are not effective preventive measures. Therefore, encouraging fluids is the correct action that addresses the underlying mechanism of acyclovir-induced renal injury.
A nurse is teaching a group of nursing students about administering medications to older adult clients. Which statement by a student indicates a need for further teaching?
A.
Nonadherence to medications among older adult clients is due to the cost of medications
B. Changes in gastrointestinal function in older adult clients lead to an increase in serum drug levels
C. Most adverse drug reactions in older adult clients are related to altered renal function
D. Alteration in hepatic function requires more frequent drug dosing
Rationale
The statement that alteration in hepatic function requires more frequent drug dosing indicates a need for further teaching, as reduced hepatic function actually requires less frequent dosing or lower doses due to slowed drug metabolism and prolonged half-lives.
Aging is associated with numerous physiological changes that affect pharmacokinetics and pharmacodynamics, making medication management in older adults complex and requiring careful consideration. Hepatic function declines with age due to reduced liver mass, decreased hepatic blood flow, and diminished activity of drug-metabolizing enzymes, particularly the cytochrome P450 system. These changes result in slower drug metabolism, prolonged half-lives, and accumulation of drugs to higher levels than would occur in younger adults receiving the same doses. The appropriate adjustment for reduced hepatic function is to decrease the dose or extend the dosing interval, not to dose more frequently. More frequent dosing would lead to drug accumulation and increased risk of toxicity.
A) Nonadherence to medications among older adult clients is due to the cost of medications
This statement is generally accurate. Cost is a significant barrier to medication adherence in older adults, who often have fixed incomes and may be taking multiple medications. Polypharmacy increases the financial burden, and some older adults may skip doses, split pills, or not fill prescriptions to save money. This demonstrates understanding of a common adherence issue.
B) Changes in gastrointestinal function in older adult clients lead to an increase in serum drug levels
This statement has some accuracy. Age-related changes in GI function, such as decreased gastric acidity, slowed gastric emptying, and reduced intestinal motility, can alter drug absorption. For some drugs, these changes may lead to increased absorption or altered metabolism, potentially affecting serum levels. While not universally true for all medications, this statement reflects awareness that GI changes can affect drug levels.
C) Most adverse drug reactions in older adult clients are related to altered renal function
This statement is accurate. Renal function declines with age, with glomerular filtration rate decreasing progressively after age 40. This reduces drug excretion and leads to accumulation of renally eliminated drugs, which is a major cause of adverse drug reactions in older adults. Many commonly used medications, including digoxin, aminoglycosides, lithium, and certain diuretics, are renally eliminated and require dose adjustment. This demonstrates understanding of a key principle.
D) Alteration in hepatic function requires more frequent drug dosing
This statement indicates need for further teaching. Reduced hepatic function slows drug metabolism, meaning that drugs are cleared more slowly from the body. This requires less frequent dosing or lower doses, not more frequent dosing. More frequent dosing would lead to drug accumulation and toxicity. The student needs education on the relationship between hepatic function and drug dosing.
Conclusion
The student needs further teaching when stating that altered hepatic function requires more frequent drug dosing, as reduced metabolism actually requires less frequent dosing or lower doses. The other statements about cost, GI changes, and renal function are generally accurate. Therefore, the incorrect statement is about hepatic function requiring more frequent dosing, and the instructor should provide education on how age-related changes in liver function affect drug metabolism and dosing requirements.
The nurse is doing discharge teaching with the parent of an asthmatic child who will be going home on steroids. Which of these comments by the parent would indicate accurate understanding of discharge teaching these medications?
A.
Prolonged steroid use causes children to grow prematurely tall because they enhance growth
B. Steroids cause weight loss and dehydration in children because they cause type 1 diabetes
C. Prolonged steroid use may lead to addiction
D. My child may need to take a gastric acid suppressant while taking steroids
Rationale
The parent demonstrates understanding by stating that the child may need to take a gastric acid suppressant while taking steroids, recognizing that steroids can increase gastric acid secretion and ulcer risk, and that prophylaxis may be needed, especially with higher doses or prolonged use.
Corticosteroids are potent anti-inflammatory medications used in the management of various conditions, including asthma exacerbations, autoimmune diseases, and allergic disorders. While they are highly effective, they also have numerous potential adverse effects that require patient and family education. One important adverse effect is on the gastrointestinal system. Corticosteroids can increase gastric acid secretion, decrease mucus production, and reduce the protective mechanisms of the gastric mucosa, increasing the risk of peptic ulcer disease. This risk is higher when steroids are combined with nonsteroidal anti-inflammatory drugs, but can occur with steroid therapy alone, particularly at higher doses or with prolonged use. For this reason, some patients on steroid therapy may be prescribed gastric acid suppressants such as proton pump inhibitors or H2 receptor antagonists for prophylaxis. The parent's recognition of this potential need indicates understanding of one of the important side effects and management strategies for steroid therapy.
A) Prolonged steroid use causes children to grow prematurely tall because they enhance growth
This statement is completely incorrect and reflects a dangerous misunderstanding of steroid effects in children. Chronic steroid use in children causes growth suppression, not enhanced growth. Steroids interfere with growth hormone secretion, reduce insulin-like growth factor-1 activity, and have direct inhibitory effects on bone growth plates. This can result in decreased linear growth velocity and reduced adult height. This is one of the major concerns with long-term steroid use in the pediatric population and is why inhaled corticosteroids, which have minimal systemic absorption, are preferred for long-term asthma control in children. The parent who believes steroids enhance growth has a fundamental misunderstanding that could lead to inappropriate expectations and failure to monitor for actual growth suppression.
B) Steroids cause weight loss and dehydration in children because they cause type 1 diabetes
This statement contains multiple inaccuracies. Steroids typically cause weight gain, not weight loss, due to increased appetite, fluid retention, and redistribution of body fat leading to characteristic changes such as moon face and central obesity. Steroids can cause hyperglycemia and steroid-induced diabetes, but this is a form of insulin resistance similar to type 2 diabetes, not type 1 diabetes which is an autoimmune destruction of pancreatic beta cells. Steroid-induced diabetes does not cause weight loss or dehydration as initial manifestations. The parent who believes this has multiple misconceptions that need correction.
C) Prolonged steroid use may lead to addiction
This statement reflects confusion between physical dependence and addiction. Steroids do not cause addiction, which is a behavioral syndrome characterized by compulsive drug-seeking and use despite harm. However, chronic steroid use does cause physical dependence, meaning that the hypothalamic-pituitary-adrenal axis becomes suppressed and cannot produce adequate cortisol if steroids are withdrawn abruptly. This requires gradual tapering of the medication to allow the HPA axis to recover, but this is physical dependence, not addiction. The distinction is important because addiction carries stigma and implies behavioral issues that are not present with appropriate steroid use. The parent needs to understand the difference and the importance of not abruptly stopping steroids, but the term addiction is incorrect and misleading.
D) My child may need to take a gastric acid suppressant while taking steroids
This statement shows appropriate understanding of one potential complication of steroid therapy and its management. As explained, steroids increase gastric acid secretion and ulcer risk, and acid suppressants may be needed for prophylaxis, particularly if the child is on higher doses or prolonged therapy. The parent who recognizes this demonstrates awareness that steroids have effects beyond the respiratory system and that additional medications may be necessary to manage side effects. This understanding will help the parent adhere to the treatment plan and recognize why multiple medications may be prescribed.
Conclusion
The parent demonstrates accurate understanding by stating the child may need a gastric acid suppressant while taking steroids, recognizing the GI effects of these medications. Growth enhancement, weight loss and diabetes, and addiction are all incorrect understandings. Therefore, gastric acid suppressant is the correct statement, reflecting awareness of GI protection needs during steroid therapy.
A nurse is talking with a client who has peptic ulcer disease and starting therapy with sucralfate. What must the nurse include in the client's education?
A.
Take it whenever indigestion occurs
B. Take it immediately after meals
C. Take it with an antacid
D. Take it 30-60 minutes before meals
Rationale
The nurse must include that sucralfate should be taken 30 to 60 minutes before meals, as this timing allows the medication to form a protective barrier over the ulcer site before food stimulates acid secretion, maximizing its therapeutic effect.
Sucralfate is a cytoprotective agent used in the treatment of peptic ulcer disease. It is a complex of aluminum hydroxide and sulfated sucrose that, in the acidic environment of the stomach, undergoes polymerization and cross-linking to form a viscous, adhesive gel. This gel binds selectively to ulcerated areas of the gastric and duodenal mucosa, forming a protective barrier that shields the ulcer from further attack by acid, pepsin, and bile salts. The barrier also promotes healing by creating an environment conducive to mucosal repair. For sucralfate to be effective, it must be present in the stomach at the right time to form this barrier. Taking it 30 to 60 minutes before meals ensures that the medication has time to form the protective barrier before food enters the stomach and stimulates acid secretion. If taken after meals, food dilutes and displaces the medication, preventing it from adhering to the ulcer site. If taken too long before meals, the barrier may have degraded by the time food and acid are present.
A) Take it whenever indigestion occurs
Sucralfate is not an as-needed medication for symptom relief. It is taken on a scheduled basis, typically four times daily, to maintain a continuous protective barrier over the ulcer and promote healing. PRN use is not appropriate and would not provide the consistent protection needed for ulcer healing. The client needs to understand that regular dosing is essential for therapeutic effect.
B) Take it immediately after meals
Taking sucralfate immediately after meals is less effective because food in the stomach dilutes and displaces the medication, preventing it from forming a uniform protective barrier over the ulcer. Additionally, the buffering effect of food temporarily raises gastric pH, which may affect the polymerization of sucralfate. The optimal timing is before meals on an empty stomach.
C) Take it with an antacid
Antacids can interfere with sucralfate's mechanism of action. Sucralfate requires an acidic environment to polymerize and form its protective barrier. Antacids raise gastric pH, which can prevent this polymerization and reduce effectiveness. Additionally, antacids can bind to sucralfate and prevent it from adhering to the ulcer. If both medications are needed, they should be spaced at least 30 minutes apart, with sucralfate taken before meals and antacids taken between meals or at bedtime.
D) Take it 30-60 minutes before meals
This is the correct timing for sucralfate administration. Taking it on an empty stomach before meals allows the medication to form a protective barrier over the ulcer before food stimulates acid secretion. The barrier then remains in place during and after the meal, protecting the ulcer from the acid and pepsin that are secreted in response to eating. This timing maximizes the therapeutic effect and promotes ulcer healing.
Conclusion
The nurse must educate that sucralfate should be taken 30 to 60 minutes before meals. PRN use, after meals, or with antacids are all incorrect. Therefore, before meals is correct, ensuring optimal protective effect for ulcer healing.

Which statement by the client shows a correct understanding of how they should take their levothyroxine?
A.
I should take it after my noon meal
B. I should stop taking it if my thyroid-stimulating hormone level is high
C. My dose should skip the next dose if the medication makes me sleepy
D. I should take it before breakfast on an empty stomach
Rationale
The client shows correct understanding by stating they should take levothyroxine before breakfast on an empty stomach, as this timing ensures optimal absorption and consistent thyroid hormone levels.
Levothyroxine absorption is significantly affected by food, calcium, iron, and other medications. Taking it on an empty stomach, 30 to 60 minutes before breakfast, ensures maximal and consistent absorption, maintaining stable thyroid hormone levels. This is the standard recommendation for all patients taking levothyroxine. The client's correct statement indicates understanding of this essential administration instruction.
A) I should take it after my noon meal
Taking after a meal reduces absorption due to food interference and is incorrect.
B) I should stop taking it if my thyroid-stimulating hormone level is high
A high TSH indicates under-replacement, meaning the dose may need to be increased, not stopped. Stopping would worsen hypothyroidism.
C) My dose should skip the next dose if the medication makes me sleepy
Levothyroxine does not typically cause sleepiness. Skipping doses is dangerous and incorrect.
D) I should take it before breakfast on an empty stomach
This is correct and shows understanding.
Conclusion
The client demonstrates correct understanding by stating levothyroxine should be taken before breakfast on an empty stomach. After meals, stopping for high TSH, or skipping for sleepiness are all incorrect. Therefore, before breakfast is correct, reflecting knowledge of proper administration for optimal absorption.
RN Exams
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests