PHARMACOLOGY PRACTICE QUESTIONS
00:00
Which statement by a client indicates an understanding of self-care precautions when taking warfarin?
A.
My warfarin dose may need to be readjusted when I take a course of antibiotics.""
B. I should expect pink urine due to metabolic by-products of the dye used in this medication.""
C. Herbal remedies are fine
D. but I shouldn't take aspirin without consulting my provider.""
Rationale
The client demonstrates understanding of warfarin self-care precautions by stating that the warfarin dose may need to be readjusted when taking a course of antibiotics.
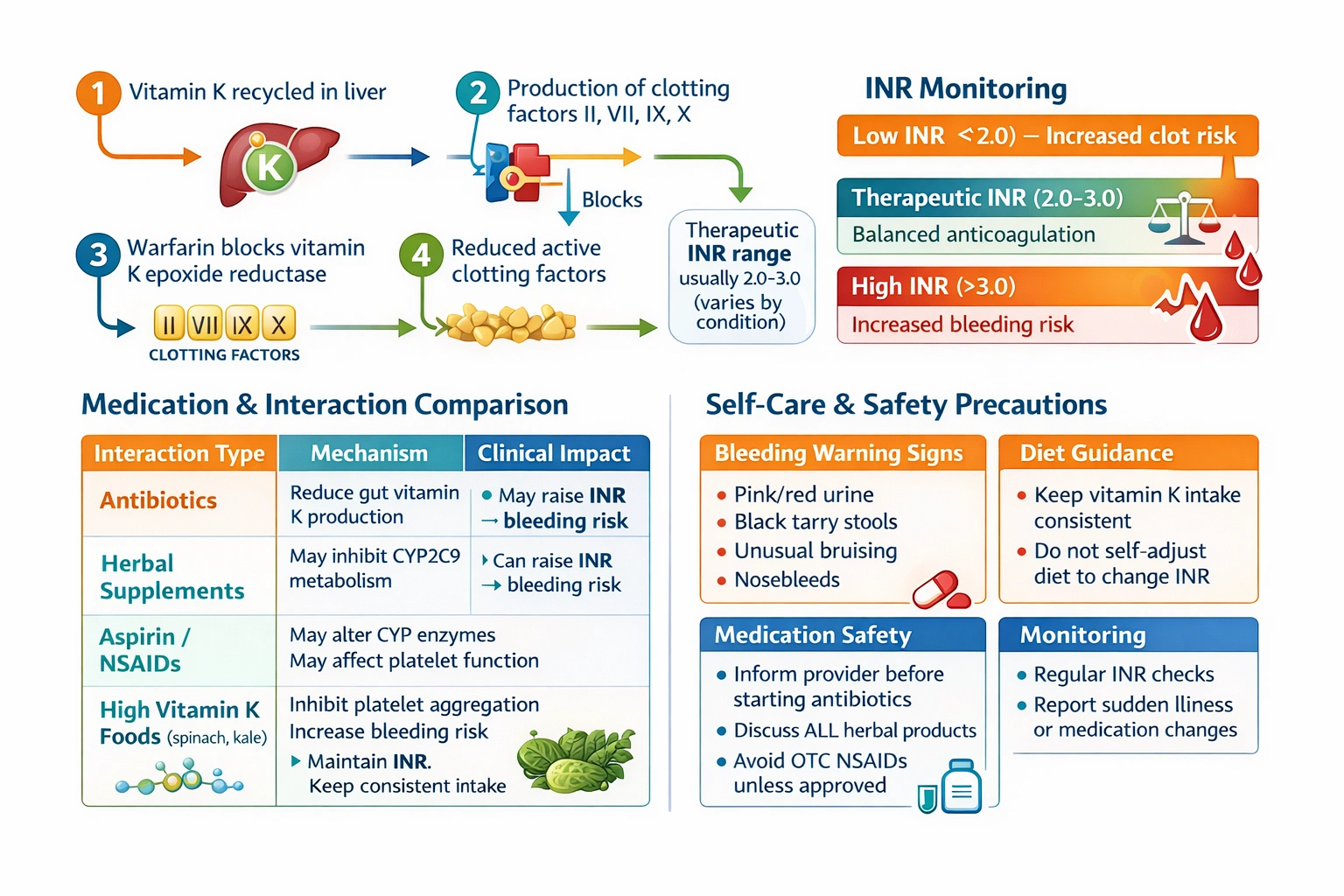
Warfarin is an oral anticoagulant medication that has been a cornerstone of therapy for preventing thrombotic events in conditions such as atrial fibrillation, deep vein thrombosis, pulmonary embolism, and in patients with mechanical heart valves for decades. Its mechanism of action involves inhibiting the enzyme vitamin K epoxide reductase, which is essential for the recycling of vitamin K in the liver. Vitamin K is a necessary cofactor for the synthesis of several clotting factors, specifically factors II, VII, IX, and X, as well as the anticoagulant proteins C and S. By inhibiting this recycling process, warfarin depletes the liver's supply of active vitamin K, thereby reducing the production of functional clotting factors and producing an anticoagulant effect. The intensity of this effect is measured by the prothrombin time, standardized as the international normalized ratio, which compares the patient's clotting time to a normal control. The therapeutic range for most indications is typically between 2 and 3, though this can vary based on the specific condition being treated. Managing warfarin therapy requires careful attention to numerous factors that can influence its anticoagulant effect, including dietary intake of vitamin K, concurrent medications, changes in health status, and various other variables. Antibiotics represent one of the most significant medication classes that can alter warfarin's effect, and a client who understands this demonstrates appropriate knowledge of self-care precautions.
A) "My warfarin dose may need to be readjusted when I take a course of antibiotics."
This statement accurately reflects a sophisticated understanding of warfarin therapy and the numerous factors that can influence its anticoagulant effect. Antibiotics can profoundly affect the international normalized ratio through multiple mechanisms that are important for any patient on warfarin to understand. Many broad-spectrum antibiotics, particularly those that target anaerobic bacteria, eliminate significant portions of the normal intestinal flora that produce vitamin K. The human gut contains bacteria that synthesize menaquinone, also known as vitamin K2, which is absorbed and contributes to the body's vitamin K pool. When antibiotics kill these bacteria, this endogenous source of vitamin K is reduced, which can potentiate the effect of warfarin and lead to an elevated INR. Additionally, some antibiotics may directly inhibit the hepatic cytochrome P450 enzymes responsible for metabolizing warfarin, particularly the more potent S-enantiomer of warfarin which is primarily metabolized by CYP2C9. This inhibition can lead to increased warfarin levels and enhanced anticoagulant effect. Other antibiotics may displace warfarin from protein-binding sites, temporarily increasing the concentration of free, active drug. The client who recognizes that antibiotic therapy may necessitate closer monitoring and possible dose adjustment demonstrates awareness of this critical safety consideration and understands that medication changes require communication with the healthcare provider rather than simply continuing the same dose without consideration of potential interactions.
B) "I should expect pink urine due to metabolic by-products of the dye used in this medication."
This statement reveals a significant misunderstanding of warfarin therapy and its potential adverse effects that could actually endanger the client if acted upon. Pink or reddish discoloration of the urine is never an expected or normal finding with warfarin use and should always raise immediate concern for hematuria, or blood in the urine, which can be an early sign of bleeding. Warfarin does not contain any dye in its formulation, nor does it produce colored metabolites that would discolor the urine. The client who believes that pink urine is an expected phenomenon may dismiss this important warning sign and delay seeking medical attention, potentially allowing a bleeding complication to progress. Hematuria can indicate that the INR has risen into a supratherapeutic range where the risk of bleeding is significantly increased, or it may signal the presence of a urinary tract pathology that is now bleeding because of the anticoagulated state. The appropriate response to noticing pink or red urine is to contact the healthcare provider immediately for evaluation, which would typically include checking the INR and a urinalysis. This statement suggests that the client requires additional education about the signs of bleeding that warrant immediate medical attention and the importance of not dismissing unusual symptoms as expected medication effects.
C) "Herbal remedies are fine, but I shouldn't take aspirin without consulting my provider."
This statement demonstrates a dangerous and incomplete understanding of warfarin precautions that could lead to serious adverse events. While the client correctly identifies that aspirin should not be taken without consulting the provider, the assertion that herbal remedies are "fine" represents a significant gap in knowledge that places the client at risk. Numerous herbal and dietary supplements have well-documented interactions with warfarin that can either increase bleeding risk or decrease anticoagulant effectiveness. St. John's wort, for example, is a potent inducer of cytochrome P450 enzymes, including CYP2C9 and CYP3A4, which metabolize warfarin, leading to decreased warfarin levels and reduced anticoagulant effect, potentially resulting in therapeutic failure and thrombotic events. Ginkgo biloba has antiplatelet effects through inhibition of platelet-activating factor and can increase bleeding risk when combined with warfarin without necessarily affecting the INR. Garlic supplements can also inhibit platelet aggregation and may potentiate the anticoagulant effects of warfarin. Ginseng has been reported to decrease warfarin's effectiveness by an unknown mechanism. Coenzyme Q10, which has a structure similar to vitamin K, may antagonize the effects of warfarin. Even seemingly innocuous supplements like fish oil can affect platelet function and increase bleeding risk. The client must understand that all herbal remedies, dietary supplements, and over-the-counter medications must be discussed with the healthcare provider before use, as even natural products can have potent pharmacological effects that interact with warfarin. This statement indicates that the client needs comprehensive re-education about the potential risks of herbal products.
D) "I should eat spinach to increase my iron count if my INR goes below two."
This statement reveals multiple fundamental misunderstandings about warfarin therapy, the meaning of the INR, the role of dietary vitamin K, and basic nutrition that require extensive re-education. First, the client confuses the concepts of iron supplementation and vitamin K intake. An INR below 2 indicates that the blood is clotting too quickly, meaning the anticoagulant effect is subtherapeutic and the client is not adequately protected against thrombotic events such as stroke or pulmonary embolism. This situation requires an adjustment in warfarin dosage, not an increase in iron. Second, spinach is high in vitamin K, which would actually further decrease the INR by providing substrate for the synthesis of vitamin K-dependent clotting factors in the liver, potentially worsening the subtherapeutic anticoagulation. The relationship between vitamin K and warfarin is competitive; higher vitamin K intake overcomes the inhibition of warfarin and promotes clotting factor synthesis. Third, the client should never self-manage warfarin therapy with dietary changes. The goal with vitamin K intake is consistency, not therapeutic adjustment. Patients are advised to maintain a consistent intake of vitamin K-rich foods so that the warfarin dose can be titrated to achieve therapeutic INR with that baseline intake. If the INR is below target, the provider should adjust the warfarin dose rather than the client attempting to manipulate their diet. Fourth, spinach is not a significant source of iron; while it does contain some iron, it also contains oxalates that inhibit iron absorption, making it a poor choice for increasing iron stores even if that were the goal. This statement indicates that the client requires comprehensive teaching about all aspects of warfarin management, including the meaning of INR values, the relationship between vitamin K and warfarin, the importance of dietary consistency, and the appropriate actions to take when INR results are outside the therapeutic range.
Conclusion
When evaluating which statement indicates a client's understanding of self-care precautions while taking warfarin, the correct choice is the acknowledgment that warfarin dose may need readjustment during antibiotic therapy, as this reflects awareness of a significant and common drug interaction. The statement about expecting pink urine from a nonexistent dye shows dangerous misunderstanding that could lead to ignoring an important sign of bleeding. The claim that herbal remedies are safe reveals incomplete knowledge of potentially serious herb-drug interactions that could either increase bleeding risk or reduce anticoagulant effectiveness. The plan to eat spinach for a low INR demonstrates confusion between iron and vitamin K, misunderstanding of the INR value's meaning, and an inappropriate attempt at dietary self-management rather than seeking professional dose adjustment. Therefore, only the statement about antibiotics and dose readjustment accurately reflects the understanding necessary for safe self-management of warfarin therapy.
A client will begin taking fexofenadine for hay fever. What education should be included regarding the use of this second-generation antihistamine?
A.
Citrus fruit juices can inactivate this class of medications
B. Fexofenadine has cholinergic side effects. It causes excessive salivation
C. Fexofenadine must be taken at bedtime
D. Fexofenadine must be taken apart from food
Rationale
The nurse should include in client education that citrus fruit juices can inactivate fexofenadine and other medications in this class by reducing their absorption, which is a crucial drug-food interaction that can significantly decrease the medication's effectiveness.
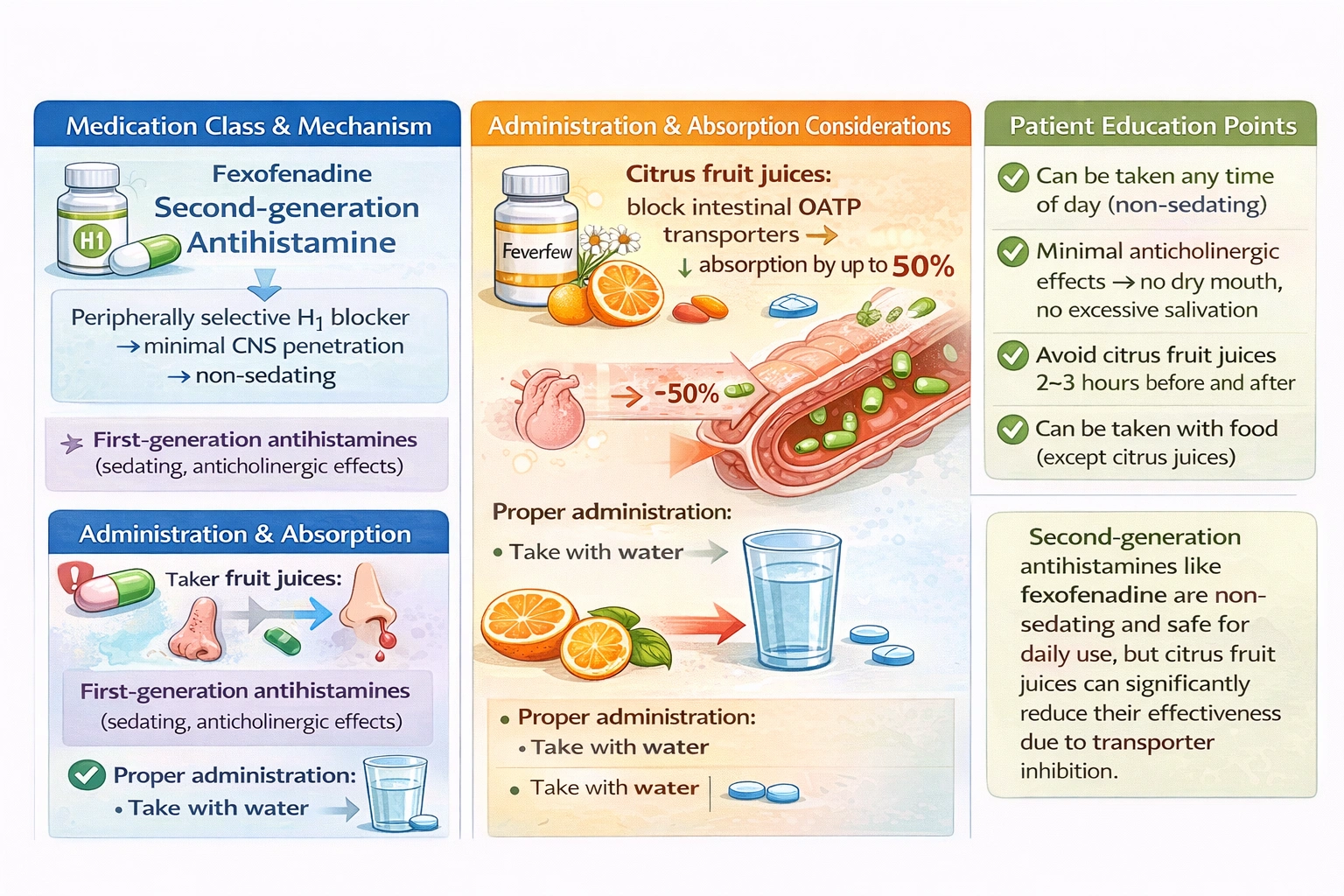
Fexofenadine is a second-generation antihistamine widely used for the treatment of seasonal allergic rhinitis, commonly known as hay fever, as well as chronic urticaria. Unlike first-generation antihistamines such as diphenhydramine, second-generation antihistamines were developed to be less sedating by limiting their penetration into the central nervous system. They achieve this through properties such as being substrates for P-glycoprotein, an efflux transporter that pumps drugs out of the brain, and having limited lipid solubility. Fexofenadine is effective at blocking peripheral H1 receptors, thereby reducing the symptoms of allergic reactions including sneezing, rhinorrhea, nasal congestion, and itchy, watery eyes. However, the effectiveness of fexofenadine depends on adequate absorption from the gastrointestinal tract into the systemic circulation, and this absorption can be significantly affected by certain foods and beverages. Understanding these interactions is essential for patients to achieve optimal therapeutic benefit from their medication.
A) Citrus fruit juices can inactivate this class of medications
This statement is accurate and represents a crucial piece of education that clients taking fexofenadine must understand. A significant drug-food interaction exists between fexofenadine and citrus fruit juices, particularly grapefruit juice, orange juice, and apple juice. The mechanism involves inhibition of organic anion transporting polypeptides, which are transport proteins in the intestinal wall responsible for uptake of fexofenadine from the gut lumen into the bloodstream. These OATP transporters, specifically OATP1A2 and OATP2B1, facilitate the absorption of fexofenadine. Citrus juices contain compounds such as naringin, hesperidin, and other flavonoids that inhibit these transporters, reducing the amount of fexofenadine that enters the circulation. Studies have shown that taking fexofenadine with grapefruit juice can reduce its bioavailability by up to 50%, meaning that only half of the medication is absorbed and available to exert its therapeutic effect. This level of reduction can render the medication ineffective for symptom control. The effect is most pronounced with grapefruit juice, but orange and apple juices also have significant impact. Clients should be instructed to take fexofenadine with water and to avoid citrus fruit juices for at least several hours before and after taking the medication to ensure adequate absorption and therapeutic effect.
B) Fexofenadine has cholinergic side effects. It causes excessive salivation
This statement reflects confusion between first-generation and second-generation antihistamines. First-generation antihistamines such as diphenhydramine, chlorpheniramine, and hydroxyzine have significant anticholinergic effects because they are not selective for peripheral H1 receptors and also block muscarinic acetylcholine receptors. These anticholinergic effects include dry mouth, urinary retention, constipation, blurred vision, and drowsiness. Excessive salivation is not an anticholinergic effect and is not associated with antihistamines at all. Fexofenadine, as a second-generation antihistamine, was specifically designed to be peripherally selective and to have minimal central nervous system penetration and minimal anticholinergic effects. It does not typically cause dry mouth or other anticholinergic symptoms, and it certainly does not cause excessive salivation. Providing this incorrect information would confuse the client and does not reflect the actual side effect profile of fexofenadine.
C) Fexofenadine must be taken at bedtime
This statement would lead to suboptimal management of hay fever symptoms. The recommendation to take antihistamines at bedtime originated with first-generation antihistamines, which cause significant sedation. Taking these medications at bedtime allowed the sedative effects to occur during sleep, minimizing daytime impairment while still providing some allergy relief. However, fexofenadine is a non-sedating, second-generation antihistamine that can and should be taken at any time of day when symptom control is needed. In fact, for hay fever, taking the medication in the morning is often recommended to provide coverage during the daytime when allergen exposure and symptoms are typically highest. Telling the client to take it at bedtime would mean they would have no medication effect during the day when they need it most, and they would be wasting the non-sedating advantage of this medication. The correct instruction is to take it at the same time each day, typically in the morning, with water and separate from citrus juices.
D) Fexofenadine must be taken apart from food
This statement is partially accurate but incomplete and potentially misleading. While fexofenadine should be taken apart from citrus fruit juices specifically, it does not need to be taken apart from food in general. In fact, taking fexofenadine with food does not significantly affect its absorption, and it can be taken with or without meals. The key education point is about the specific interaction with citrus juices, not about all food. Stating that it must be taken apart from food without specifying the citrus juice interaction could lead the client to unnecessarily take the medication on an empty stomach when that is not required, or to misunderstand that food in general is the problem. The nurse should provide specific, accurate information about the citrus juice interaction rather than a vague statement about food.
Conclusion
When educating a client starting fexofenadine for hay fever, the nurse must include that citrus fruit juices can inactivate this class of medications by inhibiting intestinal transporters and reducing absorption, potentially decreasing effectiveness by up to 50%. Fexofenadine does not have cholinergic side effects and does not cause excessive salivation; it is non-sedating and free of significant anticholinergic effects. It does not need to be taken at bedtime and can be taken in the morning for daytime symptom control. It does not need to be taken apart from all food, only from citrus juices. Therefore, the correct education is about avoiding citrus fruit juices and taking the medication with water instead.
A Client presents with tinea corporis, and the prescriber orders itraconazole. When educating the client about this medication, the nurse will include which statement?
A.
Use the medication for at least one week after the symptoms have cleared
B. Apply the medication over the entire body twice daily for two weeks
C. This drug is effective after a single application
D. Sun exposure will minimize the drugs' effects
Rationale
The nurse will include in client education that the medication should be used for at least one week after the symptoms have cleared, as fungal infections require treatment beyond symptom resolution to ensure complete eradication of the organism and prevent recurrence.
Tinea corporis, commonly known as ringworm, is a superficial fungal infection of the skin caused by dermatophytes, primarily from the genera Trichophyton, Microsporum, and Epidermophyton. These fungi infect the keratinized layers of the skin, hair, and nails, feeding on keratin and causing characteristic annular lesions with central clearing and advancing scaly borders. Treatment of dermatophyte infections requires antifungal therapy for an adequate duration to ensure complete eradication of the organism. The visible signs of infection, such as redness, scaling, and itching, often improve before the fungus is completely eliminated. If treatment is stopped at the first sign of improvement, residual fungal elements can repopulate and cause recurrence of the infection. This principle applies to both topical and systemic antifungal therapy, though the specific duration varies by medication and infection site. Itraconazole is an antifungal medication available in both oral and topical formulations that is effective against a wide range of fungal infections.
A) Use the medication for at least one week after the symptoms have cleared
This statement is accurate and represents an essential teaching point for any client receiving antifungal therapy. The rationale for continuing treatment after symptom resolution is based on the understanding that visible signs of infection reflect the host inflammatory response to the fungus, not the presence or absence of the organism itself. Fungal elements may still be present in the keratin layers even when the skin appears normal. Continuing treatment for an additional period ensures that these residual organisms are eliminated, reducing the risk of relapse. The specific duration of post-symptom treatment varies, but one week is a general guideline that applies to many antifungal regimens. The nurse should emphasize that completing the full course as prescribed, even after symptoms improve, is essential for cure.
B) Apply the medication over the entire body twice daily for two weeks
for tinea corporis and would represent a misunderstanding of how topical antifungals are used. Itraconazole for tinea corporis is typically administered orally, not topically. Even if a topical formulation were used, it would be applied only to the affected areas, not to the entire body. Applying antifungal medication over the entire body would be unnecessary, wasteful, and potentially irritating to healthy skin. The nurse should provide specific instructions about where and how to apply any topical medication, limiting application to the affected areas and a small margin of surrounding healthy skin.
C) This drug is effective after a single application
This statement is false and would lead to inadequate treatment. No antifungal medication for tinea corporis is effective after a single application or single dose. Fungal infections require an adequate course of therapy lasting days to weeks, depending on the specific medication and the extent of infection. A single application would not achieve sufficient drug levels in the keratin layers to eradicate the fungus, and the infection would persist or recur. The nurse must correct this misconception if the client expresses it.
D) Sun exposure will minimize the drugs' effects
This statement is not accurate for itraconazole. Some antifungal medications, particularly griseofulvin, can cause photosensitivity, making patients more susceptible to sunburn, but sun exposure does not minimize the drug's antifungal effects. The statement is misleading and could lead the client to believe that going in the sun might help the medication work, which is incorrect. If photosensitivity is a concern for a particular antifungal, the teaching should focus on sun protection, not on sun exposure enhancing effects.
Conclusion
When educating a client about itraconazole for tinea corporis, the nurse should include that the medication should be used for at least one week after symptoms have cleared to ensure complete eradication of the fungus and prevent recurrence. Applying over the entire body, expecting single-dose efficacy, or believing sun exposure minimizes effects are all incorrect and could lead to treatment failure. Therefore, the correct statement is about continuing treatment after symptom resolution, reflecting the principle that fungal infections require treatment beyond the visible signs of disease.

What should the nurse include in a client's discharge teaching when going home with a prescription for digoxin 0.125 mg by mouth once daily?
A.
You must be able to check your pulse
B. Take the digoxin at bedtime
C. Eat a diet high in bran, fiber, and calcium
D. Don't take digoxin if your heart rate exceeds 90 beats per minute
Rationale
The nurse should include in discharge teaching that the client must be able to check their pulse when taking digoxin, as pulse monitoring before each dose allows early detection of bradycardia, a sign of digoxin effect or toxicity, and guides decisions about holding the medication.
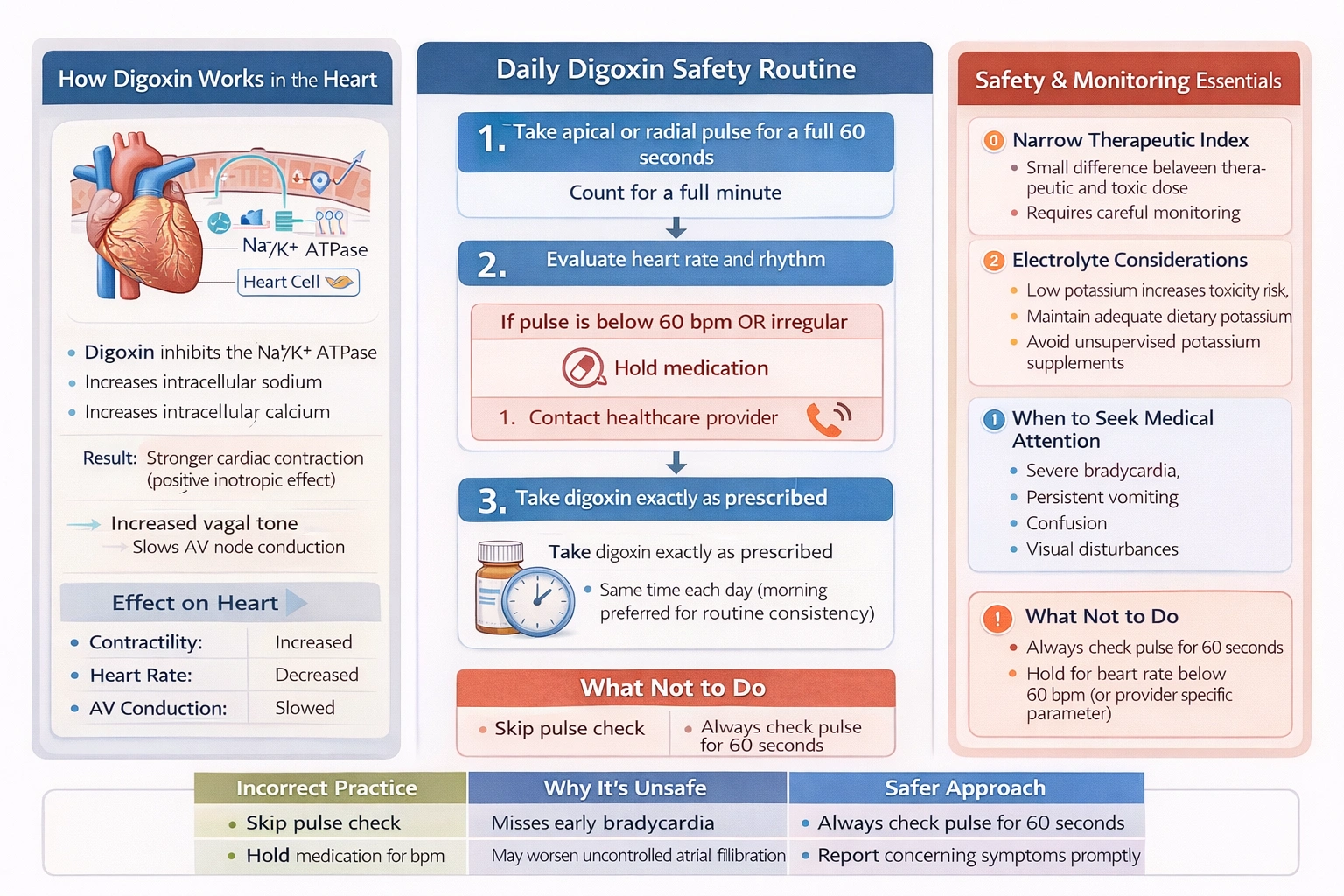
Digoxin is a cardiac glycoside that has been used for decades in the treatment of heart failure and atrial fibrillation. Its mechanism of action involves inhibition of the sodium-potassium ATPase pump in cardiac myocytes, which leads to increased intracellular sodium and subsequently increased intracellular calcium through the sodium-calcium exchanger. The increased calcium enhances myocardial contractility, producing a positive inotropic effect beneficial in heart failure. Additionally, digoxin increases vagal tone and decreases conduction through the atrioventricular node, making it useful for rate control in atrial fibrillation. However, digoxin has a narrow therapeutic index, meaning that the difference between a therapeutic dose and a toxic dose is small. Toxicity can manifest as gastrointestinal symptoms such as nausea, vomiting, and anorexia, neurological symptoms including visual disturbances and confusion, and most dangerously, cardiac effects including bradycardia, heart block, and various arrhythmias. Self-monitoring of pulse rate is a critical safety measure that empowers patients to participate in their own care and detect early signs of excessive digoxin effect.
A) You must be able to check your pulse
This is the essential teaching point for digoxin therapy and must be included in every discharge instruction. The client should be taught to take their pulse for one full minute before each dose of digoxin. They should be instructed to hold the dose and contact their healthcare provider if the pulse rate is below 60 beats per minute, or below the specific parameter provided by their provider, or if the rhythm is irregular. This monitoring allows early detection of bradycardia, which can indicate that digoxin levels are too high or that the medication is having an excessive effect. The nurse should demonstrate pulse-taking technique, have the client return the demonstration to ensure accuracy, and provide written instructions about the parameters for holding the medication. The client should also be taught about other signs of digoxin toxicity that warrant provider notification, including nausea, vomiting, loss of appetite, visual changes such as yellow-green halos or blurred vision, and unusual fatigue or weakness.
B) Take the digoxin at bedtime
This instruction is not correct and could lead to suboptimal management. Digoxin is typically taken in the morning for several reasons. Taking it at the same time each day is important for maintaining consistent blood levels, but morning dosing is preferred because it aligns with the timing of other medications and with daily routines. Bedtime dosing could make it difficult for the patient to monitor for effects, as they would be asleep during the peak action of the medication. Additionally, if the patient experiences any adverse effects, they might occur during sleep and go unnoticed. Some sources suggest that taking digoxin in the morning may also reduce the risk of nighttime arrhythmias, though this is not firmly established. The key point is that consistency is important, but bedtime is not the recommended time for most patients.
C) Eat a diet high in bran, fiber, and calcium
This dietary advice is not specifically relevant to digoxin therapy and could even be problematic if misinterpreted. A high-fiber diet is generally healthy and may be beneficial for overall cardiovascular health, but it does not directly affect digoxin therapy. The mineral of most concern with digoxin is potassium, not calcium. Hypokalemia, or low potassium levels, increases the risk of digoxin toxicity because digoxin and potassium compete for binding sites on the sodium-potassium ATPase pump. When potassium is low, more digoxin binds to the pump, increasing its effects and toxicity risk. Patients taking digoxin should be advised to maintain adequate potassium intake through diet, including foods such as bananas, oranges, potatoes, and leafy greens, but they should avoid potassium supplements unless specifically prescribed because hyperkalemia can also be dangerous. Calcium is not a primary concern, though extreme hypercalcemia can potentiate digoxin effects. The instruction about a diet high in bran, fiber, and calcium is not incorrect for general health but misses the most important nutritional consideration for digoxin therapy.
D) Don't take digoxin if your heart rate exceeds 90 beats per minute
This instruction is incorrect and could lead to inappropriate medication withholding. The usual instruction for digoxin is to hold the dose for a heart rate below 60 beats per minute, not above 90. Bradycardia indicates that digoxin may be having an excessive effect on the sinoatrial and atrioventricular nodes, slowing the heart rate too much. Tachycardia, on the other hand, may indicate that the underlying condition, such as atrial fibrillation with rapid ventricular response, is not adequately controlled, and withholding digoxin could worsen the situation. A heart rate above 90 might actually be an indication that the digoxin dose needs to be increased, not held. The client who follows this incorrect instruction could be holding medication when it is needed most, potentially leading to inadequate rate control and worsening of their cardiac condition. The correct instruction is to hold for rates below 60, not above 90.
Conclusion
In discharge teaching for digoxin, the nurse must include that the client must be able to check their pulse before each dose and hold the medication for rates below 60 or as specified. Bedtime dosing is not recommended. A diet high in bran, fiber, and calcium is not specifically relevant to digoxin safety. Holding digoxin for heart rates above 90 is incorrect and could be harmful. Therefore, pulse monitoring is the essential teaching that empowers the client to participate in safe medication management and detect early signs of toxicity.
A client taking warfarin develops hyperuricemia, and the provider orders prednisone for a flare-up of gout. What priority follow-up lab should the nurse seek from the provider?
A.
International normalized ratio
B. C-reactive protein
C. Creatinine clearance
D. Hepatic enzymes
Rationale
The priority follow-up lab the nurse should seek is an international normalized ratio, as prednisone can interact with warfarin and affect anticoagulation, requiring close monitoring to ensure therapeutic INR is maintained and to prevent bleeding or thrombotic complications.
Warfarin is an oral anticoagulant that has been used for decades to prevent and treat thrombotic events in conditions such as atrial fibrillation, venous thromboembolism, and mechanical heart valves. Its narrow therapeutic index requires careful monitoring of the INR, which measures the anticoagulant effect by comparing the patient's prothrombin time to a normal control. The target INR range varies by indication but is typically between 2 and 3 for most conditions. Many factors can alter warfarin's anticoagulant effect, including changes in diet, other medications, and various disease states. When a new medication is added to a warfarin regimen, close INR monitoring is essential because the new drug may either potentiate or inhibit warfarin's effect. Prednisone, a glucocorticoid used for its anti-inflammatory and immunosuppressive effects in conditions such as gout flares, is one such medication that can interact with warfarin.
A) International normalized ratio
This is the priority lab the nurse should ensure is ordered and monitored. The interaction between prednisone and warfarin is complex and not fully understood, but glucocorticoids have been reported to both increase and decrease the anticoagulant effect of warfarin in different patients. The mechanism may involve effects on clotting factor synthesis, protein binding, or other pathways. Regardless of the direction of effect, the addition of prednisone to a stable warfarin regimen can alter the INR, potentially pushing it out of the therapeutic range. If the INR becomes supratherapeutic, the patient is at increased risk for bleeding. If it becomes subtherapeutic, the patient is at increased risk for thrombosis. The nurse should advocate for INR monitoring shortly after prednisone is started, and then at regular intervals until the INR stabilizes. The frequency of monitoring will depend on the dose and duration of prednisone therapy and the individual patient's response.
B) C-reactive protein
C-reactive protein is a marker of inflammation that may be elevated in gout and other inflammatory conditions. It can be useful for monitoring the response to anti-inflammatory therapy, but it is not the priority for medication safety in this situation. The potential drug interaction between prednisone and warfarin poses a more immediate risk to the patient than monitoring inflammatory markers. While CRP may be checked to assess gout flare resolution, it does not guide anticoagulation management and is not the priority follow-up lab.
C) Creatinine clearance
Creatinine clearance assesses renal function, which is important for many medications but not specifically for the warfarin-prednisone interaction. Warfarin is hepatically metabolized, not renally eliminated, so changes in renal function do not directly affect warfarin levels or INR. Prednisone is also hepatically metabolized. While renal function is always important to monitor in patients with chronic diseases, it is not the priority for this specific medication interaction.
D) Hepatic enzymes
Hepatic enzymes assess liver function, which could theoretically affect warfarin metabolism since warfarin is hepatically metabolized. However, there is no specific concern that prednisone will cause acute liver injury that would affect warfarin metabolism. The more immediate concern is the direct drug interaction between prednisone and warfarin affecting INR, not an effect on liver function. While liver function tests may be monitored periodically in patients on chronic medications, they are not the priority follow-up for this new prescription.
Conclusion
When a client on warfarin starts prednisone for a gout flare, the priority follow-up lab is INR due to potential interaction affecting anticoagulation. CRP, creatinine clearance, and hepatic enzymes are not the priority for this medication change. Therefore, INR is correct, and the nurse should ensure it is checked soon after starting prednisone and monitored closely until stable.

A client is taking a drug that has potential toxic side effects. What will the nurse do?
A.
Monitor the function of all organs potentially affected by the drug
B. Continue the drug even if the client has signs of toxicity
C. Teach the client how to treat the symptoms if they develop
D. Discontinue the drug even if the client does not have signs of toxicity
Rationale
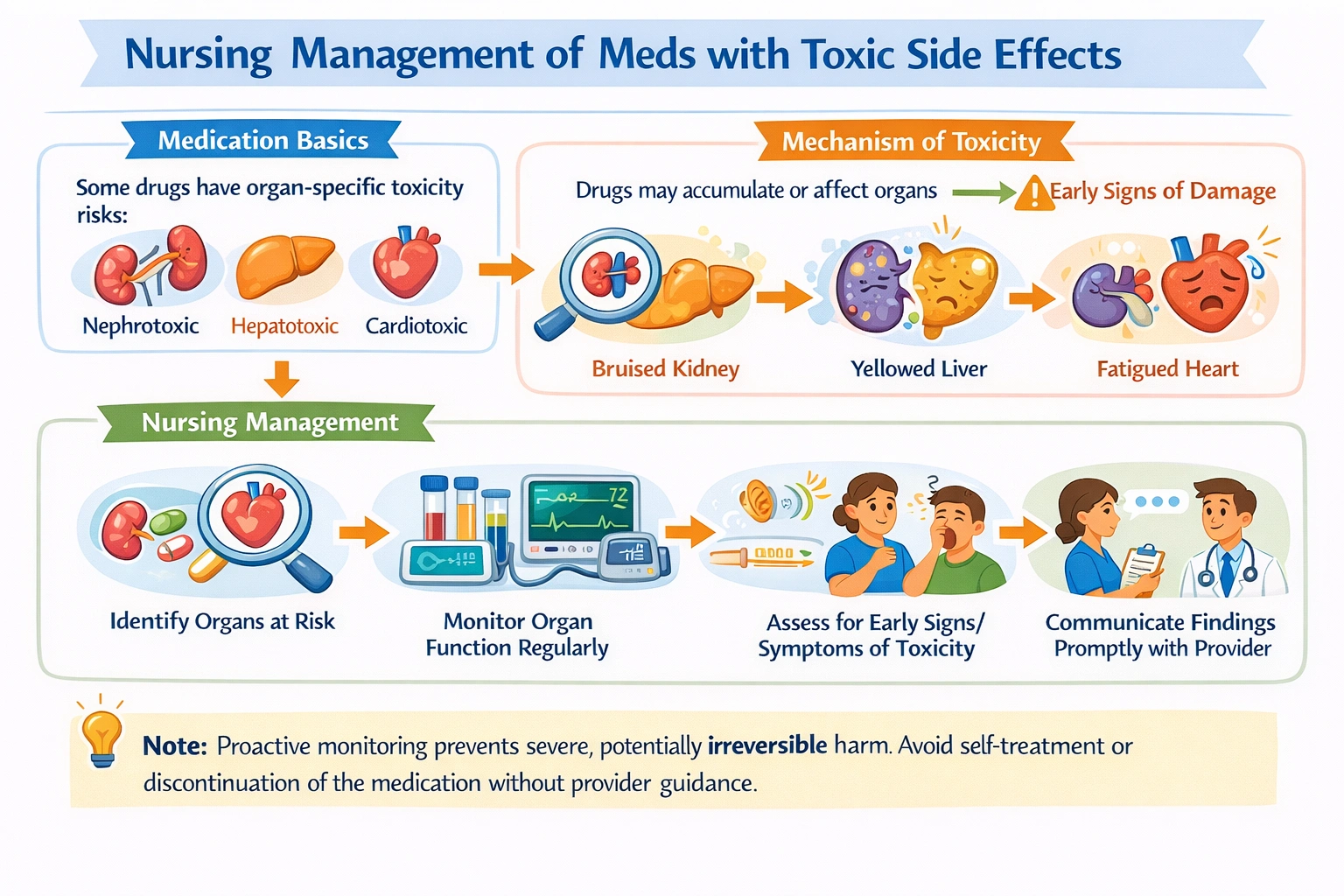
The nurse will monitor the function of all organs potentially affected by the drug, as proactive monitoring allows early detection of toxicity before it becomes severe, enabling timely intervention to prevent serious harm.
When a client is taking a medication with potential toxic side effects, the nurse's responsibility includes vigilant monitoring for early signs of toxicity. This involves understanding which organ systems are most at risk for the specific drug and implementing appropriate monitoring strategies. For example, for a nephrotoxic drug like an aminoglycoside antibiotic, the nurse monitors BUN and creatinine levels. For a hepatotoxic drug like isoniazid, the nurse monitors liver function tests. For a cardiotoxic drug like doxorubicin, the nurse monitors cardiac function through echocardiograms and ECGs. Monitoring also includes physical assessment for signs of toxicity, such as assessing for bruising or bleeding in a patient on anticoagulants, and client interview for symptoms like tinnitus in a patient on aspirin. Proactive monitoring allows detection of toxicity at an early, potentially reversible stage, before irreversible organ damage occurs.
B) Continue the drug even if the client has signs of toxicity
Continuing a drug despite signs of toxicity is dangerous and contraindicated. If toxicity is suspected, the drug should be held and the provider notified for further evaluation. Continuing could allow progression to more severe, potentially irreversible harm.
C) Teach the client how to treat the symptoms if they develop
Teaching clients to recognize symptoms is important, but they should not be taught to self-treat toxicity. Symptoms of toxicity require professional evaluation to determine the cause and appropriate management. Self-treatment could delay necessary intervention and lead to worsening of the condition.
D) Discontinue the drug even if the client does not have signs of toxicity
Discontinuing a drug without provider order and without signs of toxicity is inappropriate and could harm the client by interrupting necessary therapy. The decision to discontinue a medication should be made by the provider based on clinical judgment and monitoring results.
Conclusion
For a drug with potential toxic side effects, the nurse will monitor the function of all organs potentially affected. Continuing despite toxicity, teaching self-treatment, or discontinuing without signs are all incorrect. Therefore, organ function monitoring is correct, enabling early detection and prevention of serious toxicity.
The nurse is caring for a client who is receiving vancomycin. The nurse notes the client is experiencing flushing, rash, pruritus, and urticaria. The client's heart rate is 120 beats/min, and blood pressure is 92/57 mm Hg. What complication is the client experiencing?
A.
Red man syndrome
B. Rhabdomyolysis
C. Side effects
D. Stevens-Johnson syndrome
Rationale
The client is experiencing red man syndrome, an infusion-related reaction to vancomycin caused by rapid infusion leading to histamine release, characterized by flushing, rash, pruritus, urticaria, and sometimes hypotension and tachycardia.
Red man syndrome, also called red neck syndrome, is a common adverse reaction to vancomycin that occurs when the drug is infused too rapidly. It is not a true allergic reaction but rather a non-immunologic, dose-dependent release of histamine from mast cells and basophils. The histamine release causes vasodilation and increased vascular permeability, leading to the characteristic symptoms. Flushing, particularly of the face, neck, and upper torso, is the hallmark feature, giving the syndrome its name. Pruritus, urticaria, and rash are also common. In more severe cases, histamine release can cause significant vasodilation leading to hypotension and reflex tachycardia, as seen in this client with heart rate 120 and BP 92/57. Red man syndrome can be prevented or minimized by infusing vancomycin slowly, typically over at least 60 minutes, and by pre-treating with antihistamines in patients with a history of this reaction.
A) Red man syndrome
This is correct based on the symptoms and their association with vancomycin infusion. The nurse should stop or slow the infusion, administer diphenhydramine if ordered, and provide supportive care including IV fluids for hypotension.
B) Rhabdomyolysis
Rhabdomyolysis is muscle breakdown causing elevated creatine kinase and potential renal failure. Symptoms include muscle pain, weakness, and dark urine, not flushing and urticaria during infusion. This is incorrect.
C) Side effects
While these are side effects, "side effects" is too vague. Red man syndrome is the specific complication with a defined mechanism and management. Identifying it specifically allows for appropriate intervention.
D) Stevens-Johnson syndrome
SJS is a severe hypersensitivity reaction causing skin blistering and mucous membrane involvement, not flushing and urticaria during infusion. SJS typically develops over days, not during an infusion.
Conclusion
The client is experiencing red man syndrome from vancomycin infusion. Rhabdomyolysis, vague side effects, and Stevens-Johnson syndrome do not match the presentation. Therefore, red man syndrome is correct, and the nurse should take appropriate action to manage this infusion reaction.

The diabetic client is scheduled for a computer tomography scan with intravenous contrast. What education will the nurse provide?
A.
Hold metformin 24 hours to 48 hours before the CT
B. Resume metformin at half dose after the CT
C. Double the metformin dose after the CT
D. Hold metformin 48 hours after the CT
Rationale
The nurse should educate that metformin should be held 24 to 48 hours before the CT and held for 48 hours after the CT, as intravenous contrast can cause acute kidney injury, and metformin accumulation in renal impairment increases the risk of lactic acidosis.
Metformin is a biguanide oral hypoglycemic agent that is first-line therapy for type 2 diabetes. It works primarily by decreasing hepatic glucose production and improving peripheral insulin sensitivity. Metformin is eliminated renally, meaning it is excreted unchanged by the kidneys. Intravenous contrast dye used for CT scans can cause contrast-induced nephropathy, particularly in patients with diabetes, pre-existing renal impairment, heart failure, or dehydration. CIN is a form of acute kidney injury that typically occurs within 24 to 48 hours of contrast exposure. If a patient develops CIN and continues taking metformin, the drug can accumulate to toxic levels because it cannot be adequately excreted. This accumulation increases the risk of lactic acidosis, a rare but serious complication of metformin therapy with a high mortality rate. Lactic acidosis is characterized by elevated blood lactate levels, metabolic acidosis, and symptoms such as nausea, vomiting, abdominal pain, and altered mental status. To prevent this, metformin is typically held before and after contrast administration.
A) Hold metformin 24 hours to 48 hours before the CT
This is correct depending on the protocol and the patient's renal function. Some protocols recommend holding metformin 24 hours before contrast, while others recommend 48 hours for patients with additional risk factors. The nurse should follow institutional policy and the provider's orders.
B) Resume metformin at half dose after the CT
Resuming at half dose is not standard. Metformin should be resumed at the usual dose, but only after renal function has been confirmed to be normal. There is no indication for dose reduction after contrast unless there is persistent renal impairment.
C) Double the metformin dose after the CT
Doubling the dose is dangerous and incorrect. There is no rationale for increasing the dose after contrast, and doing so could increase the risk of adverse effects.
D) Hold metformin 48 hours after the CT
This is correct. Metformin should be held for 48 hours after contrast administration to allow monitoring of renal function. After 48 hours, if renal function is confirmed normal by checking serum creatinine, metformin can be resumed at the usual dose.
E) Take metformin as scheduled the day of the CT
This is incorrect and could be dangerous. Taking metformin on the day of contrast could lead to accumulation if CIN develops. The medication should be held.
Conclusion
For a diabetic client receiving IV contrast, education should include holding metformin before and after the CT to prevent accumulation in case of contrast-induced nephropathy. Resuming at half dose, doubling, or taking as scheduled are incorrect. Therefore, A and D are correct, ensuring patient safety by preventing metformin accumulation.

A client who is suffering from an acute gout attack wants to know how colchicine differs from probenecid and allopurinol in its actions. Which of these statements shows the need for further teaching regarding purpose and use of medications?
A.
Allopurinol prevents the synthesis of uric acid
B. All of these medications should be taken concurrently during an acute attack. NSAIDs should be added for pain control
C. Colchicine reduces inflammation caused by uric acid
D. Probenecid facilitates the elimination of uric acid in the nephrons
Rationale
The statement that all of these medications should be taken concurrently during an acute attack shows the need for further teaching, as this reflects confusion between the management of acute gout attacks and chronic urate-lowering therapy for prevention of future attacks.
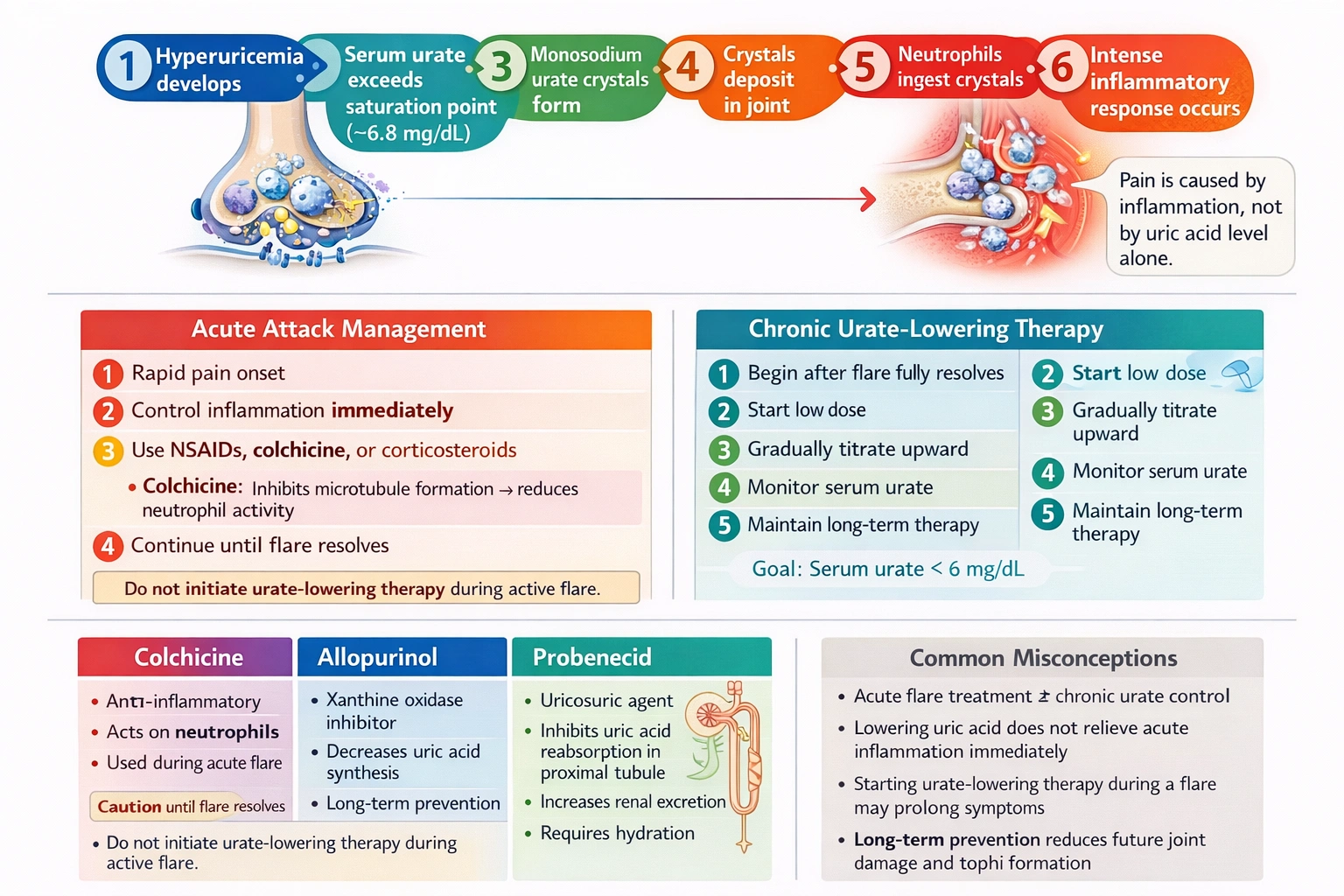
Gout is a disorder of purine metabolism characterized by hyperuricemia, which is an elevated serum urate level above the saturation point for monosodium urate crystal formation. When urate levels exceed approximately 6.8 mg/dL, the blood becomes supersaturated, and monosodium urate crystals can form and deposit in joints, soft tissues, and other structures. An acute gout attack, or gout flare, occurs when these crystals trigger an intense inflammatory response mediated by the innate immune system. The crystals are phagocytosed by synovial cells and macrophages, activating the NALP3 inflammasome and leading to the release of interleukin-1 beta and other pro-inflammatory cytokines. This cascade recruits neutrophils to the joint, where they release additional inflammatory mediators, causing the characteristic clinical presentation of sudden-onset, excruciating pain, swelling, erythema, and warmth in the affected joint. The management of gout involves two distinct phases with different therapeutic goals: treatment of acute attacks to relieve pain and inflammation, and long-term urate-lowering therapy to prevent future attacks and prevent complications such as tophi formation and joint destruction. The medications mentioned in this question have different roles in these two phases, and understanding these differences is essential for proper gout management.
A) Allopurinol prevents the synthesis of uric acid
This statement is accurate and demonstrates understanding of allopurinol's mechanism of action. Allopurinol is a xanthine oxidase inhibitor that works by inhibiting the enzyme responsible for the final steps in uric acid production. In the purine metabolism pathway, hypoxanthine is converted to xanthine, and xanthine is converted to uric acid, both steps catalyzed by xanthine oxidase. By inhibiting this enzyme, allopurinol reduces the production of uric acid, thereby lowering serum urate levels over time. This medication is used for chronic urate-lowering therapy, not for acute attack management, and the client who understands that it prevents uric acid synthesis has correctly grasped its basic mechanism. The client does not need further teaching on this specific point, though they may need education about when to start allopurinol therapy relative to an acute attack and the importance of consistent long-term use.
B) All of these medications should be taken concurrently during an acute attack. NSAIDs should be added for pain control
This statement demonstrates significant misunderstanding requiring further teaching, as it conflates the management of acute gout attacks with chronic urate-lowering therapy and shows lack of understanding of the different roles these medications play. During an acute gout attack, the priority is controlling inflammation and relieving pain. First-line options for acute attack management include nonsteroidal anti-inflammatory drugs such as indomethacin or naproxen, colchicine when started within the first 24 hours of symptom onset, and corticosteroids for patients who cannot tolerate the other options. Colchicine works by binding to tubulin and inhibiting microtubule polymerization, which impairs neutrophil chemotaxis, phagocytosis, and release of inflammatory mediators, thereby reducing the inflammatory response to urate crystals. However, urate-lowering therapies including allopurinol and probenecid are not used during acute attacks and should not be initiated at that time. In fact, starting allopurinol during an acute attack can actually prolong or exacerbate the attack by causing fluctuations in serum uric acid levels that may promote further crystal formation or shedding. The standard approach is to treat the acute attack with appropriate anti-inflammatory agents and then initiate urate-lowering therapy several weeks after the attack has completely resolved, typically starting at a low dose and gradually titrating upward to achieve target serum urate levels. The client's belief that all three medications should be taken together during an acute attack indicates confusion about the different purposes of these drugs and requires correction.
C) Colchicine reduces inflammation caused by uric acid
This statement is accurate and demonstrates understanding of colchicine's mechanism and role in gout management. Colchicine is an ancient medication derived from the autumn crocus, Colchicum autumnale, and has been used for centuries to treat gout. Its mechanism of action involves binding to tubulin, a protein that forms the structural component of microtubules. By binding to tubulin, colchicine prevents the polymerization of microtubules, which are essential for many cellular functions including cell division, intracellular transport, and, importantly for gout, neutrophil chemotaxis and phagocytosis. When urate crystals deposit in joints, they trigger an inflammatory response that involves neutrophil recruitment and activation. By impairing neutrophil function, colchicine reduces the inflammatory cascade and provides relief from the pain and swelling of acute gout. It is most effective when started within the first 24 hours of an attack. The client who understands that colchicine reduces inflammation caused by uric acid has correctly grasped its role and mechanism, and no further teaching is needed on this point.
D) Probenecid facilitates the elimination of uric acid in the nephrons
This statement is accurate and demonstrates understanding of probenecid's mechanism of action. Probenecid is a uricosuric agent that works by inhibiting the reabsorption of uric acid in the proximal convoluted tubule of the kidney. Under normal conditions, approximately 90% of filtered uric acid is reabsorbed in the proximal tubule through specific transporters, primarily URAT1. Probenecid inhibits these transporters, thereby reducing uric acid reabsorption and increasing its excretion in the urine. This lowers serum urate levels by enhancing renal elimination. Probenecid is used for chronic urate-lowering therapy in patients who are underexcreters of uric acid, meaning that their hyperuricemia is primarily due to reduced renal clearance rather than overproduction. It is not used during acute attacks and requires adequate hydration to prevent uric acid stone formation in the urinary tract. The client who understands that probenecid facilitates uric acid elimination in the nephrons has correctly grasped its mechanism and role in gout management.
Conclusion
The statement requiring further teaching is that all of these medications should be taken concurrently during an acute attack, with NSAIDs added for pain control. This reflects a fundamental misunderstanding of the different phases of gout management. Allopurinol prevents uric acid synthesis, which is accurate and shows understanding. Colchicine reduces inflammation caused by uric acid, which is accurate and shows understanding. Probenecid facilitates uric acid elimination in the nephrons, which is accurate and shows understanding. However, allopurinol and probenecid are urate-lowering therapies for chronic management to prevent future attacks, not for treating acute attacks. Initiating them during an acute attack can actually worsen or prolong the attack. Therefore, the client needs further education about the distinction between acute attack management and chronic urate-lowering therapy in gout.
A client who takes 325 mg of aspirin daily is scheduled for major surgery. Which of the following presurgical orders would the nurse expect to include in her teaching?
A.
Take two 81 mg tablets daily until surgery
B. Discontinue aspirin 7-10 days before surgery
C. Discontinue aspirin three days before surgery
D. Continue taking aspirin as scheduled
Rationale
The nurse would expect to include in preoperative teaching that the client should discontinue aspirin 7 to 10 days before surgery to allow for regeneration of new platelets with normal function, thereby reducing the risk of excessive bleeding during and after the surgical procedure.
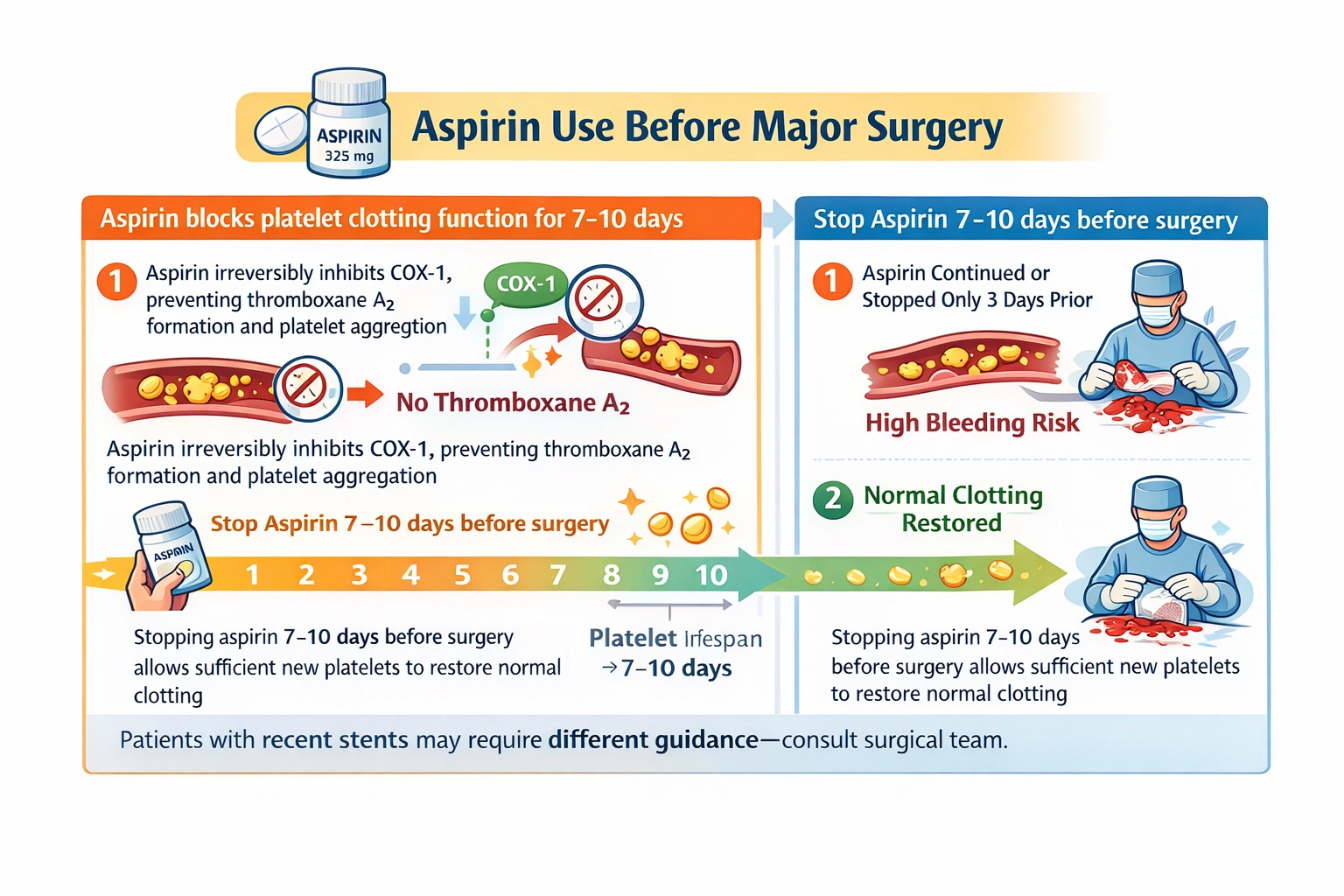
Aspirin, also known as acetylsalicylic acid, is one of the most widely used medications in the world, taken by millions of people for various indications including primary and secondary prevention of cardiovascular events, pain relief, anti-inflammatory effects, and fever reduction. The mechanism of action of aspirin involves irreversible inhibition of the enzyme cyclooxygenase-1, which is responsible for the production of thromboxane A2 in platelets. Thromboxane A2 is a potent vasoconstrictor and platelet aggregant that plays a critical role in normal hemostasis by promoting platelet plug formation at sites of vascular injury. When aspirin irreversibly inhibits COX-1, platelets lose their ability to produce thromboxane A2 for the remainder of their lifespan. Since platelets are anucleate cells that cannot synthesize new proteins, including new COX-1 enzyme, the antiplatelet effect of a single dose of aspirin persists for the entire 7 to 10 day lifespan of the affected platelets. This creates a significant challenge when patients taking aspirin require surgery, as the antiplatelet effect increases the risk of perioperative bleeding. The management of aspirin before surgery requires balancing the thrombotic risk of stopping aspirin against the bleeding risk of continuing it.
A) Take two 81 mg tablets daily until surgery
This instruction would not address the bleeding risk and demonstrates a misunderstanding of aspirin's pharmacology. Low-dose aspirin at 81 mg has the same antiplatelet effect as the 325 mg dose because both doses irreversibly inhibit COX-1 in platelets. The difference between 81 mg and 325 mg relates to the degree of systemic anti-inflammatory effects, not the antiplatelet effect. At any dose above about 30 mg, aspirin produces essentially complete inhibition of platelet COX-1. Therefore, continuing any form of aspirin until surgery, whether 81 mg or 325 mg, would maintain platelet inhibition and the associated bleeding risk. This instruction would not provide any safety benefit and would still expose the patient to increased surgical bleeding.
B) Discontinue aspirin 7-10 days before surgery
This is the correct presurgical instruction that the nurse would expect to include in teaching. The rationale for this timing is based on the platelet lifespan of approximately 7 to 10 days. When aspirin is discontinued, new platelets produced by the bone marrow are not exposed to the drug and therefore have normal COX-1 activity and normal ability to produce thromboxane A2. Over the course of 7 to 10 days, the population of platelets gradually shifts from being predominantly aspirin-inhibited to being predominantly normal. By the time 7 to 10 days have passed, enough new platelets have entered the circulation to restore adequate hemostatic function. The exact timing may vary based on the type of surgery, the indication for aspirin, and the surgeon's preference, but the 7 to 10 day window allows for adequate recovery of platelet function in most cases. For major surgery where bleeding risk is significant, this timing is standard. The nurse should confirm the exact timing with the surgical team and include this instruction in preoperative teaching, emphasizing the importance of following the specific timing provided.
C) Discontinue aspirin three days before surgery
Discontinuing aspirin only three days before surgery is insufficient to restore normal platelet function. With a platelet lifespan of 7 to 10 days, three days allows for replacement of only about 30% to 40% of the platelet population, leaving the majority of platelets still inhibited by aspirin. This would leave significant residual antiplatelet effect and increased bleeding risk. Three days is the typical recommendation for discontinuing other antiplatelet agents such as clopidogrel, which have different pharmacodynamics, but it is not adequate for aspirin. The nurse who provides this instruction would be giving incorrect information that could result in excessive surgical bleeding.
D) Continue taking aspirin as scheduled
Continuing aspirin as scheduled would maintain platelet inhibition throughout the perioperative period, significantly increasing bleeding risk during surgery. This instruction would only be appropriate in specific circumstances where the thrombotic risk of stopping aspirin outweighs the bleeding risk of continuing it. Examples include patients with recent coronary artery stents, particularly drug-eluting stents, where aspirin cessation carries a high risk of in-stent thrombosis and myocardial infarction. For most elective major surgeries in patients taking aspirin for primary prevention or even for secondary prevention without recent stents, the standard practice is to discontinue aspirin before surgery. The nurse would not expect this to be the routine instruction for a client scheduled for major surgery.
Conclusion
For a client taking 325 mg aspirin daily scheduled for major surgery, the nurse would expect to include instruction to discontinue aspirin 7 to 10 days before surgery to allow for regeneration of new platelets with normal function. Continuing aspirin or switching to a different dose without discontinuing does not address the bleeding risk. Discontinuing only three days before is insufficient to restore adequate platelet function. Therefore, discontinuation 7 to 10 days before is the correct presurgical instruction that the nurse should include in teaching, while also confirming the exact timing with the surgical team based on the specific procedure and the indication for aspirin therapy.
A nurse is concerned about renal function in an 84-year-old client who is taking several medications. What is a priority for the nurse to assess?
A.
Sodium levels
B. Serum Creatinine
C. Specific gravity
D. Troponin levels
Rationale
The priority assessment for renal function in an 84-year-old client taking multiple medications is serum creatinine, as this laboratory value provides the most clinically useful estimate of glomerular filtration rate and guides medication dosing for renally eliminated drugs.
Renal function declines progressively with age, even in the absence of specific kidney disease. This age-related decline is due to multiple factors, including loss of nephrons, reduced renal blood flow, and decreased glomerular filtration rate. By age 80, the average GFR is approximately half of what it was at age 30, even in healthy individuals. This has profound implications for medication management because many drugs are eliminated primarily by renal excretion. When renal function is impaired, these drugs can accumulate to toxic levels if standard adult doses are used. The elderly population is particularly vulnerable to adverse drug reactions, and impaired renal function is a major contributing factor. Assessing renal function is therefore essential for safe medication prescribing and administration in older adults.
A) Sodium levels
Sodium levels reflect hydration status and electrolyte balance but do not directly measure renal function. While renal dysfunction can affect sodium regulation, sodium alone is not a reliable indicator of glomerular filtration or drug excretion capacity. Hyponatremia or hypernatremia can occur with renal disease, but they can also occur with many other conditions, and normal sodium does not rule out significant renal impairment. This is not the priority for assessing renal function for medication safety.
B) Serum Creatinine
Serum creatinine is the priority assessment for renal function. Creatinine is a waste product of muscle metabolism that is produced at a relatively constant rate and is freely filtered by the glomerulus. Serum creatinine levels rise as GFR declines, making it a useful marker of renal function. However, in elderly patients, serum creatinine must be interpreted with caution because age-related muscle loss means that less creatinine is produced, so a "normal" creatinine may actually reflect significant renal impairment. For this reason, serum creatinine should be used to calculate estimated glomerular filtration rate using formulas such as the Cockcroft-Gault equation or the MDRD study equation. These calculations provide an estimate of GFR that guides medication dosing. The nurse should assess recent creatinine levels, calculate or review eGFR, and determine if dose adjustments are needed for renally eliminated medications.
C) Specific gravity
Specific gravity measures the concentration of urine and reflects the kidney's ability to concentrate urine, which is a function of the tubules, not the glomeruli. While it provides information about renal concentrating ability and hydration status, it is not a reliable indicator of overall renal function or drug excretion capacity. Specific gravity can be affected by many factors including fluid intake, diabetes mellitus, and diuretic use, and it is less useful than serum creatinine for medication dosing decisions.
D) Troponin levels
Troponin is a cardiac marker used to assess myocardial injury, not renal function. Elevated troponin indicates damage to heart muscle and is used in the diagnosis of myocardial infarction. It has no role in evaluating kidney function or medication clearance and is not relevant to the nurse's concern about renal function and medication safety.
Conclusion
When concerned about renal function in an elderly client taking multiple medications, the priority assessment is serum creatinine, which estimates glomerular filtration and guides medication dosing for renally eliminated drugs to prevent accumulation and toxicity. Sodium, specific gravity, and troponin do not directly measure renal function for this purpose. Therefore, serum creatinine is the correct priority, and the nurse should use it to calculate eGFR and ensure that all medications are dosed appropriately for the client's level of renal function.

A third grader is starting methylphenidate. What counseling should the nurse provide for the child's parents?
A.
Give the medication at bedtime
B. Store the medicine in a safe place; it is a controlled substance
C. Give the medication as needed
D. If you notice weight loss, switch dosing to every other day
Rationale
The nurse should counsel the parents to store the medicine in a safe place because it is a controlled substance with high potential for abuse and diversion, requiring secure storage to prevent misuse by the child or others in the household.
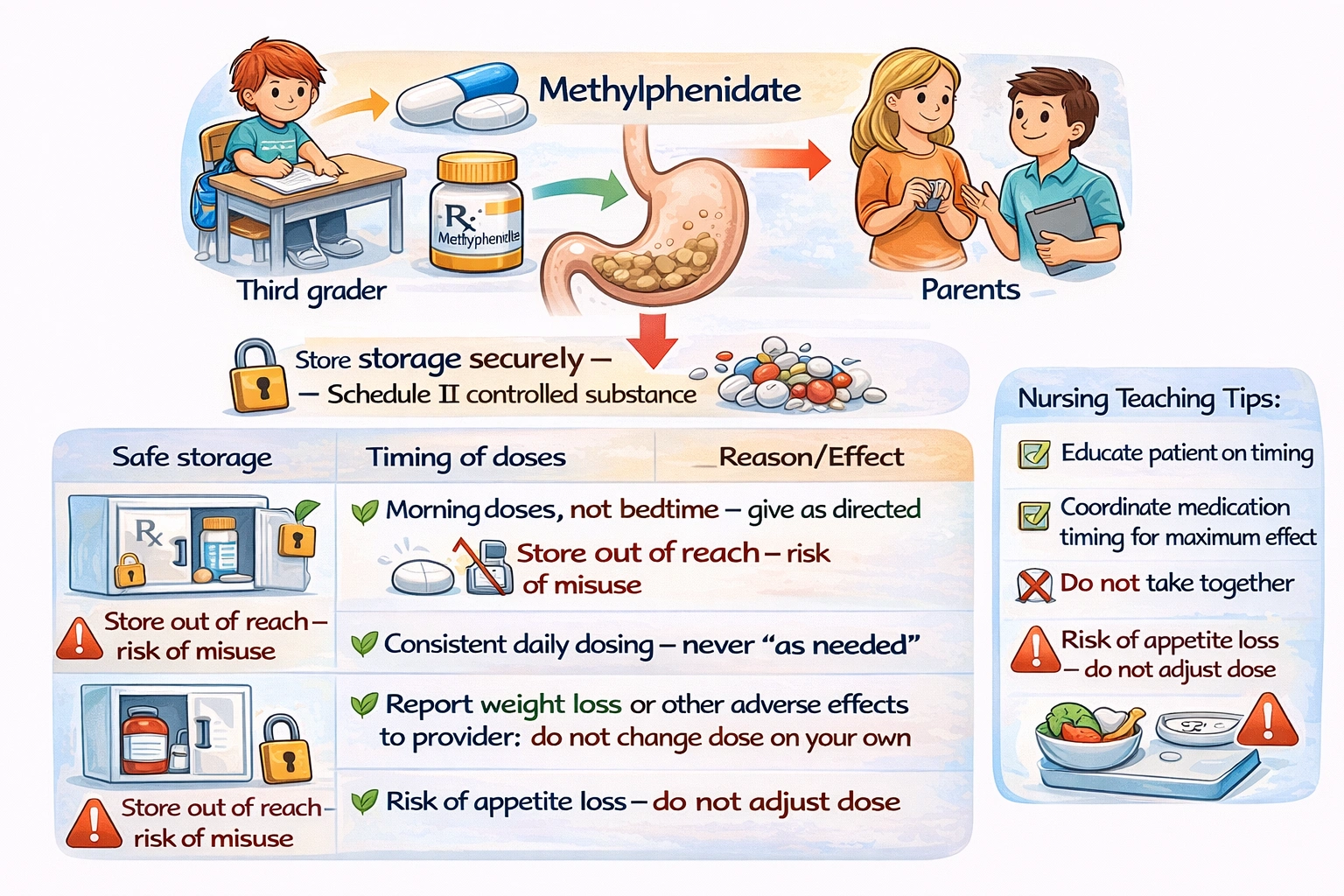
Methylphenidate is a central nervous system stimulant medication used primarily in the treatment of attention deficit hyperactivity disorder. It works by increasing the levels of dopamine and norepinephrine in the brain, which improves attention, focus, and impulse control in affected children. Methylphenidate is classified as a Schedule II controlled substance under the Controlled Substances Act due to its high potential for abuse and dependence. Stimulant medications are frequently diverted and misused by individuals without prescriptions, including other children in the household, adolescents, and adults who may seek them for cognitive enhancement, weight loss, or recreational purposes. The risks of diversion include not only legal consequences but also potential harm to others who may obtain and misuse the medication. Parents must understand their responsibility for secure storage and monitoring of this medication.
A) Give the medication at bedtime
This instruction is incorrect. Methylphenidate is a stimulant and should be taken in the morning to coincide with school hours when attention and focus are most needed. Taking it at bedtime would interfere with sleep, causing insomnia and potentially worsening ADHD symptoms due to sleep deprivation. The timing should be based on the dosing schedule prescribed, typically in the morning and possibly early afternoon if a second dose is needed, but never at bedtime.
B) Store the medicine in a safe place; it is a controlled substance
This instruction is correct and essential. As a Schedule II controlled substance, methylphenidate requires secure storage to prevent misuse, diversion, and accidental ingestion by other children. Safe storage means keeping the medication in a locked cabinet or container, out of reach of children and visitors, and monitoring the supply to ensure that the number of tablets matches what should be remaining. Parents should also be advised not to share the medication with anyone else, even if they think another child might benefit, as this is illegal and dangerous. This counseling helps protect the child, the family, and the community from the risks associated with controlled substance diversion.
C) Give the medication as needed
This instruction is incorrect. Methylphenidate for ADHD is taken on a regular schedule to maintain therapeutic blood levels and consistent symptom control. PRN or as-needed dosing is not appropriate for this condition. The medication should be taken consistently as prescribed, typically once or twice daily, to achieve the desired effects on attention and behavior throughout the school day and, if needed, into the evening for homework and other activities.
D) If you notice weight loss, switch dosing to every other day
This instruction is incorrect and dangerous. Weight loss is a known side effect of methylphenidate due to appetite suppression. Parents should report this to the provider, who may adjust the dose, timing, or consider alternatives such as ensuring the child eats before taking the medication, scheduling meals when medication effects are lower, or using medication holidays on weekends. The parents should not independently alter the dosing schedule. Every-other-day dosing is not standard and could lead to inconsistent symptom control, with symptoms returning on off days and difficulty re-establishing therapeutic effect.
Conclusion
When a child starts methylphenidate, the nurse must counsel parents to store the medicine in a safe place as it is a controlled substance with potential for abuse and diversion. Giving at bedtime would interfere with sleep. As-needed dosing is not appropriate for ADHD. Self-adjusting for weight loss is dangerous and should be reported to the provider instead. Therefore, secure storage is the essential counseling point that addresses the unique risks associated with stimulant medications.
A pregnant client asks the nurse if she can take antihistamines for seasonal allergies during her pregnancy. What will the nurse tell the client?
A.
The margin of safety for antihistamines is clearly understood for pregnant clients
B. Antihistamines should be avoided in pregnancy unless necessary
C. Second-generation antihistamines are completely safe to take during the first trimester
D. Antihistamines are safe to take during breastfeeding, but can cause spina bifida in pregnancy
Rationale
The nurse will tell the client that antihistamines should be avoided in pregnancy unless necessary, reflecting the general principle of minimizing medication exposure during pregnancy and using medications only when clearly indicated.
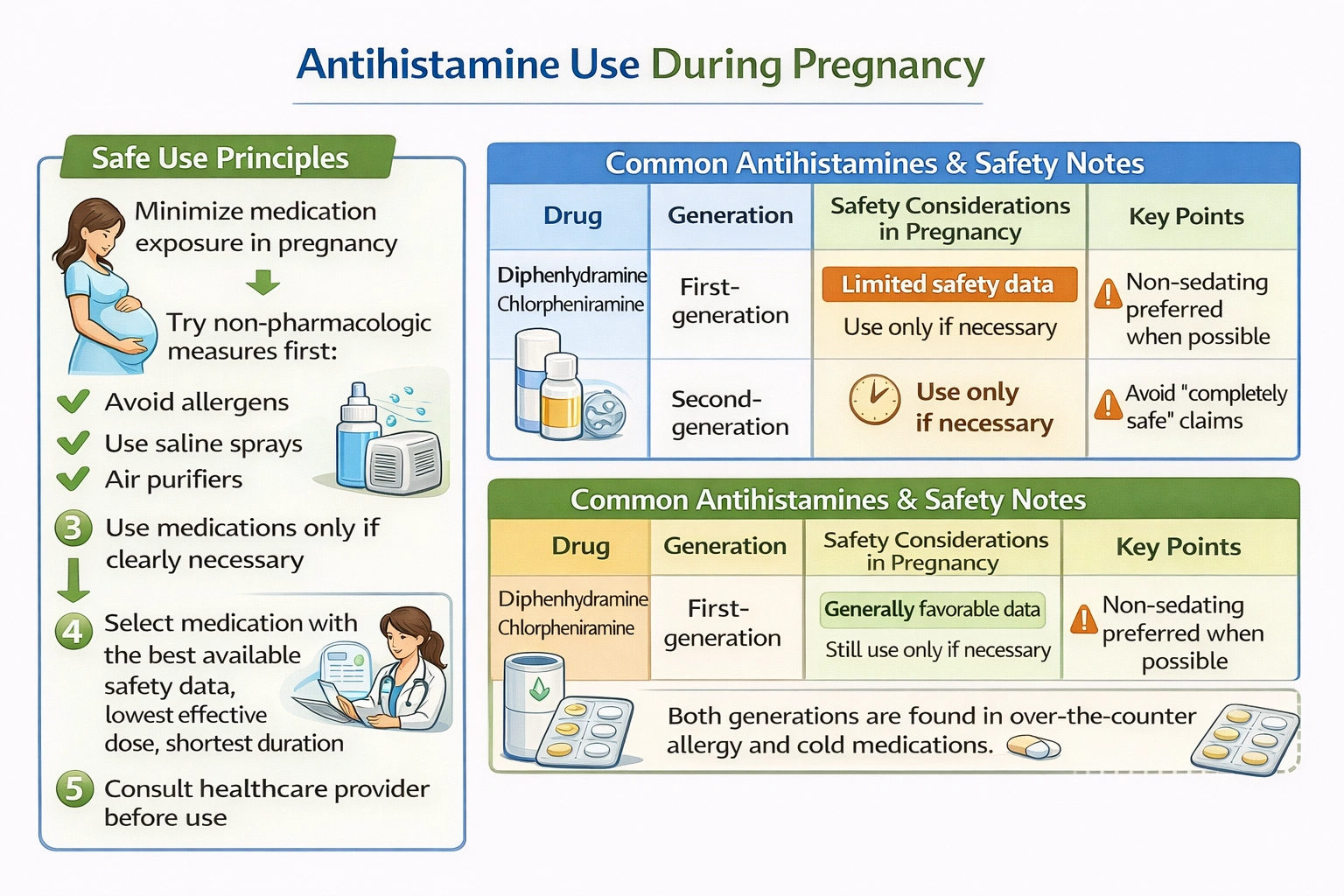
Medication use during pregnancy requires careful consideration of the risks and benefits for both the mother and the developing fetus. No medication can be guaranteed completely safe during pregnancy because pregnant women are typically excluded from clinical trials, and data on safety come from animal studies, case reports, pregnancy registries, and observational studies. The general principle is to minimize medication exposure, using non-pharmacologic measures when possible, and using medications only when the benefits clearly outweigh the potential risks. For seasonal allergies, non-pharmacologic measures include avoiding triggers, using saline nasal sprays, and using air purifiers. If medication is necessary, the safest option with the most favorable safety data should be chosen, and it should be used at the lowest effective dose for the shortest duration necessary.
A) The margin of safety for antihistamines is clearly understood for pregnant clients
This statement is false. The safety of most medications during pregnancy is not clearly understood due to lack of controlled studies in pregnant women. Available data are limited and often conflicting. The margin of safety is not clearly established for antihistamines or most other medications. This statement would provide false reassurance.
B) Antihistamines should be avoided in pregnancy unless necessary
This statement is accurate and reflects the principle of minimizing medication exposure during pregnancy. It acknowledges that while some antihistamines may be used when necessary, they should not be taken casually. This provides honest and appropriate guidance.
C) Second-generation antihistamines are completely safe to take during the first trimester
This statement is false. No medication is "completely safe" during the first trimester, when organogenesis occurs. While some second-generation antihistamines may have favorable safety profiles based on available data, they are not guaranteed safe and should only be used if clearly indicated. This statement provides false reassurance and could lead to inappropriate use.
D) Antihistamines are safe to take during breastfeeding, but can cause spina bifida in pregnancy
This statement is oversimplified and potentially misleading. Safety during breastfeeding varies among antihistamines, and some may be preferred over others. The claim about spina bifida is not accurate for antihistamines generally. Spina bifida is a neural tube defect associated with folate deficiency, not antihistamine use. This statement contains inaccurate information.
Conclusion
The nurse should tell the pregnant client that antihistamines should be avoided in pregnancy unless necessary, reflecting the principle of minimizing medication exposure. The other statements provide false reassurance or inaccurate information. Therefore, avoidance unless necessary is the correct advice, and the nurse should discuss non-pharmacologic measures and, if medication is needed, the importance of consulting the provider to select the safest option.
A client who has type 2 diabetes begins taking glipizide. Which statement by the client indicates a need for further education?
A.
I will begin by taking this once daily with breakfast
B. I may continue to have a glass of wine with dinner
C. I will need to check my blood sugar once daily or more
D. I should not take this medication if I have a sulfa allergy
Rationale
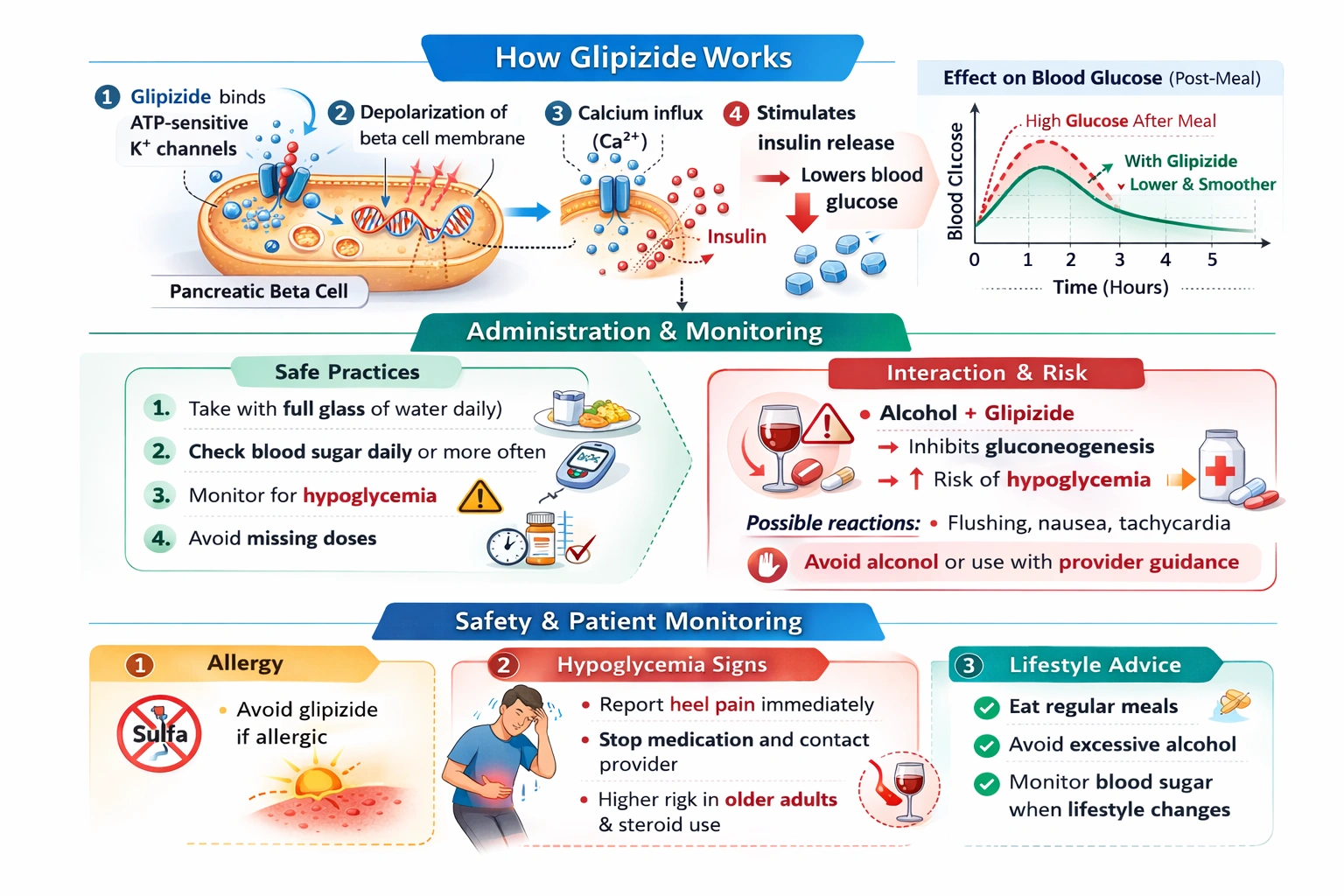
The statement that the client may continue to have a glass of wine with dinner indicates a need for further education, as alcohol can interact with glipizide to cause a disulfiram-like reaction and can significantly increase the risk of hypoglycemia.
Glipizide is an oral hypoglycemic agent belonging to the class of medications known as sulfonylureas, which have been a mainstay of type 2 diabetes management for decades. Sulfonylureas work by binding to specific receptors on the surface of pancreatic beta cells, which closes ATP-sensitive potassium channels and leads to cell membrane depolarization. This depolarization opens voltage-gated calcium channels, allowing calcium influx into the cell, which triggers the exocytosis of insulin-containing granules and increases insulin secretion. This mechanism is glucose-independent, meaning that sulfonylureas stimulate insulin release even when blood glucose levels are normal or low, which creates a significant risk of hypoglycemia. Alcohol can interact with sulfonylureas in two important ways that patients must understand to use these medications safely. First, alcohol can cause a disulfiram-like reaction when combined with some sulfonylureas, characterized by flushing, headache, nausea, vomiting, chest pain, and tachycardia. This occurs because alcohol is metabolized to acetaldehyde, and sulfonylureas can inhibit acetaldehyde dehydrogenase, leading to accumulation of acetaldehyde and these unpleasant symptoms. Second, and more importantly for diabetes management, alcohol can increase the risk of hypoglycemia by inhibiting gluconeogenesis in the liver. The liver normally produces glucose through gluconeogenesis, especially during fasting periods, and this process helps maintain stable blood glucose levels. When alcohol is present, it is preferentially metabolized, and gluconeogenesis is suppressed, reducing the liver's ability to produce glucose and increasing hypoglycemia risk, particularly if the patient has not eaten adequately.
A) I will begin by taking this once daily with breakfast
This statement shows appropriate understanding of how to initiate glipizide therapy. Glipizide is typically started at a low dose, often 5 mg once daily, taken with breakfast. Taking it with the first meal of the day serves several purposes. It coincides with the largest meal for many people, which helps to cover the postprandial glucose rise. It also reduces the risk of hypoglycemia because the medication is taken with food, and the meal provides glucose that can counteract any excessive insulin release. Additionally, morning dosing allows the peak effect of the medication to occur during daytime hours when the patient is awake and can recognize and treat hypoglycemia if it occurs. The client who understands this dosing schedule demonstrates appropriate knowledge of medication initiation.
B) I may continue to have a glass of wine with dinner
This statement indicates a need for further education about the significant interactions between alcohol and sulfonylureas. While some patients may be able to consume alcohol in moderation with careful monitoring, the statement as given suggests that the client does not appreciate the risks involved. Alcohol consumption while taking glipizide increases the risk of hypoglycemia through inhibition of hepatic gluconeogenesis. This risk is particularly significant if the patient drinks on an empty stomach, if they drink excessively, or if they have not eaten adequately. Additionally, some patients may experience the disulfiram-like reaction described earlier, which can be unpleasant and alarming. The client who believes they can simply continue their usual alcohol consumption without any precautions or concerns demonstrates a lack of understanding of these risks. The nurse should provide education about the potential interactions, advise moderation if alcohol is consumed at all, and emphasize the importance of never drinking on an empty stomach and of monitoring blood glucose more frequently when alcohol is consumed.
C) I will need to check my blood sugar once daily or more
This statement shows appropriate understanding of the importance of self-monitoring of blood glucose in diabetes management. Blood glucose monitoring is essential for assessing the effectiveness of glipizide therapy, detecting hypoglycemia, and guiding adjustments in medication, diet, and activity. The frequency of monitoring may vary depending on the patient's glycemic control, medication regimen, and individual circumstances, but checking at least once daily, often before breakfast, is a reasonable starting point. The client may need to check more frequently, such as before meals and at bedtime, especially when first starting therapy or after dose adjustments. The understanding that monitoring is necessary and that it may need to occur more than once daily demonstrates appropriate knowledge.
D) I should not take this medication if I have a sulfa allergy
This statement shows appropriate understanding of a potential contraindication to glipizide therapy. Glipizide is a sulfonylurea, and its chemical structure contains a sulfonamide group. Patients with a known allergy to sulfa antibiotics or other sulfonamide-containing medications may have cross-sensitivity to sulfonylureas and could experience allergic reactions. While not all patients with sulfa allergy will react to sulfonylureas, the potential exists, and caution is warranted. The client who understands that they should discuss this with their provider and that the medication may be contraindicated demonstrates appropriate knowledge of this important safety consideration.
Conclusion
The client needs further education when stating they may continue to have a glass of wine with dinner, as alcohol can interact with glipizide to increase hypoglycemia risk and potentially cause a disulfiram-like reaction. Taking glipizide with breakfast, monitoring blood glucose, and recognizing sulfa allergy precautions all demonstrate understanding. Therefore, the alcohol statement requires further teaching about the risks and necessary precautions.
A client who has been taking a glucocorticoid for several months arrives in the clinic. The nurse notes the client's cheeks appear full, and a prominent hump of fat is present on the upper back. The nurse will ask the provider to order which of these laboratory tests?
A.
Vitamin D levels
B. Serum electrolytes
C. Liver function tests
D. Tuberculin skin test
Rationale
The nurse will ask the provider to order serum electrolytes, as the client is exhibiting signs of Cushing's syndrome from chronic glucocorticoid use, and electrolyte imbalances, particularly hypokalemia, are common and require monitoring to prevent complications.
The client is exhibiting classic signs of Cushing's syndrome resulting from chronic glucocorticoid therapy. Moon face, characterized by rounding and fullness of the face, and buffalo hump, a prominent fat pad on the upper back, are characteristic features of glucocorticoid excess. These changes result from the metabolic effects of steroids, including redistribution of body fat to characteristic locations. Chronic glucocorticoid use produces multiple systemic effects beyond these visible changes. One important effect is on electrolyte balance through the mineralocorticoid activity of some glucocorticoids. While different steroids have varying degrees of mineralocorticoid activity, many can cause sodium and water retention, leading to hypertension and edema, and potassium wasting, leading to hypokalemia. Hypokalemia can cause muscle weakness, fatigue, cramping, and cardiac arrhythmias, including potentially life-threatening ventricular arrhythmias. Monitoring serum electrolytes, particularly potassium, is essential for detecting and managing these imbalances.
A) Vitamin D levels
Vitamin D levels may be relevant for bone health in patients on chronic steroid therapy due to the increased risk of osteoporosis. Steroids decrease bone formation, increase bone resorption, and impair calcium absorption, leading to bone loss and fracture risk. However, while important, vitamin D assessment is not the priority based on the physical findings presented. The visible signs of Cushing's syndrome suggest significant steroid exposure, and electrolyte imbalances are a more immediate concern that could have acute consequences.
B) Serum electrolytes
This is the priority laboratory test based on the client's presentation. The physical findings indicate significant glucocorticoid excess, which is often associated with electrolyte abnormalities. The nurse should request serum electrolytes, including potassium, sodium, chloride, and bicarbonate, to assess for hypokalemia and other imbalances. If hypokalemia is present, it may require treatment with potassium supplementation and possibly adjustment of the steroid regimen. Electrolyte monitoring is essential for preventing the cardiac and neuromuscular complications of hypokalemia.
C) Liver function tests
Liver function tests are not the priority for monitoring steroid side effects. While steroids can affect the liver in various ways, they are not primarily hepatotoxic, and significant liver injury is not a common complication of glucocorticoid therapy. Liver function tests may be indicated for other reasons but are not the priority based on the physical findings of Cushing's syndrome.
D) Tuberculin skin test
A tuberculin skin test may be indicated before starting steroids to rule out latent tuberculosis, as steroids can reactivate latent infections. However, the client has already been on steroids for several months, so this would have been done prior to initiation. It is not the priority now based on the physical findings of Cushing's syndrome.
Conclusion
For a client with signs of Cushing's syndrome from chronic glucocorticoid use, the nurse should request serum electrolytes to assess for hypokalemia and other imbalances that can result from mineralocorticoid effects. Vitamin D levels, liver function tests, and tuberculin skin testing are not the priority based on the presentation. Therefore, serum electrolytes are correct, allowing detection and management of potentially dangerous electrolyte abnormalities.
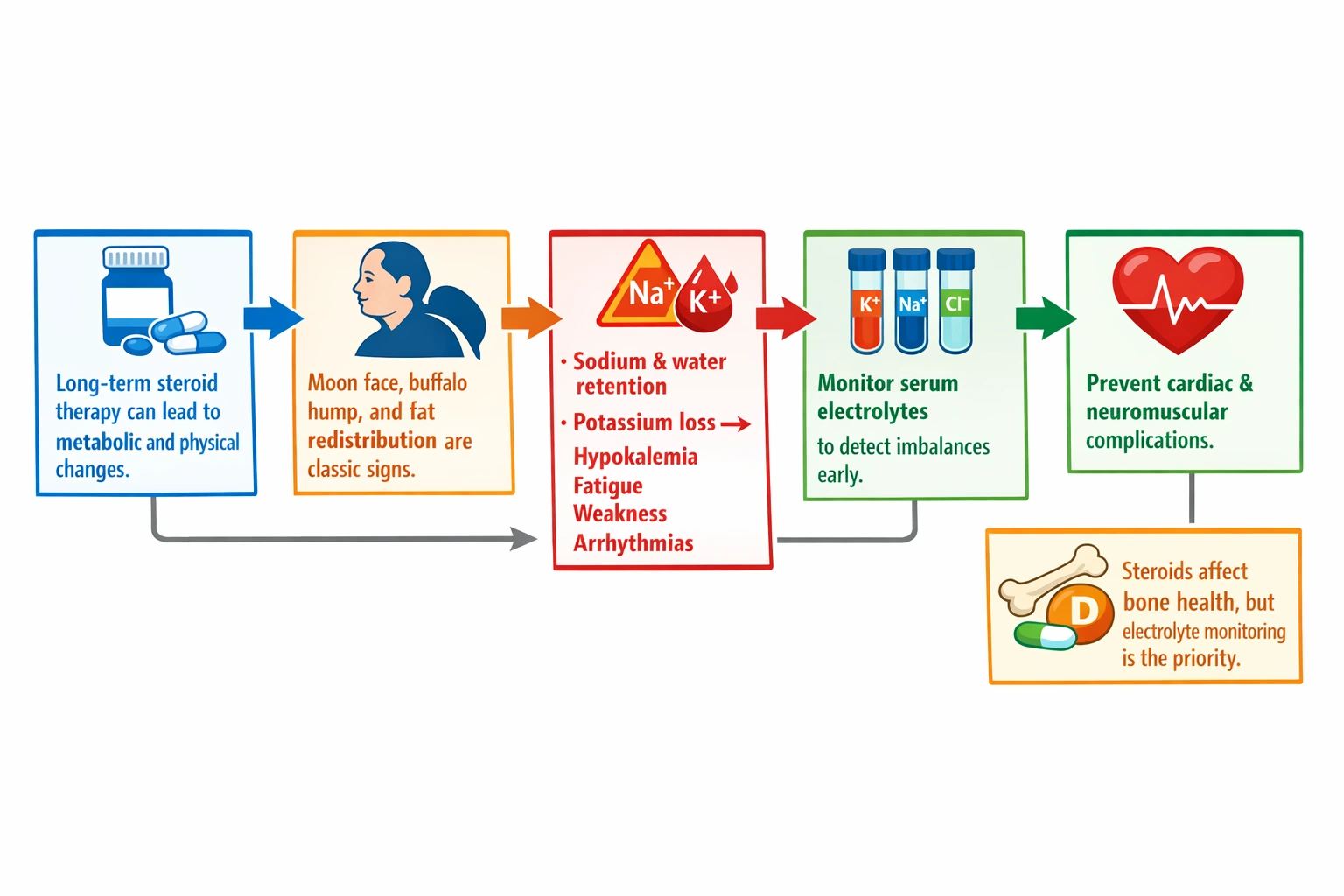
What must a nurse include in client education for an arthritic client taking high doses of aspirin?
A.
Aspirin is preferred to acetaminophen in the control of fevers in children
B. Call your provider for ringing in the ears
C. Aspirin is nephrotoxic
D. Report bruises, bleeding gums, tarry stools, and pink urine
Rationale
In client education for an arthritic client taking high doses of aspirin, the nurse must include instructions to call the provider for ringing in the ears, that aspirin is nephrotoxic, and to report signs of bleeding including bruises, bleeding gums, tarry stools, and pink urine, as these reflect the major potential adverse effects of high-dose aspirin therapy.
Aspirin has been used for decades in the management of various forms of arthritis, including rheumatoid arthritis and osteoarthritis, due to its anti-inflammatory and analgesic properties. However, the doses required for anti-inflammatory effects are significantly higher than those used for simple pain relief or cardiovascular protection. Anti-inflammatory doses of aspirin typically range from 3 to 6 grams per day, which approaches or exceeds the therapeutic range and increases the risk of toxicity. At these high doses, aspirin produces multiple predictable adverse effects that require patient education for early recognition and prevention of serious complications. These adverse effects include salicylate toxicity, nephrotoxicity, and bleeding due to antiplatelet effects. Understanding these risks and knowing when to report symptoms is essential for safe self-management.
A) Aspirin is preferred to acetaminophen in the control of fevers in children
This statement should not be included and is potentially dangerous. Aspirin use in children with viral illnesses, particularly influenza and varicella, is associated with Reye syndrome, a rare but serious condition characterized by encephalopathy and liver failure that has a high mortality rate. The association was first recognized in the 1980s, leading to public health warnings and a dramatic decrease in aspirin use in children. Acetaminophen or ibuprofen are the preferred antipyretics for children. Including this statement in client education for an arthritic client could lead to harm if the information is applied to children in the household or if the client misunderstands and uses aspirin inappropriately. This teaching point is incorrect and should never be included.
B) Call your provider for ringing in the ears
This is correct and essential teaching for high-dose aspirin therapy. Tinnitus, or ringing in the ears, is a classic early sign of salicylate toxicity. It occurs because salicylates affect the hair cells in the cochlea and can also increase cerebrospinal fluid pressure, affecting auditory function. Tinnitus typically occurs at serum salicylate levels approaching the toxic range, often above 20 to 30 mg/dL, and serves as an important warning sign that the dose may be too high. The client should be instructed to report this symptom promptly so that the dose can be adjusted or the medication changed before more serious toxicity develops, which can include hyperventilation, metabolic acidosis, fever, confusion, and even coma or death. This education enables early intervention and prevents progression to more severe toxicity.
C) Aspirin is nephrotoxic
This is correct information that clients taking high-dose aspirin must understand. Aspirin can cause nephrotoxicity through several mechanisms, particularly at high doses or with prolonged use. The primary mechanism involves inhibition of prostaglandin synthesis. Prostaglandins, particularly PGE2 and PGI2, are important mediators that help maintain renal blood flow, especially in conditions of reduced perfusion. By inhibiting cyclooxygenase and reducing prostaglandin production, aspirin can lead to renal vasoconstriction, reduced glomerular filtration rate, and sodium and water retention. This can manifest as acute kidney injury, particularly in patients with pre-existing renal impairment, heart failure, cirrhosis, or dehydration. Chronic use can lead to analgesic nephropathy, characterized by papillary necrosis and chronic interstitial nephritis. Clients with additional risk factors such as advanced age, diabetes, hypertension, or concurrent use of other nephrotoxic medications are at increased risk. The nurse should include this information so clients understand the importance of monitoring and follow-up, including regular renal function tests.
D) Report bruises, bleeding gums, tarry stools, and pink urine
This is correct and essential teaching for high-dose aspirin therapy. Aspirin irreversibly inhibits cyclooxygenase-1 in platelets, blocking the production of thromboxane A2, which is essential for platelet aggregation. This antiplatelet effect persists for the entire 7 to 10 day lifespan of the affected platelets and significantly increases bleeding risk. Clients may notice easy bruising, bleeding gums when brushing teeth, nosebleeds, or prolonged bleeding from minor cuts. More serious bleeding may manifest as melena, which is black, tarry stools indicating upper gastrointestinal bleeding, or hematuria, which is pink or red urine indicating bleeding in the urinary tract. The client must understand that these are not normal or expected effects but signs of potentially serious bleeding that require immediate reporting. The nurse should instruct the client to monitor for these signs and to contact the provider promptly if they occur, as they may indicate that the dose is too high or that there is an underlying bleeding source.
Conclusion
For an arthritic client taking high doses of aspirin, education must include calling the provider for tinnitus as an early sign of salicylate toxicity, understanding that aspirin is nephrotoxic and can cause renal impairment, and reporting signs of bleeding including bruises, bleeding gums, tarry stools, and pink urine due to the antiplatelet effect. The statement about aspirin being preferred for fever in children is incorrect and dangerous due to the association with Reye syndrome. Therefore, the correct teaching points are B, C, and D, which address the major potential adverse effects of high-dose aspirin therapy and empower the client to recognize early warning signs requiring intervention.
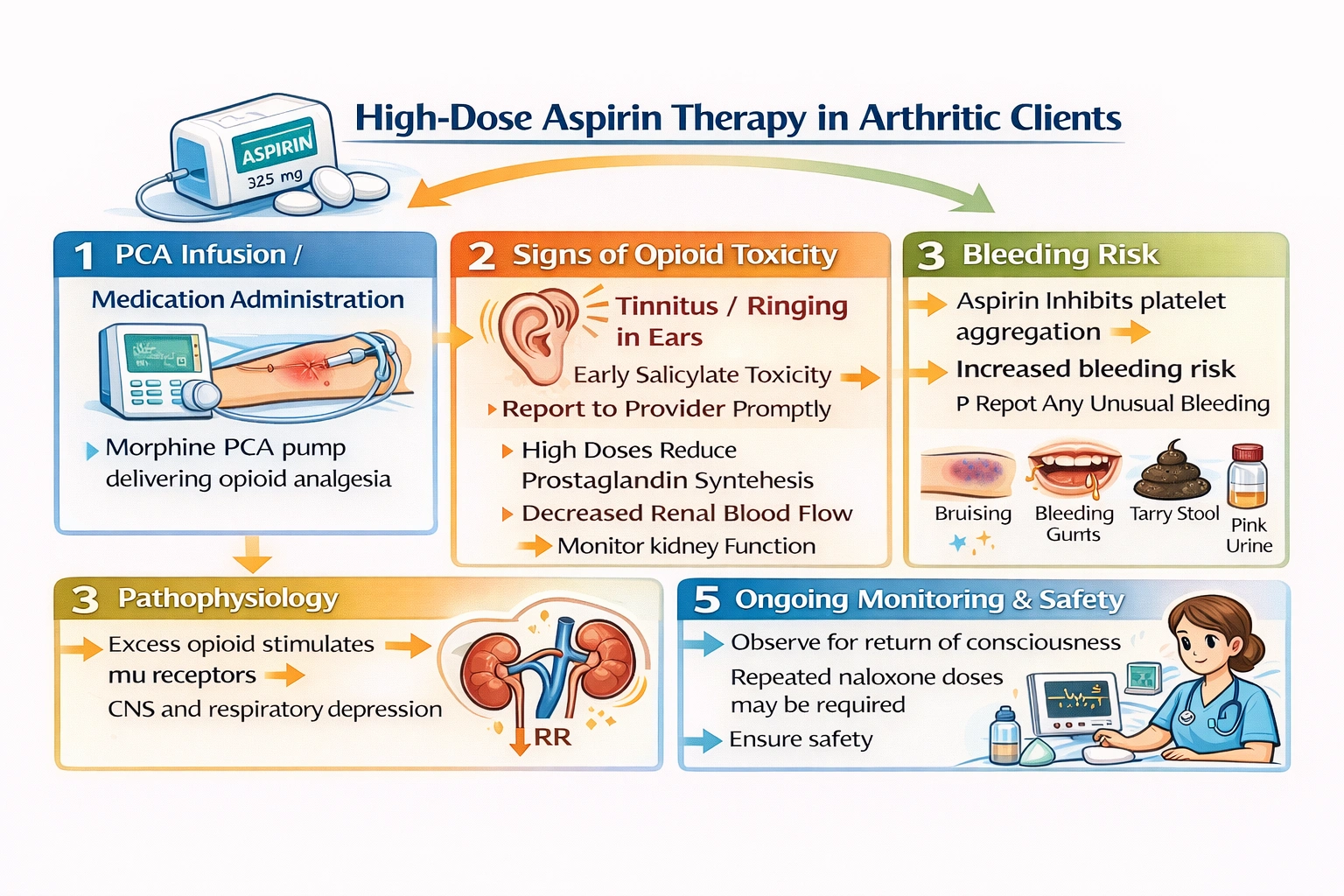
Which factors can alter a client's physiologic response to a medication?
A.
Height
B. Age
C. Liver disease
D. Genetic factors
Rationale
Factors that can alter a client's physiologic response to a medication include age, liver disease, genetic factors, and gender, as each of these influences the pharmacokinetic and pharmacodynamic processes that determine drug effects.
The study of how the body handles medications and how medications produce their effects is a complex field that recognizes significant interindividual variability in drug response. This variability means that the same dose of the same medication can produce different effects in different people, ranging from therapeutic benefit to lack of effect to toxicity. Understanding the factors that contribute to this variability is essential for nurses and other healthcare providers to individualize drug therapy, select appropriate doses, monitor for effects, and prevent adverse reactions. These factors can be broadly categorized as patient-specific characteristics, disease states, genetic variations, and environmental influences. They affect the pharmacokinetic processes of absorption, distribution, metabolism, and excretion, as well as the pharmacodynamic processes of drug-receptor interactions and cellular responses.
A) Height
Height alone does not significantly alter physiologic response to medications and is not typically considered a factor in drug dosing or response prediction. While body surface area, which incorporates both height and weight, is used for dosing certain medications such as chemotherapy agents and some pediatric medications, height by itself is not a primary determinant of drug distribution, metabolism, or effect. Weight is much more important for determining drug distribution volumes, as drugs distribute into body tissues based on factors such as lipid solubility and protein binding, which relate more to body composition than to height. Therefore, height is not included among the factors that significantly alter medication response, and it is not a correct answer for this question.
B) Age
Age significantly alters medication response through multiple mechanisms that affect both pharmacokinetics and pharmacodynamics across the lifespan. In neonates and infants, hepatic enzyme systems are immature, leading to reduced drug metabolism and prolonged half-lives. Renal function is also immature, with glomerular filtration rate reaching adult levels only by one to two years of age, slowing drug excretion. Body composition differs, with higher total body water and lower fat content affecting drug distribution. The blood-brain barrier is more permeable, increasing central nervous system penetration of drugs. At the other end of the spectrum, elderly clients experience age-related changes including decreased liver mass and blood flow, reducing drug metabolism, decreased renal function, reducing drug excretion, increased body fat and decreased lean body mass and total body water, altering drug distribution, and decreased serum albumin, affecting protein binding of highly bound drugs. Additionally, elderly patients often take multiple medications, increasing the potential for drug interactions. These age-related changes require dose adjustments and careful monitoring across the lifespan, making age a critical factor in medication response.
C) Liver disease
Liver disease profoundly alters medication response by impairing the liver's ability to metabolize drugs. The liver is the primary site for drug biotransformation through phase I reactions, which include oxidation, reduction, and hydrolysis, and phase II reactions, which involve conjugation with glucuronide, sulfate, or other molecules to make drugs more water-soluble and easier to excrete. Liver disease, including conditions such as cirrhosis, hepatitis, hepatic fibrosis, and metastatic disease, reduces the activity of drug-metabolizing enzymes, particularly the cytochrome P450 system. This leads to decreased drug clearance, prolonged half-lives, and accumulation of drugs to potentially toxic levels. Liver disease also decreases the synthesis of albumin and other plasma proteins, reducing protein binding and increasing the free fraction of highly protein-bound drugs. Portal hypertension and altered hepatic blood flow can affect drug delivery to the liver. Additionally, liver disease can impair the production of clotting factors, affecting response to anticoagulants, and can alter drug distribution due to ascites and changes in body water. These effects require dose reduction or extended dosing intervals for many medications and careful monitoring for signs of toxicity.
D) Genetic factors
Genetic factors significantly influence medication response through the field of pharmacogenomics, which studies how genetic variations affect drug metabolism, transport, and target interactions. Genetic polymorphisms in cytochrome P450 enzymes are among the most important and well-studied examples. For instance, variations in CYP2D6 can classify individuals as poor metabolizers, who have little or no enzyme activity and are at risk for toxicity from drugs metabolized by this pathway, intermediate metabolizers, extensive metabolizers who have normal activity, and ultra-rapid metabolizers who have multiple gene copies and may clear drugs so quickly that therapeutic levels are not achieved. Similar polymorphisms exist for CYP2C19, CYP2C9, and other enzymes. Genetic variations also affect drug transporters such as P-glycoprotein, which pumps drugs out of cells and affects absorption and distribution, and drug targets such as receptors and enzymes, which can alter sensitivity to drug effects. These genetic differences explain why some patients require higher or lower doses of medications such as warfarin, clopidogrel, codeine, and many others, and why some patients experience unusual adverse effects or lack of therapeutic response.
E) Gender
Gender affects medication response through multiple physiological and hormonal mechanisms. Men and women differ in body composition, with women generally having a higher percentage of body fat and lower total body water than men of similar weight. This affects the distribution volume of both lipid-soluble and water-soluble drugs. Gastric motility and emptying differ between genders, potentially affecting drug absorption. Hepatic enzyme activity can be influenced by sex hormones, with some cytochrome P450 enzymes showing gender differences in expression and activity. For example, CYP3A4, which metabolizes many drugs, may have higher activity in women. Renal function, when normalized for body size, differs between genders. Hormonal fluctuations during the menstrual cycle, pregnancy, and menopause can affect drug response. Women may experience different adverse effect profiles and may respond differently to certain drug classes. Historically, clinical trials under-represented women, leading to less understanding of gender-specific responses, but gender is now recognized as an important factor in pharmacotherapy that requires consideration in drug selection, dosing, and monitoring.
Conclusion
Factors that alter medication response include age, which affects drug metabolism, excretion, and sensitivity across the lifespan, liver disease, which impairs drug metabolism and protein binding, genetic factors, which determine individual variations in drug-metabolizing enzymes, transporters, and receptors, and gender, which influences body composition, hormone levels, and enzyme activity. Height alone is not a significant factor in medication response. Therefore, the correct selections are age, liver disease, genetic factors, and gender.
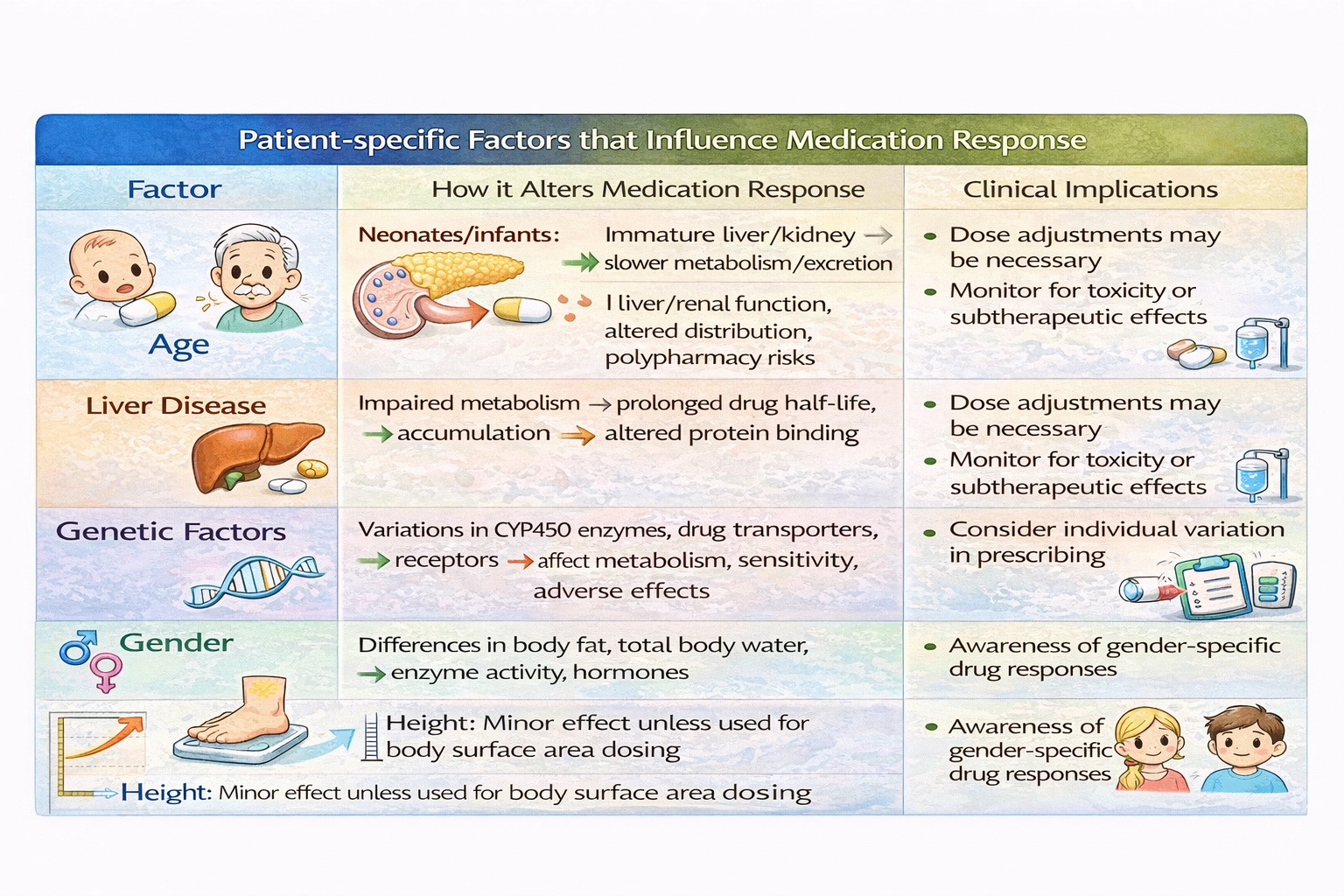
A client with bronchitis is taking trimethoprim/sulfamethoxazole 160/800 mg orally, twice daily. Before administering the third dose, the nurse observes the client has a widespread rash, a temperature and a heart rate of 100 beats/min. The client looks ill and reports not feeling well. What is the nurse's response?
A.
Request an order for intravenous trimethoprim/sulfamethoxazole
B. Initiate probiotics
C. Withhold the treatment and notify the provider of the symptoms
D. Administer the dose and request an order for an antipyretic medication
Rationale
The nurse should withhold the treatment and notify the provider immediately of the client's symptoms, as this clinical presentation raises serious concern for a severe adverse drug reaction to trimethoprim/sulfamethoxazole.
Trimethoprim/sulfamethoxazole, also known as co-trimoxazole, is a combination antibiotic that has been widely used for decades to treat a variety of infections, including respiratory tract infections such as bronchitis, urinary tract infections, and certain opportunistic infections. The medication works through sequential blockade of folate metabolism in bacteria, with sulfamethoxazole inhibiting the incorporation of para-aminobenzoic acid into dihydrofolic acid and trimethoprim inhibiting the reduction of dihydrofolic acid to tetrahydrofolic acid. While effective, this medication is also associated with a significant risk of severe hypersensitivity reactions that can be life-threatening. The client in this scenario has received two doses of the medication and is now exhibiting a constellation of symptoms that should raise immediate concern in any nurse caring for them. The presence of a widespread rash, fever, tachycardia, and general malaise represents a classic presentation of a serious drug reaction that requires urgent intervention. The appropriate nursing response requires recognition of the potential severity of the situation and immediate action to prevent further harm.
A) Request an order for intravenous trimethoprim/sulfamethoxazole
This action would be dangerous and demonstrates a fundamental misunderstanding of the clinical situation. The client is showing signs of a probable adverse reaction to the oral formulation of trimethoprim/sulfamethoxazole. Administering the drug intravenously would deliver it even more rapidly and completely into the systemic circulation, potentially exacerbating the reaction and leading to more severe manifestations. Intravenous administration does not reduce the risk of hypersensitivity reactions and, in fact, may increase the risk of certain types of reactions due to the more rapid achievement of high drug concentrations. The client's symptoms, including widespread rash, fever, tachycardia, and malaise, are not indications for changing the route of administration but rather contraindications to continuing the drug at all. The nurse who requests intravenous administration in this situation is failing to recognize the seriousness of the client's symptoms and could cause significant harm by facilitating continued exposure to the offending agent through a more direct route. This response indicates a critical gap in understanding the difference between situations requiring alternative routes of administration and situations requiring immediate discontinuation of a medication due to adverse effects.
B) Initiate probiotics
While probiotics may have a role in supporting gastrointestinal health during antibiotic therapy by helping to maintain the normal gut flora and potentially reducing the risk of antibiotic-associated diarrhea, they are completely irrelevant to the current clinical situation. The client is exhibiting signs of a systemic hypersensitivity reaction, which is an immune-mediated response that probiotics cannot address or ameliorate in any way. The widespread rash indicates cutaneous involvement, the fever suggests systemic inflammation, the tachycardia may reflect fever, discomfort, or early hemodynamic changes, and the general malaise indicates that the client feels systemically unwell. These symptoms point toward potentially serious conditions such as Stevens-Johnson syndrome, toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms, or other severe hypersensitivity reactions that require immediate discontinuation of the offending drug and prompt medical evaluation. Initiating probiotics does nothing to address this potentially life-threatening situation and delays the appropriate interventions that could prevent progression to more severe outcomes. The nurse who considers probiotics in this context is failing to recognize the urgency of the client's condition and is not prioritizing the appropriate nursing actions.
C) Withhold the treatment and notify the provider of the symptoms
This is the correct and appropriate nursing response that prioritizes client safety and follows the standard of care for suspected severe adverse drug reactions. The client's symptoms are concerning for several potentially serious conditions associated with trimethoprim/sulfamethoxazole use. Stevens-Johnson syndrome and toxic epidermal necrolysis are severe mucocutaneous reactions characterized by widespread blistering and sloughing of the skin and mucous membranes that can be life-threatening and require intensive care management. Drug reaction with eosinophilia and systemic symptoms is another severe hypersensitivity reaction that can involve multiple organ systems including the liver, kidneys, lungs, and heart, and carries significant morbidity and mortality. Even if the reaction does not progress to these extreme manifestations, the combination of rash, fever, and systemic symptoms indicates that the client is having an adverse response to the medication that warrants discontinuation. By withholding the next dose, the nurse prevents further exposure to the suspected causative agent, which is the single most important intervention in managing a drug hypersensitivity reaction. Notifying the provider ensures that the client receives prompt medical evaluation, which may include diagnostic testing to characterize the reaction, assessment of organ involvement through laboratory studies, initiation of appropriate treatment such as antihistamines or corticosteroids if indicated, and selection of an alternative antibiotic to continue treating the bronchitis. This action demonstrates appropriate clinical judgment and prioritization of client safety over completion of the prescribed medication regimen.
D) Administer the dose and request an order for an antipyretic medication
This action would be unsafe and could have serious consequences for the client. Administering another dose of trimethoprim/sulfamethoxazole to a client already showing signs of a severe hypersensitivity reaction could precipitate a more severe and potentially life-threatening reaction. In the case of Stevens-Johnson syndrome or toxic epidermal necrolysis, continued exposure to the offending drug is associated with more extensive skin involvement and worse outcomes. The rash may progress to blistering and sloughing, and systemic involvement may become more severe. While the client does have a fever, and an antipyretic medication might provide symptomatic relief, treating the fever without addressing the underlying cause is inappropriate and dangerous. Antipyretics would temporarily lower the temperature but would do nothing to halt the progression of the hypersensitivity reaction. The priority is to stop the offending agent and evaluate the client, not to mask symptoms while continuing to expose them to the drug causing the reaction. This response demonstrates a dangerous failure to recognize a potentially serious adverse drug reaction and a misunderstanding of the appropriate nursing priorities in this situation. The nurse who administers the dose is prioritizing the medication schedule over obvious clinical signs of harm, which is never appropriate.
Conclusion
When a client taking trimethoprim/sulfamethoxazole develops a widespread rash accompanied by fever, tachycardia, and malaise before the third dose is due, the nurse should withhold the treatment and notify the provider immediately of the symptoms. Requesting intravenous administration would exacerbate the reaction by delivering the drug more rapidly. Initiating probiotics is irrelevant to this acute hypersensitivity reaction. Administering the dose and adding antipyretics is dangerous and could allow the reaction to progress to more severe manifestations such as Stevens-Johnson syndrome or toxic epidermal necrolysis. Therefore, withholding the medication and notifying the provider is the correct response that prioritizes client safety and ensures prompt evaluation and management of what may be a serious adverse drug reaction requiring immediate intervention.

Which of these statements best describes the concept of half-life?
A.
It is the time it takes for half of the medication to be distributed to receptors
B. It is the time it takes for half of the medicinal effect to be achieved
C. It is the time it takes for half of the medication to be metabolized for elimination
D. The term refers to the shelf life of the drug
Rationale
Half-life is correctly defined as the time it takes for the plasma concentration of a medication to decrease by half during the elimination phase, primarily through metabolism and excretion, which is the time it takes for half of the medication to be metabolized for elimination.
The concept of half-life is fundamental to understanding pharmacokinetics, which is the study of how the body handles drugs over time. Half-life, often denoted as t½, is a mathematical concept that describes the rate at which a drug is removed from the body. More specifically, it is the time required for the plasma concentration of a drug to decrease by 50% during the elimination phase, after absorption and distribution are complete. This parameter is determined by two primary factors: the volume of distribution, which reflects how extensively the drug distributes into tissues, and clearance, which reflects the efficiency of drug elimination through metabolism and excretion. The half-life has profound clinical implications for drug therapy. It determines how long a drug remains in the body after a single dose, which affects the duration of action. It determines the time required to reach steady-state with repeated dosing, which is approximately four to five half-lives. It guides the selection of appropriate dosing intervals to maintain therapeutic drug levels without excessive fluctuation. And it predicts how long it will take for a drug to be eliminated after discontinuation, which is important when managing toxicity or switching medications.
A) It is the time it takes for half of the medication to be distributed to receptors
Distribution to receptors is not measured by half-life. Drug distribution is the process by which a drug moves from the bloodstream into tissues, including to the site of action where receptors are located. Distribution occurs during the initial phase after drug administration, often while the drug concentration is still declining due to both distribution and early elimination. The rate and extent of distribution are influenced by factors such as blood flow to tissues, capillary permeability, protein binding, and lipid solubility of the drug. Half-life specifically refers to the elimination phase, not distribution. The time to reach receptors is related to the onset of action, which depends on absorption and distribution kinetics, not half-life.
B) It is the time it takes for half of the medicinal effect to be achieved
The time to achieve half of the medicinal effect is not a standard pharmacokinetic parameter and is not what half-life measures. Drug effect is related to concentration at receptor sites, which depends on multiple factors including absorption, distribution, and the relationship between concentration and response, known as pharmacodynamics. The time to reach peak effect varies by drug and route of administration and is influenced by factors such as rate of absorption and distribution to the site of action. Half-life does not measure the onset or achievement of effect; it measures elimination.
C) It is the time it takes for half of the medication to be metabolized for elimination
This statement correctly describes half-life. The elimination half-life represents the time required for the body to reduce the drug concentration by 50% through the combined processes of metabolism and excretion. For most drugs, elimination follows first-order kinetics, meaning that a constant fraction of the drug is eliminated per unit time, and the half-life remains constant regardless of concentration. This parameter is clinically useful for determining dosing intervals, predicting drug accumulation with repeated dosing, and estimating the time to reach steady-state. For example, if a drug has a half-life of 8 hours, approximately 50% of the drug is eliminated in 8 hours, 75% in 16 hours, 87.5% in 24 hours, and so on. After four to five half-lives, the drug is considered effectively eliminated from the body.
D) The term refers to the shelf life of the drug
This statement reflects confusion between pharmacokinetic terminology and pharmaceutical storage terminology. Shelf life is the length of time a drug product remains stable and effective when stored under proper conditions. It is determined by stability studies that assess how the drug degrades over time under various temperature, humidity, and light conditions. Shelf life is a pharmaceutical concept related to drug product quality, not a pharmacokinetic concept related to drug behavior in the body. Half-life has nothing to do with shelf life, and the two terms should never be confused.
Conclusion
Half-life is correctly defined as the time it takes for half of the medication to be metabolized for elimination, representing the time required for plasma concentration to decrease by 50% through metabolism and excretion. It does not refer to distribution to receptors, achievement of medicinal effect, or shelf life of the drug. Therefore, the correct description involves metabolism and elimination, which is the standard pharmacokinetic definition of half-life.
A client with type 1 diabetes who takes insulin reports taking propranolol for hypertension. Why is the nurse concerned?
A.
Propranolol increases insulin requirements because of receptor blocking
B. Using the two agents together increases the risk of ketoacidosis
C. The beta-blocker can mask the symptoms of hypoglycemia
D. The beta-blocker can cause insulin resistance
Rationale
The nurse is concerned because propranolol, a non-selective beta-blocker, can mask the adrenergic symptoms of hypoglycemia, preventing the client from recognizing early warning signs of low blood glucose and increasing the risk of severe hypoglycemic events.
Propranolol is a non-selective beta-adrenergic blocking agent used for hypertension, angina, migraine prophylaxis, and other conditions. It works by blocking the effects of catecholamines at both beta-1 and beta-2 receptors. Beta-1 blockade reduces heart rate and cardiac output, while beta-2 blockade affects bronchial smooth muscle and various metabolic processes. In the context of diabetes, the most significant concern with beta-blockers, particularly non-selective ones like propranolol, is their effect on the recognition of hypoglycemia. Normal hypoglycemia triggers a counterregulatory response that includes release of epinephrine, which produces characteristic adrenergic symptoms such as tachycardia, palpitations, tremors, and anxiety. These symptoms serve as warning signs that alert the patient to low blood glucose so they can take corrective action by consuming carbohydrates.
A) Propranolol increases insulin requirements because of receptor blocking
This statement is not accurate. Beta-blockers do not directly increase insulin requirements. They may have minor effects on glucose metabolism, but they do not significantly alter the amount of insulin needed for glycemic control. This is not the primary concern when combining propranolol with insulin therapy.
B) Using the two agents together increases the risk of ketoacidosis
. Beta-blockers do not increase the risk of diabetic ketoacidosis. Ketoacidosis results from insulin deficiency leading to uncontrolled lipolysis and ketone production, which is not related to beta-blocker use. This is not a valid concern.
C) The beta-blocker can mask the symptoms of hypoglycemia
This is the correct concern. By blocking beta-adrenergic receptors, propranolol prevents the epinephrine-mediated symptoms that normally warn of hypoglycemia. The patient may not experience tachycardia, palpitations, or tremors as blood glucose falls, and may only become aware of hypoglycemia when neuroglycopenic symptoms develop, such as confusion, difficulty concentrating, slurred speech, or loss of consciousness. This increases the risk of severe hypoglycemia requiring assistance from others. Clients with diabetes taking beta-blockers must be aware of this effect and rely more on blood glucose monitoring rather than symptoms to detect hypoglycemia. They should also be counseled to monitor more frequently and to be alert for other subtle signs that might indicate low blood glucose.
D) The beta-blocker can cause insulin resistance
While some beta-blockers may slightly decrease insulin sensitivity, this is not the primary concern and is not a major effect of propranolol. The most significant and dangerous interaction is masking of hypoglycemia symptoms. Some beta-blockers, particularly those with beta-1 selectivity, may have less effect on hypoglycemia awareness, but non-selective agents like propranolol pose the greatest risk.
Conclusion
The nurse is concerned because propranolol, a non-selective beta-blocker, can mask the adrenergic symptoms of hypoglycemia in a client with type 1 diabetes, increasing the risk of severe hypoglycemia without warning. The other statements about increased insulin requirements, ketoacidosis risk, and insulin resistance are not accurate or are less significant concerns. Therefore, the correct understanding is that beta-blockers mask hypoglycemia symptoms, and the client must be educated about this risk and the importance of frequent blood glucose monitoring.

Insulin lispro was given to a client at 0700 by a night nurse who needed to leave early. At 0730 the client is clammy and refuses breakfast, stating, I don't feel well. I need to lie down. What is the nurse's action?
A.
Document the refusal and let the client sleep since the insulin lispro will not peak until later in the morning
B. Wait to offer breakfast until the client feels better
C. Check the blood sugar and convince the client to drink juice if possible
D. Call the night nurse at home and tell her to come back and deal with the situation
Rationale
The nurse should check the blood sugar and convince the client to drink juice if possible, as the symptoms of being clammy and not feeling well after receiving insulin lispro at 0700 are classic signs of hypoglycemia requiring immediate intervention.
Insulin lispro is a rapid-acting insulin analog with an onset of approximately 15 minutes, a peak effect at 30 to 90 minutes, and a duration of 3 to 5 hours. It is designed to be taken just before meals to cover the rise in blood glucose from food absorption. When administered at 0700, its peak effect occurs around 0730 to 0830, exactly when the client is symptomatic. The symptoms of being clammy, which likely refers to diaphoresis, and not feeling well are classic adrenergic signs of hypoglycemia, occurring as the body's counterregulatory response releases epinephrine. Refusing breakfast compounds the problem because the client needs carbohydrates to prevent or treat hypoglycemia. This is an emergency situation requiring prompt intervention to prevent progression to more severe hypoglycemia with confusion, loss of consciousness, or seizures.
A) Document the refusal and let the client sleep since the insulin lispro will not peak until later in the morning
This action is dangerous and demonstrates misunderstanding of insulin lispro's time course. Lispro peaks early, at 30 to 90 minutes, not later. Letting the client sleep without intervention could result in severe hypoglycemia and potential brain damage. The nurse who documents and walks away is abandoning the client and failing to recognize an emergency.
B) Wait to offer breakfast until the client feels better
Waiting is inappropriate because the client's symptoms are likely due to hypoglycemia, which will worsen without treatment. The client needs carbohydrates immediately, not later. Delaying intervention could allow blood glucose to fall further, leading to more severe symptoms.
C) Check the blood sugar and convince the client to drink juice if possible
This is the correct action. Rapid blood glucose testing will confirm hypoglycemia. If the blood glucose is low, typically below 70 mg/dL, the nurse should administer fast-acting carbohydrates such as juice, regular soda, glucose gel, or glucose tablets. The nurse should stay with the client, monitor response, and recheck blood glucose after 15 minutes. If the client is unable or unwilling to drink, or if symptoms are severe, the nurse should be prepared to administer glucagon or call for emergency assistance. This action addresses the emergency directly.
D) Call the night nurse at home and tell her to come back and deal with the situation
This action is inappropriate and unprofessional. The day nurse is now responsible for the client and must address the emergency immediately. Calling the night nurse wastes precious time and does nothing to help the client. The night nurse may not be available, may not answer, and even if they did, they could not intervene remotely. This response abdicates responsibility and delays treatment.
Conclusion
The nurse should check blood sugar and give juice to the client who received insulin lispro at 0700 and is now clammy and refusing breakfast, as these are signs of hypoglycemia from the peaking insulin. Documenting and letting sleep, waiting, or calling the night nurse are all inappropriate and delay treatment. Therefore, checking blood sugar and giving juice is correct, ensuring prompt recognition and management of hypoglycemia.
A client with type 1 diabetes is eating breakfast at 7:30 am. Blood sugars are on a sliding scale and are ordered before a meal and at bedtime. The client's blood sugar level is 317 mg/dL. Which insulin should the nurse prepare to administer?
A.
Insulin aspart protamine suspension 70%, insulin aspart 30%
B. No insulin should be administered
C. Insulin lispro
D. NPH
Rationale
The nurse should prepare to administer insulin lispro for a blood sugar of 317 mg/dL before breakfast, as this rapid-acting insulin is specifically designed for mealtime coverage and sliding scale correction of hyperglycemia due to its pharmacokinetic profile that matches the postprandial glucose rise.
Sliding scale insulin regimens are commonly used in hospitalized patients to manage blood glucose levels by providing rapid-acting insulin doses based on the current blood glucose reading before meals and at bedtime. The rationale behind this approach is to correct hyperglycemia when it occurs and to provide coverage for the carbohydrate load that will be consumed with the upcoming meal. The selection of the appropriate insulin type is critical because different insulins have different onsets, peaks, and durations of action, and using the wrong type can lead to inadequate glucose control or dangerous hypoglycemia. Insulin lispro is a rapid-acting insulin analog that was developed by reversing the amino acid sequence at positions 28 and 29 of the insulin B-chain, changing from proline-lysine to lysine-proline. This structural modification reduces the tendency of insulin molecules to self-associate, resulting in faster absorption from the subcutaneous tissue. Lispro has an onset of action of approximately 15 minutes, a peak effect at 30 to 90 minutes, and a duration of 3 to 5 hours. These characteristics make it ideal for mealtime use because its peak coincides with the postprandial rise in blood glucose that occurs after eating. For a blood glucose of 317 mg/dL, which represents significant hyperglycemia, rapid-acting insulin will work quickly to lower the glucose level while also covering the additional glucose from the meal.
A) Insulin aspart protamine suspension 70%, insulin aspart 30%
This preparation is a mixed insulin containing both intermediate-acting and rapid-acting components, similar to the older 70/30 NPH/regular mixtures but with aspart instead. The 70% component is insulin aspart protamine suspension, which has an intermediate duration of action, while the 30% component is regular insulin aspart, which is rapid-acting. While this mixture does contain some rapid-acting insulin, it is not typically used for sliding scale corrections for several important reasons. The fixed ratio of 70:30 means that the dose cannot be adjusted independently for basal and prandial needs. If the patient requires a larger dose for hyperglycemia correction, they will also receive a larger dose of intermediate-acting insulin, which could cause late hypoglycemia hours after the meal. Additionally, the intermediate component is not necessary for pre-meal correction and could complicate the overall insulin regimen. Sliding scale orders are typically written for rapid-acting insulin alone, allowing for flexible dosing based on blood glucose without affecting basal coverage.
B) No insulin should be administered
Withholding insulin for a blood glucose of 317 mg/dL in a patient with type 1 diabetes would be inappropriate and potentially dangerous. Type 1 diabetes is characterized by absolute insulin deficiency due to autoimmune destruction of pancreatic beta cells. These patients require exogenous insulin for survival and to prevent diabetic ketoacidosis. A blood glucose of 317 mg/dL indicates significant hyperglycemia that, if left untreated, could worsen and lead to ketone production and potentially DKA. The sliding scale orders are specifically designed to address such elevations by providing additional rapid-acting insulin to correct the hyperglycemia. The nurse who withholds insulin in this situation would be failing to follow the prescribed orders and would be putting the patient at risk for complications of uncontrolled hyperglycemia. The correct action is to administer the dose of rapid-acting insulin specified by the sliding scale for a blood glucose of 317 mg/dL.
C) Insulin lispro
Insulin lispro is the correct choice for this situation. As a rapid-acting insulin, it is specifically intended for pre-meal use and for correction of hyperglycemia. When administered before breakfast, its onset of approximately 15 minutes means it will begin working as food is being absorbed, its peak at 30 to 90 minutes will coincide with the postprandial glucose rise, and its duration of 3 to 5 hours will cover the meal without extending into the late post-meal period where it could cause hypoglycemia. The sliding scale orders will specify the exact dose to administer based on the blood glucose level, typically with higher blood glucose levels receiving larger doses. For a value of 317 mg/dL, the dose might be in the range of 6 to 10 units depending on the specific scale and the patient's individual sensitivity. The nurse should verify the ordered dose, draw up the insulin accurately, and administer it subcutaneously, ensuring that the patient eats breakfast soon after to prevent hypoglycemia.
D) NPH
NPH insulin is an intermediate-acting insulin that is not appropriate for sliding scale correction of pre-meal hyperglycemia. NPH has an onset of 1 to 2 hours, a peak at 4 to 12 hours, and a duration of 14 to 18 hours. It is designed to provide basal coverage or, when used in split-dose regimens, to cover daytime insulin needs. Administering NPH for a blood glucose of 317 mg/dL before breakfast would not provide the rapid correction needed for the current hyperglycemia, as its slow onset would not begin working for hours. Additionally, its prolonged duration could cause hypoglycemia later in the day, particularly if the patient does not eat regularly. NPH also has a pronounced peak that can increase hypoglycemia risk. The nurse who administered NPH instead of rapid-acting insulin would be using the wrong tool for the job, potentially leaving the patient hyperglycemic for hours while creating risk for later hypoglycemia.
Conclusion
For a pre-meal blood glucose of 317 mg/dL in a patient with type 1 diabetes on a sliding scale, the nurse should prepare to administer insulin lispro, a rapid-acting insulin that will provide timely correction of hyperglycemia and coverage for the meal. The mixed insulin product contains an inappropriate intermediate component and fixed ratio. Withholding insulin is dangerous and could lead to DKA. NPH is an intermediate-acting insulin not suitable for acute correction. Therefore, insulin lispro is correct, reflecting appropriate understanding of the role of rapid-acting insulin in sliding scale regimens.
Which of these comments by a client taking a calcium channel blocker would indicate the need for additional teaching?
A.
I will elevate my legs if edema occurs
B. I can limit my risk for constipation by increasing fluid and fiber
C. I will take the medication with grapefruit juice
D. I will rise slowly from lying to sitting, to standing
Rationale
The comment that the client will take the medication with grapefruit juice indicates need for additional teaching, as grapefruit juice inhibits intestinal CYP3A4 enzymes, leading to significantly increased drug levels and risk of toxicity with many calcium channel blockers.
Calcium channel blockers are a class of medications widely used for hypertension, angina, and certain arrhythmias. They work by blocking voltage-gated calcium channels in vascular smooth muscle and cardiac muscle cells, leading to vasodilation, reduced peripheral vascular resistance, decreased myocardial contractility, and slowed cardiac conduction. Different calcium channel blockers have varying degrees of selectivity for vascular versus cardiac effects, but all share the common mechanism of reducing calcium influx through L-type calcium channels. Many calcium channel blockers, including felodipine, nifedipine, and others, are metabolized by the cytochrome P450 enzyme system, specifically the CYP3A4 isoenzyme, in both the intestinal wall and the liver. Grapefruit juice contains compounds called furanocoumarins, which irreversibly inhibit CYP3A4 in the intestinal wall. This inhibition is not just a temporary effect; it can last for up to 24 hours or more after grapefruit juice consumption. When intestinal CYP3A4 is inhibited, much more of the calcium channel blocker escapes metabolism during absorption and enters the systemic circulation, leading to drug levels that can be two to three times higher than normal. This can result in profound hypotension, bradycardia, dizziness, and other signs of toxicity.
A) I will elevate my legs if edema occurs
This comment shows appropriate understanding of how to manage a common side effect of calcium channel blockers. Peripheral edema, particularly of the ankles and lower legs, is a frequent adverse effect of these medications, especially with dihydropyridine calcium channel blockers like amlodipine and nifedipine. The edema occurs not because of fluid overload but because of vasodilation and increased capillary hydrostatic pressure, which causes fluid to shift from the vascular space into the interstitial tissues. Leg elevation helps mobilize this fluid by using gravity to promote venous and lymphatic return, reducing the dependent edema. This is an appropriate self-care measure that demonstrates understanding of the mechanism and management of this side effect.
B) I can limit my risk for constipation by increasing fluid and fiber
This comment shows appropriate understanding of how to manage another common side effect of some calcium channel blockers. Constipation is particularly associated with verapamil, which affects smooth muscle in the gastrointestinal tract in addition to its cardiovascular effects. Verapamil can slow intestinal motility, leading to constipation that can be significant and bothersome. Increasing fluid intake and dietary fiber are appropriate measures to promote regular bowel movements and prevent constipation. The client who understands this demonstrates knowledge of self-care for medication side effects.
C) I will take the medication with grapefruit juice
This comment indicates need for additional teaching about a potentially dangerous drug interaction. As explained, grapefruit juice inhibits intestinal CYP3A4, leading to increased absorption and higher blood levels of many calcium channel blockers. This can result in toxicity, including severe hypotension, dizziness, syncope, and bradycardia. The effect of grapefruit juice can last for more than 24 hours, so even if the medication is taken at a different time of day, there can still be interaction if grapefruit juice is consumed regularly. The client who plans to take their calcium channel blocker with grapefruit juice is at significant risk for adverse effects and needs immediate education about this interaction. They should be advised to avoid grapefruit and grapefruit juice entirely while taking these medications, and to check with their provider or pharmacist about any other citrus juices that might interact.
D) I will rise slowly from lying to sitting, to standing
This comment shows appropriate understanding of how to prevent orthostatic hypotension, another potential side effect of calcium channel blockers. These medications cause vasodilation, which can impair the body's normal compensatory responses to position changes. When a person stands up quickly, blood pools in the lower extremities due to gravity, and the body normally responds with vasoconstriction to maintain blood pressure. Calcium channel blockers interfere with this vasoconstriction, leading to a drop in blood pressure upon standing, which can cause dizziness, lightheadedness, and falls. Rising slowly allows the body time to adjust and reduces this risk. The client who understands this demonstrates appropriate knowledge of fall prevention while on this medication.
Conclusion
The client needs additional teaching when stating they will take calcium channel blockers with grapefruit juice due to the dangerous drug interaction that increases drug levels and toxicity risk. Leg elevation for edema, increasing fluid and fiber for constipation, and rising slowly to prevent orthostatic hypotension all demonstrate understanding. Therefore, grapefruit juice comment requires correction, and the nurse must explain the importance of avoiding grapefruit products entirely.
A nurse is teaching a client who has asthma the appropriate use of inhaled fluticasone. What advice should the nurse give to help the client avoid complications with the use of inhaled steroids?
A.
Limit your caffeine intake
B. Check the pulse after the medication
C. Rinse your mouth after inhaling the medicine
D. Take the medication before eating
Rationale
The nurse should advise the client to rinse their mouth after inhaling fluticasone to prevent oropharyngeal candidiasis, a common local side effect of inhaled corticosteroids caused by drug deposition in the mouth and throat.
Fluticasone is an inhaled corticosteroid used as a controller medication for asthma. Inhaled steroids work by reducing airway inflammation, decreasing bronchial hyperresponsiveness, and preventing asthma symptoms and exacerbations. They are highly effective and, when used at recommended doses, have minimal systemic absorption. However, they do have local side effects related to deposition of the medication in the oropharynx. When the patient inhales the medication, a portion of the dose can deposit on the mucous membranes of the mouth, throat, and vocal cords rather than reaching the lower airways. This deposited steroid suppresses local immunity in these areas, creating an environment where Candida albicans, a fungus normally present in small amounts, can overgrow and cause infection. This condition, oropharyngeal candidiasis or thrush, presents as white, plaque-like lesions on the buccal mucosa, tongue, and palate that can be painful and interfere with eating and swallowing. Rinsing the mouth with water after each use and spitting the water out removes residual drug from the oropharynx, significantly reducing the risk of thrush.
A) Limit your caffeine intake
Caffeine has no relation to inhaled steroid use or its complications. This advice is not relevant and would not help prevent any complications associated with fluticasone.
B) Check the pulse after the medication
Inhaled steroids do not typically affect pulse rate. This advice is more appropriate for bronchodilators such as albuterol, which can cause tachycardia. Checking pulse is not necessary for fluticasone.
C) Rinse your mouth after inhaling the medicine
This is correct and essential advice. The nurse should instruct the client to rinse their mouth thoroughly with water after each use of inhaled fluticasone and to spit the water out, not swallow it. This removes drug deposited in the mouth and throat, preventing local immunosuppression and fungal overgrowth. The client should also be advised to brush their teeth regularly and to report any signs of thrush, such as white patches or soreness in the mouth.
D) Take the medication before eating
Timing relative to meals is not critical for fluticasone. Some patients may find it convenient to take it at the same time each day, but there is no specific requirement to take it before eating. Rinsing after use is more important than timing around meals.
Conclusion
To avoid complications with inhaled fluticasone, the nurse should advise the client to rinse the mouth after each use to prevent oral thrush. Caffeine restriction, pulse checking, and timing before meals are not relevant. Therefore, mouth rinsing is correct, a simple but crucial step for preventing this common local side effect.
Male client tells the nurse he awakens once or twice each night to void and has difficulty starting his stream of urine. He describes these symptoms as \annoying.\" The client provider examines him and notes that the prostate is moderately enlarged. The client is sexually active and tells the nurse that he doesn't want to take any medication that will interfere with sexual function. The nurse anticipates the provider will order which of the following?"""
A.
Silodosin
B. A transurethral prostatectomy
C. Finasteride
D. Doxazosin
Rationale
The nurse anticipates that the provider will order doxazosin for this client with symptomatic benign prostatic hyperplasia who wishes to preserve his sexual function.
Benign prostatic hyperplasia is a common condition affecting aging men in which the prostate gland enlarges due to non-malignant proliferation of stromal and glandular elements. This enlargement occurs primarily in the transition zone of the prostate, which surrounds the urethra, leading to compression of the urethral lumen and obstruction of urinary flow. The clinical consequences of this obstruction are referred to as lower urinary tract symptoms and include both storage symptoms such as nocturia, frequency, and urgency, and voiding symptoms such as hesitancy, weak stream, straining, and sensation of incomplete emptying. The client in this scenario describes classic symptoms of BPH with nocturia, indicating he awakens once or twice at night to void, and hesitancy, meaning he has difficulty initiating his urinary stream. The provider's examination confirming moderate prostatic enlargement supports this diagnosis. The management of BPH involves a stepped approach beginning with lifestyle modifications and progressing to pharmacologic therapy and, when necessary, surgical intervention. The client's explicit statement that he does not want any medication that will interfere with his sexual function is a critical piece of information that guides the selection of appropriate pharmacotherapy, as different classes of medications used for BPH have markedly different profiles regarding sexual side effects.
A) Silodosin
Silodosin represents a highly selective alpha-1a adrenergic antagonist that was developed specifically for the treatment of BPH. The rationale behind its high selectivity for the alpha-1a receptor subtype, which is the predominant alpha receptor subtype found in the prostate, bladder neck, and urethra, was to achieve effective relaxation of smooth muscle in these areas while minimizing effects on alpha-1b receptors found in blood vessels, thereby reducing the risk of hypotension. While silodosin is indeed effective at improving urinary flow rates and reducing BPH symptoms, it has a significant and well-documented drawback regarding sexual function. Clinical studies have demonstrated that silodosin is associated with a high incidence of ejaculatory dysfunction, specifically retrograde ejaculation or anejaculation, occurring in approximately 28% of patients taking the medication. This side effect occurs because the alpha-1a receptors are also involved in the coordination of seminal emission and bladder neck closure during ejaculation. When these receptors are blocked, the bladder neck fails to close properly, allowing semen to flow backward into the bladder rather than forward through the urethra. While this condition is not harmful and does not affect the sensation of orgasm, it can be distressing for men who are sexually active and concerned about fertility or the subjective experience of ejaculation. The client explicitly stated that he does not want medication that will interfere with sexual function, and silodosin's high rate of ejaculatory dysfunction makes it a poor choice for this particular patient despite its efficacy for symptom relief.
B) A transurethral prostatectomy
Transurethral prostatectomy, commonly abbreviated as TURP, represents a surgical intervention rather than a medication and is typically reserved for specific clinical situations rather than as first-line therapy for mild to moderate symptoms. TURP involves the insertion of a resectoscope through the urethra to remove excess prostate tissue that is compressing the urethral lumen, thereby physically relieving the obstruction. This procedure is generally indicated for patients with moderate to severe lower urinary tract symptoms that have not responded adequately to medical therapy, patients who develop complications from BPH such as acute urinary retention, recurrent urinary tract infections, bladder stones, or renal insufficiency, or patients who simply prefer surgical management after discussing all options. The client in this scenario describes his symptoms as "annoying," which suggests they are mild to moderate in severity and not complicated by the more serious sequelae that would necessitate surgical intervention. He has not yet tried medical therapy, and there is no indication that he has failed any medication trials. Furthermore, TURP carries its own risks regarding sexual function, with retrograde ejaculation occurring in up to 75% of patients undergoing the procedure and possible erectile dysfunction in a smaller percentage. Given the client's explicit preference to avoid interference with sexual function and the early stage of his symptom management, surgical intervention would be premature and inappropriate at this time. The nurse would not anticipate the provider ordering TURP for this clinical presentation.
C) Finasteride
Finasteride belongs to a class of medications known as 5-alpha-reductase inhibitors, which work through an entirely different mechanism than alpha-blockers for the treatment of BPH. The enzyme 5-alpha-reductase is responsible for converting testosterone to dihydrotestosterone within the prostate gland. Dihydrotestosterone is the primary androgen responsible for stimulating prostate growth, and by inhibiting its production, finasteride can actually reduce the size of the prostate over time, typically achieving a 20% to 30% reduction in prostate volume after six to twelve months of therapy. This mechanism makes finasteride particularly effective in men with significantly enlarged prostates, generally defined as those with prostate volumes greater than 40 milliliters. However, finasteride has well-documented sexual side effects that occur in a significant percentage of men taking the medication. Clinical trials have reported decreased libido in approximately 3% to 8% of men, erectile dysfunction in 4% to 8%, and decreased ejaculate volume in 3% to 8%. These effects can persist even after discontinuing the medication in some cases, a phenomenon that has been termed post-finasteride syndrome. The client explicitly stated that he does not want medication that will interfere with sexual function, making finasteride an inappropriate choice for this particular patient despite its effectiveness in reducing prostate size and improving symptoms over the long term. The nurse would not anticipate the provider ordering finasteride given this important patient preference.
D) Doxazosin
Doxazosin represents an appropriate and rational choice for this client based on his symptom profile, prostate examination findings, and explicit preference regarding sexual function. Doxazosin is an alpha-1 adrenergic antagonist that works by blocking the effects of norepinephrine at alpha-1 receptors located on smooth muscle cells throughout the body, including those in the prostate, bladder neck, and urethra. In the context of BPH, these receptors are abundant in the stromal smooth muscle of the prostate and the smooth muscle of the bladder neck. When stimulated by norepinephrine, these receptors cause smooth muscle contraction, which contributes to the dynamic component of bladder outlet obstruction. By blocking these receptors, doxazosin causes relaxation of the smooth muscle in these areas, reducing urethral resistance and improving urinary flow. The therapeutic effects of alpha-blockers are typically noticeable within days to weeks of starting therapy, providing relatively rapid symptom relief. Unlike finasteride, alpha-blockers do not affect prostate size but rather address the dynamic component of obstruction caused by smooth muscle tone. Regarding sexual function, doxazosin has a favorable profile compared to other BPH treatments. It does not typically cause the erectile dysfunction, decreased libido, or ejaculatory problems associated with 5-alpha-reductase inhibitors or the high rate of ejaculatory dysfunction seen with silodosin. While doxazosin can cause other side effects such as dizziness and orthostatic hypotension due to its blood pressure-lowering effects, these are manageable with proper dosing, typically starting with a low dose at bedtime and gradually titrating upward to minimize symptoms. The client's desire to maintain sexual function makes doxazosin a suitable option among available BPH treatments, and the nurse would anticipate the provider ordering this medication.
Conclusion
The nurse anticipates that the provider will order doxazosin for this client with symptomatic benign prostatic hyperplasia who wishes to preserve sexual function. Silodosin, while effective for symptom relief, carries a high incidence of ejaculatory dysfunction that would conflict with the client's stated preference. Transurethral prostatectomy is a surgical intervention not indicated for mild, annoying symptoms that have not yet been treated with medication. Finasteride carries significant risk of sexual side effects including decreased libido and erectile dysfunction that would also conflict with the client's preference. Therefore, doxazosin represents the most appropriate choice given the client's symptom profile of nocturia and hesitancy with moderate prostatic enlargement, combined with his explicit desire to avoid any medication that would interfere with his sexual function.

A client who just took his first dose of glipizide, is now experiencing tremors, pallor, and agitation. How should the nurse respond?
A.
Ask the client's family to come to sit with him until the client's panic attack subsides
B. Give diphenhydramine per standing order for this allergic reaction
C. Acknowledge how hard a diagnosis of diabetes can be and offer to listen
D. Check the blood glucose and give carbohydrates if the client is hypoglycemic
Rationale
The nurse should check the blood glucose and give carbohydrates if the client is hypoglycemic, as the symptoms of tremors, pallor, and agitation after a first dose of glipizide are classic signs of hypoglycemia requiring immediate intervention.
Glipizide is an oral hypoglycemic agent belonging to the class of medications known as sulfonylureas, which have been used for decades in the management of type 2 diabetes mellitus. Sulfonylureas work by binding to specific receptors on the surface of pancreatic beta cells, which closes ATP-sensitive potassium channels and leads to cell membrane depolarization. This depolarization opens voltage-gated calcium channels, allowing calcium influx into the cell, which triggers the exocytosis of insulin-containing granules and increases insulin secretion. This mechanism is glucose-independent, meaning that sulfonylureas stimulate insulin release even when blood glucose levels are normal or low, which creates a significant risk of hypoglycemia. The first dose of a sulfonylurea is particularly concerning because the patient's response is unpredictable, and if the medication produces a robust insulin release, blood glucose can drop rapidly. The symptoms described by the client are the classic adrenergic manifestations of hypoglycemia, which occur as the body's counterregulatory system responds to falling blood glucose levels.
A) Ask the client's family to come to sit with him until the client's panic attack subsides
This response is inappropriate and demonstrates a failure to recognize the signs of a potentially serious medication adverse effect. While the symptoms of hypoglycemia, including tremors, pallor, and agitation, can resemble those of an anxiety or panic attack, assuming it is a psychological event without checking blood glucose could delay life-saving treatment. The client has just taken a medication known to cause hypoglycemia, making this the most likely cause of his symptoms. The nurse who attributes these symptoms to a panic attack is not thinking critically and is not considering the context of recent medication administration. This response could result in the client's condition deteriorating while the nurse waits for family members to arrive, potentially leading to loss of consciousness, seizures, or permanent neurological damage from severe hypoglycemia.
B) Give diphenhydramine per standing order for this allergic reaction
This response misinterprets the symptoms as an allergic reaction, which is incorrect and could have harmful consequences. While allergic reactions can occur with any medication, the symptoms described are not typical of an allergic response. Allergic reactions more commonly present with rash, urticaria, pruritus, angioedema, or respiratory symptoms such as wheezing or dyspnea. Tremors, pallor, and agitation are not signs of an allergic reaction but are classic for hypoglycemia. Diphenhydramine is an antihistamine that would not correct hypoglycemia and would actually worsen the situation by causing sedation, potentially masking neurologic changes and making assessment more difficult. The nurse who administers diphenhydramine is treating the wrong condition and delaying appropriate intervention for the actual problem.
C) Acknowledge how hard a diagnosis of diabetes can be and offer to listen
This response addresses emotional support but completely misses the acute physiologic problem that requires immediate intervention. While emotional support is certainly important for clients adjusting to a new diabetes diagnosis, and a new diagnosis can be overwhelming and anxiety-provoking, the client is experiencing acute physical symptoms that suggest a potentially serious medication adverse effect. Offering to listen and providing emotional support does nothing to address hypoglycemia and delays necessary intervention. The nurse must prioritize physical assessment and treatment over psychosocial support when there are signs of a possible medical emergency. After addressing the acute situation, there will be time to provide emotional support and education about living with diabetes.
D) Check the blood glucose and give carbohydrates if the client is hypoglycemic
This is the correct and appropriate response that demonstrates recognition of the likely problem and prompt intervention. The symptoms of tremors, pallor, and agitation after a first dose of glipizide strongly suggest hypoglycemia. The nurse should immediately check the client's blood glucose using a glucose meter to confirm the diagnosis. If the blood glucose is low, typically below 70 mg/dL, the nurse should administer fast-acting carbohydrates such as oral glucose gel, fruit juice, regular soda, or glucose tablets if the client is conscious and able to swallow safely. This intervention rapidly corrects hypoglycemia and should lead to resolution of symptoms within minutes. The nurse should stay with the client, monitor for improvement, and be prepared to administer glucagon or call for emergency assistance if the client's condition worsens or they lose consciousness. After the acute episode is managed, the nurse should document the event, notify the provider, and discuss possible adjustment of the medication regimen to prevent recurrence.
Conclusion
When a client who just took glipizide develops tremors, pallor, and agitation, the nurse should check blood glucose and give carbohydrates if hypoglycemic, as these symptoms are classic for sulfonylurea-induced hypoglycemia. Assuming a panic attack, treating for allergy, or offering emotional support without addressing the physiologic cause are all inappropriate responses that could result in patient harm from delayed treatment of hypoglycemia. Therefore, checking blood glucose and treating hypoglycemia is the correct action that prioritizes the client's immediate safety.

A client who is recovering from total knee surgery is preparing for discharge. Which of these statements indicates the client needs further teaching?
A.
I can rotate acetaminophen with ibuprofen if needed for pain control, so I don't take too much of either one
B. Taking more than 4000 mg of acetaminophen in a day can cause liver problems
C. Taking acetaminophen often could mask any infection-related fevers I might have
D. If I still have pain 10 minutes after taking 1000 mg of acetaminophen, I should take two of oxycodone-acetaminophen
Rationale
The statement indicating need for further teaching is that the client would take two oxycodone-acetaminophen tablets 10 minutes after taking plain acetaminophen, as this demonstrates dangerous misunderstanding of acetaminophen dosing, combination products, and appropriate pain management principles.
Postoperative pain management after total knee surgery requires a multimodal approach that balances effective pain control with safety considerations. Acetaminophen and opioid-acetaminophen combination products are commonly used, but they require careful education to prevent unintentional overdose and other complications. Acetaminophen is present in many over-the-counter and prescription products, and the maximum daily dose of 3000 to 4000 mg must not be exceeded to prevent hepatotoxicity. Patients must understand the acetaminophen content of all medications they take and must allow adequate time for medications to work before taking additional doses. The statement about taking two oxycodone-acetaminophen tablets 10 minutes after plain acetaminophen reveals multiple gaps in understanding that require correction.
A) I can rotate acetaminophen with ibuprofen if needed for pain control, so I don't take too much of either one
This statement shows understanding. Rotating different classes of analgesics is an appropriate pain management strategy that can provide better pain control while minimizing the total dose of each medication. Acetaminophen and ibuprofen have different mechanisms of action and can be alternated safely as long as each is taken within its recommended dosing parameters. This demonstrates appropriate knowledge of multimodal pain management.
B) Taking more than 4000 mg of acetaminophen in a day can cause liver problems
This statement shows understanding. The maximum recommended daily dose of acetaminophen for most adults is 4000 mg, though many sources recommend a lower limit of 3000 mg for safety, particularly in patients with risk factors. Exceeding this limit can cause hepatotoxicity, which can be severe and even fatal. The client correctly identifies this risk, demonstrating awareness of the importance of dose limits.
C) Taking acetaminophen often could mask any infection-related fevers I might have
This statement shows understanding. Acetaminophen has antipyretic effects and can lower fever. After surgery, fever can be an important sign of infection, and masking it with antipyretics could delay recognition and treatment of postoperative infection. The client recognizes this potential issue, demonstrating appropriate awareness of how medications can affect clinical assessment.
D) If I still have pain 10 minutes after taking 1000 mg of acetaminophen, I should take two of oxycodone-acetaminophen
This statement demonstrates dangerous misunderstanding requiring immediate correction. Ten minutes is insufficient time for oral acetaminophen to reach peak effect. Onset of action for oral acetaminophen is typically 30 to 60 minutes. Taking additional medication after only 10 minutes could lead to dose stacking and eventual overdose. Additionally, the client does not know the acetaminophen content of the oxycodone-acetaminophen combination product. Common formulations contain 325 mg or 500 mg of acetaminophen per tablet, so taking two tablets could add 650 to 1000 mg of acetaminophen, potentially pushing the total toward or beyond the daily limit depending on what else has been taken. The client should follow the prescribed schedule and contact the provider if pain is not controlled, not self-escalate with additional medications. This statement requires further teaching about medication timing, combination product ingredients, and appropriate pain management escalation.
Conclusion
The client needs further teaching when stating they would take two oxycodone-acetaminophen tablets 10 minutes after plain acetaminophen due to risk of acetaminophen toxicity and inadequate time for the initial dose to work. The statements about rotating analgesics, knowing acetaminophen limits, and recognizing fever masking all demonstrate understanding. Therefore, the incorrect statement is about taking combination product shortly after plain acetaminophen, and the nurse must provide education about medication timing, acetaminophen content in combination products, and appropriate pain management strategies.

The diabetic client receives an injection of insulin glargine. What is the duration of insulin glargine?
A.
6 to 14 hours
B. 15 minutes
C. 2 to 4 hours
D. 18 to 24 hours
Rationale
The duration of insulin glargine is 18 to 24 hours, making it a long-acting basal insulin suitable for once-daily dosing to provide consistent background insulin coverage between meals and overnight.
Insulin glargine is a recombinant human insulin analog that was developed to provide a prolonged, peakless profile of insulin activity. It is created by modifying the human insulin molecule, replacing asparagine with glycine at position A21 and adding two arginines to the C-terminus of the B-chain. These modifications shift the isoelectric point, making glargine less soluble at neutral pH. When injected subcutaneously, it forms microprecipitates that slowly dissolve and release insulin into the circulation over an extended period. This provides a relatively constant, peakless level of insulin that mimics the body's basal insulin secretion, which is the low-level insulin release that occurs continuously between meals and during fasting periods such as overnight.
A) 6 to 14 hours
This duration describes intermediate-acting insulins such as NPH insulin. NPH has an onset of 1 to 2 hours, a peak at 4 to 12 hours, and a duration of 14 to 18 hours, though it can vary. It is not the duration of insulin glargine.
B) 15 minutes
This duration is not correct for any insulin. Even rapid-acting insulins have durations of several hours. Fifteen minutes might describe the onset of rapid-acting insulins, not their duration.
C) 2 to 4 hours
This duration describes rapid-acting insulins such as insulin lispro, aspart, and glulisine. These are used for mealtime coverage and have short durations that limit their effect to the postprandial period. They are not basal insulins.
D) 18 to 24 hours
This is the correct duration for insulin glargine, consistent with its use as a once-daily basal insulin. The exact duration can vary slightly among individuals, but it is consistently in the 18 to 24 hour range, providing stable coverage throughout the day and night.
Conclusion
Insulin glargine has a duration of 18 to 24 hours, making it suitable for once-daily basal coverage. The other options describe other insulin types: 6 to 14 hours for intermediate-acting, 15 minutes for onset not duration, and 2 to 4 hours for rapid-acting. Therefore, 18 to 24 hours is correct.

Which of these situations would cause the nurse to hold a dose of morphine?
A.
The temperature is above 38 degrees Celsius
B. The heart rate is above 90 bpm
C. The blood pressure is above 140 mm Hg systolic
D. Respiratory rate of 10 breaths per minute with an oxygen saturation level of 86%
Rationale
The nurse would hold a dose of morphine when the client has a respiratory rate of 10 breaths per minute with an oxygen saturation of 86%, as this indicates significant respiratory depression and hypoxemia, making further opioid administration dangerous.
Morphine is an opioid analgesic that produces its effects by binding to mu receptors in the central nervous system and elsewhere. While this provides effective pain relief, it also carries the risk of respiratory depression, which is the most serious adverse effect of opioid therapy. Respiratory depression occurs because mu receptor activation in the brainstem reduces the sensitivity of respiratory centers to carbon dioxide, the primary stimulus for breathing. This leads to decreased respiratory rate and depth, hypoventilation, and eventually hypoxia and hypercapnia. Before administering any opioid, the nurse must assess the client's respiratory status to ensure that further opioid administration is safe.
A) The temperature is above 38 degrees Celsius
Fever is not a contraindication to morphine administration. While fever should be investigated and treated appropriately, it does not preclude giving morphine if needed for pain. The nurse should assess the cause of fever but would not hold morphine based on temperature alone.
B) The heart rate is above 90 bpm
Tachycardia alone is not a reason to hold morphine. Pain itself can cause tachycardia, and morphine may actually help by relieving pain and reducing sympathetic stimulation. This finding does not indicate opioid toxicity and would not warrant holding the dose.
C) The blood pressure is above 140 mm Hg systolic
Hypertension is not a contraindication to morphine. Pain can elevate blood pressure, and morphine may help lower it through analgesia and sedation. This does not indicate opioid toxicity and would not warrant holding the dose.
D) Respiratory rate of 10 breaths per minute with an oxygen saturation level of 86%
This finding indicates significant respiratory depression and hypoxemia, making further morphine administration dangerous. A respiratory rate of 10 is below normal (bradypnea), and oxygen saturation of 86% is below normal (hypoxemia). Administering more morphine in this situation would worsen respiratory depression and could lead to respiratory arrest. The nurse should hold the dose, notify the provider, and be prepared to administer naloxone and provide respiratory support.
Conclusion
The nurse would hold a dose of morphine when respiratory rate is 10 with oxygen saturation of 86%, indicating respiratory depression and hypoxemia. Fever, tachycardia, and hypertension are not contraindications to morphine administration. Therefore, the respiratory findings warrant holding the dose and initiating appropriate interventions to address the opioid-induced respiratory depression.
The nurse is educating a client regarding the use of omeprazole. What statement by the client shows a proper understanding of how to take this medication?
A.
I should plan to take this medication for the rest of my life
B. I should take this medication with an antacid to maximize its effects
C. I should chew the medication when my heartburn is bad, so it absorbs more rapidly
D. I should take this medication on an empty stomach before I eat
Rationale
The client shows proper understanding by stating they should take omeprazole on an empty stomach before eating, as proton pump inhibitors require administration before meals for optimal activation and effectiveness in suppressing gastric acid secretion.
Omeprazole is a proton pump inhibitor that is widely used for conditions involving excessive gastric acid, including gastroesophageal reflux disease, peptic ulcer disease, Zollinger-Ellison syndrome, and as part of Helicobacter pylori eradication regimens. PPIs work by irreversibly inhibiting the hydrogen-potassium ATPase enzyme system, also known as the proton pump, in gastric parietal cells. This enzyme is responsible for the final step in acid secretion, pumping hydrogen ions into the stomach lumen in exchange for potassium ions. By inhibiting this pump, PPIs produce profound and long-lasting reduction in gastric acid secretion. However, for maximal effectiveness, the timing of administration is critical. The proton pump is not constantly active; it is stimulated to insert into the apical membrane of the parietal cell and become active primarily in response to meals, particularly the first meal of the day. When a PPI is taken on an empty stomach, approximately 30 to 60 minutes before a meal, it is absorbed and reaches the parietal cells just as they are being stimulated by the impending meal. This allows the drug to inhibit the active proton pumps, producing the greatest acid suppression. If taken at other times, many proton pumps may be inactive and sequestered within the cell, and the drug will not be as effective.
A) I should plan to take this medication for the rest of my life
This statement is not necessarily correct and reflects a misunderstanding of the duration of PPI therapy. While some patients with chronic conditions such as severe GERD or Zollinger-Ellison syndrome may require long-term maintenance therapy, many patients use PPIs for short, defined courses. For example, a standard course for erosive esophagitis might be 4 to 8 weeks, and H. pylori eradication regimens are typically 10 to 14 days. The duration of therapy should be determined by the underlying condition and the response to treatment, and patients should be periodically reassessed to determine if continued therapy is necessary. Assuming lifelong use without discussion with the provider is not appropriate.
B) I should take this medication with an antacid to maximize its effects
. Antacids can affect the absorption of PPIs and may reduce their effectiveness. Antacids work by neutralizing acid already present in the stomach, while PPIs work by inhibiting acid production. If taken together, the antacid could raise gastric pH and potentially affect the dissolution and absorption of the PPI, which is formulated to be released in an acidic environment. If both medications are needed, they should be spaced apart, typically with the PPI taken on an empty stomach before a meal and the antacid taken at a different time, such as between meals or at bedtime.
C) I should chew the medication when my heartburn is bad, so it absorbs more rapidly
This statement demonstrates a dangerous misunderstanding. Omeprazole capsules or tablets are formulated as delayed-release preparations, meaning they have an enteric coating that protects the drug from degradation by stomach acid. The coating allows the medication to pass through the stomach intact and be absorbed in the small intestine. Chewing or crushing the medication destroys this protective coating, exposing the drug to stomach acid where it will be degraded and rendered ineffective. Additionally, chewing would release the entire dose at once, potentially causing irritation and not providing the intended prolonged effect. The medication should always be swallowed whole, not chewed, crushed, or opened.
D) I should take this medication on an empty stomach before I eat
This statement is correct and shows proper understanding of omeprazole administration for optimal effect. Taking it 30 to 60 minutes before the first meal of the day ensures maximal absorption and inhibition of the proton pumps that are activated by the meal. This timing produces the best acid suppression and therapeutic response.
Conclusion
The client demonstrates proper understanding by stating that omeprazole should be taken on an empty stomach before eating. Assuming lifelong use, taking with antacids, or chewing are all incorrect. Therefore, empty stomach before meals is correct, reflecting knowledge of PPI administration for maximal acid suppression.
Which of these self-care measures should be emphasized in client education regarding phenytoin?
A.
Gradually reduce prescribed dose if seizures do not occur for one month
B. Instill mineral oil into both ears once a week
C. Expect green urine due to medication metabolites
D. Brush after every meal and floss teeth daily
Rationale
The self-care measure to emphasize with phenytoin is to brush after every meal and floss teeth daily, as meticulous oral hygiene helps prevent or minimize phenytoin-induced gingival hyperplasia, a common and potentially significant side effect.
Phenytoin is a hydantoin anticonvulsant that has been used for decades in the management of various seizure disorders. It works by stabilizing neuronal membranes and decreasing seizure activity through effects on sodium channels. While effective, phenytoin has a well-known and characteristic side effect: gingival hyperplasia, or overgrowth of gum tissue. This condition occurs most frequently in children and young adults but can affect patients of any age. The exact mechanism is not fully understood but involves stimulation of fibroblast proliferation and increased collagen production in response to phenytoin or its metabolites. The hyperplasia typically begins as painless, firm, nodular enlargement of the interdental papillae and can progress to cover a significant portion of the tooth crowns. This can interfere with chewing, speech, and aesthetics, and can also create areas where plaque accumulates, increasing the risk of periodontal disease and dental caries. Meticulous oral hygiene is the most important preventive measure. Regular brushing and flossing remove plaque and reduce gingival inflammation, which appears to potentiate the hyperplastic response. Patients should be instructed to brush after every meal, floss daily, and have regular dental check-ups.
A) Gradually reduce prescribed dose if seizures do not occur for one month
This instruction is dangerous and must never be given. Anticonvulsant medications must be taken consistently as prescribed, and doses should never be adjusted or discontinued without direct provider supervision. Abrupt withdrawal or dose reduction can precipitate breakthrough seizures, including status epilepticus, which is a medical emergency. The absence of seizures indicates that the current regimen is effective, not that it can be reduced.
B) Instill mineral oil into both ears once a week
Mineral oil instillation into the ears has no relation to phenytoin therapy and is not a recognized self-care measure for any condition related to this medication. This instruction is irrelevant and potentially harmful if the client has any ear pathology. It should never be included in phenytoin education.
C) Expect green urine due to medication metabolites
Phenytoin does not cause green urine. Some medications can discolor urine, but phenytoin is not among them. Providing this information would be incorrect and could cause unnecessary concern or lead the client to dismiss other changes in urine color that might be significant.
D) Brush after every meal and floss teeth daily
This is the correct and essential self-care measure to emphasize. The client should understand why this is important, including the mechanism of gingival hyperplasia and the role of plaque and inflammation in exacerbating the condition. They should be advised to use a soft toothbrush to avoid gum irritation, to floss gently but thoroughly, and to see a dentist regularly for professional cleaning and monitoring. Early intervention can prevent progression and may reduce the need for surgical gingivectomy in severe cases.
Conclusion
The self-care measure to emphasize with phenytoin is meticulous oral hygiene including brushing after meals and flossing daily to prevent or minimize gingival hyperplasia. Dose adjustment, ear oil, and green urine are all incorrect. Therefore, oral hygiene is correct, helping the client manage this common side effect and maintain dental health.
RN Exams
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests
ATI Quizzes
3 Practice Tests